Dec 16, 2020 | Volume 10 - Issue 4
Jennie Ju, Rose Merrell-James, J. Kelly Coker, Michelle Ghoston, Javier F. Casado Pérez, Thomas A. Field
Few models exist that inform how counselor education programs proactively address the gap between diverse student needs and effective support. In this study, we utilized grounded theory qualitative research to gain a better understanding of how 15 faculty members in doctoral counselor education and supervision programs reported that their departments responded to the need for recruiting, retaining, and supporting doctoral students from underrepresented racial minority backgrounds. We also explored participants’ reported successes with these strategies. A framework emerged to explain the strategies that counselor education departments have implemented in recruiting, supporting, and retaining students from underrepresented racial minority backgrounds. The main categories identified were: (a) institutional and program characteristics, (b) recruitment strategies, and (c) support and retention strategies. The latter two main categories both had the same two subcategories, namely awareness and understanding, and proactive and intentional efforts. The latter subcategory had three subthemes of connecting to cultural identity, providing personalized support, and faculty involvement.
Keywords: underrepresented racial minority, recruitment, retention, counselor education, doctoral
For the past several years, doctoral counselor education and supervision (CES) programs accredited by the Council for Accreditation of Counseling and Related Educational Programs (CACREP) have experienced a greater enrollment of students from diverse backgrounds (CACREP, 2014, 2015). According to the CACREP Vital Statistics report (2018), two-fifths of doctoral students have a diverse racial or ethnic identity. This stands in contrast to the less than 30% of full-time faculty in CACREP-accredited programs who identify as having a diverse racial or ethnic identity. In 2012, the total doctoral-level enrollment in CACREP institutions was 2,028, where 37% of the students were from racially or ethnically diverse backgrounds (CACREP, 2014). Enrollment increased to 2,561 in 2017, with 1,016 students from racially or ethnically diverse communities, which translates to 39.7% of total enrollment (CACREP, 2018).
Accompanying this trend is a growing awareness that diverse doctoral students in counseling and related disciplines are not receiving adequate support and preparation to succeed (Barker, 2016; Henfield et al., 2011; Hollingsworth & Fassinger, 2002; Zeligman et al., 2015). CACREP-accredited programs are charged with making a “continuous and systematic effort to attract, enroll, and retain a diverse group of students and to create and support an inclusive learning community” (CACREP, 2016, section 1.K.). Yet few models exist that inform how CES programs proactively address the gap between diverse student needs and effective support. Literature is limited on this topic. Little is known about effective and comprehensive structures for recruiting, supporting, and retaining CES doctoral students from underrepresented minority (URM) backgrounds that take into consideration CACREP standards, student needs, economics, sociocultural barriers, and student opportunities.
In this study, we used Federal definitions of URM status in higher education to guide our inquiry. A section of the U.S. Code pertaining to minority persons provides the following definition for minority, and it is the one we chose to use in our study: “American Indian, Alaskan Native, Black (not of Hispanic origin), Hispanic (including persons of Mexican, Puerto Rican, Cuban, and Central or South American origin), Pacific Islander, or other ethnic group” (Definitions, 20 U.S.C. 20 § 1067k, 2020). This definition is important to higher education, as it is used by institutions to allocate funding for URM students. We note here that cultural diversity also spans other aspects of minority status, such as gender identity, sexual/affectional identity, and ability/disability status, among others. We restricted the focus of this study to exploring racial identity pertinent to URM status, following the U.S. Code definition.
Recruitment of Doctoral Students From URM Backgrounds
Understanding the diversification of doctoral students in CES programs begins by first considering effective methods for recruitment used by those programs. Recruitment of CES doctoral students of color may necessitate intentional and active approaches, such as building personal connections in the community and family (Hipolito-Delgado et al., 2017; McCallum, 2016). CES doctoral programs might consider recruitment not as a yearly endeavor, but a long-term, day-to-day strategy. Early exposure, responsiveness to student needs (e.g., financial needs), commitment to diversity (e.g., hiring and retaining faculty members from diverse backgrounds), community relationships, and program location have all been identified as important factors to consider in the extant literature.
Early Exposure and Recruitment
Programs can promote more representative recruitment through earlier exposure to the disciplinary field and community connections (Grapin et al., 2016; Hipolito-Delgado et al., 2017; McCallum, 2016). Introducing the possibility of pursuing doctoral studies in CES during the high school and undergraduate experience can increase student familiarity with the profession and may promote their long-term attention to the field (Luedke et al., 2019; McCallum, 2016). McCallum (2015, 2016) found that early familial and social messages about the low viability of doctoral studies was a deterrent among African American students and that mentorship and exposure to doctoral careers by professionals can help renew interest. Many undergraduate students from culturally diverse backgrounds lack opportunities to learn and develop ownership of doctoral-level professions and in some cases lack knowledge that those professions even exist (Grapin et al., 2016; Luedke et al., 2019).
Responsiveness to Needs and Commitment to Diversity
To successfully recruit doctoral students from culturally diverse backgrounds, CES programs need to be responsive to potential students’ needs. In fact, a program’s commitment to diversity and the demonstration of that commitment through student and faculty representation have been found to be highly influential factors in applicants’ decisions to enter a doctoral program (Foxx et al., 2018; Grapin et al., 2016; Zeligman et al., 2015). An additional aspect of this responsiveness in recruitment is the program’s ability to ensure and provide financial support to incoming students (Dieker et al., 2013; Proctor & Romano, 2016). Given the unique barriers experienced by culturally diverse communities throughout the educational system, doctoral programs can be prepared to compensate for some of these obstacles through financial and academic support.
Community Relationships and Program Location
In keeping with recruitment as a long-term endeavor, research has found that community relationships and program location are essential when recruiting doctoral students from culturally diverse backgrounds (Foxx et al., 2018; Hipolito-Delgado et al., 2017). CES programs can look to build relationships with their local culturally diverse communities and recruit from those communities, rather than looking nationally for their doctoral students (Foxx et al., 2018; Hipolito-Delgado et al., 2017). Proctor and Romano (2016) found that proximity to representative communities and applicants’ support systems had a significant impact on their decision to enter doctoral programs. Community connections also offered more opportunities to clarify admission requirements for interested students, a barrier for many first-generation students (Dieker et al., 2013; Hipolito-Delgado et al., 2017).
Support and Retention of Culturally Diverse Doctoral Students
Once admitted to a doctoral program in CES, program faculty are required by the CACREP (2015) standards to make a continuous and systematic effort to not only recruit but also to retain a diverse group of students. To do so, faculty should be attentive to both common and unique personal and social challenges, experiences of marginalization and isolation, and acculturative challenges that students from URM backgrounds may face.
Personal and Social Challenges
Students from URM backgrounds have faced ongoing challenges with their ability to establish a clear voice and ethnic identity in predominately Euro-American CES programs (Baker & Moore, 2015; González, 2006; Guillory, 2009; Lerma et al., 2015). This phenomenon has been written about for decades (Lewis et al., 2004). Lewis et al. (2004) described the lived experiences of African American doctoral students at a predominantly Euro-American, Carnegie level R1 research institution. Key themes that emerged included feelings of isolation, tokenism, difficulty in developing relationships with Euro-American peers, and learning to negotiate the system. Further review of the literature found consistent challenges across diverse students, especially with establishing voice and ethnic identity (Baker & Moore, 2015; González, 2006; Lerma et al., 2015). Guillory (2009) noted that the level of difficulty American Indian students will face in college depends in large measure on how they see and use their ethnic identity. Utilizing a narrative inquiry approach, Hinojosa and Carney (2016) found that five Mexican American female students experienced similar challenges in maintaining their ethnic identities while navigating doctoral education culture.
Challenges of Marginalization and Isolation
Marginalization and isolation were additional common themes across diverse groups. Blockett et al. (2016) concluded that students experience marginalization in three areas of socialization, including faculty mentorship, professional involvement, and environmental support. Other researchers have also concluded that both overt and covert racism is a contributing factor to marginalization in the university culture (Behl et al., 2017; González, 2006; Haizlip, 2012; Henfield et al., 2013; Interiano & Lim, 2018; Protivnak & Foss, 2009). Study themes also indicated that students often expressed frustration from tokenism in which they felt expectations to represent the entire race during doctoral programs (Baker & Moore, 2015; Haizlip, 2012; Henfield et al., 2013; Lerma et al., 2015; Woo et al., 2015). Henfield et al. (2011) investigated 11 African American doctoral students and found that the challenges included negative campus climates regarding race, feelings of isolation, marginalization, and lack of racial peer groups during their graduate education. Similarly, using critical race theory to examine how race affects student experience, Henfield et al. (2013) found African American students experienced a lack of respect from faculty because of their racial and ethnic differences. Students who had previously studied at historically Black colleges and universities (HBCUs) or Hispanic serving institutions (HSIs) reported that the lack of racial/ethnic diversity representation during doctoral study in predominantly White institutions (PWIs) contributed to their experience of stress, anxiety, and irritation (Henfield et al., 2011, 2013).
Culture and Acculturation Challenges
Collectivity and community seem to be consistent values that doctoral students from URM backgrounds have expressed as missing or not understood by faculty (González, 2006; Lerma et al., 2015). For example, faculty may not understand familia, a Latinx student’s obligation to family (González, 2006; Lerma et al., 2015). Several authors have reported that culturally diverse doctoral students experience difficulty adjusting to a curriculum or program that values a Eurocentric individualist form of counseling (Behl et al., 2017; Interiano & Lim, 2018; Woo et al., 2015).
International students also experience similar anxiety and stress during their doctoral studies in the United States. In addition to adjusting to speaking and writing in a language that may not be their primary language, their supervision skills and clinical abilities can be questioned by Euro-American supervisees despite international students having advanced training and supervisory status (Behl et al., 2017). Interiano and Lim (2018) used the term “chameleonic identity” (p. 310) to describe foreign-born doctoral students’ attempts to adapt to the Euro-American cultural context of their CES programs. They posited that international students experienced a sense of conflict, loss, and grief associated with the pressure to adopt cultural norms embedded in Euro-American counseling and higher education in the United States.
Strategies to Support and Retain Culturally Diverse Doctoral Students
To address these stressors and barriers to persistence in doctoral studies, faculty members can employ several strategies to support and retain students from culturally diverse backgrounds, such as mentorship, advising, increasing faculty diversity, understanding students’ cultures, and offering student support services.
Mentorship
Some scholars recommend intentional utilization of mentorship as a strategy for improving retention and graduation rates of diverse students in higher education (Evans & Cokley, 2008; Rogers & Molina, 2006). Chan et al. (2015) defined mentoring relationships as a “one-to-one ongoing connection between a more experienced member (mentor) and less experienced member (protégé) that is aimed to promote the professional and personal growth of the protégé through coaching, support and guidance” (p. 593). Chan and colleagues added that mentoring can involve transferring needed information, feedback, and encouragement to the protégé as well as providing emotional support.
Zeligman and colleagues (2015) indicated that mentoring impacts both the recruitment and the retention of doctoral students from URM backgrounds. The quality and significance of mentoring relationships and participants’ connection with faculty members during a doctoral program seems to influence choice in continuing doctoral study for URM students (Baker & Moore, 2015; Protivnak & Foss, 2009). Blackwell (1987) noted that the most powerful predictor of enrollment and graduation of African American students at a professional school was the presence of an African American faculty member serving as the student’s mentor.
Although a powerful tool for recruiting and retaining diverse doctoral students, mentoring can also create retention issues if inadequate or problematic. Students may receive ambiguous answers to advising questions and may not receive support when life circumstances interfere with study (Baker & Moore, 2015; Henfield et al., 2013; Interiano & Lim, 2018). In such situations, some students may seek other faculty mentors within the department (Baker & Moore, 2015; Henfield et al., 2013; Interiano & Lim, 2018) or may specifically establish mentoring relationships with faculty from diverse cultural backgrounds to receive greater support for their experience of being a person of color (González, 2006; Woo et al., 2015; Zeligman et al., 2015). Diverse students may also seek mentors from outside of their doctoral program. Woo and colleagues (2015) found that international students selected professional counseling mentors from their home community that they considered to be caring and nonjudgmental of their doctoral work in comparison to faculty supervisors they felt were neither culturally sensitive nor supportive of international students.
Because of an existing disparity in the availability of African American counselor educators and supervisors who can serve as mentors to African American doctoral counseling students, Euro-American counselor educators and supervisors can provide mentorship support to underrepresented African American doctoral students. Brown and Grothaus (2019) conducted a phenomenological study with 10 African American doctoral counseling students. The authors found that trust was a primary factor in establishing successful cross-racial relationships, and that African American students could benefit from “networks of privilege” (p. 218) during cross-racial mentoring. The authors also found that if issues of racism and oppression are not addressed, it can interfere with establishing mentoring relationships.
Establishing same-race, cross-race, and/or cultural community affiliations provides support to culturally diverse doctoral students. In addition, increasing faculty diversity can be a viable measure to support and retain diverse doctoral students.
Increasing Faculty Diversity
The presence of diverse faculty members in CES has been discussed in the literature as a positive element in the recruitment, support, and retention of diverse doctoral students (Henfield et al., 2013; Lerma et al., 2015; Zeligman et al., 2015). Henfield and colleagues (2013) emphasized the need to proactively recruit and retain African American CES faculty to attract, recruit, and retain African American CES doctoral students. Recruiting and retaining faculty members from URM backgrounds requires intentional effort. Ponjuan (2011) suggested the development of mentoring policies that establish Hispanic learning communities and improve overall departmental climate as efforts to help increase the number of Latinx faculty at an institution. The next section discusses the relational significance of having counselor educator mentors who share cultural backgrounds and worldviews.
Understanding of Students’ Culture
Lerma et al. (2015) recommended that doctoral faculty in CES programs be responsive to both the professional and personal development of their students. One area of dissonance for doctoral students from URM backgrounds involves differences in cultural worldview. Marsella and Pederson (2004) posited that “Western psychology is rooted in an ideology of individualism, rationality, and empiricism that has little resonance in many of the more than 5,000 cultures found in today’s world” (p. 414). Ng and Smith (2009) found that international counselor trainees, particularly those from non-Western nations, struggle with integrating Eurocentric theories and concepts into the world they know. This presents opportunities for counselor educators to intentionally search for appropriate pedagogies and to critically present readings and other media that portray the multicultural perspective (Goodman et al., 2015).
Counseling departments can promote, facilitate, and value a multicultural orientation when focusing on student success and development. Lerma et al. (2015) and Castellanos et al. (2006) emphasized the need to understand the importance of family and peer support among Latinx students and faculty, specifically in recreating familia in the academic environment to help increase resilience. When working with African American students, Henfield et al. (2013) recommended that faculty should possess an understanding and respect of African American culture and be more “cognizant of how a history of oppression may influence students’ perception, behavior, and nonbehavior” (p. 134). Faculty members should also possess an understanding of student financial difficulties and potential knowledge gaps in preparation for graduate school (González, 2006; Zeligman et al., 2015).
Student Support Services
Another effective area of support for doctoral students from diverse backgrounds is student-based services. These services include broader institutionally based resources, student-guided groups or activities, and community-based efforts. Institutional resources that seem to hold promise in increasing support for and the potential success of diverse students include race-based organizations (Henfield et al., 2011). Peer support has been consistently identified as an important factor in doctoral student persistence (Chen et al., 2020; Henfield et al., 2011; Rogers & Molina, 2006). Student-centered organizations can effectively provide a sense of belonging and an environment that facilitates peer support among those with shared interests on campus (Rogers & Molina, 2006). Henfield et al. (2011) found that African American students sought collaborative support through race-based campus organizations and with students who share similar backgrounds and interests. Multicultural-based, student-centered organizations and events are resources that institutions utilize as active support for multicultural individuals that contribute to “sustaining diverse students to reach the finish line of graduation with a strong foundation from which to launch their counseling career” (Chen et al., 2020, p. 10).
Chen et al. (2020) and Behl et al. (2017) have both reported that writing centers are an important support for international students as well as students from refugee, immigrant, and underprivileged communities. Ng (2006) reported that counseling students from non–English-speaking countries often experience challenges related to English proficiency. Chen et al. (2020) added that tutoring in writing is critical for students who come from cultures that are unaccustomed to the formal use of writing styles (e.g., APA style). Furthermore, helping international students understand classroom norms and culture through an orientation as part of the onboarding process can be a preventive support (Behl et al., 2017).
Purpose of the Present Study
The CACREP standards have created expectations and requirements for counseling programs to recruit, retain, and support students from diverse backgrounds. There now exists a wide swath of literature that has reported a variety of efforts toward these goals (Baker & Moore, 2015; Evans & Cokley, 2008; Rogers & Molina, 2006; Woo et al., 2015). Yet at the time of writing, there is not a clearly articulated path for CES programs to follow with regard to these efforts. For example, there is currently no information available regarding which strategies are more successful or easier to implement than others. This study aimed to address this gap in knowledge for how to attract, support, and retain students from diverse backgrounds in CES doctoral programs. The purpose of our study was to explore: (a) strategies doctoral programs use to recruit, retain, and support underrepresented doctoral students from diverse backgrounds, and (b) the level of success these programs have had with their implemented strategies.
Methodology
Throughout the study, we were grounded by a shared belief in constructivist philosophy that participants’ realities are socially co-constructed, and therefore, all responses are valued regardless of frequency. From this philosophical position, we chose to approach the topic using a qualitative framework (Lincoln & Guba, 2013). Grounded theory was selected because it utilizes a systematic and progressive gathering and analysis of data, followed by grounding the concepts in data that accurately describe the participants’ own voices (Charmaz, 2014; Corbin & Strauss, 2015). This approach allows the integration of both the art and science aspects of inquiry while supporting systematic development of theoretical constructs that promote richer comprehension and explanation of social phenomena (Charmaz, 2014; Corbin & Strauss, 2015). Through the grounded theory approach, we hoped to establish an emergent framework to explain practice and provide recommendations for CES programs striving to support diverse doctoral students.
This study was part of a larger comprehensive qualitative study based on the basic qualitative research design described by Merriam and Tisdell (2016) that examined a series of issues pertinent to doctoral counselor education. Preston et al. (2020) described the larger qualitative project that involved the collection and analysis of in-depth qualitative interviews with 15 doctoral-level counselor educators. This article focuses on the analysis of interview data gathered through two of the interview questions: 1) Which strategies has your program used to recruit underrepresented students from diverse backgrounds? How successful were those? and 2) Which strategies has your program used to support and retain underrepresented students from diverse backgrounds? How successful were those?
Researcher Positioning, Role, and Bias
The last author utilized the etic position, which is through the perspective of the observer, to conduct all interviews with selected participants. Approaching the interview process around the topic of doctoral-level counselor education through the etic status was important because the author had not worked in a doctoral-level CES program previously but has been a member of the counselor education community.
The situational context was composed of the researchers’ and participants’ experiences and perceptions, the social environment, and the interaction between them (Ponterotto, 2005). Therefore, we engaged in reflexivity to increase self-awareness of biases related to this topic (Corbin & Strauss, 2015). This required continual examination of the potential influence that identified biases may have on the research process. In keeping with the standard of reflexivity, we recorded our personal experiences as they related to the research questions with the use of memoing to bracket potential biases throughout the coding and analysis process.
All members of the research team are from CACREP-accredited institutions in the Western and Eastern parts of the United States. The coding team consisted of the first four authors. The fifth author contributed to writing the manuscript, and the sixth author conducted the interviews as part of the larger study and assisted in writing sections of the methodology. All four coding team members had previously been doctoral students in a CES program, though only one of the coding team members had ever worked in a CES doctoral program as a full-time faculty member. This person thus had emic positioning, while other team members held etic positioning.
Four of the five members of the coding team were from diverse backgrounds themselves and were influenced by their personal experiences as doctoral students. Two members of the coding team identified as cisgender, heterosexual African American females. One member identified as a cisgender, heterosexual Asian American female and another as a cisgender, heterosexual Euro-American female. The coding team members were aware of potential biases around expectations toward the programs discussed in the transcripts and recognized the need to closely examine personal perceptions and understanding of the interview data.
Two coding team members observed the lack of racial/ethnic diversity at the counseling programs where they currently work. They experienced Eurocentric, non–culturally responsive methods of support and development that led them to recognize the potential bias of shared experience with multicultural participants. One coding team member was Euro-American and was a part of an all Euro-American doctoral cohort. The program they attended had an all Euro-American faculty and she wondered whether the predominantly Euro-American participants in this study had an understanding of the challenges of diverse students. Having taught in doctoral programs, this researcher was aware of potential biases around types of universities that might be successful in recruiting but less so in retaining diverse students.
Participants
Participants were selected based on the following study design criteria: 1) current full-time core faculty members in CES, and 2) currently working in a doctoral-level CES program that is accredited by CACREP. At the time of writing, there were 85 CACREP-accredited doctoral CES programs in the United States (CACREP, 2019). Purposeful sampling was used to identify and recruit participants who had experiences working in doctoral-level counselor education (Merriam & Tisdell, 2016). Information-rich cases were sought to understand the phenomenon of interest.
Maximum variation sampling was also employed for the purposes of understanding the perspectives of counselor educators from diverse backgrounds with regard to demographic characteristics and program characteristics and to avoid premature saturation (Merriam & Tisdell, 2016). Based on the belief that counselor educator perspectives may differ by background, the research team used the following criteria to select participants: (a) racial and ethnic self-identification; (b) gender self-identification; (c) length of time working in doctoral-level CES programs; (d) Carnegie classification of the university where the participant was currently working (The Carnegie Classification of Institutions of Higher Education, 2019); (e) region of the counselor education program where the participant was currently working, using regions commonly defined by national counselor education associations and organizations; and (f) delivery mode of the counselor education program where the participant was currently working (e.g., in-person, online; Preston et al., 2020).
The 15 study participants belonged to separate doctoral-level CES programs, with no more than one participant representing each program. The sample was composed of 11 participants (73.3%) who self-identified as White, with multiracial/multiethnic (n = 1, 6.7%), African American (n = 1, 6.7%), Asian (n = 1, 6.7%), and Latinx ethnic backgrounds (n = 1, 6.7%) also represented. Seven participants self-identified as female (46.7%), eight participants as male (53.3%), and none identified as non-binary or transgender. The majority of participants identified as heterosexual (n = 14, 93.3%), with one participant (6.7%) identifying as bisexual.
Participants’ experience as faculty members averaged full-time work for 19.7 years (SD = 9.0 years) and a median of 17 years, with a range from 4 to 34 years. For most of those years, participants worked in doctoral-level CES programs (M = 17.3 years, SD = 9.2 years, Mdn = 16 years), ranging from 3 to 33 years. More than half of participants (n = 9, 60%) spent their entire careers working in doctoral-level CES programs. Geographic distribution of the programs where participants worked were as follows: eight belonged to the Southern region (53.3%); two each (13.3%) belonged to the North Atlantic, North Central, and Western regions; and one program (6.7%) belonged to the Rocky Mountain region. Twelve participants (80%) were working in brick-and-mortar programs, and three participants (20%) were working in online or hybrid programs. With regard to Carnegie classification representation, nine (60%) were working at Doctoral Universities – Very High Research Activity (i.e., R1) institutions, two (13.3%) were working at Doctoral Universities – High Research Activity (i.e., R2) institutions, and four (26.7%) were working at universities with the Master’s Colleges and Universities: Larger Programs designation (The Carnegie Classification of Institutions of Higher Education, 2019; Preston et al., 2020).
Procedure
After receiving approval from the last author’s IRB, the last author used the CACREP (2018) website directory to identify and recruit doctoral-level counselor educators who worked at the CACREP-accredited CES programs. Recruitment emails were sent to one faculty member at each of the 85 accredited programs. Fifteen of the 34 faculty (40% response rate) who responded were selected to participate on the basis of maximal variation.
Interview Protocol
Each interview began with demographic questions that addressed self-identified characteristics such as race, ethnicity, gender, sexual/affectional orientation, years as a faculty member, years working in doctoral-level CES programs, number of doctoral programs the participant had worked in, and regions of the programs in which the counselor educator had worked. A series of eight in-depth interviews followed to address the research questions of the larger qualitative study. Interview questions developed in accordance with Patton’s (2014) guidelines were open-ended, as neutral as possible, avoided “why” questions, and were asked one at a time in a semi-structured interview protocol, with sparse follow-up questions salient to the main questions to ensure understanding of participant responses. Adhering to the interview protocol as outlined in Appendix A helped to ensure that data was gathered for each research question to the highest extent possible. Participants received the interview questions ahead of time upon signing the informed consent agreement. A pilot of the interview protocol was conducted with a faculty member in a doctoral-level CES program prior to commencing the study.
