Cross-Validation of the Mental Distress Response Scale: Implications for Counselors
Michael T. Kalkbrenner
College counselors work collaboratively with professionals in a variety of disciplines in higher education to coordinate gatekeeper training to prepare university community members to recognize and refer students in mental distress to support services. This article describes the cross-validation of scores on the Mental Distress Response Scale (MDRS), a questionnaire for appraising university community members’ responses to encountering a student in mental distress, with a sample of faculty members. A confirmatory factor analysis revealed the dimensions of the MDRS were estimated adequately. Results also revealed demographic differences in faculty members’ responses to encountering a student in mental distress. The MDRS has implications for augmenting the outreach efforts of college counselors. For example, the MDRS has potential utility for enhancing campus-wide mental health screening efforts. The MDRS also has implications for supporting psychoeducation efforts, including gatekeeper training workshops, for professional counselors practicing in college settings.
Keywords: Mental Distress Response Scale, mental health, college counselors, gatekeeper, outreach
College counselors play crucial roles in supporting students’ personal, social, and academic growth, as well as students’ success (Golightly et al., 2017). Outreach and prevention programming, including campus violence prevention and supporting college student mental health, are two key elements in the practice of college counselors (Brunner et al., 2014; Golightly et al., 2017). Addressing these two key areas has become increasingly challenging in recent years because of the prevalence of campus violence incidents, including mass shootings in the most severe cases, and the frequency of mental health distress among college students, which has increased substantially since the new millennium (Auerbach et al., 2016; Barrett, 2014; Vieselmeyer et al., 2017). In fact, supporting college student mental health has become one of the greatest challenges that institutions of higher education are facing (Reynolds, 2013).
Most college students suffering from mental health issues do not seek treatment (Downs & Eisenberg, 2012). In response, college counselors, student affairs professionals, and higher education administrators are working collaboratively to develop and implement mental health awareness initiatives and gatekeeper training workshops, which include training university community members (e.g., students, faculty, and staff) as referral agents to recognize and refer students who are showing warning signs for suicide or other mental health issues to support services (Albright & Schwartz, 2017; Hodges et al., 2017). Faculty members are particularly valuable referral agents, as they tend to interact with large groups of students on frequent occasions, and they generally report positive attitudes about supporting college student mental health (Albright & Schwartz, 2017; Kalkbrenner, 2016).
Despite the utility of faculty members as gatekeepers for recognizing and referring students to the university counseling center and to other resources, the results of a recent national survey indicated that a significant proportion of faculty members (63%) do not refer a student in mental distress to support services (Albright & Schwartz, 2017). The literature is lacking research on how faculty members are likely to respond to encountering a student in mental distress, including but not limited to making a faculty-to-student referral to mental health support services. The primary aim of this investigation was to confirm the psychometric properties of the Mental Distress Response Scale (MDRS), a screening tool for measuring university community members’ responses to encountering a student in mental distress. Past investigators validated the MDRS for use with 4-year university students (Kalkbrenner & Flinn, 2020) and community college students (Kalkbrenner, 2019). If found valid for use with faculty members, college counselors could find the MDRS useful for screening and promoting faculty-to-student mental health support. A review of the extant literature is provided in the following section.
Mental Health and the State of Higher Education
Active shooter incidents on college campuses are some of the most tragic events in American history (Kalkbrenner, 2016). The 2015 massacre that occurred on a college campus in Oregon received attention at the highest level of government; former President Barack Obama urged the nation to decide when voting “whether this cause of continuing death for innocent people should be a relevant factor.” (Vanderhart et al., 2015, section A, p. 1). Seung-Hui Cho was a perpetrator of another one of these tragedies at Virginia Polytechnic Institute in 2007. According to Cho’s mother, he had a history of social isolation and unresolved mental health issues (Klienfield, 2007). Without treatment, the effects of mental health disorders can be debilitating and widespread for students, including impairments in academic functioning, attrition, self-harm, social isolation, and suicide or homicide in the most serious cases (Kalkbrenner, 2016; Shuchman, 2007). The early detection and treatment of students who are at risk for mental health disorders is a harm-prevention strategy for reducing campus violence incidents and promoting college student mental health (Futo, 2011; Kalkbrenner, 2016). Consequently, the practice of college counselors involves deploying outreach and systems-level mental health support interventions (Albright & Schwartz, 2017; Brunner et al., 2014; Golightly et al., 2017).