The interviews lasted approximately 60 minutes and were recorded using the Zoom online platform. One exception was an interview that occurred in-person during a professional conference and thus was recorded via a Sony digital audio recorder. All demographic information and recordings were assigned an alphabetical identifier known only to the last author and were blinded to subsequent transcribers and coders.
Data Analysis
Data analysis, as outlined by Corbin and Strauss (2015), employs the techniques of coding interview data to derive and develop concepts. In the initial step of open coding, the primary task is to “break data apart and delineate concepts to stand for blocks of raw data” (Corbin & Strauss, 2015, p. 197). During this step, the coding team sought to identify a list of significant participant statements about how they and their department perceive, value, and experience the responsibility of recruiting, retaining, and supporting underrepresented cultural groups. We met to code the first three of 15 transcripts together via Zoom video platform. The task of identifying codes included searching for data that was salient to the research questions and engaging in constant comparison until reaching saturation (Corbin & Strauss, 2015). We maintained a master codebook of participant statements that the team decided were relevant, then added descriptions and categories to the codes. Utilizing this same strategy, the remaining 12 transcripts were coded in dyads to make sure the coding team was not overlooking pertinent information.
When discrepancies occurred, the coding team utilized the following methods to resolve them:
(a) checking with each other for clarification and understanding of each person’s view on the code, (b) reviewing previous and subsequent lines for context, (c) slowing down the pace of coding to allow space for reflection on the team members’ thoughts and feeling about a code, (d) considering the creation of a new code if one part of the statement added new data that was not covered in the first part of the statement, and (e) referring back to the research questions to determine relevance of the statement. Discrepancies in coding were questions around statements that: (a) were vague, (b) contained multiple codes, (c) were similarly phrased, (d) reflected a wish rather than an action on the part of the program, and (e) presented interesting information about the participant’s program but did not address the research question.
The subsequent step of axial coding involved the task of relating concepts and categories to each other, from which the contexts and processes of the phenomena emerge (Corbin & Strauss, 2015). The researchers then framed emerging themes and concepts to identify higher-level concepts and lower-level properties as well as delineated relationships between categories until saturation was reached. In the step of selective coding, the researchers engaged in an ongoing process of integrating and refining the framework that emerged from categories and relationships to form one central concept (Strauss & Corbin, 1998).
Trustworthiness
Standards of trustworthiness were achieved by incorporating procedures as outlined by Creswell et al. (2007) and Merriam and Tisdell (2016). The strategies included enhancing credibility through clarification of researcher bias to illustrate the researchers’ position as well as identifying a priori biases and assumptions that could potentially impact our inquiry. In addition, the research team members were from different counselor education programs, which contributed to moderating bias in coding and analysis. In an attempt to avoid interpreting data too early during the coding process, the researchers used emergent, in vivo, verbatim, line-by-line open coding. Furthermore, the interviewer intentionally chose not to participate in coding the data in order to minimize bias through being too close to the data. To promote consistency, the last author clearly identified and trained research teams associated with the larger study. The last author also used member checking and kept an audit trail of the process to enhance credibility. Purposive sampling and thick description were used to ensure adequate representation of perspectives and thus strengthen the transferability and dependability qualities of the study (Merriam & Tisdell, 2016).
Results
Implementing strategies that make a difference was the central concept in describing the process of CES faculty participants’ experience with recruiting and retaining diverse doctoral students. These strategies refer to programmatic steps that counselor educator interview participants had found to be effective in the recruitment, support, and retention of culturally diverse doctoral students. This central concept was composed of three progressive and interconnected categories, each with its own subcategories, properties, and accompanying dimensions. These three categories were institutional and program characteristics, recruitment strategies, and support and retention strategies. The three major categories shared the subcategory of awareness and understanding, while the recruitment strategies and support and retention strategies categories shared the subcategory of proactive and intentional efforts. The conceptual diagram of these categories and subcategories is depicted in Figure 1.
Figure 1
Conceptual Diagram of Strategies That Make a Difference in Recruiting and Supporting
Culturally Diverse Doctoral Students
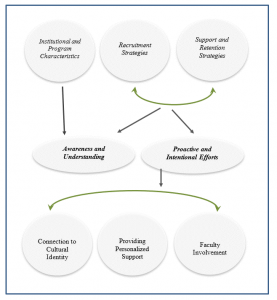
Institutional and Program Characteristics
The category institutional and program characteristics refers to features that are a part of program identity. This category was significant, as it represents the backdrop for a unique set of conditions in which the participants experienced the limitations as well as strengths of the program environment. Institutional and program characteristics may be part of the institution’s natural setting that the faculty participant had little control over, such as geographic location, institution size, institution reputation, tuition cost, or demographic composition of the area in which the program was located. At times, these factors were helpful for recruitment purposes. One participant described how the program’s geographic location positively impacted the recruitment of prospective students, including diverse students: “We are the only doctoral program in the state, so I think that carries some clout.” Another participant added, “A lot of it is financial . . . They largely choose programs because they are geographically convenient, so they can work or be close to family. So, their choice is largely guided by economic and geographic factors.”
Institutional and program characteristics also included factors that influenced support and retention of diverse students through their doctoral journey. Characteristics mentioned as either a hindrance or a support for diverse students included: (a) presence of diverse faculty, visual representation, and student body; (b) supportive environment for diverse students; (c) faculty attitudes and dispositions which create either a welcoming or hostile sociocultural climate; (d) fellowship or scholarship monies intended for diverse students; (e) evidence of valuing of and commitment to diversity; (f) multicultural and social justice focused activities; and (g) faculty who share common research interests with their students. From this list, it was evident that doctoral students seemed best supported by program qualities and actions that communicated a valuing of and commitment to diversity.
Awareness and Understanding
Participants indicated awareness that the context in which the institution and program exist presents as either a hindrance or a benefit to diversity. For example, geographic location and demographic composition of the locality can pose a barrier to recruitment as one participant expressed: “Our university itself is not going to attract people. It is a very White community.” This participant understands that this means the program will need to develop specific recruitment efforts to mitigate this potential barrier to “show students that this is a program that would be welcoming and take proactive steps to do that.”
Participants also indicated an awareness that students can sense whether diversity-related issues will be given priority. One participant stated, “Students are really astute about getting a sense for how committed a department is to diversity. So, having tangible evidence there is a willingness to commit to diversity at the faculty level is super important.” Another participant shared, “Our interview process is a barrier . . . There can be some privileged White males who are highly, highly confrontational, and I don’t think that’s an appropriate recruitment style for sending a welcoming message to minority candidates.”
Recruitment Strategies
The second major category identified in the data, recruitment strategies, pertains to the process of developing and implementing plans for the primary purpose of attracting individuals from diverse backgrounds to apply and enroll in the program. The recruitment strategies category is composed of two subcategories that are shared with the support and retention strategies, namely awareness and understanding and proactive and intentional efforts.
Awareness and Understanding
Participants shared a variety of responses regarding their awareness and understanding of the importance of creating a diverse learning community. Some participants reported that their departments proactively sought to recruit underrepresented students, whereas others acknowledged that their departments made no such attempt. At times, this was due to the structure of recruiting at the university: “Our program doesn’t necessarily get involved in admissions that much . . . We have an admissions team, and they have a whole series of strategies in place.” At other times, participants reported that their program was unintentional about recruiting diverse students: “We don’t have any good strategy particularly. It’s accident, dumb luck and accident.” One participant experienced distress and confusion because of their program’s perceived misalignment with CACREP standards: “These are key standards for programs, and one that programs have struggled with, and we certainly have too.”
Proactive and Intentional Efforts
Participants reported engaging social resources such as personal connections and networks to recruit diverse students. As one participant described, “Recruiting diverse students begins with personal networks. So, we use personal networks, professional networks, alumni network.” In addition to recruiting through alumni and professional organizations and conferences, participants found success through partnerships with community agencies as well as building relationships with HBCUs and HSIs. One participant captured the process this way: “It’s about maintaining relationships with graduates, with colleagues. We know, for us to diversify our student body, we cannot just look to the surrounding states to produce a diverse student body. We have to go beyond that.”
In addition to reaching out to master’s programs with sizable diverse student populations, one common strategic effort involved finding financial support for diverse doctoral students, from departmental, institutional, or external funding sources. One participant stated, “We also know in our program where the sources for funding underrepresented populations are; we know how to hook people into those sources of funding.” Another participant shared, “Our institutions have funding mechanisms, including some that are for historically marginalized populations or underrepresented populations. We have been successful in applying for those and getting those.”
Participants indicated a commitment to making changes to their typical mode of recruitment strategy and recognized that supporting diverse students required the implementation of strategies that differed from typical recruiting and retaining activities. Three subcategories that emerged as representing effective recruitment and support strategies were (a) connection to cultural identity, (b) providing personalized support, and (c) involvement of faculty.
Connection to Cultural Identity. Consistent with the literature, participants reported that students seemed drawn to programs that valued their cultural background and research interests associated with their identity. For example, participants reported that it was important to have faculty who are interested in promoting social justice and diversity and sharing similar research interests to their students. As one participant described: “The student picked us because we supported their research interest of racial battle fatigue.” This participant had shared with their prospective student that “I’m really excited about that [topic], and it overlaps with my own research in historical trauma with native populations.”
Personalized Support. Participants indicated personalized support was crucial to recruiting diverse students to their CES doctoral program. One participant reported that most of the diverse students who chose to attend their doctoral program typically shared the same response when asked about their choice: “Their comments are consistent. . . . They say, ‘We came and interviewed, and we met you, and we met the students, and we feel cared about.’”
Faculty Involvement. Third, faculty involvement was an essential component of proactive and intentional efforts. Faculty involvement seemed to take a variety of forms: (a) activities related to promoting multiculturalism and social justice, (b) engagement in diverse areas of the profession and representing the program well, and (c) advocating to connect potential students to external funding resources or professional opportunities. One participant explained faculty involvement this way: “An anchor person who strongly identifies not only with their own diversity, but also with a body of scholarship related to diversity.” Another participant shared, “Our faculty have had some nice engagements with organizations and research strands focused on multiculturalism and social justice issues.” These types of involvement made an impact on the impressions of prospective students from diverse backgrounds: “We have students who came to us and said, ‘I looked at the work your faculty were doing, I looked at what they said was important on the website, and it struck a chord with me.’”
Support and Retention Strategies
The third major category of support and retention strategies was characterized as responding to awareness and understanding of diverse students’ perspectives, experiences, and needs while enrolled in the doctoral program. Participants reported that faculty engaged in proactive and intentional efforts that integrated considerations for cultural identity, personalized support, and faculty involvement.
Awareness and Understanding
As with recruitment, participants reported that successful retention and support of enrolled doctoral students integrated considerations for the students’ cultural identity as well as values, needs, and interests that are a part of that identity. One participant described exploring missing aspects of each student’s experience for the purpose of providing effective support: “It’s super important on a very regular basis to sit down with students of color specifically and talk with them about what they’re not getting . . . those conversations really are key.” Often, these personalized conversations are part of a healthy, intentional mentoring relationship in which students are purposely paired with faculty who can understand their experience, support them in navigating professional organizations, and foster success in the program and in their future career. Two participants added that an effective support strategy involves reaching out and engaging in regular conversations about student struggles and experience with microaggressions, tokenism, or other socioemotional matters.
Some participants reported that diverse students may be lacking in foundational skills and knowledge that put them at a disadvantage in the doctoral program, such as deficits in research competence. Personal conversations between mentors and protégés include being “willing to have difficult conversations about skill deficits” in a manner that encourages and empowers diverse students to succeed.
Proactive and Intentional Efforts
Successful education of diverse doctoral students is a mission that requires thoughtful, intentional, and proactive efforts on the part of doctoral faculty. A participant whose program had a good track record in recruiting diverse students explained, “Proactive efforts take a lot of thought” and aiming for effective retention necessitates “an intentional effort, and that’s what it takes to provide comfort for a more diverse group of students.” For many participants in the study, showing intentionality started with provision of financial support in the form of scholarships, fellowships, and graduate assistantships. Doctoral faculty also advocated for students by connecting them to funding sources because financial support “is the best predictor of keeping people in the program.”
Connection to Cultural Identity. Proactive and intentional efforts were considered to be a step beyond planning, in that doctoral faculty commit tangible and intangible resources along with taking actions toward promoting diversity in the program. In addition to inquiring about the missing aspects of their identity in the program, participants reported that ongoing conversations about cultural identity during the students’ program of study was important to support and retention. For example, some students chose a doctoral program to pursue a specific line of research connected with cultural identity and wanted their faculty members to make intentional efforts to help them further their line of inquiry related to cultural issues.
Personalized Support. Participants reported that personalized support was a critical strategy in helping culturally diverse doctoral students to thrive in the program. Participants believed that supportive faculty–student relationships had a strong impact on retention. As articulated by one participant, “One of our strengths is the relationship that we have with our students . . . it may be making the difference in the students that we keep.” Participants also used a buddy system whereby each student applicant was paired with a current doctoral student as their go-to person for any questions or concerns, to help them transition into the program.
Faculty Involvement. Embracing diversity is a proactive and intentional business, which translated to participants purposefully and thoughtfully changing the way they interact with prospective and current students from diverse backgrounds. Participants reported that diverse students may need more availability and outreach from faculty. As one participant stated, “We try to be available to them when they’ve got concerns that they need to address. We’re always trying to reach out more and being more proactive.” This proactive responsiveness and intentional mentoring seemed particularly important with regard to helping diverse students with professional identity development. One participant reflected that “some students coming from diverse backgrounds are going to need to be socialized into the profession, to make them comfortable in that identity.” Elaborating further, this participant said that, “this requires a lot of very intentional mentoring” and included formal as well as informal activities. For example, they said, “Even having them come to conferences, to introduce them to people. Having meals with them. Modeling how you interact with colleagues. Making sure they go to luncheons . . . to dinners.”
Discussion
In this study, 15 counselor educator participants gave voice to strategies that doctoral programs use to recruit, retain, and support underrepresented doctoral students from diverse backgrounds and their perceptions of the level of success these programs have had with their implemented strategies. We examined these experiences and identified two overarching themes of awareness and understanding and proactive and intentional efforts in the way they approached the need to recruit and support diverse doctoral students.
During the process of data analysis, a substantive framework emerged to explain participant strategies that had led to success. Analysis of the participants’ narratives shed light on counselor educators’ awareness and understanding that being proactive and intentional in integrating approaches that connect to the student’s cultural identity, provide personalized support, and involve faculty appear to be successful strategies for recruiting, retaining, and supporting diverse students. These categories reflect a program’s commitment to and demonstration of diversity, with the necessity of intentional and active approaches indicated in literature (Evans & Cokley, 2008; Hipolito-Delgado et al., 2017; McCallum, 2016; Rogers & Molina, 2006). Commitment to diversity has been found to be a highly influential factor in applicants’ decisions to enter a doctoral program (Haizlip, 2012; Zeligman et al., 2015) and once enrolled, for students from URM backgrounds to feel a sense of inclusion, connection, and belonging (Henfield et al., 2013; Hollingsworth & Fassinger, 2002; Protivnak & Foss, 2009).
The literature has indicated that a program’s commitment and intentionality about increasing the diversity of both students and faculty has a direct impact on the number of applicants received by that program (Zeligman et al., 2015). Participant narratives from this study supported this strategy. Diverse students are drawn to programs that value their cultural background and the research interests that come with that identity. This might mean presence of diverse faculty and student body, being encouraged to express their uniqueness, and having faculty who share their research interests. The unique needs, values, and interests of diverse students require CES faculty to be mindful of providing personalized support during the recruitment process as well as during their enrollment in the program. These can be in the form of intentional mentoring, support in addressing possible skills deficits, having personalized conversations, and engaging in a buddy system. A third essential strategy is faculty involvement in multiculturalism and social justice issues, engagement in diverse areas of the profession, and advocating for students academically, professionally, and socioeconomically.
Implications for Counselor Education
The findings from this study reveal the need for a change on the part of some CES doctoral programs in developing intentional and proactive efforts to recruit, support, and retain students from culturally diverse backgrounds. In this study, several participants noted that their doctoral program employed passive recruiting and retention strategies, which appeared to be inadequate and contrary to CACREP standards. Some participants also highlighted barriers to both recruiting and retaining diverse doctoral students, such as unclear standards and faculty attitudes and behaviors that include complacency, defensiveness and dismissiveness, lack of awareness, and assumptive thinking about diversity. Other CES departments seem to be partially implementing a comprehensive and systematic plan for recruiting and retaining diverse students. For example, they may utilize alumni networks to help with recruiting diverse students but lack a plan to support and retain enrolled students.
An important potential barrier for supporting diverse students in CES doctoral programs is the time required for faculty mentorship. Some participants in the study reported that some diverse students needed more close mentoring, and this time commitment would likely reduce available time for other faculty activities such as conducting research and writing for publication. For faculty on the tenure-track system in research institutions, losing time to research endeavors poses a potential threat to career advancement. One participant shared that while “by and large, most faculty want to mentor diverse students and put the time in,” this time commitment stood in opposition to their own tenure and promotion process. This participant elaborated that the pressure to “publish or perish” can “somewhat alter career trajectory for the faculty, if they spend too much time in mentoring.” This participant believed that this issue was “one of the real tensions here in academia” and explained that “either you want diversity, and you’re willing to reward people who are willing to invest themselves in the diversity . . . or you’re not. But you can’t have it both ways.” It appears that the current structure within universities, such as the criteria for tenure and promotion, can present a significant barrier to supporting diverse students. Prior authors have noted that established university and program culture can create a sense of marginalization for diverse students, making it difficult to both recruit and retain URM doctoral students (Holcomb-McCoy & Bradley, 2003; Zeligman et al., 2015). Faculty may need to advocate for structural changes within their universities to ensure that their students are adequately supported. Some participants in the study indicated that low teaching loads were another avenue of freeing up time for mentoring.
The CACREP standards (2015) contain a mandate for systematic and continuous efforts to retain a diversified student body in counselor education programs. Some participants noted in this study that the actual appraisal by CACREP site visit teams of how this standard was being met was unclear. Confusion about this standard may result in not having a strategy for ensuring that the standard was being met. Clarification and accountability are necessary to ensure that programs are meeting this standard.
It is crucial that counselor education programs continue to develop specific strategies to both recruit and retain underrepresented doctoral students. It is no longer acceptable to rest on the institutional name or location. Intentionality that addresses the needs of underrepresented students should include connection to students’ cultural identity, personalized support, and faculty involvement, as these will ensure that students feel wanted and valued throughout the entire process (recruitment to completion).
Limitations
Although grounded theory provides a richness and depth to understanding questions for research, it comes with potential limitations. Clarke (2005) discussed limitations typical in qualitative research and grounded theory. Researchers are faced with an overwhelming amount of information to code, categorize, and analyze. Qualitative researchers can quite easily get bogged down with the complexity and amount of data, which can lead to a diluting of results (Clarke, 2005). The research team addressed this challenge by engaging in a two-step coding process: engaging in group coding of the first three transcripts and then dyadic coding of the remaining transcripts. Through saturation, the research team was able to establish categories that captured the main themes and ideas of the participant statements and check their own biases and values as potentially impacting the interpretation of the codes.
The research team was composed of members who themselves are from diverse backgrounds and who had experiences as doctoral students in CES programs. In addition, all members of the research team currently work in counselor training programs and wrestle with the same questions under review—namely, how to recruit, support, and retain diverse students. The research team attempted to address limitations through developing a priori codes potentially rooted in their own experiences and through recording memos during each group and individual coding session to capture the presence of personal values, biases, or experiences, as well as checking other team members’ codes. Although it is impossible to fully account for all potential biases present in a qualitative analysis, these efforts of diligently checking experiences aimed to mitigate this impact on the overall results and conclusions of the study.
Although the coding team believed that data reached saturation at 15 interviews, the sample was small (N = 15) for the method of inquiry according to Creswell and Poth (2018). Although we believe that limiting the number of respondents to no more than one faculty member per program was helpful in reducing the potential for bias due to group effect, it is possible that the faculty members surveyed were not the sole representations of their counselor education program. As with many qualitative studies, generalizability to the larger population is limited. However, it is noteworthy that the demographics of the participants in the current study do align with typical cultural representation of counselor education programs (CACREP, 2018).
Future quantitative studies are needed to evaluate the size of the effect of these strategies on recruitment and retention rates of diverse students in CES doctoral programs. For example, future studies could evaluate the relationship between student perceptions of proactive and intentional efforts toward connecting with cultural identity, personalized support, and faculty involvement with actual retention rates of diverse students in CES programs and their overall student satisfaction. Such information would be helpful to decipher which of these factors has the greatest impact on recruiting, retaining, and supporting diverse students in CES doctoral programs, which would be useful information for current CES doctoral programs.
Conclusion
This study highlights that although more efforts to recruit and retain students from diverse backgrounds are needed, when counselor education programs are intentional and proactive, it has a meaningful impact. What seems to be effective in recruiting, retaining, and supporting diverse students is developing a connection to cultural identity, support that is personalized, and faculty involvement. When students from diverse backgrounds feel some connection to their specific cultural identity and receive personalized support, they are more likely to enter a program and persist. Finally, the involvement of faculty at all levels of the recruitment and retention process is monumental. Students from diverse backgrounds perceive counselor education programs as inviting and able to meet their cultural needs when programming is intentional and proactive.
Conflict of Interest and Funding Disclosure
The authors reported no conflict of interest
or funding contributions for the development
of this manuscript.
References
Baker, C. A., & Moore, J. L., III. (2015). Experiences of underrepresented doctoral students in counselor education. Journal for Multicultural Education, 9(2), 68–84. https://doi.org/10.1108/JME-11-2014-0036
Barker, M. J. (2016). The doctorate in black and white: Exploring the engagement of Black doctoral students in cross race advising relationships with White faculty. Western Journal of Black Studies, 40(2), 126–140.
Behl, M., Laux, J. M., Roseman, C. P., Tiamiyu, M., & Spann, S. (2017). Needs and acculturative stress of international students in CACREP programs. Counselor Education and Supervision, 56(4), 305–318.
https://doi.org/10.1002/ceas.12087
Blackwell, J. E. (1987). Mainstreaming outsiders: The production of Black professionals (2nd ed.). Rowman & Littlefield.
Blockett, R. A., Felder, P. P., Parrish, W., III, & Collier, J. N. (2016). Pathways to the professoriate: Exploring Black doctoral student socialization and the pipeline to the academic profession. The Western Journal of Black Studies, 40(2), 95–110.
Brown, E. M., & Grothaus, T. (2019). Experiences of cross-racial trust in mentoring relationships between Black doctoral counseling students and White counselor educators and supervisors. The Professional Counselor, 9(3), 211–225. https://doi.org/10.15241/emb.9.3.211
The Carnegie Classification of Institutions of Higher Education. (2019). Basic classification description. http://carn
egieclassifications.iu.edu/classification_descriptions/basic.php
Castellanos, J., Gloria, A. M., & Kamimura, M. (Eds.). (2006). The Latina/o pathways to the Ph.D.: Abriendo caminos. Stylus.
Chan, A. W., Yeh, C. J., & Krumboltz, J. D. (2015). Mentoring ethnic minority counseling and clinical psychology students: A multicultural, ecological, and relational model. Journal of Counseling Psychology, 62(4), 592–607. https://doi.org/10.1037/cou0000079
Charmaz, K. (2014). Constructing grounded theory (2nd ed.). SAGE.
Chen, S. Y., Basma, D., Ju, J., & Ng, K.-M. (2020). Opportunities and challenges of multicultural and international online education. The Professional Counselor, 10(1), 120–132. https://doi.org/10.15241/syc.10.1.120
Clarke, A. E. (2005). Situational analysis: Grounded theory after the postmodern turn. SAGE.
Corbin, J., & Strauss, A. (2015). Basics of qualitative research: Techniques and procedures for developing grounded theory (4th ed.). SAGE.
Council for Accreditation of Counseling and Related Educational Programs. (2014). CACREP vital statistics 2013: Results from a national survey of accredited programs. http://www.cacrep.org/wp-content/uploads/20
19/05/2013-CACREP-Vital-Statistics-Report.pdf
Council for Accreditation of Counseling and Related Educational Programs. (2015). CACREP standards 2016. https://www.cacrep.org/for-programs/2016-cacrep-standards
Council for Accreditation of Counseling and Related Educational Programs. (2016). CACREP vital statistics 2015: Results from a national survey of accredited programs. http://www.cacrep.org/wp-content/uploads/20
19/05/2015-CACREP-Vital-Statistics-Report.pdf
Council for Accreditation of Counseling and Related Educational Programs. (2018). CACREP vital statistics 2017: Results from a national survey of accredited programs. http://www.cacrep.org/wp-content/uploads/20
19/05/2017-CACREP-Vital-Statistics-Report.pdf
Council for Accreditation of Counseling and Related Educational Programs. (2019). Annual report 2018. https://www.cacrep.org/wp-content/uploads/2019/05/CACREP-2018-Annual-Report.pdf
Creswell, J. W., Hanson, W. E., Plano, V. L. C., & Morales, A. (2007). Qualitative research designs: Selection and implementation. The Counseling Psychologist, 35(2), 236–264. https://doi.org/10.1177/0011000006287390
Creswell, J. W., & Poth, C. N. (2018). Qualitative inquiry and research design: Choosing among five approaches (4th ed.). SAGE.
Definitions, 20 U.S.C. 20 § 1067k (2020). November 2, 2019. https://uscode.house.gov/view.xhtml?req=granuleid
:USC-prelim-title20-section1067k&num=0&edition=prelim
Dieker, L., Wienke, W., Straub, C., & Finnegan, L. (2013). Reflections on recruiting, supporting, retaining, graduating, and obtaining employment for doctoral students from diverse backgrounds. Teacher Education and Special Education, 37(2), 147–160. https://doi.org/10.1177/0888406413505874
Evans, G. L., & Cokley, K. O. (2008). African American women and the academy: Using career mentoring to increase research productivity. Training and Education in Professional Psychology, 2(1), 50–57.
https://doi.org/10.1037/1931-3918.2.1.50
Foxx, S. P., Kennedy, S. D., Dameron, M. L., & Bryant, A. (2018). A phenomenological exploration of diversity in counselor education. Journal of Professional Counseling: Practice, Theory & Research, 45(1), 17–32.
https://doi.org/10.1080/15566382.2019.1569320
González, J. C. (2006). Academic socialization experiences of Latina doctoral students: A qualitative understanding of support systems that aid and challenges that hinder the process. Journal of Hispanic Higher Education, 5(4), 347–365. https://doi.org/10.1177/1538192706291141
Goodman, R. D., Williams, J. M., Chung, R. C.-Y., Talleyrand, R. M., Douglass, A. M., McMahon, H. G., & Bemak, F. (2015). Decolonizing traditional pedagogies and practices in counseling and psychology education: A move towards social justice and action. In R. D. Goodman & P. C. Gorski (Eds.), Decolonizing “multicultural” counseling through social justice (pp. 147–164). Springer.
Grapin, S. L., Bocanegra, J. O., Green, T. D., Lee, E. T., & Jaafar, D. (2016). Increasing diversity in school psychology: Uniting the efforts of institutions, faculty, students, and practitioners. Contemporary School Psychology, 20(4), 345–355. https://doi.org/10.1007/s40688-016-0092-z
Guillory, R. M. (2009). American Indian/Alaska Native college student retention strategies. Journal of Developmental Education, 33(2), 14–16, 18, 20, 22–23, 40. https://files.eric.ed.gov/fulltext/EJ897631.pdf
Haizlip, B. N. (2012). Addressing the underrepresentation of African-Americans in counseling and psychology programs. College Student Journal, 46(1), 214–222.
Henfield, M. S., Owens, D., & Witherspoon, S. (2011). African American students in counselor education programs: Perceptions of their experiences. Counselor Education and Supervision, 50(4), 226–242.
https://doi.org/10.1002/j.1556-6978.2011.tb00121.x
Henfield, M. S., Woo, H., & Washington, A. (2013). A phenomenological investigation of African American counselor education students’ challenging experiences. Counselor Education and Supervision, 52(2), 122–136. https://doi.org/10.1002/j.1556-6978.2013.00033.x
Hinojosa, T. J., & Carney, J. V. (2016). Mexican American women pursuing counselor education doctorates: A narrative inquiry. Counselor Education and Supervision, 55(3), 198–215. https://doi.org/10.1002/ceas.12045
Hipolito-Delgado, C. P., Estrada, D., & Garcia, M. (2017). Counselor education in technicolor: Recruiting graduate students of color. Interamerican Journal of Psychology, 51(1), 73–85.
https://doi.org/10.30849/RIP/IJP.V51I1.293
Holcomb-McCoy, C., & Bradley, C. (2003). Recruitment and retention of ethnic minority counselor educators: An exploratory study of CACREP-accredited counseling programs. Counselor Education and Supervision, 42(3), 231–243. https://doi.org/10.1002/j.1556-6978.2003.tb01814.x
Hollingsworth, M. A., & Fassinger, R. E. (2002). The role of faculty mentors in the research training of counseling psychology doctoral students. Journal of Counseling Psychology, 49(3), 324–330.
https://doi.org/10.1037/0022-0167.49.3.324
Interiano, C. G., & Lim, J. H. (2018). A “chameleonic” identity: Foreign-born doctoral students in U.S. counselor education. International Journal for the Advancement of Counselling, 40, 310–325.
https://doi.org/10.1007/s10447-018-9328-0
Lerma, E., Zamarripa, M. X., Oliver, M., & Vela, J. C. (2015). Making our way through: Voices of Hispanic counselor educators. Counselor Education and Supervision, 54(3), 162–175. https://doi.org/10.1002/ceas.12011
Lewis, C. W., Ginsberg, R., Davies, T., & Smith, K. (2004). The experiences of African American Ph.D. students at a predominately White Carnegie I-research institution. College Student Journal, 38(2), 231–245.
Lincoln, Y. S., & Guba, E. G. (2013). The constructivist credo. Left Coast Press, Inc.
Luedke, C. L., Collom, G. D., McCoy, D. L., Lee-Johnson, J., & Winkle-Wagner, R. (2019). Connecting identity with research: Socializing students of color towards seeing themselves as scholars. The Review of Higher Education, 42(4), 1527–1547. https://doi.org/10.1353/rhe.2019.0074
Marsella, A. J., & Pedersen, P. (2004). Internationalizing the counseling psychology curriculum: Toward new values, competencies, and directions. Counselling Psychology Quarterly, 17(4), 413–423.
https://doi.org/10.1080/09515070412331331246
McCallum, C. M. (2015). Turning graduate school aspirations into enrollment: How student affairs professionals can help African American students. New York Journal of Student Affairs, 15(1), 1–18. https://journals.canisius.edu/index.php/CSPANY/article/view/448/717
McCallum, C. M. (2016). “Mom made me do it”: The role of family in African Americans’ decisions to enroll in doctoral education. Journal of Diversity in Higher Education, 9(1), 50–63. https://doi.org/10.1037/a0039158
Merriam, S. B., & Tisdell, E. J. (2016). Qualitative research: A guide to design and implementation (4th ed.). Wiley.
Ng, K.-M. (2006). Counselor educators’ perceptions of and experiences with international students. International Journal for the Advancement of Counseling, 28(1), 1–19. https://doi.org/10.1007/s10447-005-8492-1
Ng, K.-M., & Smith, S. D. (2009). Perceptions and experiences of international trainees in counseling and related programs. International Journal for the Advancement of Counselling, 31, 57–70.
https://doi.org/10.1007/s10447-008-9068-7
Patton, M. Q. (2014). Qualitative research and evaluation methods: Integrating theory and practice (4th ed.). SAGE.
Ponjuan, L. (2011). Recruiting and retaining Latino faculty members: The missing piece to Latino student success. Thought & Action, 99–110. https://vtechworks.lib.vt.edu/bitstream/handle/10919/84034/Recruit
ingLatinoFacultyMembers.pdf?sequence=1&isAllowed=y
Ponterotto, J. G. (2005). Qualitative research in counseling psychology: A primer on research paradigms and philosophy of science. Journal of Counseling Psychology, 52(2), 126–136. https://doi.org/10.1037/0022-0167.52.2.126
Preston, J., Trepal, T., Morgan, A., Jacques, J., Smith, J., & Field, T. (2020). Components of a high-quality doctoral program in counselor education and supervision. The Professional Counselor, 10(4), 453–471. https://doi.org/10.15241/jp.10.4.453
Proctor, S. L., & Romano, M. (2016). School psychology recruitment research characteristics and
implications for increasing racial and ethnic diversity. School Psychology Quarterly, 31(3), 311–326. https://doi.org/10.1037/spq0000154
Protivnak, J. J., & Foss, L. L. (2009). An exploration of themes that influence the counselor education doctoral student experience. Counselor Education and Supervision, 48(4), 239–256.
https://doi.org/10.1002/j.1556-6978.2009.tb00078.x
Rogers, M. R., & Molina, L. E. (2006). Exemplary efforts in psychology to recruit and retain graduate students of color. American Psychologist, 61(2), 143–156. https://doi.org/10.1037/0003-066X.61.2.143
Strauss, A., & Corbin, J. (1998). Basics of qualitative research: Techniques and procedures for developing grounded theory (2nd ed.). SAGE.
Woo, H., Jang, Y. J., & Henfield, M. (2015). International doctoral students in counselor education: Coping strategies in supervision training. Journal of Multicultural Counseling and Development, 43(4), 288–304. https://doi.org/10.1002/jmcd.12022
Zeligman, M., Prescod, D. J., & Greene, J. H. (2015). Journey toward becoming a counselor education doctoral student: Perspectives of women of color. The Journal of Negro Education, 84(1), 66–79.
https://doi.org/10.7709/jnegroeducation.84.1.0066
The authors present this article in memory of Dr. Rose Merrell-James, who shared her knowledge, experience, strength, and wisdom with all of us through this scholarly work.
Jennie Ju, PhD, LPC, is an assistant professor at Palo Alto University. Rose Merrell-James was an assistant professor at Shippensburg University. J. Kelly Coker, PhD, MBA, NCC, BC-TMH, LCMHC, is a professor and program director at Palo Alto University. Michelle Ghoston, PhD, ACS, LPC(VA), LCMHC, is an assistant professor at Wake Forest University. Javier F. Casado Pérez, PhD, NCC, LPC, CCTP, is an assistant professor at Portland State University. Thomas A. Field, PhD, NCC, CCMHC, ACS, LPC, LMHC, is an assistant professor at the Boston University School of Medicine. Correspondence may be addressed to Jennie Ju, 1791 Arastradero Road, Palo Alto, CA 94304, jju@paloaltou.edu.
Appendix A
Interview Protocol
For context, please briefly describe how you self-identify and your background. This information will be aggregated; individual participant responses will not be associated with any quotes in subsequent manuscripts.
Gender:
Sexual/Affective Orientation:
Race and Ethnicity:
Years as a Faculty Member in a Counselor Education Program:
Years as a Faculty Member in a Doctoral Counselor Education Program:
Number of Doctoral Counselor Education Programs You Have Worked In:
Regions of Doctoral Counselor Education Programs You’ve Worked In (using regions
commonly defined by national counselor education associations and organizations):
How might you define a “high-quality” doctoral program?
What do you believe to be the most important components? The least important?
How have you helped students to successfully navigate the dissertation process?
Which strategies has your program used to recruit underrepresented students from diverse
backgrounds? How successful were those?
Which strategies has your program used to support and retain underrepresented students from diverse
backgrounds? How successful were those?
What guidance might you provide to faculty who want to start a new doctoral program in counseling
with regards to working with administrators and gaining buy-in?
What guidance might you provide to faculty who want to sustain an existing doctoral program in
counseling with regards to working with administrators and gaining ongoing support?
Last question. What other pieces of information would you like to share about running a successful,
high-quality doctoral program?
Dec 16, 2020 | Volume 10 - Issue 4
Susan F. Branco, Melonie Davis
In 2012, the Substance Abuse and Mental Health Services Administration awarded funding for the Minority Fellowship Program (MFP) to be managed by the National Board for Certified Counselors (NBCC) Foundation. The MFP aims to increase representation of minoritized students enrolled in counselor education and supervision doctoral programs accredited by the Council for Accreditation of Counseling and Related Educational Programs (CACREP). From 2012 to 2018, the NBCC MFP has disseminated 20–24 monetary fellowships each year. This article reviews representation within counselor education, offers a history of the MFP, provides doctoral fellowship recipient outcome data, and concludes with implications for counselor education.
Keywords: Minority Fellowship Program, counselor education and supervision, National Board for Certified Counselors Foundation, CACREP, representation
In August 2012, the Substance Abuse and Mental Health Services Administration (SAMHSA) awarded $1.6 million to the National Board for Certified Counselors Foundation (NBCCF) to oversee the Minority Fellowship Program (MFP) for underrepresented, minoritized students in doctoral counselor education and supervision (CES) programs (Shallcross, 2012). The groundbreaking award for the counseling profession aimed to increase minoritized student representation in CES doctoral programs accredited by the Council for Accreditation of Counseling and Related Educational Programs (CACREP). It is important to note that NBCC now also offers MFP master’s-level fellowships for those students committed to collaborating with underrepresented and minoritized populations (NBCCF, n.d.). The goal of this article is to review the status of underrepresented racially and ethnically diverse faculty within counselor education, describe the doctoral MFP, and share the grant outcome data from its inception in 2012 through 2019.
Underrepresentation in CES
Diverse racial and ethnic representation within counselor education impacts recruitment and retention of master’s- and doctoral-level students of color (Henfield et al., 2013), perceived quality and content of course instruction to promote diverse perspectives (Seward, 2014), and preparation for graduates to work with diverse client populations (SAMHSA, 2020). Further, the ACA Code of Ethics (American Counseling Association [ACA], 2014) mandates that “counselor educators are committed to recruiting and retaining a diverse faculty” (F.11.a, p. 15). Similarly, CACREP (2015) requires that counselor education programs seek to recruit and retain both diverse faculty and students. Although representation of faculty of color in counselor education has increased (Baggerly et al., 2017), the majority of counselor educators are White (71.38%), with 14.52% Black, 4.77% Latinx, 4.03% Asian American, and 0.7% Native American (CACREP, 2018).
Gains made in ethnic and racial diversity among counselor education faculty and their subsequent experiences have shed light on oppressive factors that impact minoritized faculty members’ success. Spanierman and Smith (2017) urged ACA and the American Psychological Association to initiate a closer examination of how White hegemonic practices can be dismantled within their profession and training programs. Research has documented the experiences of faculty of color with microaggressions and disappointment in the counselor education profession during the on-campus interview process (Cartwright et al., 2018) and throughout the tenure and promotion academic journey, including experiencing isolation as a faculty member of color (Pérez & Carney, 2018). Other studies of female faculty of color in counselor education have illuminated the professional and personal strain experienced as they navigate a system traditionally built for White male faculty (Haskins et al., 2016; Shillingford et al., 2013).
However, despite the documented challenges for counselor educators of color, research also has highlighted factors that support their success and resilience in the academy. Cartwright et al. (2018) recommended that counselor education programs seek to understand the mentorship experiences of students of color in order to bolster retention. Henfield et al. (2013) and Spanierman and Smith (2017) echoed support for ongoing mentorship for students of color by faculty of color and intentionally recruiting and retaining faculty and students of color. Likewise, Pérez and Carney (2018) supported developing mentorship for new faculty of color as well as concerted preparation tailored for doctoral students of color to enter the academy. Lerma et al. (2015) additionally proposed the promotion of bicultural flexibility for faculty of color, which includes encouraging maintaining family ties as well as creating academic family support systems to include mentors, advisors, and allies. Next, a review of the MFP will be presented with focus on its incorporation into CACREP-accredited CES doctoral programs.
The Minority Fellowship Program (MFP)
SAMHSA commenced the MFP in 1973 in an effort to increase the number of ethnically and racially diverse, doctoral-level mental health practitioners to serve minoritized communities (SAMHSA, 2020). Currently, the SAMHSA (2020) MFP website notes that although racial and ethnic minority populations account for approximately 28% of the population, only 20% or less of the behavioral health care workforce includes those who identify as ethnically or racially minoritized individuals. Hence, the MFP also aims to reduce mental health disparities with regard to quality of service and access to behavioral health care (SAMHSA, 2020). J. M. Jones and Austin-Daily (2009) described the inception of the MFP as born from the advocacy of a group of Black psychiatrists. They reported that the initial MFP grant funding was distributed to ten doctoral-level minoritized psychology students led by an inaugural MFP Advisory Committee composed of prominent minoritized psychologists. Eventually, SAMHSA awarded MFP grant funding to additional mental health disciplines, including the American Nurses Association, the American Psychiatric Association, the Council on Social Work Education, and the American Association for Marriage and Family Therapy (Shallcross, 2012).
The counseling profession was notably absent from the MFP grant awardee list until 2012, when the U.S. Congress approved the funding to include professional counselors (Shallcross, 2012). At the time, NBCC was awarded a $1.6 million grant to initiate and oversee the MFP for doctoral-level CES students. Then–NBCC President and CEO Thomas Clawson stated:
The NBCC Minority Fellowship Program will strategically promote and provide fellowships to doctoral students in the counseling profession. The fellows will obtain training in mental health and substance abuse, with specialty training in culturally competent service delivery. Fellows will provide leadership to the profession through education, research and practice benefiting vulnerable underserved consumers. The fellowship program will increase system capacity by increasing the number of culturally competent professional counselors available to underserved populations through engaging 24 doctoral fellows per year, by promoting national standards in culturally competent care and by providing online and conference-based training to practicing professional counselors. We like to project this yearly number over a decade to imagine more than 200 doctoral-level counselors and counselor educators being added to our ranks. (as cited in Shallcross, 2012, para. 8)
The inaugural NBCC MFP awarded 24 fellowships to doctoral students enrolled in CACREP-accredited CES programs (NBCCF, 2014). From 2013 to 2018, NBCC MFP doctoral-level fellowships were awarded to 138 students (NBCCF, 2018). Table 1 offers a demographic breakdown of doctoral-level NBCC MFP recipients.
Table 1
MFP Demographic Information from 2013–2018
| Year |
Number of Fellowships Awarded |
Female |
Male |
Other |
Racial Category
AA W H AI A/PI MR |
Doctoral Completion |
Post-Doctoral Employment
CE Clinical |
| 2013 |
24 |
17 |
7 |
|
17 |
2 |
5 |
– |
– |
– |
100% |
– |
| 2014 |
22 |
15 |
7 |
|
10 |
5 |
4 |
1 |
1 |
1 |
100% |
1 2 |
| 2015 |
23 |
20 |
3 |
|
18 |
– |
2 |
1 |
1 |
1 |
100% |
7 2 |
| 2016 |
23 |
19 |
4 |
|
9 |
3 |
6 |
1 |
2 |
2 |
IP |
6 2 |
| 2017 |
23 |
19 |
4 |
|
12 |
5 |
1 |
2 |
2 |
1 |
IP |
2 2 |
| 2018 |
23 |
19 |
3 |
1 |
15 |
5 |
– |
– |
3 |
– |
IP |
2 2 |
| 2019 |
20 |
13 |
7 |
|
10 |
4 |
5 |
– |
1 |
– |
IP |
– |
| Total |
158 |
122 |
35 |
1 |
91 |
24 |
23 |
5 |
10 |
5 |
|
18 10 |
Note. The U.S. Census defines racial categorization based on identifying with “original peoples” of designated racial group (N. A. Jones & Bullock, 2012, p. 2): African American (AA), White (W), Hispanic/Latinx (H), American Indian (AI), Asian/Pacific Islander (A/PI), and Multi-Racial (MR). IP = degree completion in progress; CE = counselor education.
NBCC MFP Structure
Applications for the doctoral MFP are reviewed by NBCCF volunteers, many of whom are NBCC MFP alumni (NBCCF, 2019). Applicants must demonstrate a strong commitment to working with underserved and marginalized populations—including those who identify as racially, ethnically, and culturally diverse as well as members of the LGBTQIA population—after completion of their CES doctoral degree. Final applicant decisions are made by the MFP Advisory Council, composed of six counselors and/or counselor educators who represent diverse ethnic, racial, or linguistic backgrounds and have extensive experience “providing mental health counseling services to underserved racial and ethnic minority communities” (NBCCF, 2019, p. 63). Before MFP awards are conferred, finalists must agree and attest to the terms of the MFP: (a) documentation of enrollment in a CACREP-accredited program, (b) attendance at required MFP orientation and relevant training, and (c) continued and ongoing collaboration with underserved and marginalized clients or students within counselor education (NBCCF, 2019).
Individual Fellowship Plan. NBCC MFP staff work with each individual fellow to craft an Individual Fellowship Plan (IFP) in which educational and impact goals for the fellow’s targeted underserved community are created with the goal of completion during the fellowship year (NBCCF, 2019). Goals must have a stated benefit for or impact on the underserved or marginalized community with whom the MFP fellow is working and must also demonstrate an educational impact for the MFP fellow. Progress toward IFP goals are tracked by MFP staff and in collaboration with assigned mentors throughout the fellowship year in order to provide the necessary resources and support (NBCCF, 2019).
Mentors. MFP fellows are paired with volunteer mentors, many of whom are MFP alumni themselves and/or serve as counselor educators and practicing counselors (NBCCF, 2019). Mentorship occurs throughout the fellowship year in an effort to provide support and guidance for fellows as they navigate completion of their IFP, journey through the CES doctoral program, and consider professional careers (NBCCF, 2019). Mentors and mentees determine mutually agreed-upon goals, meeting times, and frequency, and establish the boundaries of the relationship for the fellowship.
Webinars and Trainings. All MFP fellows attend a minimum of six live or recorded webinars offered by NBCCF in their webinar series Innovations in Counseling: Working with Minority Populations and Building Professional Excellence (NBCCF, 2019). Training opportunities, such as attendance at the ACA or Association for Counselor Education and Supervision national or regional conferences promote fellows’ educational and professional IFP goals. The fellowship year culminates in the annual Bridging the Gap Symposium on Eliminating Mental Health Disparities where “counselors, counselor educators, and counselors-in-training come together from around the country to focus on the provision of mental health care for underserved minority, military, rural, and marginalized groups” (NBCCF, 2019, p. 58).
NBCC has awarded MFP fellowships to seven doctoral cohorts since 2013. Many MFP fellows have graduated from their doctoral programs and entered the counseling profession as advanced practitioners, supervisors, and counselor educators. However, a comprehensive description of outcome information from all the cohorts has not been undertaken. Therefore, we aimed to collate MFP data gleaned from awardee demographic information and annual surveys completed by the fellowship cohort members.
Method
In order to access the NBCC MFP cohort data for our analysis, we sought permission from the NBCC MFP administrators. Because our analysis utilized previously collected data by the NBCC MFP administrators and would not divulge protected health information, the project was deemed to be “not human research” by the first author’s institutional office of the IRB. Therefore, IRB approval was not warranted.
We aimed to collate the descriptive statistics gleaned from demographic data captured from applications of those doctoral students awarded the fellowship. We also culled qualitative responses from surveys distributed to NBCC MFP doctoral fellows during their fellowship year and 1 year after fellowship completion. The survey created by members of the NBCCF staff overseeing the MFP was developed to meet SAMHSA’s reporting criteria for MFP grant recipients. The survey consisted of 39 questions and included nine open-ended questions, allowing for short answers from the survey recipients. We aimed to analyze responses to only one of the survey questions—“In what ways has this scholarship or fellowship been meaningful to you?”—as we believed responses would offer a broad range of fellow experiences. In total, surveys were distributed to 158 active and alumni fellows.
Sample
Surveys were distributed once per quarter, or four times, throughout the fellowship year to active MFP fellows. Alumni fellows who had completed their fellowship year received the survey in June. All surveys were distributed via electronic correspondence using the email on record for each fellow. During the MFP orientation, all fellows were instructed to complete the end-of-fellowship survey as a condition to acceptance of the NBCC MFP enrollment. The demographic and doctoral completion rate data was retrieved from the MFP applications and the surveys captured responses from 54 NBCC MFP cohort members from 2013 through 2018 (Table 1).
Procedure
First, we ensured that all NBCC MFP fellows had previously offered consent for their feedback and participation in the program to be used in a variety of ways including research activities as evidenced in the “Terms and Conditions of Program Participation” (NBCCF, 2019, p. 7). Next, we collated all MFP fellow demographic data using information found in their MFP applications and from the survey responses (Table 1). Surveys were distributed to active fellows four times a year and to alumni fellows once per year in June. In total, the surveys were sent to 158 fellows (both active and alumni).
Authors’ Stance
The first author is a 2014 NBCC MFP cohort doctoral fellow alumna and identifies as a Latinx cisgender woman. She is a licensed professional counselor and is also a clinical assistant professor in a CACREP-accredited master’s in clinical mental health counseling program. The second author identifies as an African American cisgender woman and is a licensed professional counselor associate. She serves as the Professional Development Coordinator for NBCCF. Both consulted frequently with regard to collating the descriptive and qualitative data for the manuscript.