The Role of College Counselors in Providing Systems-Level Interventions
Providing individual counseling is a key role of college counselors (Golightly et al., 2017). In recent years, however, the practice of college counselors has been extended to providing systems-level and preventative mental health interventions to meet the growing mental health needs of college student populations (Brunner et al., 2014; Golightly et al., 2017). In particular, college counselors and their constituents engage in both campus-wide and targeted prevention and outreach programs (Golightly et al., 2017; Lynch & Glass, 2019), including gatekeeper training workshops to prepare university community members as referral agents or train them to recognize and refer students at risk for suicide and other mental health issues to the university counseling center (Albright & Schwartz, 2017; Brunner et al., 2014). These collaborative, educative, and preventative efforts are particularly crucial given the increase in both the severity and complexity of mental health disorders among college students (Gallagher, 2015; Reetz et al., 2016). The findings of past investigators suggest that faculty members are particularly viable referral agents for recognizing and referring students in mental distress to the counseling center (Kalkbrenner, 2016; Margrove et al., 2014).
Faculty Members as Referral Agents
Faculty members have a propensity to serve as referral agents (i.e., recognize and refer students in mental distress to resources) because of their frequent contact with students and their generally positive attitudes and willingness to support their students’ mental and physical wellness (Albright & Schwartz, 2017). Albright and Schwartz (2017) found that approximately 95% of faculty members and staff considered connecting students in mental distress to resources as one of their roles and responsibilities. Similarly, Margrove et al. (2014) found that 64% of untrained university staff members expressed a desire to receive training to recognize warning signs of mental health disorders in students.
Past investigators extended the line of research on the utility of faculty members as gatekeepers by identifying demographic differences by gender and help-seeking history (previous attendance in counseling) in faculty members’ tendency to support college student mental health (Kalkbrenner & Carlisle, 2019; Kalkbrenner & Sink, 2018). In particular, Kalkbrenner and Sink (2018) identified gender as a significant predictor of faculty-to-student counseling referrals, with faculty who identified as female more likely to make faculty-to-student referrals to the counseling center compared to their male counterparts. Similarly, Kalkbrenner and Carlisle (2019) found that faculty members’ awareness of warning signs for mental distress in students was a significant positive predictor of faculty-to-student referrals to the counseling center. In addition, faculty members with a help-seeking history (previous attendance in counseling) were significantly more aware of warning signs for mental distress in their students compared to faculty without a help-seeking history (Kalkbrenner & Carlisle, 2019).
Faculty Members’ Responses to Encountering a Student in Mental Distress
Despite the growing body of literature on institutional agents’ participation in gatekeeper training (i.e., recognize and refer), research on the measurement and appraisal of how faculty members are likely to respond when encountering a student in mental distress is in its infancy. The results of a recent national survey of college students (N = 51,294) and faculty members (N = 14,548) were troubling, as 63% of faculty members did not refer a student in psychological distress to mental health support services (Albright & Schwartz, 2017). Making a referral to the university counseling center is one possible response of students and faculty members to encountering a peer or student in mental distress (Kalkbrenner & Sink, 2018). However, the findings of Albright and Schwartz (2017) highlight a gap in the literature regarding how university community members are likely to respond when encountering a student in mental distress, including but not limited to making a faculty-to-student referral to the college counseling center.