Data Analysis and Trustworthiness
We utilized thematic analysis (Nowell et al., 2017) to categorize the qualitative data culled from one survey question: “In what ways has this scholarship or fellowship been meaningful to you?” Braun and Clarke (2012) suggested that thematic analysis specifically allows for exploration and understanding of “meaning across a data set” to allow the researcher to “see and make sense of collective or shared meanings of experiences” (p. 57). Specifically, we adhered to the following steps in the thematic analytic process.
We familiarized ourselves with the data and read through the entirety of the survey questions and responses multiple times and then separated out the short-answer responses to the survey question of focus. We then reviewed each short answer to the survey question in multiple rounds to absorb the content. We initiated the coding process by way of extracting meaning from the survey response phrases, and we utilized qualitative software to aid in the categorization of codes, ultimately developing an initial codebook. Next, we examined the codes to note patterns of connection in order to group data together to generate themes and subthemes. The categorization was added to the revised codebook. We reviewed the themes, then created and compared the codes to the themes to determine coherence and/or if we needed to recategorize. During this quality review phase, as described by Braun and Clark (2012), we asked ourselves critical questions to ensure that themes were not really codes and if there was enough data in the survey responses to support the themes. Then we defined and named our themes to aid in clarity and included relevant participant quotes from the survey responses to illuminate the themes. Finally, we added our findings to our initially written literature review.
We followed Nowell et al.’s (2017) recommendations to increase trustworthiness within thematic analysis to correspond with previously described analytic steps. We reviewed the survey responses at multiple points in the data gathering process prior to initiating analysis. We then utilized peer debriefing to discuss the coding process and developed an audit trail where we stored the coding iterations within qualitative software. In this step, we used the developed codebooks to organize codes into themes where subthemes emerged. We continued the vetting process of the themes to ensure the codes fit coherently within each theme and subtheme and adjusted the codebook accordingly. Eventually we reached consensus on the final theme and subtheme definitions. Then, we utilized an outside auditor, a counselor educator, who confirmed coherence for the themes, with one recommendation to provide justification for one subtheme, which we addressed. Lastly, during the reporting phase we asked a staff member of NBCCF to read through the manuscript to confirm that the themes aligned with the data presented.
Results
In regard to the survey question, “In what ways has this scholarship or fellowship been meaningful to you?”, the overarching theme of access to the profession emerged, as evidenced by the number of responses highlighting the MFP as the “open door that gave me access.” Within this theme, the subthemes of doctoral program completion, networking, supportive cohort, financial support, and mentorship surfaced. The remaining themes included clinical and multicultural competence, with the subtheme of counselor identity, and paying it forward, with the subtheme of leadership.
Access to the Profession
Survey respondents’ experiences spoke to the overall sentiment of the MFP offering them an opportunity to enter the counseling profession, either as counselor educators or as clinical supervisors. The subthemes in this category described those aspects of the MFP that respondents utilized to gain access to the profession. Many of the responses reflected more than one subtheme.
The first subtheme, doctoral program completion, captures those respondents who indicated the MFP aided in their overall success to complete their studies. Examples included:
- “I achieved my dream of a PhD.”
• “I would not have been able to complete my degree without it. I have made some
lasting relationships.”
• “Helped me graduate.”
• “I was able to finish my doctoral program.”
The following responses demonstrate how several factors supported a successful completion of the CES doctoral program:
- “The fellowship allowed me to complete my PhD and receive extra training to
prepare for my career.”
- “The fellowship helped me complete my program and support my family.”
• “It allowed me to finish my PhD, strengthen my private practice, and get a job as
an assistant professor. This fellowship has been the most meaningful and
beneficial award I’ve ever received.”
The networking subtheme describes how access to other CES doctoral students, professional counselors, and counselor educators benefited fellows’ entrance into the profession. Responses underscored how networking aided the fellows both during and after the fellowship year:
- “I was able to connect with other scholars of color and the resources provided by
the Foundation.”
• “Through the fellowship, I have developed professional and personal
relationships that have resulted in jobs, consultation opportunities, and peer
networks.”
• “Networking has been the key element of the fellowship.”
• “It has provided invaluable contacts and collegial relationships that are
invaluable.”
- “The fellowship was instrumental in making connections with other counselor
educators. We have done presentations at conferences together as well as sharing
our experiences in counselor education. Also, we have shared resources.”
The following responses also merge into the next subtheme related to the benefit of supportive cohort members:
- “I continue to benefit from the fellowship experience through connections with
other fellows and by continuing to plow the ground cleared during the fellowship
experience.”
- “This fellowship has connected me with many leaders in the profession that I
would not have been able to connect with. It has also provided another cohort of
peers to receive support and encouragement from when career challenges become
overwhelming and discouraging.”
The next subtheme, supportive cohort, reflects how the camaraderie, encouragement, and relationships developed with cohort members acted as positive reinforcement throughout the doctoral CES experience. Statements emphasized the respondents’ healthy dependence on the MFP cohort model, in which members may provide motivation and guidance even beyond the fellowship year:
- “My NBCC MFP cohort is my family. I have continued the relationships with
other cohort members, and we share resources with one another as well as
support one another in the work we are doing.”
- “The network of fellows has been my peer group and support system since 2013.”
- “The group has guided me through my dissertation and job search.”
- “The relationships built from the fellowship provided a long-lasting impact in my
professional development.”
The penultimate subtheme, financial support, described how the $20,000 financial grant offered to doctoral-level fellows aided in their ability to successfully complete their CES doctoral education:
- “The fellowship provided a financial opportunity that allowed me to graduate
with less debt. Even more so, it has provided an invaluable professional network.”
- “It has changed my life and my career. Being part of the NBCC family is amazing!
Taking leaps of faith with the money was the best thing I could have ever done.”
- “The NBCC fellowship has meant the world to me because otherwise I would
have been in a significant amount of debt in completing my doctoral studies. In
the last year of the doctoral program, our school did not provide any funding, so
the fellowship brought me to the finish line so that I could initiate my career as a
counselor educator.”
All exemplify MFP fellow statements regarding the benefit of funding toward their doctoral degree. Similar to other subthemes, some respondents identified many areas that crossed subthemes and contributed to their success: “This fellowship has been instrumental in my successful completion of the doctoral program through resources, mentorship, financial support, and a network of professionals.”
Mentorship, the final subtheme in this category, reflects the impact of the mentors supporting fellows through their doctoral journey. Respondents indicated, “It allowed me to get the funding and mentorship needed to successfully graduate and transition into the mental health counseling field,” and “The scholarship was meaningful in providing collegial relationships with others pursuing their PhD, connected me with mentors and provided useful resources.” Mentorship, among other resources, is a core component of the MFP.
Clinical and Multicultural Competence
Survey respondents spoke to the NBCC MFP’s structured training in clinical and multicultural competencies woven within the fellowship year. Some responses included the following:
- “It helped me become more confident about my counseling skills, especially when
working with minority populations.”
- “Assisted me in completing my dissertation and getting the cultural training I
needed.”
- “The fellowship allowed me to intern at the U.S. Department of Education, which
enriched my understanding of services to people with disabilities.”
The annual Bridging the Gap Symposium and its emphasis on mental health inequalities was mentioned in one response: “The [Symposium] networking with other fellows has been valuable. I’ve been able to build upon my education in regard to health care disparities for people of color.”
The subtheme of counselor identity describes survey respondents’ development as counselors within the profession. Examples included, “This fellowship validated my counselor identity because my interest is with minority populations,” and “Expanding my professional development and further defined my counselor identity.”
Paying It Forward
The final theme highlights how NBCC MFP fellow respondents desired to give back to the MFP community via mentorship, application reviews, and/or serving on the MFP Advisory Council. Some statements included:
- “I’ve also been able to give back and mentor others as well as review scholarship/
fellowship proposals. Having those opportunities allowed me to have an
influence on the counseling field.”
- “Further, I have been able to share my experiences as a fellow with my master’s
students and encourage them to apply.”
- “The most meaningful elements of the fellowship have been the increased
professional network and the opportunity to give back to the MFP by working
with NBCCF and new fellows.”
The subtheme of leadership spotlights how the fellowship experience strengthened fellows’ leadership capacities and skills. One example included, “The fellowship has afforded me the opportunity to increase my leadership skills within the counseling profession, as well as provided me with resources and tools to enhance professional networking.” Another respondent encapsulated leadership within their fellowship experience:
I was able to complete my PhD with less financial burden than I had expected. I have made fabulous professional connections with other giants in the field of counseling and cohorts in the fellowship program, which has encouraged my ongoing research and presentation schedule. I have been motivated to give back to my physical community and my academic community because of a newfound sense of responsibility to utilize my degree and skills to their fullest advantage. The fellowship made me realize that my education was much more than a personal and professional milestone, but an opportunity to become a leader and an advocate in the counseling field. I take that very seriously.
Discussion
Since its inception within doctoral counselor education, the NBCC MFP has awarded fellowships to 158 CES doctoral students all committed to continued work with marginalized and underrepresented students and/or clients within the profession. The SAMHSA-funded MFP aimed to increase diversity among doctoral-level clinical providers and educators. The findings suggest the MFP within counselor education is successfully meeting this goal as evidenced by the theme of access to the profession, in which survey respondents described how the support system offered by the MFP, including networking, the cohort model, the $20,000 financial award, and mentorship, aided in their completion of their doctoral studies and, in many cases, supported their transition to the profession, either as clinical practitioners or counselor educators. According to the survey results, 18 MFP fellows have entered the counselor education profession.
Additionally, the NBCC MFP is meeting its intended goal to promote multicultural competence by training doctoral-level counselors who then may appropriately serve diverse communities and students. The theme of clinical and multicultural competence reflected the advantages of ongoing clinical and multiculturally competent training offered throughout the MFP fellowship year. Former NBCC President and CEO Thomas Clawson also reported that another goal for the NBCC MFP was to train and prepare doctoral-level leaders within the counseling profession (as cited in Shallcross, 2012). This goal is also being met as evidenced by the subtheme of leadership within the paying it forward theme. The survey respondents described their commitment to give back to their communities as a result of their participation in the NBCC MFP and indicated that acting as leaders within the profession is one relevant way in which to do so. The survey results report 10 participants are serving as clinical supervisors and/or practitioners in their target communities.
In addition, the survey responses also offer glimpses into the NBCC MFP’s potential buffers to known challenges faced by counselor educators of color. These include lack of mentorship by other faculty of color (Henfield et al., 2013), isolation (Seward, 2014), and overall lack of preparedness to adjust to the demand of a system created for White males (Spanierman & Smith, 2017). Participants’ responses suggest that MFP resources, including mentorship, networking, and the cohort model, offered ongoing opportunities for fellows to engage in communities of support, encouragement, and motivation to complete their doctoral degrees and, in many instances, enter the academy. In some cases, responses indicated that fellows experienced a heightened level of support well beyond their fellowship year and into their new roles as early professionals. These reported factors might prevent and or buffer challenges experienced by counselor educators of color.
Implications
Several recommendations for counselor educators, supervisors, and doctoral students of diverse backgrounds can be ascertained from what we know about the NBCC MFP since its inception in CES in 2012. First, counselor educators can become knowledgeable about the NBCC MFP and its application deadlines to encourage CES doctoral students committed to working with diverse communities to apply. In so doing, counselor educators can also mentor CES students as they gather application materials.
Secondly, counselor educators and clinical supervisors may increase their multicultural competency knowledge by accessing the clinical trainings offered by NBCCF and may likewise encourage all doctoral- and master’s-level counseling graduate program students to access those resources. Such training aligns with Seward’s (2014) call to systemically infuse training to address the needs of students and faculty of color. In addition, more direct and open communication about such training needs may also promote an improved classroom and program racial climate (Seward, 2014).
According to survey respondents, many aspects of the NBCC MFP bolstered and supported their efforts to complete their doctoral programs and transition to the profession. Counselor educators, supervisors, and CES doctoral students may capitalize on the access and relationships that are made available through the MFP, thereby creating inclusion and support in academic spaces where faculty of color might otherwise be overlooked or misunderstood. Counselor educators and supervisors may consider how the structural elements of the MFP could be replicated within their programs in addition to the focus on clinical and multicultural training, mentorships, networking, and a collaborative student experience, with emphasis placed on addressing cultural factors to create a supportive environment for students and faculty of color (Shillingford et al., 2013). Such an endeavor requires intentionality through an honest evaluation of CES program recruitment and retention practices of faculty of color (Baggerly et al., 2017), an examination of how multiculturalism and social justice are infused throughout the program (Spanierman & Smith, 2017), and ongoing program assessment.
Limitations and Recommendations for Future Research
One significant limitation is the low number of survey responses. Although we had access to survey responses from cohort members between 2013 through 2018, approximately one third of the 158 fellows across the six cohorts responded to the surveys. Therefore, the findings cannot be generalized to all MFP fellows’ experiences. Given this limitation, future reviews should include larger numbers of cohort data. To address this limitation, in 2020, MFP administrators initiated a fellow engagement committee to encourage ongoing fellow participation after fellowship completion as well as enforce stricter regulations surrounding survey completion (M. Davis, personal communication, June 29, 2020).
In addition, only one out of the nine short-answer survey questions was selected for data analysis. The remaining survey data could be further analyzed for a more in-depth examination of respondent experiences. Future research should include qualitative studies to gain greater clarity on fellow experiences in order to better understand what aspects of the MFP structure were perceived as most beneficial as well as MFP fellow recommendations for improvements to the program. Additional quantitative research focusing on fellow self-efficacy within counselor education could be conducted utilizing pre- and post-fellowship year assessments. Another area deserving attention is how the NBCC MFP might recruit and maintain more male-identifying applicants of color given the lower number of males awarded MFP fellowships. Finally, exploration examining counselor education faculty awareness of the MFP would be helpful to learn how to reach a broader audience of potential doctoral applicants.
Conclusion
Since 2012, the SAMHSA-grant funded MFP in collaboration with NBCC has awarded 158 fellowships to CES doctoral students throughout the country. This article reviewed the most recent demographics reflecting diverse representation within counselor education and included challenges encountered by counselor education faculty of color. Next, descriptive outcome data and qualitative themes culled from MFP fellow survey responses were presented. The findings demonstrate evidence that the goals of the NBCC MFP to promote diverse representation within counselor education are being met.
Conflict of Interest and Funding Disclosure
The authors reported no conflict of interest
or funding contributions for the development
of this manuscript.
References
American Counseling Association. (2014). ACA code of ethics. https://www.counseling.org/resources/aca-code-of-ethics.pdf
Baggerly, J., Tan, T. X., Pichotta, D., & Warner, A. (2017). Race, ethnicity, and gender of faculty members in APA- and CACREP-accredited programs: Changes over five decades. Journal of Multicultural Counseling and Development, 45(4), 292–303. https://doi.org/10.1002/jmcd.12079
Braun, V., & Clarke, V. (2012). Thematic analysis. In H. Cooper, P. M. Camic, D. L. Long, A. T. Panter, D. Rindskopf, & K. J. Sher (Eds.), APA handbook of research methods in psychology: Vol. 2, Research designs: Quantitative, qualitative, neuropsychological, and biological (pp. 57–71). American Psychological Association. https://doi.org/10.1037/13620-004
Cartwright, A. D., Avent Harris, J. R., Munsey, R. B., & Lloyd-Hazlett, J. (2018). Interview experiences and diversity concerns of counselor education faculty from underrepresented groups. Counselor Education and Supervision, 57(2), 132–146. https://doi.org/10.1002/ceas.12098
Council for Accreditation of Counseling and Related Educational Programs. (2015). 2016 CACREP standards. http://www.cacrep.org/wp-content/uploads/2017/08/2016-Standards-with-citations.pdf
Council for Accreditation of Counseling and Related Educational Programs. (2018). CACREP vital statistics 2017: Results from a national survey of accredited programs. http://www.cacrep.org/wp-content/uploads/20
19/05/2017-CACREP-Vital-Statistics-Report.pdf
Haskins, N. H., Ziomek-Daigle, J., Sewell, C., Crumb, L., Appling, B., & Trepal, H. (2016). The intersectionality of African American mothers in counselor education: A phenomenological examination. Counselor Education and Supervision, 55(1), 60–75. https://doi.org/10.1002/ceas.12033
Henfield, M. S., Hongryun, W., & Washington, A. (2013). A phenomenological investigation of African American counselor education students’ challenging experiences. Counselor Education and Supervision, 52(2), 122–136. https://doi.org/10.1002/j.1556-6978.2013.00033.x
Jones, J. M., & Austin-Dailey, A. T. (2009). The Minority Fellowship Program: A 30-year legacy of training psychologists of color. Cultural Diversity and Ethnic Minority Psychology, 15(4), 388–399.
https://doi.org/10.1037/a0017558
Jones, N. A., & Bullock, J. (2012). The two or more races population: 2010 (Report number C20010BR-13). U.S. Census Bureau. https://www.census.gov/library/publications/2012/dec/c2010br-13.html
Lerma, E., Zamarripa, M. X., Oliver, M., & Vela, J. C. (2015). Making our way through: Voices of Hispanic counselor educators. Counselor Education and Supervision, 54(3), 162–175. https://doi.org/10.1002/ceas.12011
National Board for Certified Counselors Foundation (n.d.). Meet the fellows. https://nbccf.org/programs/schola
rships/fellows
National Board for Certified Counselors Foundation. (2014). 2013–2014 Annual report [Unpublished report].
National Board for Certified Counselors Foundation. (2018). 2017–2018 Annual report [Unpublished report].
National Board for Certified Counselors Foundation. (2019). 2019 MFP doctoral mental health counselors (MHC-D) fellowship manual [Unpublished manual].
Nowell, L. S., Norris, J. M., White, D. E., & Moules, N. J. (2017). Thematic analysis: Striving to meet the trustworthiness criteria. International Journal of Qualitative Methods, 16(1), 1–13. https://doi.org/10.1177/1609406917733847
Pérez, J. F. C., & Carney, J. V. (2018). Telling of institutional oppression: Voices of minoritized counselor educators. Counselor Education and Supervision, 57(3), 162–177. https://doi.org/10.1002/ceas.12108
Seward, D. X. (2014). Multicultural course pedagogy: Experiences of master’s-level students of color. Counselor Education and Supervision, 53(1), 62–79. https://doi.org/10.1002/j.1556-6978.2014.00049.x
Shallcross, L. (2012, November 1). NBCC awarded federal Minority Fellowship Program grant. Counseling Today. https://ct.counseling.org/2012/11/nbcc-awarded-federal-minority-fellowship-program-grant
Shillingford, M. A., Trice-Black, S., & Butler, S. K. (2013). Wellness of minority female counselor educators. Counselor Education and Supervision, 52(4), 252–269. https://doi.org/10.1002/j.1556-6978.2013.00041.x
Spanierman, L. B., & Smith, L. (2017). Confronting white hegemony: A moral imperative for the helping professions. The Counseling Psychologist, 45(5), 727–736. https://doi.org/10.1177/0011000017719550
Substance Abuse and Mental Health Services Administration. (2020). About the Minority Fellowship Program (MFP). https://www.samhsa.gov/minority-fellowship-program/about
Susan F. Branco, PhD, NCC, ACS, BC-TMH, LPC, LCPC, is a clinical assistant professor at The Family Institute at Northwestern University. Melonie Davis, MA, NCC, LCMHC-A, is Professional Development Coordinator for the National Board for Certified Counselors Foundation. Correspondence may be addressed to Susan Branco, 618 Library Place, Evanston, IL 60201, susan.branco@northwestern.edu.
Dec 16, 2020 | Volume 10 - Issue 4
Michelle Ghoston, Tameka Grimes, Jasmine Graham, Justin Grimes, Thomas A. Field
This research was conducted as part of a larger qualitative study that involved the collection and analysis of in-depth interviews with 15 counselor educators at counselor education and supervision doctoral programs accredited by the Council for Accreditation of Counseling and Related Educational Programs (CACREP). The participants were asked to identify strategies used to help students navigate the dissertation process and if the strategies were successful. Structural and relational strategies were identified as significant to the successful completion of the dissertation process. Although additional research is necessary to determine if the strategies are successful for faculty and students in other counselor education and supervision doctoral programs, we identified five themes that support the completion of the dissertation process: (a) mechanics of the program, (b) supportive environment, (c) selecting and working with committee members, (d) intentionality in developing a scholar identity, and (e) accountability.
Keywords: dissertation process, counselor education and supervision, CACREP, strategies, doctoral
Nearly 100,000 people pursue a doctoral degree in the United States every year (Jairam & Kahl, 2012). The pursuit of a doctoral degree in one’s identified field of study is considered an extraordinary feat. Earning a doctoral degree is an indication that one has achieved the apex in their identified area of expertise. Nevertheless, across all disciplines, the doctoral completion rate lags at 57% (Neale-McFall & Ward, 2015). There is a paucity of literature regarding how individuals navigate the process necessary to obtain a doctoral degree, including completing a dissertation. As with other fields, counselor education has a dearth of research into factors associated with doctoral completion and graduation (Golde, 2005; Hill et al., 2005; Protivnak & Foss, 2009).
The dissertation process can be confusing and arduous despite completing the journey with the support and guidance of a faculty member chairperson (Mauch & Park, 2003). The chairperson holds a senior position in terms of knowledge in the field and understanding of the process needed to ensure a successful dissertation. Although this process can take differing paths depending on the field, completing the dissertation is the ultimate goal in order to cross the threshold of earning a Doctor of Philosophy (PhD) or Doctor of Education (EdD) degree. For doctoral candidates who desire to progress through the dissertation process, a successful dissertation is the difference between achieving the pinnacle of one’s educational and professional goals versus remaining at the “all but dissertation” (ABD) phase.
Two major themes exist in the research literature relevant to successful dissertation experiences: the development of research identity and the importance of the advising relationship (Limberg et al., 2013; Neale-McFall & Ward, 2015). Further, Flynn et al. (2012) developed a theory that explains the experiences of counseling professionals during the dissertation phase. Their specific theory of initiation, management, and completion of the dissertation includes three elements: relational factors (i.e., personal relationships and friends), professional factors (i.e., career and professional identity), and internal factors (i.e., within the person). These themes are explored to position this study in the context of what is currently known about high-quality doctoral dissertation advising from the perspective of the chairperson, which further supports the theory of initiation, management, and completion of the dissertation process.
Research Identity Development
The experiences and challenges associated with the pursuit of a doctoral degree in counselor education and supervision (CES) have received increased focus within scholarly literature (Hinkle et al., 2014; Hoskins & Goldberg, 2005; Lamar & Helm, 2017; Neale-McFall & Ward, 2015). Critical to the pursuit of a doctoral degree is the scholarly identity forged among students during the dissertation process (Dollarhide et al., 2013; Limberg et al., 2013). For some doctoral students, the pursuit of a doctoral degree in CES is connected to research interests and goals developed during post–master’s degree experiences (Farmer et al., 2017; Hinkle et al., 2014). Upon entering a doctoral program, students often maintain those initial interests and goals or adopt new interests that align with expanded goals and/or faculty and program expectations (Lei, 2009). According to Hoskins and Goldberg (2005), congruence between students’ goals, faculty expectations, and doctoral program goals is a key determinant of student attrition and persistence in CES doctoral programs.
Faculty have an important role in the development of a scholar and research identity among CES doctoral students (Dollarhide et al., 2013; Limberg et al., 2013). Relationships with mentors and faculty contribute to doctoral students’ professional identity development as counselor educators (Limberg et al., 2013). To that end, faculty support is important in doctoral students’ research identity development (Dollarhide et al., 2013; Lamar and Helm, 2017). Nevertheless, gaps persist within the study of research identity development in CES. Although there has been examination into students’ rationales for the pursuit of graduate education in professional counseling and how this pursuit informs the development of one’s professional identity (Limberg et al., 2013), less is known about the experiences of doctoral students in CES (Dollarhide et al., 2013). As a result, little is known about the professional, research, and scholar identity development of doctoral students in CES and how doctoral study impacts the aforementioned areas of identity development (Dollarhide et al., 2013).
Chairpersons provide research-related ideas, strategies, and requirements useful to the development of students’ research identity. Examples of ideas and strategies include students seeing themselves as knowledge creators, the ability to identify gaps in literature, and a focus on completing a study that can be done in a reasonable time (Dollarhide et al., 2013). The dissertation stage is a place where students understand and accept their responsibility for creating new knowledge in the field. Yet, as faculty postulate these ideas and disseminate their recommendations to doctoral candidates, there may be a disconnect between seeing one’s role as a knowledge creator (student) and gatekeeper (faculty).
As gatekeepers for their doctoral candidates, faculty create barriers and maintain rules around what they deem is research, a structure for how to conduct research, and how the research will impact the field of counselor education. Researchers have yet to explore how students receive this feedback. Having their needs considered and receiving consistent feedback have been outlined as helpful with doctoral students understanding how gatekeeping supports them throughout the dissertation process (Dollarhide et al., 2013; Hilliard, 2013).
Approaches to Advising
The dissertation chairperson has a number of roles to help a doctoral candidate be successful. According to Garcia et al., (1988), a lack of chairperson supervision or mentorship contributes to delayed completion or non-completion of the dissertation process. Given the importance of the dissertation chairperson, understanding chairpersons’ approaches to advising and feedback is critical. Previous literature indicates three important elements of chairperson–student interactions in the dissertation process: (a) transparent and supportive feedback, (b) collaborative interactions, and (c) established communication expectations. These will be discussed below.
Transparent and Supportive Feedback
Hilliard (2013) provided a number of recommendations regarding transparent and supportive feedback to doctoral students. First, according to Hilliard, because chairpersons hold a major responsibility to ensure the student receives specific feedback for accepting improvements from other committee members, it is incumbent upon chairpersons to maintain positivity and professionalism when working with students. Second, chairpersons should demonstrate an ability to understand students’ needs in the context of their current dissertation stage. Lastly, Hilliard advises chairpersons to make consistent efforts to provide appropriate and useful feedback to students that informs them of their progress toward dissertation completion.
Nevertheless, there are a number of additional challenges in addressing feedback, including the strategies and ideas provided through feedback. Giving and receiving feedback can be challenging. Questions regarding when, where, and how feedback should be given further complicates the feedback process (Purgason et al., 2016). The complication in the feedback process occurs largely because both parties, chairperson and doctoral candidate, have a responsibility to provide and share feedback and oftentimes expectations are not established. However, in general, the chairperson has the added responsibility of initially broaching feedback, as well as establishing norms and expectations around how and when feedback can occur (Purgason et al, 2016).
Finally, faculty provide critical feedback in a supportive manner. Learning is most likely to occur when feedback is critical yet supportive, provided in a timely manner, and given with time for the advisee to receive and respond (Dollarhide et al., 2013; Idrus et al., 2018). The challenge faculty members face in following this structure of providing and receiving feedback is that it can create growth but may lead to feelings of frustration experienced by both individuals (Idrus et al., 2018; Waring, 2017). A response to address this challenge is to consider the whole person (i.e., professional identity and social and emotional wellness beyond academics) and educate students on the usefulness of giving and receiving feedback (Idrus et al., 2018).
Collaborative Interactions
Neale-McFall and Ward (2015) found that CES doctoral students were most satisfied when working with chairpersons who they perceived to be collaborative. This was a significant contributor to doctoral student satisfaction with the dissertation process. Additionally, Hilliard (2013) recommended that chairpersons work collaboratively by utilizing dissertation committee members’ expertise.
Established Communication Expectations
Hilliard (2013) noted that students are more likely to move successfully through the dissertation process if there are clear expectations communicated, written, and agreed upon with the faculty. Expectations that include each of these elements provide a foundation for the way feedback will be given and received. Moreover, clear communication expectations can help the doctoral candidate with productivity and keep both parties accountable throughout the dissertation process (Hilliard, 2013). Clear expectations provide a structure for the dissertation process and help candidates efficiently move through this phase of their doctoral journey (Flynn et al., 2012; Hilliard, 2013). In establishing these expectations, department and program faculty share the roles of the dissertation chairperson as coach and supporter of the doctoral student. Faculty and students have named other essential parts of successfully advancing through the process, including the degree of involvement, having systems of support, mentoring, and fitting within the departmental culture (Dollarhide et al., 2013). Despite naming these essential parts for success, little is known about how these factors impact successful navigation of the dissertation process.
Purpose of the Study
Previous research with current and former doctoral students has found that students see a number of criteria as vital to their success in the doctoral process. These criteria include professionalism, clear expectations, and consistent feedback from their advisor, as well as a collaborative approach to the dissertation and mentoring processes (Neale-McFall & Ward, 2015; Purgason et al., 2016; Sinady et al., 2009). Although these studies provide a detailed picture from the students’ perspective, limited research exists regarding the topic of successful dissertation advising from the perspective of faculty advisors. Faculty advisors play an integral role in the success of doctoral students as they progress through the dissertation process (Dollarhide et al., 2013; Limberg et al., 2013). To address this gap in knowledge, this research explored the following question: From a faculty member’s perspective, what strategies help students navigate the dissertation process, and how successful are those strategies? A qualitative design was selected to elicit an in-depth analysis of the experiences of faculty members supporting students in the dissertation process, affording the research team the opportunity to value all responses regardless of the frequency or number of responses (Lincoln & Guba, 2013).
Methods
This study was a part of a larger qualitative research study that was led by the fifth author. That larger study utilized a basic qualitative research design, with the primary goal of collecting and analyzing qualitative data, and employed the constant comparative method to collect, code, and categorize the data (Corbin & Strauss, 2015; Merriam & Tisdell, 2016). The data was collected using in-depth qualitative semi-structured interviews (see Appendix) with 15 faculty members in CES doctoral programs. Data collection continued until saturation was achieved and no new ideas were presented. Saturation was determined when the same themes were repeated by multiple participants. Participants responded to interview questions regarding issues pertinent to doctoral CES programs, specifically the components of high-quality programs, strategies to recruit and retain underrepresented students, strategies for working with administrators, and strategies for successful dissertation advising. In this study, a research team comprised of the first four authors analyzed and coded interview data pertinent to the research question: From a faculty member’s perspective, what strategies help students navigate the dissertation process, and how successful are those strategies? The goal of employing this research question was to identify successful strategies utilized by faculty to support doctoral students in completing the dissertation process and to understand the effectiveness of these strategies.
Participants
Participants in this study were full-time core faculty members in CES doctoral programs accredited by the Council for the Accreditation of Counseling and Related Educational Programs (CACREP). The participants worked in CACREP-accredited CES programs that had doctoral-level students. All participants had experience serving as a dissertation chairperson. Maximum variation sampling—that is, deliberately selecting a wide range of extremes from the population—was used to select participants to increase the likelihood of a diverse and representative sample (Merriam & Tisdell, 2016). Participants were selected one at a time to ensure adequate variation of the selection criteria. The selection criteria included: a) gender self-identification, b) racial and ethnic self-identification, c) Carnegie classification of the university where the participant was currently employed (The Carnegie Classification of Institutions of Higher Education, 2019), d) length of time working in doctoral-level counselor education programs, e) the method used to deliver the counselor education program where the participant was currently working (e.g., in person, online), and f) the region of the counselor education program where the participant was currently working. Based on previous research (Cartwright et al., 2018; Hill et al., 2005; Lambie et al., 2014; Smith et al., 2015), each of the noted criterion were believed to have some impact on the participants’ perspectives and, ultimately, their responses. Data saturation occurred after 15 interviews. A constant comparative method was utilized to assure saturation.
All 15 participants interviewed for this study taught in separate and unique CES programs. No program was represented by more than one participant. The demographics of the participants included eight self-identified males (53.3%) and seven self-identified females (46.7%). No participants identified as non-binary or transgender. All but one of the participants identified as heterosexual (n = 14, 93.3%); the one remaining participant identified as bisexual (6.7%). Racial and ethnic representation, also self-reported, was largely White (n = 11, 73.3%). Other racial groups represented included African American (n = 1, 6.7%), Asian (n = 1, 6.7%), Latinx (n = 1, 6.7%), and multiracial/multiethnic (n = 1, 6.7%). According to the 2017 CACREP Vital Statistics report, 71.38% of counselor education faculty in CACREP-accredited programs are White (CACREP, 2018). Thus, our sample was representative of the CES profession as it relates to the cultural identification of being White.
The participants averaged 19.7 years (SD = 9.0 years) of experience as full-time faculty members. Most of the participants’ years as faculty members were spent at the doctoral level in CES programs (M = 17.3 years, SD = 9.2 years, Mdn = 16 years). The number of years as a faculty member ranged from 3 to 33 years.
Procedure
After receiving approval from the last author’s IRB, a database of doctoral-level counselor educator contacts who worked at the then 85 programs accredited by CACREP was created (CACREP, n.d.). Thirty-four faculty responded to the request to participate. Of the 34 respondents, 15 respondents (41% response rate) were selected to participate in the study. The process of selecting and interviewing the 15 participants was scheduled and conducted by the fifth author. The selection of the 15 participants was done using maximum variation sampling (Merriam & Tisdell, 2016). The interviews lasted for approximately 60 minutes and were recorded with the consent of each participant via the Zoom online format. One interview was completed during a professional conference and was recorded with a Sony digital audio recorder. Participants were assigned an alphabetical identifier to protect individual identities during the data analysis process. This step allowed all researchers to be blinded to the participants’ identities except for the fifth author. The fifth author did not participate in the coding and analysis process in order to enhance participant anonymity and reduce the potential for bias during the data analysis process.
Interview Protocol
The interview question analyzed for this study was “How have you helped students to successfully navigate the dissertation process?” To start each interview, participants were asked the demographic questions mentioned above. Following the demographic information, eight in-depth questions were asked that addressed the research questions of the larger qualitative study (see Appendix). Per Patton’s (2015) recommendations, interview questions were open-ended, “why” questions were avoided, questions were as neutral as possible, and questions were asked one at a time. The interview protocol was piloted prior to the study commencing. Several questions were divided into two questions to ensure that only one question was asked at a time. A conventional semi-structured interview was used with follow-up questions allowed to ensure understanding of the participant responses. Each participant reviewed and signed the informed consent agreement approved by the last author’s IRB prior to the interviews.
Data Analysis
The team coded, categorized, and analyzed data from the 15 interview transcripts. Transcripts were coded using an open verbatim coding process, followed by the development of axial codes using the constant comparative method to create themes that emerged from the data (Corbin & Strauss, 2015). The research team used a shared Google Sheet to document codes, descriptions for the codes, and, later in the coding process, broader categories. All members of the research team had access to each transcript in a Microsoft Word document through Dropbox. Each line of the transcript was read and discussed by team members, and then a verbatim portion(s) of the line that answered the research question was copied to the shared Google Sheet. Once the code was selected, the group determined a description for the code, using the context in the transcript as a guide. The first three of the 15 transcripts were coded collaboratively as a team during online coding sessions. This was necessary to establish consistency among the researchers and to increase trustworthiness in the data (Corbin & Strauss, 2015; Merriam & Tisdell, 2016). Transcripts 4 through 11 were coded in pairs and the final four were coded individually with a second researcher available if there were questions. The first and second authors established a code key upon the completion of the first four transcripts.
Following initial coding, the first two authors met three additional times to come to a consensus regarding the collapsing of codes. For example, the code “playing politics” was initially identified. After all transcripts were coded, this code only had two direct quotes for support. Therefore, during a subsequent coding team meeting, the first two authors determined that this code had limited evidence from the data and it was collapsed into the code “selecting and working with committee members.” Creating a code book made it possible for the team to track categories and to ultimately identify the themes that emerged from the data. Verbatim quotes of participants were noted and organized into themes. Themes were agreed upon by the first two authors and reviewed and supported by the third and fourth authors.
The research team continued coding until completion, maintaining agreement on new categories and descriptions added to the code key. Any discrepancies were resolved by all team members, reaching consensus on the final coding. The following steps were adhered to by the team: 1) asking clarifying questions of each other to be sure every perspective was considered; 2) rereading previous lines of the transcript and reading ahead a few lines to better understand context; 3) allowing space to reflect on what each person was thinking and feeling about a code; 4) considering new codes when participant statements seemed to indicate different data points within the same line of the transcript; and 5) referring back to the research question when considering if a statement fit the purpose of the study.
Trustworthiness
To ensure a reliable process, the researchers adhered to a 4-step process proposed by Moustakas (1994). First, the researchers bracketed personal experiences and assumptions regarding what was instrumental in completing the dissertation process. For example, the research team discussed the nature of their own dissertation experiences as people of color at predominantly White universities; their beliefs that advising has a critical impact on student success, particularly for students of color; and their awareness that the faculty members’ perspectives may not speak to what is actually experienced by doctoral candidates. There also was a need to discuss what is actually meant by a successful dissertation. For the purpose of this research, the team determined successful as completing the dissertation process and having a degree conferred. Additionally, the first author participated in another project from the larger qualitative study that allowed access to participant responses regarding other topics that were not analyzed as part of this study. The information obtained from the other project was not shared during meetings for coding nor data analysis. Further bracketing was achieved by fleshing out any potential areas of overlap with the fifth author, who had knowledge of all transcripts but did not participate in coding. Memos were kept regarding each team member’s process.
Second, the researchers completed line-by-line, verbatim coding to identify repeated concepts and words within the transcripts. Third, the research team met on a regular basis to ensure consistency in coding and to resolve any discrepancies in the analysis process. During each of these meetings, memos were maintained to track methodological decisions and reactions to the data. Memos were kept by each coder to note thoughts, reactions, and methodological decisions during paired and individual coding. These memos were reviewed periodically by the fifth author, who was not actively participating in the coding process. Finally, the researchers questioned and investigated the constructs for themes to be sure to indicate the depth and breadth of the participants’ perspectives.
Positioning
The coding team was comprised of the first four authors. The coding team consisted of three counselor educators and one graduate school assistant director. Coding team members were from three institutions, with two team members working at the same institution (one counselor educator and one graduate school assistant director). Three of the coding team members identified as Black women, and one member identified as a Black man. All four coding team members held Doctor of Philosophy (PhD) degrees earned within the last 7 years. Two of the four coding team members completed their dissertation process within the last 18 months. All four of the coding team members worked at institutions conferring doctoral-level degrees. All but one coding team member had etic (outsider) status, as they had not yet served on doctoral dissertation committees. One coding team member had emic (insider) status, having served on two dissertation committees and participated in three dissertation defense presentations and discussions. This coding team member had not yet served as a chairperson of a dissertation.
Coding team members with etic positioning knew that their own experiences as doctoral students would be the most present in their minds when coding data. This required a significant amount of bracketing and identification of a priori codes. The first four authors’ initial meeting was dedicated to discussing these factors to ensure internal researcher accountability.
Potential biases of the research team included: (a) over-identifying with the data; (b) bracketing own negative experiences; (c) race and gender considerations (how our race and gender impacts how we see the recommendation); (d) having a higher education perspective and not a counselor education perspective; (e) role of privilege and how it plays out in the dissertation process and the lasting impact on early career progress; (f) awareness of differing program structures (some doctoral students mentored master’s-level students and developed writing teams, setting them up to be more successful once they had graduated); (g) having participated in faculty searches and seen successful dissertation advising (turning dissertations into manuscripts) be a key component in who is hired; and (h) having projects prioritized over opportunities that helped the doctoral candidate be more successful (e.g., publications, grants). These were all areas that required the coding team to discuss and process prior to delving into the transcripts. The coding team regularly challenged each other (i.e., suggested that a team member stop and reevaluate their position as it seemed more personal than based on the data) regarding these potential biases throughout the process.
The researchers identified a priori codes that included: (a) participants will be of the dominant culture; (b) how voices are centered would impact the data and results (hearing from the faculty member versus hearing from the student); (c) communication between student and chair, as well as student and committee, being important; (d) lack of awareness of race and gender influences on the dissertation advising process; (e) belief that the influence of the full identities of the doctoral candidate on their dissertation experience would not be captured in the data; (f) type of university (i.e., traditional, hybrid, online) impacts advising process; and (g) the doctoral student’s timeline does not align with the chairperson’s expectations of what the student needs (can impede the student getting to the end of the process successfully). Reconciling the a priori codes required coding team members to be open and honest regarding how their own experiences and perceptions have impacted their lens as educators and researchers. All researchers agreed to engage in these discussions during each meeting to ensure proper bracketing and to reduce the potential for bias negatively impacting the coding and analysis process.
Results
Five themes were identified based on the analysis of interviews with the 15 counselor educators who have served as dissertation chairpersons. The first and second authors collapsed 11 broader categories into the five emerging themes. The themes identified demonstrated some impact on a successful dissertation process: (a) mechanics of the program, (b) selecting and working with committee members, (c) intentionality in developing a scholar identity, (d) supportive environment, and (e) accountability. Each of these themes will be expounded upon below.
Mechanics of the Program
The mechanics of the program theme referred to program structures put in place that allowed students to move through the dissertation process. These program structures addressed the curriculum sequence and timelines. Faculty acknowledged that successfully navigating the dissertation process required a structured process on the program’s part. A participant commented that, in their experience, having an unstructured program usually led to “more ABDs than if it is structured.” Such a structured process started with “getting to know faculty members in terms of their research interests and identities and processes.” As students developed this knowledge, they were able to see examples of different faculty research identities within counselor education, while also learning which professor might be a good fit as the chairperson for their dissertation committee.
From there, programs put curriculum sequences in place that allow students to begin thinking about the dissertation process from the start of their doctoral journey. According to multiple chairpersons, doctoral students in their programs had at least one class in which they wrote research papers or miniature dissertation proposals that could be a starting point for their actual dissertation proposal. Creating this structure in the program, they believed, also supported students in developing a scholar identity, a theme that will be addressed in more detail later in this article. As one participant shared, “Students would essentially write a mini version of their dissertation proposal with lots of feedback and guidance from the course instructor and lots of check-ins with their major professor.” The class and check-ins became accountability measurements for the students, and these were established by the program as formalities rather than steps the students had to implement on their own.
Finally, chairpersons highlighted the importance of timelines as a necessary program structure to ensure student success in the dissertation process. These timelines are often externally imposed by larger entities, such as the graduate school and the university. In some circumstances, external deadlines created additional chaos for students. As a participant noted, sometimes an email was sent to the chairperson by administrators saying, “Grad College has changed their timeline for drops and deposits of thesis.” In response, all the faculty member can do is “forewarn [the students].” Instances such as these were out of the control of the chairperson. On the other hand, internal deadlines created by the program and agreed upon between the student and dissertation chairperson were beneficial. Overall, chairpersons who highlighted timelines in discussions with students noted a higher level of success in completing the dissertation process.
Selecting and Working With Committee Members
Selecting and working with committee members specifically applied to which faculty members were invited to serve on the dissertation committee. The dissertation committee tends to include three, and in some cases four, faculty members. These members often include the chairperson, a co-chairperson, a methodologist and, in some cases, a specialty person (someone who has expertise with the identified topic). Participants indicated that the selection of these members could have a strong impact on the likelihood of successfully completing a dissertation rather than the student remaining ABD. Although there was some variability in whether the doctoral candidate selected the committee members or if this was done by the chairperson, all participants were consistent in disclosing the importance of selecting the “right” committee members.
Several participants reported that faculty and students should give careful thought to committee composition before inviting faculty to serve on a student’s dissertation committee. Some faculty members can cause problems, such as being unresponsive and unsupportive. As one participant noted, “I don’t let [doctoral candidates] select [faculty members] who have a history of causing problems on committees.” Participants further noted that some students can get caught in political power dynamics between faculty. When this happens, the doctoral student has little to no power and has to rely on the chairperson to intervene.
Another participant noted that some faculty members are simply not able to be a part of a dissertation committee, stating, “Some faculty members are horrible. And some faculty members are not capable of being helpful to students. They have agendas of their own and they obstruct the progress.” When faculty obstruct progress, it can have significant impacts on the student’s likelihood of defending a dissertation successfully. When advising students, giving careful consideration to the composition of the dissertation committee seemed to be an important strategy to increase student likelihood of completing their dissertation.
Intentionality in Developing a Scholar Identity
Intentionality in developing a scholar identity was an important element of a successful dissertation strategy. Participants indicated that doctoral candidates should begin considering their dissertation topic and also identifying research methods of interest to them. As one participant shared, “When [doctoral candidates] are taking research methods . . . we encourage our students from day one to identify the general area of research that they’re interested in and then apply that in research methods and stats and qualitative.” Two participants both noted that students are more likely to go through the motions of completing a dissertation when they have not been thoughtful about their dissertation topic and have not been identifying a preferred methodology to address research questions pertinent to their topic.
In addition to helping students develop a research identity, participants identified the need for a balanced advising approach that helped students complete dissertations rather than becoming stuck in attempting to complete an unwieldy and unachievable dissertation. Participants reported that doctoral faculty needed to strike a balance between supporting the research ideas and interests of students and helping students identify projects that are achievable and realistic. As one participant noted, “It’s more about finding the balance between what’s gonna be a good and meaningful study for the student—hopefully what’s going to be a potential contribution to the field—and then what can be done.”
The participants noted that faculty should attend to the student’s development of a scholar identity during the dissertation process. Per one participant, as the chairperson, there is a need for “demystifying what research development looks like.”
Supportive Environment
The importance of creating a supportive environment was another key factor expressed by participants. A supportive environment, as described by several participants in this study, is relational: “[Mentoring] needs to happen in the context of relationship.” A supportive environment appears to be established when faculty individualize their advising and mentoring to each student’s personality and unique circumstances. As one participant stated, “Just as when we have to meet the client where they are, we also have to apply the same principle to our doc students.” Participants also reported that doctoral students needed different approaches and styles of advising. One participant shared, “My style varies depending on the student and my assessment of the student’s needs.” Some students will need more direct instruction than others, as “not every student needs the same level of guidance.” Other participants felt that faculty members could best guide students if they engaged in sustained relationships with them over time—“knowing somebody well enough and having enough contact with them over time to foresee some of those obstacles and help them navigate some of the roadblocks.” Participants also spoke to the importance of the chairperson detecting how much challenge and support to provide. As one participant stated, “I constantly try to figure out how much [support] is enough for this person, without being so much that they’re not learning what they need to learn in the process.” A faculty member’s established relationship with their doctoral students assists them in making such determinations.
The chairperson must provide feedback regarding whether a student’s proposal fits within their identified timeline. As one participant stated, “My job is to ensure that the product is gonna be the best it can possibly be for the timeline that it is.” Timelines, program structure, and the supportive environment overlap when the chairperson guides students to discern how to narrow their research idea into a manageable project that could be completed within the expected dissertation timeline. This conversation was another opportunity for faculty to mentor students and provide feedback in a way that would help the students be more successful in the dissertation process.
Many participants felt that a supportive environment enabled faculty to provide feedback and help students get “unstuck.” Providing feedback must happen early, otherwise students “just keep making the same mistakes over and over again.” When students become stuck in their dissertation process, a supportive environment helps students to be honest about their status. This honesty provides the chairperson with the information needed to give direction and feedback. As one participant shared, “Students almost embellish a little bit on how they were working because they were too afraid to say that they were stuck. So, for us, it’s really dissecting that component. ‘Where are you stuck? Let’s talk about this.’” Engaging in such conversations in an honest and transparent way gave the chairperson the opportunity to target their support toward specific goals that helped the student make progress.
Accountability
Participants reported that faculty chairpersons were in regular contact with their doctoral candidates to provide accountability. For most participants, this contact needed to be face-to-face, whether in person or via an online platform. As one participant shared, “I want that student in my office or on a screen in front of me every single week with actionable goals.” For this chairperson, a regular schedule of meetings ensured that there was a “constancy of contact.” Another participant agreed with this suggestion and specifically noted that these check-ins should be weekly after the dissertation writing began. The concept of accountability seemed to intersect with the supportive environment because many participants saw accountability as a means of supporting the student throughout the dissertation process.
The five themes identified in this study highlighted what dissertation chairpersons believed led to a successful dissertation. Both structural factors (mechanics, committee selection, and scholar identity) and relational factors (supportive environment and accountability) appeared to impact the success of the dissertation process.
Discussion
The purpose of this study was to identify successful strategies utilized by faculty to support doctoral students in completing the dissertation process and to understand the effectiveness of these strategies, as reported by the faculty members. The researchers engaged in verbatim coding to ensure that the perspectives of the participants were captured. Responses appeared to fall within two broad categories of structural and relational strategies. The structural elements highlighted the importance of a timeline and intentional department- and university-level scheduling and selection of committee members who are invested in the process of supporting the doctoral candidate in developing a scholar identity. Relational elements included a supportive environment and accountability as successful strategies in completing the dissertation process.
Structural Strategies
Institutions have their own timelines and processes, which doctoral candidates and chairpersons should know (e.g., approval of committee members, defense timeline, final submission procedures). When institutions change their processes or timelines, it greatly impacts the student’s ability to complete the process.
Chairpersons hold a major responsibility in helping the doctoral candidate understand the process of completing the dissertation (Flynn et al., 2012). The chairperson should clearly communicate requirements and guidelines for successfully completing the dissertation process (Hilliard, 2013). Ineffective communication by the chairperson can result in doctoral candidates lacking a clear understanding of the structure, leaving the candidate feeling unsupported and discouraged (Flynn et al., 2012; Hilliard, 2013).