To begin filling this gap in the literature, Kalkbrenner and Flinn (2020) developed, validated, and cross-validated scores on the MDRS to assess 4-year university students’ responses to encountering a student in mental distress, including but not limited to making a referral to mental health support services. In a series of two major phases of psychometric analyses, Kalkbrenner and Flinn identified and confirmed two dimensions or subscales of the MDRS, including Diminish/Avoid and Approach/Encourage, with two large samples of undergraduate students. The Diminish/Avoid subscale measures adverse or inactive responses of university community members to encountering a student in mental distress (e.g., stay away from the person or warn the person that mental issues are perceived as a weakness). The Approach/Encourage subscale appraises facilitative or helpful responses of university community members when encountering a student in mental distress that are likely to help connect the person to resources (e.g., talking to a college counselor or suggesting that the person go to the campus counseling or health center). However, the psychometric properties of the MDRS have not been tested with faculty members. If found valid for such purposes, the MDRS could be a useful tool that college counselors and their constituents can use to screen and promote faculty-to-student referrals to mental health support services. In particular, the following research questions were posed: (1) Does the two-dimensional hypothesized MDRS model fit with a sample of faculty members? and (2) To what extent are there demographic differences in faculty members’ responses to encountering a student in mental distress?
Method
Participants and Procedures
Data were collected electronically from faculty members using Qualtrics, a secure e-survey platform. A nonprobability sampling procedure was used by sending a recruitment email message with an electronic link to the survey to 1,000 faculty members who were teaching at least one course at a research-intensive, mid-Atlantic public university at the time of data collection. A total of 221 faculty members clicked on the electronic link to the survey and 11 responses were omitted from the data set because of 100% missing data, resulting in a useable sample size of 210, yielding a response rate of 21%. This response rate is consistent with the response rates of other investigators (e.g., Brockelman & Scheyett, 2015; Kalkbrenner & Carlisle, 2019) who conducted survey research with faculty members. For gender, 58% (n = 122) identified as female, 41% (n = 86) as male, and 0.5% (n = 1) as non-binary or third gender, and 0.5% (n = 1) did not specify their gender. For ethnicity, 79.0% (n = 166) identified as Caucasian, 6.2% (n = 11) as African American, 3.8% (n = 8) as Hispanic or Latinx, 2.9% (n = 6) as Asian, 2.9% (n = 6) as multiethnic, 0.5% (n = 1) as Hindu, and 0.5% (n = 1) as Irish, and 5.2% (n = 11) did not specify their ethnic identity. Participants ranged in age from 31 to 78 (M = 50; SD = 11). Participants represented all of the academic colleges in the university, including 28.6% (n = 60) Arts and Letters, 22.9% (n = 48) Education, 18.1% (n = 38) Sciences, 12.9% (n = 27) Health Sciences, 9% (n = 19) Engineering and Technology, and 7.6% (n = 16) Business, while 1% (n = 2) of participants did not specify their college.
Instrumentation
Demographic questionnaire
Following informed consent, participants were asked to indicate that they met the inclusion criteria for participation, including (1) employment as a faculty member, and (2) teaching at least one course at the time of data collection. Participants then responded to a succession of demographic items about their gender, ethnicity, age, academic college, and highest level of education completed. Lastly, respondents indicated their rank and help-seeking history (previous attendance in counseling or no previous attendance in counseling) and if they had referred at least one student to mental health support services.
Mental Distress Response Scale (MDRS)
The MDRS is a screening tool comprised of two subscales (Approach/Encourage and Diminish/Avoid) for measuring university community members’ responses to encountering a student in mental distress (Kalkbrenner & Flinn, 2020). The items that mark the Approach/Encourage subscale appraise responses to mental distress that are consistent with providing support and encouragement to a student in mental distress (e.g., “suggest that they go to the health center on campus”). The Diminish/Avoid subscale measures adverse or inactive responses to encountering a student in mental distress (e.g., “try to ignore your concern”). Kalkbrenner and Flinn (2020) found adequate reliability evidence for an attitudinal measure (α > 0.70) and initial validity evidence for the MDRS in two major phases of analyses (exploratory and confirmatory factor analysis [CFA]) with two samples of college students. Kalkbrenner (2019) extended the line of research on the utility of the MDRS for use with community college students and found adequate reliability (α > 0.80) and validity evidence (single and multiple-group confirmatory analysis).