Chairpersons who know their doctoral candidate’s strengths and weaknesses must seek committee members whose expertise fills gaps in areas where the student is not a content expert. The chairperson should also consider that the doctoral candidate’s success hinges on everyone’s investment in the process (Hilliard, 2013). The selection of committee members must thus be intentional, as not all faculty members are appropriate to serve on dissertation committees (Flynn et al., 2012). When the chairperson and doctoral candidate are strategic about selecting dedicated committee members, this may enhance the likelihood of a successful dissertation process. Students may benefit from reviewing former student dissertations. This current study further supports these structural strategies previously highlighted by Hilliard (2013) and Flynn et al. (2012).
Although a successful dissertation is a goal, the participants indicated the need to also ensure that doctoral candidates develop a scholar identity. This scholar identity allows the doctoral candidate to establish themselves as a researcher beyond the program (Lambie et al., 2008; Lambie & Vaccaro, 2011). The development of a scholar identity brings the process full circle as the former doctoral candidate represents their graduating institution and the profession (Flynn et al., 2012; Lamar & Helm, 2017).
Relational Strategies
Developing a supportive environment is a crucial strategy for a successful dissertation experience (Perera-Diltz & Sauerheber, 2017). Supportive environments include open communication, mentorship, providing helpful feedback, and providing appropriate challenge to candidates when writing the manuscript (Dollarhide et al., 2013; Neale-McFall & Ward, 2015; Purgason et al., 2016).
Communication primarily happens through the use of digital mediums such as email and virtual conferencing, or verbally through face-to-face meetings and telephone calls (Hilliard, 2013). This communication establishes support and a means of accountability. Both the candidate and chairperson should establish expectations regarding when to meet, the purpose of the meeting, and items to bring to the meetings (e.g., written sections of a manuscript, updates on the IRB decision regarding review requests).
Irrespective of the meeting format and candidate support, communication and feedback with candidates must be clear, precise, timely, and offer candidates some direction for how to move forward through their process. Feedback should also hold the doctoral candidate accountable for meeting any agreed-upon deadlines and items to submit. The style and type of feedback provided should be individualized to unique student needs and issues. Hilliard (2013) noted that feedback should (a) be given orally in meetings and electronically on items submitted from the candidate via their manuscript or email; (b) be frequent, with dates listed for each revision or submission of new information; (c) be detailed to what chapter or area in the dissertation the candidate needs to address; (d) be direct around dissertation progress and areas needing more development, and consistent so that candidates can move swiftly through their writing; and (e) include helping students understand the seriousness of academic integrity.
Doctoral candidates need the chairperson to be available and to communicate clearly and authentically. A defensible dissertation happens as a result of navigating the structural and relational components of the dissertation process. This study further aligns with Flynn and colleagues’ (2012) theory of initiation, management, and completion. Specifically, the relational and structural categories that emerged, from the perspective of the chairpersons working with doctoral candidates, are all support elements of a successful navigation of the dissertation process.
Implications
Doctoral students’ preparedness for the dissertation process varies throughout CES programs. Students’ experiences during the dissertation process also vary. The dissertation chairperson plays an important role in both the students’ preparedness and experiences. Yet, standards for best practices in dissertation advising in CES are not clearly articulated in the profession. It is possible that some doctoral students, particularly those who need additional support for research or writing, would benefit greatly from more structured and intentional dissertation methods (Perera-Diltz & Sauerheber, 2017). Without such guidelines, faculty members may rely on their own dissertation experiences to inform their current advising practices as faculty (Knox et al., 2011). Over time, the lack of standardized dissertation advising may contribute to disproportionate outcomes in (a) CES doctoral program completion rates, (b) research identity development among graduates of CES doctoral programs, and (c) overall CES program reputations.
Although chairpersons have many strategies to use in providing feedback, they cannot determine how their feedback impacts their students’ progression. Gaining a better understanding of how doctoral candidates internalize feedback may lead to more clarity regarding whether the strategy and style of feedback was successful. A similar study from the perspective of current doctoral candidates or recent graduates would add tremendous value to the field.
Quantitative studies could also explore relationships among variables. For example, the relationship between dissertation advising strategies and career choice is unknown. Schweiger et al. (2012) reported that approximately 50% of doctoral graduates in CES pursue non-academic careers, and it is possible that these graduates have different dissertation advising needs and/or received different forms of dissertation advising than candidates who entered academia after graduation.
Limitations
This study had several limitations. First, respondents were current faculty members in doctoral CES programs, and the data thus represents faculty perceptions and experiences. Future studies are needed to examine the perspectives of students when working with chairpersons to triangulate these strategies. Although prior research has shown that graduate students described similar strategies as those espoused by the participants in this study (Sinady et al., 2009), a follow-up study could be helpful to ascertain whether students felt the findings of this study were commensurate with their own experience.
A limitation of qualitative methodology is the ability to generalize findings. Because dissertation processes look different across programs and universities, it is unclear whether the strategies highlighted by participants in this study are transferable to other programs. Additional quantitative studies are needed that use a larger sample to examine the relationship between these strategies and outcomes such as dissertation completion rates and time to completion.
In this study, the research team only used one definition of success (i.e., completing the dissertation and graduating with a doctoral degree) when coding and analyzing data. Because the participants did not provide their own definition of success, we cannot say with certainty that they had the same conception in mind when responding to the question. Other definitions of success could include developing a scholar identity or being prepared to be an effective counselor educator. These alternative ways of understanding success could impact the way in which the participant responded to the question. In future research, it would be important to clarify these definitions with participants prior to their responding to the question.
Finally, two coding team members had recently completed their own dissertations and may have found it difficult to bracket their experiences during the coding and analysis process. To mitigate these potential biases, the research team frequently discussed and documented their personalized reactions to the data when coding, used multiple coders for the first 11 transcripts, and used consensus coding to resolve discrepancies.
Conclusion
Successfully navigating the dissertation process is a necessary step for obtaining a doctorate in CES. Though many doctoral students start the journey, the degree completion rate remains just above 50% (Neale-McFall & Ward, 2015). The completion rate for doctoral students in CES is currently unknown. Understanding ways that chairpersons effectively support students in the dissertation process can lead to more students completing their doctoral journey. Some of these ways include creating a supportive environment, establishing consistent accountability, and providing timely feedback. As students successfully navigate the dissertation process, they build confidence in their scholar identity and counselor educator identity and move forward into the counseling profession to support future generations of CES doctoral students.
The current study explored strategies for successful navigation of the dissertation process from the perspective of faculty members. Future research should examine the generalizability of our findings throughout other CES doctoral programs. Although some norms and expectations regarding the path to the dissertation in CES may exist, it is possible that other strategies were not fully captured in this study. Moreover, while the current study examined successful dissertation advising from the chairperson’s perspective, future research should examine the topic from the perspective of doctoral students and candidates. Moreover, it may be that current doctoral students and doctoral alumni may hold differing perspectives regarding their dissertation experience. To that end, future research may examine recent graduates of CES doctoral programs. A longitudinal study that explores the perspective of current students and the same sample later as alumni may capture nuances not accounted for in existing counselor education literature.
Conflict of Interest and Funding Disclosure
The authors reported no conflict of interest
or funding contributions for the development
of this manuscript.
References
The Carnegie Classification of Institutions of Higher Education. (2019). Basic classification description. http://carnegieclassifications.iu.edu/classification_descriptions/basic.php
Cartwright, A. D., Avent-Harris, J. R., Munsey, R. B., & Lloyd-Hazlett, J. (2018). Interview experiences and diversity concerns of counselor education faculty from underrepresented groups. Counselor Education and Supervision, 57(2), 132–146. https://doi.org/10.1002/ceas.12098
Corbin, J., & Strauss, A. (2015). Basics of qualitative research: Techniques and procedures for developing grounded theory (4th ed.). SAGE.
Council for Accreditation of Counseling and Related Educational Programs. (n.d.). Find a program. Retrieved December 12, 2020, from https://www.cacrep.org/directory
Council for Accreditation of Counseling and Related Educational Programs. (2018). CACREP vital statistics 2017. http://www.cacrep.org/wp-content/uploads/2019/05/2017-CACREP-Vital-Statistics-Report.pdf
Dollarhide, C. T., Gibson, D. M., & Moss, J. M. (2013). Professional identity development of counselor education doctoral students. Counselor Education and Supervision, 52(2), 137–150.
https://doi.org/10.1002/j.1556-6978.2013.00034.x
Farmer, L. B., Sackett, C. R., Lile, J. J., Bodenhorn, N., Hartig, N., Graham, J., & Ghoston, M. (2017). An exploration of the perceived impact of post-master’s experience on doctoral study in counselor education and supervision. The Professional Counselor, 7(1), 15–32. https://doi.org/10.15241/lbf.7.1.15
Flynn, S. V., Chasek, C. L., Harper, I. F., Murphy, K. M., & Jorgensen, M. F. (2012). A qualitative inquiry of the counseling dissertation process. Counselor Education and Supervision, 51(4), 242–255.
https://doi.org/10.1002/j.1556-6978.2012.00018.x
Garcia, M. E, Malott, R. W., & Brethower, D. (1988). A system of thesis and dissertation supervision: Helping
graduate students succeed. Teaching of Psychology, 15(4), 186–191.
https://doi.org/10.1207/s15328023top1504_2
Golde, C. M. (2005). The role of the department and discipline in doctoral student attrition: Lessons from four departments. The Journal of Higher Education, 76(6), 669–700.
https://doi.org/10.1080/00221546.2005.11772304
Hill, N. R., Leinbaugh, T., Bradley, C., & Hazler, R. (2005). Female counselor educators: Encouraging and discouraging factors in academia. Journal of Counseling & Development, 83(3), 374–380.
https://doi.org/10.1002/j.1556-6678.2005.tb00358.x
Hilliard, A. T. (2013). Advising doctorate candidates and candidates’ views during the dissertation process. Journal of College Teaching & Learning, 10(1), 7–12. https://doi.org/10.19030/tlc.v10i1.7525
Hinkle, M., Iarussi, M. M., Schermer, T. W., & Yensel, J. F. (2014). Motivations to pursue the doctoral degree in counselor education and supervision. The Journal of Counselor Preparation and Supervision, 6(1), 1–19. https://doi.org/10.7729/61.1069
Hoskins, C. M., & Goldberg, A. D. (2005). Doctoral student persistence in counselor education programs: Student–program match. Counselor Education and Supervision, 44(3), 175–188.
https://doi.org/10.1002/j.1556-6978.2005.tb01745.x
Idrus, M. M., Nor, N. F. M., Hashim, R. S., & Mydin, R. M. (2018). Advice-giving roles and strategies in selected faculty member-graduate student advising. Journal of Language Studies, 18(2), 217–234.
https://doi.org/10.17576/gema-2018-1802-15
Jairam, D., & Kahl, D. H., Jr. (2012). Navigating the doctoral experience: The role of social support in successful degree completion. International Journal of Doctoral Studies, 7, 311–329. http://ijds.org/Volume7/IJDSv7p311-329Jairam0369.pdf
Knox, S., Burkard, A. W., Janecek, J., Pruitt, N. T., Fuller, S. L., & Hill, C. E. (2011). Positive and problematic dissertation experiences: The faculty perspective. Counselling Psychology Quarterly, 24(1), 55–69.
https://doi.org/10.1080/09515070.2011.559796
Lamar, M. R., & Helm, H. M. (2017). Understanding the researcher identity development of counselor education and supervision doctoral students. Counselor Education and Supervision, 56(1), 2–18.
https://doi.org/10.1002/ceas.12056
Lambie, G. W., Ascher, D. L., Sivo, S. A., & Hayes, B. G. (2014). Counselor education doctoral program faculty members’ refereed article publications. Journal of Counseling & Development, 92(3), 338–346.
https://doi.org/10.1002/j.1556-6676.2014.00161.x
Lambie, G. W., Sias, S. M., Davis, K. M., Lawson, G., & Akos, P. (2008). A scholarly writing resource for counselor educators and their students. Journal of Counseling & Development, 86(1), 18–25.
https://doi.org/10.1002/j.1556-6678.2008.tb00621.x
Lambie, G. W., & Vaccaro, N. (2011). Doctoral counselor education students’ levels of research self-efficacy, perceptions of the research training environment, and interest in research. Counselor Education and Supervision, 50(4), 243–258. https://doi.org/10.1002/j.1556-6978.2011.tb00122.x
Lei, S. A. (2009). Strategies for finding and selecting an ideal thesis or dissertation topic: A review of literature. College Student Journal, 43(4), 1324–1332.
Limberg, D., Bell, H., Super, J. T., Jacobson, L., Fox, J., DePue, M. K., Christmas, C., Young, M. E., & Lambie,
G. W. (2013). Professional identity development of counselor education doctoral students: A qualitative investigation. The Professional Counselor, 3(1), 40–53. https://doi.org/10.15241/dll.3.1.40
Lincoln, Y. S., & Guba, E. G. (2013). The constructivist credo. Left Coast Press.
Mauch, J., & Park, N. (2003). Guide to the successful thesis and dissertation: A handbook for students and faculty (5th ed.). CRC Press. https://doi.org/10.1201/9781482293081
Merriam, S. B., & Tisdell, E. J. (2016). Qualitative research: A guide to design and implementation (4th ed.). Wiley.
Moustakas, C. (1994). Phenomenological research methods. SAGE.
Neale-McFall, C., & Ward, C. A. (2015). Factors contributing to counselor education doctoral students’ satisfaction with their dissertation chairperson. The Professional Counselor, 5(1), 185–194. https://doi.org/10.15241/cnm.5.1.185
Patton, M. Q. (2015). Qualitative research and evaluation methods: Integrating theory and practice (4th ed.). SAGE.
Perera-Diltz, D., & Sauerheber, J. D. (2017). Mentoring and other valued components of counselor educator doctoral training: A Delphi study. International Journal of Mentoring and Coaching in Education, 6(2), 116–127. https://doi.org/10.1108/IJMCE-09-2016-0064
Protivnak, J. J., & Foss, L. L. (2009). An exploration of themes that influence the counselor education doctoral student experience. Counselor Education and Supervision, 48(4), 239–256.
https://doi.org/10.1002/j.1556-6978.2009.tb00078.x
Purgason, L. L., Avent, J. R., Cashwell, C. S., Jordan, M. E., & Reese, R. F. (2016). Culturally relevant advising: Applying relational-cultural theory in counselor education. Journal of Counseling & Development, 94(4), 429–436. https://doi.org/10.1002/jcad.12101
Schweiger, W. K., Henderson, D. A., McCaskill, K., Clawson, T. W., & Collins, D. R. (2012). Counselor preparation: Programs, faculty, trends. Routledge.
Sinady, C., Floyd, D. L., & Mulder, A. E. (2009). The AACC competencies and the PhD completion project: Practical implications. Community College Journal of Research and Practice, 34(1–2), 218–226.
https://doi.org/10.1080/10668920903451442
Smith, R. L., Flamez, B., Vela, J. C., Schomaker, S. A., Fernandez, M. A., & Armstrong, S. N. (2015). An exploratory investigation of levels of learning and learning efficiency between online and face-to-face instruction. Counseling Outcome Research and Evaluation, 6(1), 47–57.
https://doi.org/10.1177/2150137815572148
Waring, H. Z. (2017). Going general as a resource for doing advising in post-observation conferences in teacher training. Journal of Pragmatics, 110, 20–33. https://doi.org/10.1016/j.pragma.2017.01.009
Appendix
Interview Protocol
- For context, please briefly describe how you self-identify and your background. This information will be aggregated; individual participant responses will not be associated with any quotes in subsequent manuscripts.
Gender:
Sexual/Affective Orientation:
Race and Ethnicity:
Years as a Faculty Member in a Counselor Education Program:
Years as a Faculty Member in a Doctoral Counselor Education Program:
Number of Doctoral Counselor Education Programs You Have Worked In:
National Regions of Doctoral Counselor Education Programs You’ve Worked In:
- How might you define a “high-quality” doctoral program?
- What do you believe to be the most important components? The least important?
- How have you helped students to successfully navigate the dissertation process?
- Which strategies has your program used to recruit underrepresented students from diverse backgrounds? How successful were those?
- Which strategies has your program used to support and retain underrepresented students from diverse backgrounds? How successful were those?
- What guidance might you provide to faculty who want to start a new doctoral program in counseling with regards to working with administrators and gaining buy-in?
- What guidance might you provide to faculty who want to sustain an existing doctoral program in counseling with regards to working with administrators and gaining ongoing support?
- Last question. What other pieces of information would you like to share about running a successful, high-quality doctoral program?
Michelle Ghoston, PhD, ACS, LPC, LCMHC, is an assistant professor at Wake Forest University. Tameka Grimes, PhD, NCC, is an assistant professor at Virginia Polytechnic Institute and State University. Jasmine Graham, PhD, is an assistant professor at Indiana University–Purdue University Indianapolis. Justin Grimes, PhD, is an assistant director for the Office of Recruitment, Diversity, & Inclusion for the Graduate School at Virginia Polytechnic Institute and State University. Thomas A. Field, PhD, NCC, CCMHC, ACS, LPC, LMHC, is an assistant professor at the Boston University School of Medicine. Correspondence may be addressed to Michelle Ghoston, 7406 Reynolda Station, Winston-Salem, NC 27109, ghostonm@wfu.edu.
Dec 16, 2020 | Volume 10 - Issue 4
Rebecca Scherer, Regina Moro, Tara Jungersen, Leslie Contos, Thomas A. Field
Initiating and sustaining a counselor education and supervision doctoral program requires navigating institutions of higher education, which are complex systems. Using qualitative analysis, we explored 15 counselor educators’ experiences collaborating with university administrators to gain support for beginning and sustaining counselor education and supervision doctoral programs. Results indicate the need to understand political elements, economical aspects, and the identity of the proposed program. Limitations and areas for future research are presented.
Keywords: counselor education and supervision, doctoral, university administrators, counselor educators, support
The Council for Accreditation of Counseling and Related Educational Programs’ (CACREP) 2009 CACREP Standards (2008) included a new requirement for core faculty in both entry-level (i.e., master’s) and doctoral programs. This requirement endured in the 2016 CACREP Standards (2015). Although West et al. (1995) predicted the necessity of growth of CACREP-accredited doctoral-level counselor education programs in the mid-1990s, it was not until 2013 that core faculty in all CACREP-accredited programs were required to possess doctorates in counselor education and supervision (CES; or be grandfathered in from previous employment experience; CACREP, 2008). Master’s-level programs that are seeking new CACREP accreditation, as well as existing programs that are seeking to maintain accreditation, must therefore hire faculty with doctorates in CES. This requirement has created a need for greater numbers of doctoral graduates in counselor education, and institutions with master’s-level programs may be seeking to establish new doctoral-level programs to meet this need.
The creation of a doctoral program requires intricate navigation of complex systems of administration, accreditation, funding, laws, facilities, infrastructure, and politics. Additionally, universities have different requirements and levels of approval for new program development (S. Fernandez, personal communication, November 27, 2017). Counselor educators proposing a CES doctoral program must have an understanding of the complexity of the specific university (e.g., its organization, the history of university support for doctoral programs, the mission of the institution, the needs of the surrounding community, and the resources required for program development and implementation). Furthermore, counselor educators must have a firm grasp of accreditation standards for both the university’s regional accreditation bodies (e.g., Commission on Colleges of the Southern Association of Colleges and Schools), as well as specialty CES accreditation through CACREP.
Structure of Universities
The hierarchical structure of universities varies from institution to institution. In this section, we provide a general outline of how universities are structured to help counselor educators who are interested in proposing a CES doctoral program. This information is very important when considering how to advocate for a doctoral program because of the many organizational layers and levels associated with an institution.
Typically, counseling programs are housed in a department, college, or school of the university (e.g., College of Education). The program is led by a program head, coordinator, or department chair. This person reports to the dean of the college. The dean reports to the provost or chancellor or chief executive officer. The president of the university then supersedes this level.
It is important for faculty members to assess the priorities of their institution for academic, student, and financial affairs. For example, a small private college in an urban area may have a mission to train adult learners and to provide access to education through lower admissions standards and flexible pathways to degree completion. In contrast, a large, public, research-intensive university may have a mission to support exceptional research and secure external grant contracts, and to raise college rankings through metrics such as low acceptance rates (The Carnegie Classification of Institutions of Higher Education, 2019). Based on administrative experience with doctoral program creation, structural information must be taken into consideration when advocating to administrators on behalf of CES doctoral program development.
Successful Initiation of Doctoral Programs
In the higher education literature, there are a few publications on the creation of doctoral programs. Researchers have proposed that doctoral programs can be successfully initiated in the context of three circumstances: (a) top-down initiation, (b) filling a need in the local area, or (c) focusing on new delivery methods (Brooks et al., 2002; Haas et al., 2011; Slater & Martinez, 2000). In regard to top-down initiation, some authors have proposed that doctoral programs are likely to be launched if the initial idea comes from the provost or president of the university. Slater and Martinez (2000) described the process of successful initiation of a doctoral program in a small institution in Texas. They reported that the president suggested the idea to the dean, with later onboarding of faculty members.
Doctoral programs also seem to be initiated successfully if a need exists for such a program in the local area (Brooks et al., 2002; Haas et al., 2011). Haas and colleagues (2011) emphasized the importance of faculty members and administrators assessing program fit within the region. In both the Brooks et al. (2002) and Haas et al. (2011) studies, the importance of current delivery modalities in successfully recruiting support for a doctoral program, including the use of online delivery and interdisciplinary studies, was presented.
Rationale and Purpose
At the time of writing, no studies could be identified in the CES literature regarding how to successfully gain administrative support for starting a doctoral program in CES. Another manuscript in this special issue (Field et al., 2020) illustrates a potential pipeline problem in counselor education, in particular the need for more CES doctoral programs in the North Atlantic and Western regions of the country. CES faculty members who are contemplating starting a CES doctoral program currently have little guidance on how to gain support for starting a program. In addition, no studies could be located regarding how to successfully sustain an existing doctoral program in CES. The purpose of this study was to collect and analyze qualitative data to address the research question guiding this study: Which strategies are helpful in gaining initial and ongoing support from administrators for a CES doctoral program, and how successful are those?
Method
This study was conducted as part of a larger basic qualitative study sampling counselor educators. The purpose of the larger qualitative study was to identify perceptions of doctoral-level counselor educators regarding four major issues pertinent to doctoral counselor education: (a) components of high-quality programs, (b) strategies to recruit and retain underrepresented students, (c) strategies for successful dissertation advising, and (d) strategies for working with administrators. In order to explore these four major issues, four research teams were assembled, one of which included the authors of this manuscript. All four coding teams worked together to select these four issues, as it was felt that these issues were most pressing for faculty who were seeking to establish new doctoral CES programs and that little information and guidance existed in these areas. In-depth interviews were then conducted with doctoral-level counselor educators in CACREP-accredited programs to answer a series of research questions that addressed the issues above. Faculty from CACREP-accredited programs were selected because the focus of the larger project was to support faculty who intended to seek CACREP accreditation for new doctoral CES programs.
In the basic qualitative tradition, qualitative data were collected, coded, and categorized using the constant comparative method from grounded theory methodology (Corbin & Strauss, 2015; Merriam & Tisdell, 2016). Basic qualitative designs involve the collection and analysis of qualitative data for the purpose of answering research questions outside of other specialized qualitative focus areas (e.g., developing theory, understanding essence of lived experience, describing environmental observations). Because we were not seeking to develop theory, understand lived experience, or research any other specialized qualitative focus area with this study, and because the research question did not require a specialized approach to data analysis, the large research team selected the basic qualitative approach described above.
Each coding team designed interview questions to directly answer their specific research question. The research questions explored in this study were as follows: Which strategies are helpful in gaining initial and ongoing support from administrators when seeking to start a new doctoral program in CES, and how successful are those? The interview questions that were developed and used as the basis for data collection for this study were: 1) What guidance might you provide to faculty who want to start a new doctoral program in counseling, with regard to working with administrators and gaining buy-in? and 2) What guidance might you provide to faculty who want to sustain an existing doctoral program in counseling with regard to working with administrators and gaining ongoing support?
Participants
Participants met two inclusion criteria for entrance into the study: (a) current core faculty members in a doctoral CES program that was (b) accredited by CACREP. Email requests were sent to 85 CACREP-accredited programs; faculty from 34 programs responded (40% response rate). Interviews were conducted with 15 full-time faculty members at CACREP-accredited CES doctoral programs. Participants were each from separate and unique doctoral programs, with no program represented by more than one participant.
The 15 participants were selected one at a time, using a maximal variation sampling procedure to avoid premature saturation (Merriam & Tisdell, 2016). The authors used maximal variation to understand perspectives from faculty of diverse backgrounds who worked at different types of institutions. Participant selection was predicated on six criteria grounded in research data about factors that may impact perceptions about doctoral program delivery: (a) racial and ethnic self-identification (Cartwright et al., 2018); (b) gender self-identification (Hill et al., 2005); (c) length of time working in doctoral-level counselor education programs (Lambie et al., 2014; Magnuson et al., 2009); (d) Carnegie classification of university where the participant was currently working using The Carnegie Classification of Institutions of Higher Education database (Lambie et al., 2014); (e) region of the counselor education program where the participant was currently working (e.g., Field et al., 2020), using the regional classifications commonly applied in the counseling profession; and (f) delivery mode of the counselor education program where the participant was currently working, such as in-person or online (Smith et al., 2015). As an example of this procedure, the first two participants were selected because of variation in gender, years of experience, and Carnegie classification. The third and fourth participants were selected on the basis of differences from prior interviewees with regard to ethnicity and region. Interviews continued until data seemed to reach saturation and redundancy at 15 interviews.
Although unintended, participant characteristics closely approximated CACREP statistics for faculty characteristics. The demographics of counselor educators in the sample was 73.3% White (n = 11), with 73.3% (n = 11) of participants working at research-intensive (i.e., R1 and R2) institutions. The sample was highly experienced, with an average of 19.7 years (SD = 9.0 years) as a counseling faculty member, with a range of 4 to 34 years. More than half of the participants (n = 9) had spent their entire career in doctoral counselor education.
Procedure
The last author of this manuscript sought IRB approval. Once we received IRB approval, potential participants were contacted from 85 CACREP-accredited programs with doctoral-level graduate studies in CES. Fifteen faculty were interviewed based on maximal variation sampling described above. All but one participant (n = 14) was interviewed via the Zoom video conference platform, chosen because of its privacy settings (i.e., end-to-end encryption). Interviews were recorded using the built-in Zoom recording feature. One participant was interviewed in person at a national counseling conference. This interview was recorded using a Sony digital audio recorder.
Interview Protocol
Each videoconference interview was begun by collecting demographics and informed consent. Following the introductory phase, interviewees were asked eight questions that addressed the research questions of the larger study. Two of the questions were specific to this sub-research team. Interview questions were developed using Patton’s (2015) guidelines to inform question development. Specifically, the questions were open-ended, neutral, avoided “why” questioning, and asked one at a time. The questions were piloted with peer counselor educators prior to the start of the research project in order to get feedback on clarity and ease of answering. Participants received the questions by email before their scheduled interview. The participants were identified using alphabetical letters to blind participant identity to all members of the research team.
Each semi-structured interview lasted at least 60 minutes, during which participants responded to questions that were evenly distributed among the four research teams. Participants were therefore able to respond to interview questions with significant depth. Data did not appear saturated until 15 interviews had been conducted. Each research team was asked to review the transcripts developed from the 15 interviews to deduce whether adequate saturation had been achieved and until consensus was reached.
Transcription
All interview recordings were transcribed by graduate students. These students had no familiarity with the interviewees and were trained in how to transcribe verbatim. Once completed, each transcript was sent back to the interviewees to ensure accuracy. After all interviewees checked their document, the sections of the transcripts with the questions related to each team were copied and pasted into a document organized by the participants’ alphabetical identifiers. Each team was responsible for coding and analyzing the responses to their respective questions from the interviews.
Coding and Analysis
The first, second, third, and fourth authors served as coding team members. The fifth author conducted the interviews as part of the larger study and assisted with writing sections of the methodology only. The demographics of the coding team were as follows. Team member ages ranged from mid-30s to 40s. All four identified as White cisgender females. Two of the coding team members were employed as full-time counselor educators, one identified as an administrator and counselor educator, and one coding team member was completing doctoral training as a counselor educator. Two participants had worked in doctoral counselor education programs, and two had not. We have served on both sides of the faculty–administrator relationship. These differences in backgrounds allowed for both etic and emic positioning pertinent to the topic of working with administrators to start and sustain doctoral programs in CES.
Because of the nature of both insider (emic) and outsider (etic) perspectives, the authors used a memo system when coding the manuscripts. This memo system involved three components. First, we created a blank memo every time a transcript was coded. Second, each time an interviewee’s transcribed response provoked some response within one of us, we raised it to the group and reflected on our individual experience. This response was documented in a memo. Third, one of us took notes to bracket any biases that might have been present. Identified biases often stemmed from our own experiences as faculty members talking to administrators, our service in an administrative role, or our own personal experiences developing doctoral programs. This occurred during joint coding team meetings and individual coding meetings once the open coding had been solidified into a set of codes. The memos were kept in a shared, encrypted, electronic folder for later review.
The following steps were followed by the coding team in the current study to ensure trustworthiness of analysis. The four coding team members jointly coded the first three participant transcripts to gain consensus. Following this open coding process, the second author condensed the open codes for the next phase of analysis. The coding team members then reached consensus on the condensed codes. Following agreement, we used the condensed codes to continue the coding process for the next two transcripts in joint coding meetings. This process allowed for discussion to assist with consistent understanding of the codes across the team. Following the joint open coding of the fifth transcript, the remaining 10 transcripts were assigned to one of us for open coding to be completed independently. After the open coding process was completed, the fourth author proposed a framework of the emerging themes. She examined the open codes and considered discussions that emerged throughout the team process to identify the emergent themes from the data. Open codes were only included in the analysis if they emerged in at least four transcripts, which resulted in the removal of three codes from the final results. All team members reached consensus for the themes that were originally identified by the fourth author.
Results
The data analysis process resulted in three emergent themes regarding strategies for gaining initial and ongoing support from administrators for CES doctoral programs and the level of success of those strategies. The three themes were political landscape, economic landscape, and identity landscape. Each theme had five associated subthemes. Each theme and subtheme are discussed in more detail below, and brief participant quotes are inserted to highlight the experiences of the participants in their own words for the purpose of thick description (Merriam & Tisdell, 2016).
Political Landscape
Considering the political landscape appeared to be a crucial strategy for recruiting administrative support when having conversations with administrators about CES doctoral programs. Participants described the importance of understanding the context of conversations with administrators within the larger political system of higher education institutions. The subthemes represented factors that influenced political decisions.
Political Endeavor: “Watching Your Politics”
Participants reported that conversations with administrators were highly political in nature and having these conversations was a form of political endeavor. One example of political endeavor was to ensure that other academic units and programs were in support of a CES doctoral program. As one participant stated, “First make sure that you’ve got your politics in order, so social work agrees with you and psychology agrees with you. So, you’ve got support of any competitor on campus.” If other academic units or programs are opposed to a CES doctoral program, it may result in administrators being cautious about supporting the program because of fears that they may be caught in the middle of a turf battle.
Gaining administrative support seemed to be predicated on the ability to “strategically build relationships” with administrators, as one participant put it. One participant commented on the complexity of developing these relationships with administrators. This participant believed that faculty needed to strike a balance of being flexible and adaptive to the administrators’ agenda and “order of the day,” while also retaining one’s “own ideology and belief systems.” Building relationships with administrators also seemed to involve avoiding unnecessary conflict that may reduce administrator support for faculty ideas. One participant cautioned that “watching your politics” and “keeping your mouth shut when you know you shouldn’t be speaking up against key administrators” was important during conversations with administrators to avoid unnecessary conflict that could “hurt your own doc program.” Learning this form of engagement seemed to be a struggle for some participants. One participant stated that they “don’t know how to navigate those conversations effectively” and felt “saddened and frustrated” as a result.
Status, Prestige, and Recognition: “A Huge Feather in One’s Cap”
Participants conveyed that CES faculty could gain administrative support through the strategy of arguing how a doctoral program could enhance status, prestige, and recognition for an institution. One participant commented that “all university presidents want doctoral programs. They want them because of the prestige.” This participant elaborated that faculty should therefore “show them how doctoral programs bring recognition, how it raises you in the rankings, and all of those kinds of things.” Some participants noted that the degree to which administrators cared about enhanced status, prestige, and recognition depended on the type of institution. For example, administrators who work at an institution that is less concerned with college rankings may be unpersuaded by the potential for enhanced status and recognition.
Participants also encouraged CES faculty to strategically engage in actions that increase recognition for the program and university. Some potential strategies that may appeal to administrators include being “identified as an expert, and to go out and do public radio broadcasts and be featured in the newspaper. Be featured in national publications.” This recognition helps with both program and university visibility, which participants believed was important to administrators. Participants also shared that visibility can help to protect the program from losing administrative support. As one participant stated, “If you’re invisible in the eyes of the administrators, they’re not going to think of you if some opportunities are coming to the fore.” This participant further commented that administrators needed to be reminded of the doctoral program through continual visibility efforts, as administrators often operate from an “out of sight, out of mind” position.
Demonstration: “Wanting Empirical Evidence”
Participants identified the strategy of sharing evidence with administrators to support and sustain doctoral programs. As one participant stated, “Once you get to the doctoral level, then we’re talking about people wanting empirical evidence.” In the early stages of program formation, this evidence might be a comprehensive proposal that is supported by data. As one participant stated, faculty need to develop a “solid plan” and be “as prepared as possible” for conversations in which administrators will “ask a ton of questions.”
Once a program is formed, it seems crucial that programs continuously provide updates to administration about program successes to sustain administrative support. Participants identified several approaches to demonstrating the success of a program. Some participants indicated that it was important to keep administration informed about student successes that occurred during doctoral study. One participant reported that their program kept administration informed via email about “every little success of the doctoral program” and provided the following examples: “Every time somebody successfully defends a dissertation, every time somebody presents at a conference, every time somebody gets a job congratulated, the president knows about it.” Other participants believed that it was helpful to report program outcomes such as graduation rates and employment statistics, which requires faculty to maintain contact with alumni to understand where they are working after graduation. It therefore seems possible that administrators may differ in which types of evidence they value, requiring faculty to carefully consider which information their administration most values when sending them updates of program successes. As one participant stated, “I think the question is, what information do you need to feed to administration to be convincing?”
Scrutiny: “Internal Credibility Is Super Important”
Participants reported that program faculty should understand the different ways that administration will scrutinize the credibility of a doctoral program. One participant defined credibility as, “Do what you’re doing well.” Administrators might withdraw support for a program that is perceived as not producing quality graduates or has problems such as not graduating students. Administrator scrutiny of the program’s financial situation also appears to be an important consideration. Administrators who are concerned about the financial viability of the program may withdraw their support.
Timeline and Trajectory: “It’s a Long Journey”
Participants reported that political decisions, such as starting and sustaining academic programs, particularly doctoral programs, may be influenced by unique timelines and trajectories. Participants encouraged faculty to develop the strategy of thinking long-term about cultivating administrative support for a doctoral program. One participant emphasized the need to “work together” with administrators in a collaborative fashion and make compromises so that administrators will support the doctoral program throughout the “long haul” and “long journey” of the program.
The length of administrator tenure at the university is another factor that faculty are advised to consider. One participant stated that faculty tend to have longer tenure than administrators at their university. As a “lifer,” this participant saw “a lot of rotation in and out of leadership.” Administrator turnover can result in changes to administrative priorities and agendas, which can impact support for a CES doctoral program. This participant encouraged faculty to “be cognizant of the fact that winds change.”
Economic Landscape
Considering the economic landscape and economic realities of starting and sustaining a doctoral program was the second main overarching theme. Developing an understanding of the economic landscape is important context for faculty when preparing for discussions with administrators. Several subthemes comprise the economic landscape, each detailed below.
Financial Aspects: “It Takes a Lot of Money”
Of utmost importance when discussing starting and sustaining CES doctoral programs with administrators is understanding the financial resources required. Many participants spoke about the cost of CES doctoral programs for universities. Participants believed that a crucial strategy to gaining administrator support was being able to explain how programs can be at least revenue-neutral or even generate revenue for the university, as administrators are less likely to support a CES doctoral program that is a drain on financial resources.
Participants varied in their perceptions of whether CES doctoral programs could generate revenue for the university. The key distinction between these participants seemed to be whether they believed doctoral programs should charge students tuition or fully fund them. Some participants believed that “high-quality doc programs do not make money for institutions” because they should be fully funding doctoral students rather than generating tuition revenue. These participants proposed that faculty should instead be “thinking creatively about funding sources” and seeking alternative methods of offsetting the financial burden on the institution. Examples of identified alternate funding sources included grants and undergraduate teaching opportunities for doctoral students.
Others were aware of this prevailing belief that doctoral programs do not generate revenue and argued the opposite: “Most faculty, when they want to start a doctoral program, they repeat this thing that they hear, which is ‘doctoral programs cost money, they don’t make money.’ And that’s not true.” These participants proposed that student tuition should be used to fund doctoral programs. One participant argued that if tuition exceeded the cost of faculty salaries, the program was likely to be generating revenue. This participant believed that counseling programs could generate money because they were relatively inexpensive. Unlike hard science disciplines, CES doctoral programs do not require expensive lab equipment, and CES faculty salaries are “lower compared to other programs.”
Tangible Benefits to Ecosystem: “How Do We Help?”
Participants discussed that administrator support for a doctoral program can be bolstered through demonstrations of how the program is supporting the local community. One participant shared that their program provides data to administrators about the number of hours of free counseling that the program provides to the community, which in turn helps the dean to gain the provost’s support for the program. Such data can help administrators when they conduct a cost–benefit analysis for whether to start a new program or sustain an existing program. Likewise, another participant encouraged faculty to take an “ecological view” and consider “how do we help . . . the surrounding communities?”
Need for Resources: “Pit Bulls in a Fighting Ring”
Participants discussed the need to address the competition for resources when attempting to gain administrator support. Participants mentioned the scarcity of resources that included faculty positions (i.e., lines) and physical building space. This scarcity resulted in programs needing to compete for resources. One participant stated, “I think we’re all going to be like pit bulls in a fighting ring over resources at this point.” Another participant shared a similar statement: “Once we get outside of our building, it is very territorial. So, we have to basically anticipate resistance from other pockets in the university if we want a new program at the doctoral level.” This participant elaborated that the provost needs to be aware of these dynamics and that faculty should attempt to make a strong case for needing resources if they are in competition with other programs.
Competition for resources seemed to occur not only within a university’s departments but also between CES programs at different universities. Doctoral applicants appear to be increasingly making enrollment decisions based on tuition costs and graduate assistantships, which increases the pressure for programs to provide financial support packages. One participant reported that it is becoming less feasible to operate a doctoral program without “some form of stipend or assistantship” because “if you don’t, there’s too many other programs that do.” This participant elaborated that administrators must support the program with assistantships and concluded, “I wouldn’t try to start a program without it.”
Some participants discussed strategies to maximize resources across the college or school in which the program exists, such as with college-wide methodology courses. Such strategies seemed particularly important when adapting to the pressure of accepting more students to make the program revenue-neutral. One participant suggested that such resource sharing was “of utmost importance… in the early beginnings of programs.”
Faculty and Program Responsibilities
Faculty have more complex responsibilities when operating a doctoral program compared with a master’s program, such as attending conferences with students and engaging in the larger campus community. As one participant stated, “It’s also being at events, interacting with administrators, making sure when walking around campus or buildings that they know who you are and that they can connect with what you’re doing.” Participants explored the economic aspects of the responsibilities that individual faculty members and the larger program have when responsible for the doctoral education of counseling students: “At our institution, you don’t get a lot of credit per se, or release time or extra pay for all of the work it takes to mentor doctoral students.” This credit that is or is not allocated to doctoral education impacts faculty members’ well-being. Another participant cautioned faculty to be aware of “faculty burnout” that accompanies tensions around adequately funding faculty positions: “If you shrink, and you still maintain the same number of students, there is simply not enough time, not enough emotional capacity, to do the good work.” Another participant shared that their doctoral programs felt like “hell on wheels” because “we ended up with a program that had more than 100 students with two real tenured faculty running the program.”
Influence of University: “Know the Size and Culture”
This subtheme represented faculty considerations of the larger university system context where the counseling program is situated. As one participant summarized, “part of it is looking at the context of the program in the university.” Participants particularly referenced size as an influencing factor. As one participant stated, “Know the size and culture of your institution.” University size influenced participants’ access to decision-makers: “We’re so small that I could literally walk out of my office and two minutes later I can be in the provost’s office. I can ask a question. They’re very approachable, and so I don’t feel intimidated.” Understanding the institution’s mission and its funding priorities is crucial to forging successful alliances with administrators regarding whether to start and sustain a CES doctoral program. Understanding where a CES doctoral program fits within the institution’s academic structure therefore helps faculty to effectively communicate with administrators, and consistently reviewing this can help inform ongoing dialogues with administrators.
Identity Landscape
The overarching identity landscape theme represents how programs both understand their internal identity regarding doctoral education, as well as the external identity factors that contribute to the program. Each subtheme is detailed below with participant quotes.
Operationalize and Define Commitment: “Faculty Have to Buy In”
Gaining faculty buy-in prior to conversations with administrators and gaining approval for a doctoral program was a consistent message relayed by participants. One participant reflected, “Everybody has to be on board and has to buy in to the concept that the mission can’t be the mission of one person.” Another participant recommended that faculty leadership (e.g., program directors) need to operationalize this commitment through intentional dialogues with faculty. This participant stated that “the evidence for faculty buy-in isn’t always there until you probe.” They elaborated that faculty leadership can facilitate discussions around the following questions: “Are you willing to do X, are you willing to do Y?” and “If we start a doctoral program, do you feel like you have the skills you’ll need or do you fear that you’re going to be left behind?” Such conversations appeared important to developing a unified collective commitment to the doctoral program, which was critically important when challenges arose. Other participants reflected on personal buy-in and encouraged self-reflection in this regard: “Things to consider including one’s own personal meaning making.” Participants reflected that doctoral education was significantly different than master’s-level education and required a different level of commitment. Administrators are unlikely to support a doctoral program if the faculty are divided in their commitment to the program.
Understanding Differences: “Know What Your Program Is Worth”
Participants spoke about the need for faculty to possess knowledge about multiple aspects of doctoral education when conveying information to administrators. Faculty should be familiar with the differences between master’s and doctoral education, between doctorates in other disciplines within the university, and among doctoral programs at different universities in the state. This information assists faculty “to really know what your program is worth and to be able to explain it.” For example, faculty should make administrators aware of how doctoral education can enhance master’s-level training rather than result in master’s students being “ignored” and treated as “second class citizens.”
Participants indicated that administrators may not be familiar with the counseling profession and thus may need education. Participants reported the need for “educating your administrative colleagues about what counselor ed is, what they do, how we train.” Another participant stated that “even at the dean level, they don’t know what the heck a mental health counselor is. Not a clue.” Consistent with this, administrators may also need information about other aspects of the profession, such as the value of specialized accreditation. One participant reported, “I think that we can do a better job of telling our admin the pros of CACREP versus the cons.” Education about CACREP accreditation was important because of the costs associated with accreditation fees and hiring core faculty to meet the CACREP doctoral standards.
Quality in Programs: “High-Quality Output”
Participants reflected on the importance of program quality as a reflection of the programs’ overall identity. Program outputs seemed to be a particularly important measure of program quality. Some participants, particularly those at research-intensive universities, emphasized the importance of research-related outputs such as “grants, high-quality output, and visibility.” Across participants, employment rates were a particularly important measure of program quality, especially employment in academic and administrative jobs post-graduation. Participants reported that such metrics were useful as a “selling point” to administrators, especially if needs existed for doctoral-level graduates in the local area. As one participant stated, “Some of those outcomes become really important to administrators, and I think that we need to be good at putting those outcomes in front of them.”
Participants also shared concerns with program quality. These concerns often centered on admitting more students than can be adequately mentored through the dissertation process. One participant was “concerned about doc programs that bring in cohorts of 20 and churn them out” because they feared that “big doc programs” are “just course-based models without a whole lot happening outside of that. . . . And, you know, I worry about dissertation mentoring.”
Program accreditation was explored as an influencing factor in program quality that ultimately influences the overall program identity through reputation. One participant stated, “We built the program around the accreditation standards and took those standards very seriously.” Another participant explored how the accreditation process can influence administrators’ opinions of the program: “If we had bombed that visit, from the president to the vice president on down, we would have looked really bad.”
Advancing the Institutional Mission: “It Has to Match”
Study participants commented on the importance of the identity of the doctoral program connecting to the mission of the larger institution. One participant encouraged faculty to consider the institutional mission when communicating with administrators: “When we advocate for programs, we need to understand the mission of the institution.” This participant reported that administrators in a university that values community service may be in favor of doctoral programs that “create more service providers for the local community.” Another participant stated that “it has to match the university’s mission. I hear that more and more and more.” This participant acknowledged that a proposed doctoral program would only receive administrative support if it “fits with the strategic plan of the university.” Participants indicated that the program should align not only with the institutional mission but also with the mission of the college or school where the program is housed.
Stakeholder Dynamics: “Making the Administrators Happy”
Participants discussed the variety of stakeholders that faculty should consider when developing a CES doctoral program. Such stakeholders include the students being educated, faculty in the program, administrators who make decisions about the program, and employers of future program graduates. Participants reflected that each stakeholder group can contribute meaningfully to the identity of the program.
At times, a stakeholder group’s contributions and agendas may be at odds with those of another stakeholder group. This is particularly problematic when tensions exist between a stakeholder group and administrators. For example, faculty may prefer a smaller program than administrators. One participant stated that “one of the things that I’ve fought with faculty about my whole life, has been that [faculty] want small classes and they want few students.” This participant added that administrators tend to close smaller programs when pressured to cull the number of doctoral programs at an institution, and thus smaller size represents a potential threat to the program: “Any time an administrator is going to cut a program or deny resources to a program, they do it with the program with the least number of students in it. It’s just the absolute way it’s done.” This participant proposed that faculty stakeholders must therefore understand the dynamics of higher education administration when advocating, as “making the administrators happy with the numbers” is an important priority.
Discussion
In this study, we conducted a qualitative analysis of interviews with 15 experts in the field to examine the research question. We identified participant-reported strategies for gaining initial and ongoing support from administrators for a CES doctoral program. The overarching themes of political, economic, and identity landscapes emerged from the data, alongside associated strategies necessary for gaining support. Navigation of complex university systems, including accreditation, finances, legal concerns, infrastructure, and politics, seem to be required for successful initial administrator approval of a CES doctoral program. Awareness of institutional mission and history, purpose, community needs, fiscal realities, and the university’s organizational chart also can facilitate approval and successful program sustenance.
Implications for CES Faculty
The findings from this study may be utilized by existing master’s degree counseling program faculty who want to create a CES doctoral program. Faculty should embark on a data-driven process to inform administrators of tangible benefits across multiple systems and articulate the financial resources necessary for long-term success. As new CES doctoral programs are proposed, faculty should ensure that university administrators are aware of the relative worth of counselors and counselor educators, particularly in contrast to other mental health disciplines that may exist on campus. They may need to document the tangible benefits that CES programs bring to the university that are in alignment with the university’s mission and strategic plan. In 2013, Adkison-Bradley noted, “As universities change and grow, academic programs are often required to justify their request for resources or asked to explain how they uniquely contribute to the overall mission of the college and surrounding communities” (p. 48). Faculty could benefit from open dialogue with administrators and mentors about what it costs the institution to have a doctoral program compared to what revenue and resources a doctoral program can generate. CES faculty also can provide data to explain how accreditation requirements that may appear expensive to administrators (e.g., 1:6 faculty–student ratios in practica; 1:12 faculty–student ratios) do benefit students, clients, and communities, including protection of “broad public interests” (Urofsky, 2013, p. 13).
Faculty must engage in systemic thought that goes beyond the program and department. Bronfenbrenner’s (1979) ecological systems model provides a useful model for program faculty to understand. This model includes four main systems in which individuals exist—microsystem, mesosystem, exosystem, and macrosystem, with each system growing in size and complexity. Faculty without this perspective risk experiencing their department in a bubble and may not realize how their smaller microsystem (i.e., program, department) fits within the larger macrosystem of the university. The political landscape can become entangled in the developing exosystem where these systems overlap. This exosystem includes considerations for the college’s or school’s strategic priorities where the doctoral program is located. Faculty also should consider larger systemic interactions, such as the doctoral program’s relationship with the local community, with other master’s and doctoral programs in the state, and with other doctoral programs nationally.