Data Analysis
A CFA based on structural equation modeling was computed using IBM SPSS Amos version 25 to cross-validate scores on the MDRS with a sample of faculty members (research question #1). Using a maximum likelihood estimation method, the following goodness-of-fit indices and thresholds for defining model fit were investigated based on the recommendations of Byrne (2016) and Hooper et al. (2008): Chi square absolute fit index (CMIN, non-significant p-value with an x2/df ratio < 3), comparative fit index (CFI > 0.95), incremental fit index (IFI > 0.95), Tucker-Lewis index (TLI > 0.95), goodness-of-fit index (GFI > 0.95), root mean square error of approximation (RMSEA < 0.07), and standardized root mean square residual (SRMR < 0.08). Based on the findings of past investigators (e.g., Kalkbrenner & Sink, 2018) regarding demographic differences in faculty members’ propensity to support college student mental health, a 2 X 2 (gender X help-seeking history) MANOVA was computed to investigate demographic differences in faculty members’ responses to encountering a student in mental distress (research question #2). The independent variables included gender (male or female) and help-seeking history (previous attendance in counseling or no previous attendance in counseling). Discriminant analysis was used as the post hoc procedure for significant findings in the MANOVA (Warne, 2014). The researcher examined both main effects and interaction effects and applied Bonferroni adjustments to control for the familywise error rate.
Results
CFA
The researcher ensured that the data set met the necessary assumptions for CFA (Byrne, 2016; Field, 2018). A missing values analysis revealed that less than 5% of data was missing for all MDRS items. Little’s Missing Completely at Random (MCAR) test revealed that the data was missing at random: χ2 (387) = 407.98, p = 0.22. Expectation maximization was used to impute missing values. Outliers were winsorized (Field, 2018) and skewness and kurtosis values for the MDRS items (see Table 1) were largely consistent with a normal distribution (+ 1; Mvududu & Sink, 2013). Inter-item correlations between the 10 items were favorable for CFA, and Mahalanobis d2 indices revealed no extreme multivariate outliers. The researcher ensured that the sample size was sufficient for CFA by following the guidelines provided by Mvududu and Sink (2013), including at least 10 participants per estimated parameter with a sample > 200.
Table 1
Descriptive Statistics for MDRS Items
| Item Content | M | SD | Skew | Kurtosis |
| 1. I would stay away from this person | 49.83 | 9.46 | 1.11 | 0.22 |
| 2. Suggest that they go to the health center on campus | 50.15 | 9.48 | -0.60 | -0.08 |
| 3. Try to ignore your concern | 49.74 | 9.08 | 1.07 | 1.08 |
| 4. Take them to a party | 49.21 | 3.11 | 0.70 | 0.81 |
| 5. Tell them to “tough it out” because they will feel better over time | 49.73 | 8.94 | 1.32 | 1.26 |
| 6. Suggest that they see a medical doctor on campus | 50.00 | 9.98 | -0.24 | -0.06 |
| 7. Avoid this person | 49.70 | 9.02 | 1.80 | 1.33 |
| 8. Suggest that they see a medical doctor in the community | 50.00 | 9.98 | -0.49 | -0.10 |
| 9. Warn the person that others are likely to see their mental health issues as a weakness | 49.31 | 7.14 | 1.90 | 1.59 |
| 10. Talk to a counselor about your concern | 50.00 | 9.97 | -0.83 | 0.15 |
SEKurtosis = 0.15, SESkewness = 0.17.
Note. Values were winsorized and reported as standardized t-scores (M = 50; SD = 10).
The 10 MDRS items (see Table 1) were entered in the CFA. A strong model fit emerged based on the GFI recommended by Byrne (2016) and Hooper et al. (2008). The CMIN absolute fit index demonstrated no significant differences between the hypothesized model and the data: χ2 (34) = 42.41, p = 0.15, CMIN/df = 1.25. In addition, the CFI = 0.98, GFI = 0.96, IFI = 0.98, TLI = 0.98, RMSEA = 0.03, 90% confidence interval [<.00, .06], and SRMR = 0.05 also demonstrated a strong model fit. Internal consistency reliability analyses (Cronbach’s coefficient alpha) revealed satisfactory reliability coefficients for an attitudinal measure, Diminish/Avoid (α = 0.73) and Approach/Encourage (α = 0.70). In addition, the path model coefficient (-0.04) between factors supported the structural validity of the scales (see Figure 1).
Figure 1
Confirmatory Factor Analysis Path Diagram for the Mental Distress Response Scale
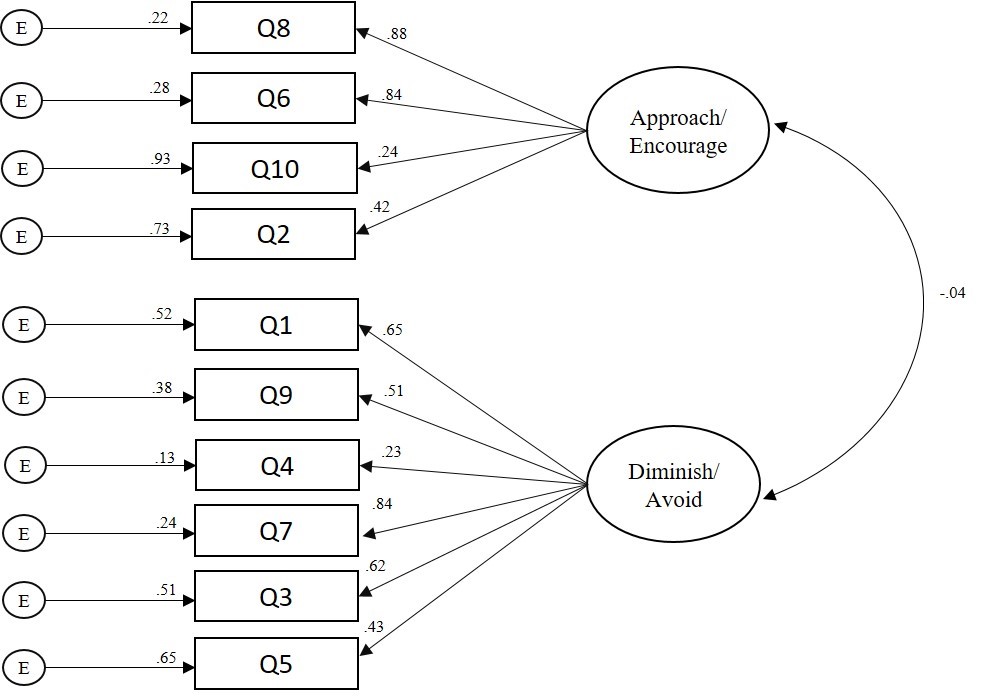
Note. CFA = confirmatory factor analysis, MDRS = Mental Distress Response Scale.
Multivariate Analysis
A 2 X 2 (gender X help-seeking history) MANOVA was computed to investigate demographic differences in faculty members’ responses to encountering a student in mental distress (research question #2). G*Power was used to conduct an a priori power analysis (Faul et al., 2007) and revealed that a minimum sample size of 151 would provide a 95% power estimate, α = .05, with a moderate effect size, F2(v) = 0.063. A significant main effect emerged for gender: F(3, 196) = 8.27, p < 0.001, Wilks’ λ = 0.92, = 0.08. The MANOVA was followed up with a post hoc discriminant analysis based on the recommendations of Warne (2014). The discriminant function significantly discriminated between groups: Wilks’ λ = 0.91, X2 = 18.85, df = 2, p < 0.001. The correlations between the latent factors and discriminant function showed that Diminish/Avoid loaded more strongly on the function (r = 0.98) than Approach/Encourage (r = 0.29), suggesting that Diminish/Avoid contributed the most to group separation in gender. The mean discriminant score on the function was -0.27 for participants who identified as female and 0.37 for participants who identified as male.
Discussion
The results of tests of internal consistency reliability (Cronbach’s coefficient alpha), CFA, and correlations between factors supported the psychometric properties of the MDRS with a sample of faculty members. The results of the CFA were promising as GFI demonstrated a strong model fit between the two-dimensional hypothesized MDRS model and a sample of faculty members (research question #1). In particular, based on one of the most conservative and rigorous absolute fit indices, the CMIN (Byrne, 2016; Credé & Harms, 2015), the researchers retained the null hypothesis—there were no significant differences between the hypothesized factor structure of the MDRS and a sample of faculty members. The strong model fit suggests that Approach/Encourage and Diminish/Avoid are two latent variables that comprise faculty members’ responses to encountering a student in mental distress. The findings of the CFA add to the extant literature about the utility of the MDRS for use with 4-year university students (Kalkbrenner & Flinn, 2020), community college students (Kalkbrenner, 2019), and now with faculty members.