The 2016 CACREP Standards (2015) require doctoral education to focus on leadership. However, the standards require this education to be in relation to counselor education programs and in professional organizations, not specifically in institutions of higher education as larger systems. It is unknown how or if students receive formal education about how to navigate university systems, as it is not typically included in CES doctoral program curricula. However, in our own personal experiences as faculty members and doctoral students, we have found that this knowledge seems to be acquired through observation, experience, and on-the-job mentoring. Unfortunately, this learning may occur when new and junior faculty are under pressure to establish themselves for tenure and promotion. Senior faculty, including those nearing retirement, are likely to possess this systemic knowledge and understanding. This knowledge could be conveyed via formal or informal mentoring programs; however, junior faculty in counselor education programs report a lack of mentoring experiences (Borders et al., 2011). The lack of mentoring could be from a variety of reasons, as junior faculty members may be intimidated by senior faculty (Savage et al., 2004), or senior faculty may lack the commitment to put forth the long-term effort to gain support for a new CES doctoral program.
Faculty must be willing to invest in learning about the processes involved in doctoral program creation—to listen, be respectful, and exercise patience for the time required for program approval, funding, and development. The results of this study indicate that program generation is a political process, and junior faculty must be aware of their environment. Faculty have different levels of input and leadership at different institutions, such as with different forms of shared governance (Crellin, 2010). Faculty who do not understand political savviness, the role of fiscal constraints, and the historical precedents for doctoral program initiation may struggle more than those who understand the lens by which individual institutional decisions are made.
Implications for University Administrators
University administrators could utilize the results of this study to understand how to work with faculty who are requesting the initiation of a new doctoral program. Administrators could consider establishing dedicated time and orientation to new and junior faculty to assist them in conceptualizing how faculty requests are prioritized within the institution, perhaps via a formal mentoring program (Savage et al., 2004). For example, if the university’s current vision is to respond to the lack of STEM (science, technology, engineering, and mathematics) graduates in the local job market, counseling faculty could better manage their expectations about the estimated timeline of new degree program creation while aligning their new CES doctoral degree proposal to a more attainable target date. Communication about the timeline of decisions and the patience involved in systemic change (e.g., state legislature involvement) could also benefit the faculty perspective. Opportunities for learning about the organization are a crucial ingredient in organizational change (Boyce, 2003).
Although it is the responsibility of deans and department chairs to communicate the university’s vision and strategic plan, administrators should also trust the CES faculty’s distinct knowledge of the field and dynamic accreditation standards. Faculty are uniquely qualified to anticipate shifts in the profession that could impact their programs. From our experience, CES faculty who serve as internship clinical supervisors may also possess unique knowledge of the needs of the surrounding communities through their supervisees’ reports of client needs.
It is suggested that administrators include a university organizational chart in new faculty orientation or in the faculty handbook so that faculty can be aware of the hierarchy within the university. The orientation should include a clear explanation of how the particular institution prioritizes agendas and provide a history of the institution, with specific examples of prior program creation in the face of competing needs (e.g., missions, financial). Faculty can then understand how the university invests in its future.
Limitations and Suggestions for Future Research
Several limitations exist with qualitative research in general, and with this unique project specifically. In general, qualitative research is limited by researcher bias, interviewer bias, interviewee bias, and participant demographics (Corbin & Strauss, 2015). To control for potential bias during the analysis process, the coding team used several strategies to enhance trustworthiness, including recruiting coding team members who had identities as both CES faculty and administrators, bracketing biases throughout coding, using consensus to resolve discrepancies in coding, and using memos to document decisions. Future studies could seek to triangulate the data from this study to determine whether the findings are transferable to the perspectives of other faculty in CES doctoral programs.
The focus of this particular research study was to explore faculty perspectives regarding how to gain administrative support for initiating and sustaining CES doctoral programs. As such, the perspectives of administrators were not surveyed regarding how to gain administrative support for CES doctoral programs (beyond those counselor educator faculty participants who have served in administrative roles). Future studies, perhaps in the form of quantitative research, could include these perspectives to determine whether the perspectives of CES doctoral faculty are consistent or divergent with administrator experiences regarding how to work effectively with administrators.
We sought to understand strategies for successfully gaining initial and ongoing administrative support for a CES doctoral program. This exploration included both participants who had recently started new programs and those who had long worked in CES doctoral programs. However, an analysis of thematic differences between participants who had and had not spearheaded the creation of a CES doctoral program was not conducted. Future research could explore whether strategies varied for those who had recently started a CES doctoral program versus those who had not. In addition, data were not organized and analyzed by differences in participants’ institution type (i.e., private or public), because it was outside the scope of the research question. Finally, the study focused solely on faculty at CACREP-accredited institutions. It is unknown whether the perspectives of participants in this study would be consistent with faculty at non–CACREP-accredited institutions.
Conclusion
The counseling profession continues its efforts to address the pipeline shortage of doctoral-level CES faculty to meet CACREP accreditation requirements. To meet this need, some master’s-level programs are seeking to start CES doctoral programs. The findings from this study may be useful to CES faculty when planning a strategic approach for collaboration with administrators regarding the initiation of new CES doctoral programs. This strategic approach will involve exploring political elements, economical components, and the identity of the proposed program. The findings of this study indicate these areas of knowledge promote a more comprehensive planning process to help prepare for working with administrators on the creation of a doctoral program.
Conflict of Interest and Funding Disclosure
The authors reported no conflict of interest
or funding contributions for the development
of this manuscript.
References
Adkison-Bradley, C. (2013). Counselor education and supervision: The development of the CACREP doctoral standards. Journal of Counseling & Development, 91(1), 44–49. https://doi.org/10.1002/j.1556-6676.2013.00069.x
Borders, L. D., Young, J. S., Wester, K. L., Murray, C. E., Villalba, J. A., Lewis, T. F., & Mobley, A. K. (2011). Mentoring promotion/tenure-seeking faculty: Principles of good practice within a counselor education program. Counselor Education and Supervision, 50(3), 171–188. https://doi.org/10.1002/j.1556-6978.2011.tb00118.x
Boyce, M. E. (2003). Organizational learning is essential to achieving and sustaining change in higher education. Innovative Higher Education, 28(2), 199–136. https://doi.org/10.1023/B:IHIE.0000006287.69207.00
Bronfenbrenner, U. (1979). The ecology of human development: Experiments by nature and design. Harvard University Press.
Brooks, K., Yancey, K. B., & Zachry, M. (2002). Developing doctoral programs in the corporate university: New models. Profession, 89–103. https://www.jstor.org/stable/25595734
The Carnegie Classification of Institutions of Higher Education. (2019). Basic classification description. http://car
negieclassifications.iu.edu/classification_descriptions/basic.php
Cartwright, A. D., Avent-Harris, J. R., Munsey, R. B., & Lloyd-Hazlett, J. (2018). Interview experiences and diversity concerns of counselor education faculty from underrepresented groups. Counselor Education and Supervision, 57(2), 132–146. https://doi.org/10.1002/ceas.12098
Corbin, J., & Strauss, A. (2015). Basics of qualitative research: Techniques and procedures for developing grounded theory (4th ed.). SAGE.
Council for Accreditation of Counseling and Related Educational Programs. (2008). 2009 CACREP standards. https://www.cacrep.org/wp-content/uploads/2017/07/2009-Standards.pdf
Council for Accreditation of Counseling and Related Educational Programs. (2015). 2016 CACREP standards. http://www.cacrep.org/wp-content/uploads/2017/08/2016-Standards-with-citations.pdf
Crellin, M. A. (2010). The future of shared governance. New Directions for Higher Education, 2010(151), 71–81. https://doi.org/10.1002/he.402
Field, T. A., Snow, W. H., & Hinkle, J. S. (2020). The pipeline problem in doctoral counselor education and supervision. The Professional Counselor, 10(4), 434–452. https://doi.org/10.15241/taf.10.4.434
Haas, B. K., Yarbrough, S., & Klotz, L. (2011). Journey to a doctoral program. Journal of Professional Nursing, 27(5), 269–282. https://doi.org/10.1016/j.profnurs.2011.04.006
Hill, N. R., Leinbaugh, T., Bradley, C., & Hazler, R. (2005). Female counselor educators: Encouraging and discouraging factors in academia. Journal of Counseling & Development, 83(3), 374–380.
https://doi.org/10.1002/j.1556-6678.2005.tb00358.x
Lambie, G. W., Ascher, D. L., Sivo, S. A., & Hayes, B. G. (2014). Counselor education doctoral program faculty members’ refereed article publications. Journal of Counseling & Development, 92(3), 338–346.
https://doi.org/10.1002/j.1556-6676.2014.00161.x
Magnuson, S., Norem, K., & Lonneman-Doroff, T. (2009). The 2000 cohort of new assistant professors of counselor education: Reflecting at the culmination of six years. Counselor Education and Supervision, 49(1), 54–71. https://doi.org/10.1002/j.1556-6978.2009.tb00086.x
Merriam, S. B., & Tisdell, E. J. (2016). Qualitative research: A guide to design and implementation (4th ed.). Wiley.
Patton, M. Q. (2015). Qualitative research and evaluation methods: Integrating theory and practice (4th ed.). SAGE.
Preston, J., Trepal, H., Morgan, A., Jacques, J., Smith, J. D., & Field, T. A. (2020). Components of a high-quality doctoral program in counselor education and supervision. The Professional Counselor, 10(4), 453–471. https://doi.org/10.15241/jp.10.4.453
Savage, H. E., Karp, R. S., & Logue, R. (2004). Faculty mentorship at colleges and universities. College Teaching, 52(1), 21–24. https://doi.org/10.3200/CTCH.52.1.21-24
Slater, C. L., & Martinez, B. J. (2000). Transformational leadership in the planning of a doctoral program. The Educational Forum, 64(4), 308–316. https://doi.org/10.1080/00131720008984775
Smith, R. L., Flamez, B., Vela, J. C., Schomaker, S. A., Fernandez, M. A., & Armstrong, S. N. (2015). An exploratory investigation of levels of learning and learning efficiency between online and face-to-face instruction. Counseling Outcome Research and Evaluation, 6(1), 47–57. https://doi.org/10.1177/2150137815572148
Urofsky, R. I. (2013). The Council for Accreditation of Counseling and Related Educational Programs: Promoting quality in counselor education. Journal of Counseling & Development, 91(1), 6–14.
https://doi.org/10.1002/j.1556-6676.2013.00065.x
West, J. D., Bubenzer, D. L., Brooks, D. K., Jr., & Hackney, H. (1995). The doctoral degree in counselor education and
supervision. Journal of Counseling & Development, 74(2), 174–176.
https://doi.org/10.1002/j.1556-6676.1995.tb01846.x
Rebecca Scherer, PhD, NCC, ACS, CPC, is an assistant professor at St. Bonaventure University. Regina Moro, PhD, NCC, BC-TMH, LPC, LMHC, LCAS, is an associate professor at Boise State University. Tara Jungersen, PhD, NCC, CCMHC, LMHC, is an associate professor and department chair at Nova Southeastern University. Leslie Contos, NCC, CCMHC, LCPC, is a doctoral candidate at Governors State University. Thomas A. Field, PhD, NCC, CCMHC, ACS, LPC, LMHC, is an assistant professor at the Boston University School of Medicine. Correspondence may be addressed to Rebecca Scherer, B43 Plassman Hall, 3261 West State Road, St. Bonaventure, NY 14778, rscherer@sbu.edu.
Aug 18, 2020 | Volume 10 - Issue 3
Joshua D. Smith, Neal D. Gray
Each year TPC presents an interview with a seminal figure in counseling as part of its Lifetime Achievement in Counseling series. This year I am honored to introduce Dr. Mona Robinson. She identifies as a counselor with expertise in rehabilitation counseling, is among the distinguished faculty at Ohio University, and is an internationally recognized scholar. I am grateful to Dr. Joshua Smith and Dr. Neal Gray, who continue to bring the contributions and wisdom of leaders in the profession to TPC readers. Here they present a view to Dr. Robinson’s accomplishments throughout her career, along with her reflections on the CACREP and CORE merger and the evolution of the profession. —Amie A. Manis, Editor

Mona Robinson, PhD, LPCC-S, LSW, CRC, is a professor at Ohio University and Program Coordinator for both their Counselor Education Program and their Human Services Program. She is the Immediate Past Chair of the Department of Counseling and Higher Education. She holds a BS in psychology, an MA in rehabilitation counseling, and a PhD in rehabilitation services (Rehabilitation Counselor Education) from The Ohio State University. Dr. Robinson is a certified rehabilitation counselor, a licensed professional clinical counselor supervisor, and a licensed social worker.
Prior to her employment at Ohio University, Dr. Robinson served as a counselor and administrator of vocational rehabilitation counseling and employment services to clients with severe mental illness and other barriers to employment. Additionally, she served as a consultant and adjunct professor at Wilberforce University. Her areas of expertise include psychiatric rehabilitation, disability advocacy, multicultural counseling, ethics, and dual diagnosis.
Dr. Robinson serves as the institute director for study abroad programs held in Italy and Botswana. She is currently 1st Vice President for the National Council on Rehabilitation Education, Accessibility Coordinator for the Association for Multicultural Counseling and Development 2019 Summit, and a member of their 2019 Day of Service Committee. She has served as Past President of the National Association of Multicultural Rehabilitation Concerns, Ohio Rehabilitation Association, and Ohio Rehabilitation Counseling Association. She is a past board member of the National Rehabilitation Association and the Ohio Counseling Association Executive Council, and a Past President and Past Secretary of the Central Ohio Counseling Association.
In addition to her extensive professional service, she is also a current member of numerous professional organizations, including but not limited to the American Counseling Association, American Rehabilitation Counseling Association, Association for Multicultural Counseling and Development, National Rehabilitation Counseling Association, Ohio Rehabilitation Association, and Ohio Rehabilitation Counseling Association. She is on the editorial boards of the Journal of Applied Rehabilitation Counseling and the International Journal of Applied Guidance and Counseling, a Vocational Expert for the Social Security Administration Office of Hearing Operations, and a Site Team Chair for the Council for Accreditation of Counseling and Related Educational Programs (CACREP).
Dr. Robinson’s awards and honors include the 2008 and 2014 Ohio University College of Education Distinguished Faculty Graduate Teaching Award; the 2009 Sylvia Walker Multicultural Education Award; and the 2010 Visiting Scholar to South Korea Award, through which she taught global communication at the Kyungpook National University. She was a presenter at the 2012 International Conference on Education in Honolulu, Hawaii, and a speaker at the 2017 4th Biennial Bhutan International Counseling Conference held in Thimphu, Bhutan. Dr. Robinson has been the recipient of the 2014 Ohio University College of Education Distinguished Faculty Outstanding Outreach Award, the 2016 and 2017 Ohio University Faculty Newsmakers Award, the 2017 Virgie Winston-Smith Lifetime Achievement Award, and a 2018 National Association of Multicultural Rehabilitation Concerns Fellow Award. Dr. Robinson was an invited speaker at the University of Botswana in 2017 and 2019 for the Ultimate Motivational Speaker Competition. Lastly, she was the keynote speaker for the Seminar on Guidance and Counseling Conference held in Yogyakarta, Indonesia, in October 2019.
In this interview, Dr. Robinson shares insights on growth and change within the counseling profession, her experience as a woman of color in counselor education, and her outlook on the future development of the profession.
- As a rehabilitation counselor educator, how has the merger between the Council on Rehabilitation Education (CORE) and CACREP impacted your role and the counseling profession?
For me personally, I am pleased to see the merger finally come to fruition. In the past, I worked as a vocational rehabilitation counselor and a licensed professional clinical counselor, so I certainly see the value of both specialty areas. I view myself as a counselor with a specialty area in clinical rehabilitation counseling. I am fortunate to work in a program that has historically integrated clinical mental health counseling, rehabilitation counseling, and school counseling at the master’s level. Holding accreditation with both CORE and CACREP meant we had to go through the accreditation process twice. However, since the merger occurred, we now have one accreditation cycle and our students can obtain credentialing under CACREP for both clinical mental health and rehabilitation counseling.
With respect to the counseling profession, I continue to be involved in discussions regarding the merger, including the revisions to the 2023 CACREP standards, particularly as they relate to clinical rehabilitation counseling. For the purpose of clarification, I think it is noteworthy to mention that rehabilitation counselors receive the same general training as clinical mental health counselors with the exception of diagnosis and treatment of mental and emotional disorders. Traditional rehabilitation counselor training focuses on vocational rehabilitation, specifically as it relates to assisting people with physical and mental disabilities in obtaining meaningful employment and/or independent living opportunities that improve their quality of life. Clinical rehabilitation counselor training would continue to focus on vocational rehabilitation with the inclusion of a clinical mental health counselor curriculum that focuses on treating mental and emotional disorders that lead to licensure as a professional clinical counselor as well as certification as a certified rehabilitation counselor.
Over the years, I presented at national conferences regarding the advantages and disadvantages of the merger. One of the main points of contention in the field of rehabilitation counseling centers around the lack of coursework necessary to treat and diagnose mental and emotional disabilities, including completing an internship in a setting that treats and diagnoses mental and emotional conditions. I firmly believe that the counseling profession as a whole will benefit from the merger with the infusion of clinical rehabilitation standards. This is a first step toward standardization so that all counseling programs can offer the same educational requirements that lead to licensure. Having a standardized counseling program will aid licensure portability as well as serve as a precursor to a national license for counselors. Counseling students reap the benefits of being taught by counselor educators with multiple specialty areas. Rehabilitation counselor educators play a pivotal role in teaching students knowledge from their specialty areas in addition to the clinical mental health competencies.
- What are the benefits and challenges associated with that merger, and where do you see rehabilitation counseling going in the future?
Students in rehabilitation counseling programs will benefit from a more well-rounded education that gives them an opportunity to work with people with physical, mental, and emotional disabilities. Having this additional knowledge will prepare students to work in integrated medical and behavioral settings. Counselor educators who teach from a holistic approach allow students an opportunity to gain skills that will assist them in achieving better outcomes for their clients. In addition to the obvious time considerations, one accreditation cycle for all programs instead of two has positive financial implications for students and institutions alike. Some of the challenges associated with the merger include concerns that rehabilitation counselor educators may need to take additional counseling coursework to become eligible for licensure as a professional clinical counselor. Currently, rehabilitation counseling professionals who teach in rehabilitation counselor programs come from varying backgrounds, including vocational rehabilitation counselors (public and private sector), rehabilitation specialists, physical therapists, and occupational therapists; while beneficial to rehabilitation counseling, they may not be eligible to become licensed as professional clinical counselors without taking additional courses or obtaining another degree. Additionally, there are concerns about rehabilitation counselors losing their professional identity. Therefore, adopting a curriculum that focuses on vocational rehabilitation learning outcomes while infusing clinical mental health learning outcomes will aid in alleviating these fears. Long term, a reunification of the rehabilitation counseling professions (i.e., rehabilitation counselor educators, vocational rehabilitation counselors, rehabilitation specialists, physical therapists, and occupational therapists) will need to happen, as splintering of the profession occurred well before the CORE and CACREP merger process began. It is my hope that the merger will bring about changes in counseling that are beneficial for all counseling professionals.
- What do you consider to be your major contribution to the development of the counseling profession and why?
Increasing faculty diversity as well as student diversity has been a cornerstone of my contribution to the development of the counseling profession. I have been intentional about recruiting AND retaining diverse students and faculty worldwide. The counseling profession has historically been predominantly White. However, the clients that present for counseling continue to come from increasingly diverse backgrounds. Hence, recruitment and retention of African American students and faculty are essential in the 21st century to meet the needs of diverse client populations. Therefore, I will continue to present and publish on the topic of diversity and the need to be responsive to all aspects of diversity. Undertaking my mission to speak about the necessity to respect diversity not only in conversation but also through action is an endeavor that I will continue to pursue.
Another contribution of mine is mentorship. When working in academia, one of the most valuable resources faculty members can acquire is a mentor. Personal relationships and support systems are important factors for a successful career. I believe that participation in formal and informal networks and mentoring relationships is critical in the persistence of African American female faculty in the academy. Mentors provide support, guidance, information, and advice to their mentees who may be struggling with career advancement. A mentor can serve as a support system for a faculty member by providing protection, coaching, and even validation for them through acceptance, friendship, and role modeling.
I believe in the importance of mentoring counselors, students, and faculty. While recruitment is important, retention efforts are even more crucial. I have spent countless hours focusing on the recruitment and retention of African American students and faculty. Additionally, I enjoy speaking locally, nationally, and internationally about issues that affect people of color, including those with varying disabilities. While licensed professional clinical counselors are trained to work with people with mental and emotional conditions, they often lack knowledge to effectively assist people with physical disabilities. I have been fortunate to fill the gap by providing trainings in this area.
- What three challenges to the counseling profession as it exists today concern you most?
Despite the fact that counseling has been a helping profession for decades, it still lags behind social work and psychology in terms of recognition as a profession. If the counseling profession aspires to obtain the same status as other helping professions such as social work and psychology, we must utilize our specialty areas as one cohesive profession. Social workers have done this successfully for decades through being known by the profession first, and then by their specialty areas. For example, someone may seek out a medical social worker that works in a hospital setting. In essence, the setting determines the specialty area of the social worker; counseling should consider adopting the same process. Counselor training is frequently viewed as not being on par with psychology. Therefore, adopting a standardized curriculum for training counselors will aid in eradicating this myth.
Another challenge is the lack of access to billing for Medicare on the part of counselors. Part of the reason for this disparity is that counselors are not viewed as having the appropriate training to serve as professional helpers similar to social workers and psychologists. While the need for trained professionals continues to increase, counseling has not been embraced by the mainstream. Efforts are underway to achieve parity that will allow counselors to bill Medicare—to date, this has not happened. Again, adopting a standardized curriculum will increase the likelihood of counselors serving as vendors for Medicare.
A third area of concern is the looming financial crisis that many institutions of higher learning face. Declining enrollments and increasing tuition costs make recruiting and retaining quality students and faculty a challenge. More attention should be given to offering alternatives to traditional classroom settings as a way to reach more students. Developing and implementing a curriculum that appeals to a broader audience is one way to attract diverse faculty and students. Institutions that offer welcoming environments and appreciate differences will be at the forefront of any future growth.
- What needs to change in the counseling profession for these three concerns to be successfully resolved?
I think it will be important for the counseling profession to take the time to respect diversity in all forms, not only in language but also in action. More unification is necessary between disciplines. Embracing an approach that demonstrates that we are ALL counselors first will be an important first step toward unification of the profession. Professional conferences should be inclusive of all specialty areas when offering sessions. Counselors should take the time to learn about other specialties. We show ourselves as a much stronger profession if we train counselors who can provide services to a diverse population, and that includes meeting the needs of people with disabilities.
With respect to billing parity, counselors should band together to advocate for Medicare. Standing as one unified profession will allow our voices to be heard on a broader scale. Finally, offering a diverse curriculum that meets the needs of underrepresented and underserved populations will aid in increasing enrollment in institutions of higher learning.
- As a woman of color, what has been your experience in counselor education? What advice would you give to others from your experience?
I am thankful for my position and experiences as a counselor educator. I have had many experiences that most counselors do not get to have, and for that I am eternally grateful. I have had the opportunity to travel all over the country and abroad. My entire career as a counselor educator has consisted of working at a predominately White institution (PWI). I believe my training at a Research I PWI contributed to my gaining access to my position. I was fortunate to have mentors who advocated on my behalf and helped open doors that probably would not have been opened otherwise. I worked my way up from an assistant professor to a professor over a 10-year period. I served as the first African American department chair in the College of Education. Throughout my tenure, I actively recruited diverse students and faculty to the university. I had to work harder to prove I was as qualified as the dominant culture. I’ve had decisions challenged as well as faced harassment simply because of the color of my skin. At the end of the day, I’ve learned to do my best and not worry about it. The advice I would give to others based upon my experiences is to be the best you can be and do not let anyone make you feel that you are less—know your self-worth. I always share these words with my mentees: “We have to be better.” Last but not least, self-care!
- If you were advising current counseling leaders, what advice would you give them about moving the counseling profession forward?
Unity makes strength. If we stand together as a profession, we will remain relevant. Advocate for the profession as a whole. Be knowledgeable about Medicare and other issues that affect our profession. Be a part of advocacy efforts that benefit all counselors. Be open-minded to being a counselor first with varying specialty areas. Listen to the concerns of the members of our professional counseling organizations, and finally, recruit students—they are our future!
This concludes the fifth interview for the annual Lifetime Achievement in Counseling Series. TPC is grateful to Joshua D. Smith, PhD, NCC, and Neal D. Gray, PhD, for providing this interview. Joshua D. Smith is a counselor at the Center for Emotional Health in Concord, North Carolina. Neal D. Gray is a professor and Chair of the School of Counseling and Human Services at Lenoir-Rhyne University. Correspondence can be emailed to Joshua Smith at jsmit643@uncc.edu.