An investigation of the path model coefficient between subscales (see Figure 1) revealed a small and negative association between factors, which supports the structural validity of the MDRS. In particular, the low and negative relationship between the Approach/Encourage and Diminish/Avoid subscales indicates that the dimensions of the MDRS are measuring discrete dimensions of a related construct. As expected, faculty members who scored higher on the Approach/Encourage subscale tended to score lower on the Diminish/Avoid subscale. However, the low strength of the association between factors suggests that faculty members’ responses to encountering a student in mental distress might not always be linear (e.g., a strong positive approach/encourage response might not always be associated with a strong negative diminish/avoid response). Haines et al. (2017) demonstrated that factors in the environment and temperament of a person showing signs of mental distress were significant predictors of mental health support staff’s perceptions of work safety. It is possible that under one set of circumstances faculty members might have an approach/encourage response to mental distress. However, under a difference set of circumstances, a faculty member might have a diminish/avoid response. For example, the extent to which a faculty member feels threatened or unsafe might mediate their propensity of having diminish/avoid or approach/encourage responses. Future research is needed to evaluate this possibility.
Consistent with the findings of previous researchers (Kalkbrenner & Carlisle, 2019; Kalkbrenner & Sink, 2018), the present investigators found that faculty members who identified as male were more likely to report a diminish/avoid response to encountering a student in mental distress compared to female faculty members. Similarly, Kalkbrenner and Sink (2018) found that male faculty members were less likely to make faculty-to-student referrals to the counseling center, and Kalkbrenner and Carlisle (2019) found that male faculty members were less likely to recognize warning signs of mental distress in college students. Similarly, the multivariate results of the present investigation revealed that male faculty members were more likely to report a diminish/avoid response to encountering a student in mental distress when compared to female faculty members. The synthesized findings of Kalkbrenner and Carlisle (2019), Kalkbrenner and Sink (2018), and the present investigation suggest that faculty members who identify as male might be less likely to recognize and refer a student in mental distress to mental health support services. The MDRS has valuable implications for enhancing the practice of professional counselors in college settings.
Implications for Counseling Practice
Outreach, consultation, and psychoeducation are essential components in the practice of college counselors (Brunner et al., 2014; Golightly et al., 2017). The findings of the present investigation have a number of practical implications for enhancing college counselors’ outreach and psychoeducation work—for example, gatekeeper workshops geared toward promoting faculty-to-student referrals to mental health support resources. The complex and multidimensional nature of college student mental health issues calls for interdisciplinary collaboration between college counselors and professionals in a variety of disciplinary orientations in higher education (Eells & Rockland-Miller, 2011; Hodges et al., 2017). College counselors can take leadership roles in coordinating these collaborative efforts to support college student mental health. In particular, college counselors can work with student affairs officials, higher education administrators, and their constituents, and attend new faculty orientations as well as department meetings to administer the MDRS, establish relationships with faculty, and discuss the benefits of gatekeeper training as well as supporting college student mental health. The results of the MDRS can be used to gain insight into the types of responses that faculty members are likely to have when encountering a student in mental distress. This information can be used to structure the content of gatekeeper training workshops aimed at promoting faculty-to-student referrals to mental health support services. Specifically, college counselors might consider the utility of integrating brief interventions and skills training components into gatekeeper training workshops. Motivational interviewing, for example, is an evidence-based, brief approach to counseling that includes both person-centered and directive underpinnings with utility for increasing clients’ intrinsic motivation to make positive changes in their lives (Iarussi, 2013; Resnicow & McMaster, 2012). Professional counselors who practice in higher education are already using motivational interviewing to promote college student development and mental health (Iarussi, 2013). Although future research is needed, integrating motivational interviewing principles (e.g., expressing empathy, rolling with resistance, developing discrepancies, and supporting self-efficacy; Iarussi, 2013) into gatekeeper training workshops might increase faculty members’ commitment to supporting college student mental health.
The MDRS has the potential to enhance college counselors’ outreach and mental health screening efforts (Golightly et al., 2017). College counselors can incorporate the MDRS into batteries of pretest/posttest measures (e.g., the MDRS with a referral self-efficacy measure) for evaluating the effectiveness of mental health awareness initiatives and gatekeeper training programs for faculty and other members of the campus community. If administered widely, the MDRS might have utility for assessing faculty members’ responses to students in mental distress across time and among various campus ecological systems, providing data to drive the prioritization and allocation of outreach efforts aimed at facilitating and maintaining referral networks for connecting students in mental distress to support services.
The results of the present study have policy implications related to campus violence prevention programming. The sharp increase in campus violence incidents has resulted in several universities implementing threat assessment teams as a harm-prevention measure (Eells & Rockland-Miller, 2011). Threat assessment teams involve an interdisciplinary collaboration of university faculty and staff for the purposes of recognizing and responding to students who are at risk of posing a threat to themselves or to others. College counselors can take leadership roles in establishing and supporting threat assessment teams at their universities. College counselors can administer the MDRS to faculty and staff and use the results as one way to identify potential threat assessment team members. University community members who score higher on the Approach/Encourage scale might be inclined to serve on threat assessment teams because of their propensity to support college student mental health. The brevity (10 questions) and versatility of administration (paper copy or electronically via laptop, smartphone, or tablet) of the MDRS adds to the practicality of the measure. Specifically, it might be practical for college counselors and their constituents to administer the MDRS during new faculty orientations, annual opening programs, or department meetings, or via email to faculty and staff. Results can potentially be used to recruit threat assessment team members.
Our findings indicate that when compared to their female counterparts, male faculty members might be more likely to have a diminish/avoid response when encountering a student in mental distress. College counselors might consider working collaboratively with student affairs professionals to implement gatekeeper training and mental health awareness workshops in academic departments that are comprised of high proportions of male faculty members. It is possible that male faculty members are unaware of how to identify warning signs of mental distress in their students (Kalkbrenner & Carlisle, 2019). College counselors might consider the utility of distributing psychoeducation resources for recognizing students in mental distress to faculty and staff. As just one example, the REDFLAGS model is an acronym of eight red flags or warning signs for identifying students who might be struggling with mental health issues (Kalkbrenner, 2016). Kalkbrenner and Carlisle (2019) demonstrated that the REDFLAGS model is a promising psychoeducational tool, as faculty members’ awareness of the red flags was a significant positive predictor of faculty-to-student referrals to the counseling center. The REDFLAGS model appears to be a practical resource for college counselors that can be distributed to faculty electronically or by paper copy, or posted as a flyer (Kalkbrenner, 2016; Kalkbrenner & Carlisle, 2019).
Limitations and Future Research
The findings of the present study should be considered within the context of the limitations. A number of methodological limitations (e.g., self-report bias and social desirability) can influence the validity of psychometric designs. In addition, the dichotomous nature of the faculty-to-student counseling referral variable (referred or not referred) did not provide data on the frequency of referrals. Future researchers should use a continuous variable (e.g., the number of student referrals to the counseling center in the past 2 years) to appraise faculty-to-student referrals. Future researchers can further test the psychometric properties of the MDRS through cross-validating scores on the measure with additional, unique populations of faculty members from a variety of different geographic and social locations. Invariance testing can be computed to examine the degree to which the MDRS and its dimensions maintain psychometric equivalence across different populations of faculty members. In addition, the criterion validity of the MDRS can be examined by testing the extent to which respondents’ MDRS scores are predictors of their frequency of student referrals to the counseling center and to other resources. Furthermore, future qualitative research is needed to investigate faculty members’ unique experiences around supporting college student mental health.
The low and negative association between the Approach/Encourage and Diminish/Avoid subscales suggests that faculty members might have an approach/encourage response to encountering a student in mental distress under one set of circumstances; however, they might have a diminish/avoid response under a difference set of circumstances. Future investigators might test the extent to which attitudinal variables mediate respondents’ MDRS scores—for example, the extent to which faculty members’ sense of safety predicts their MDRS scores. In addition, given the widespread public perception of individuals living with mental illness as violent and dangerous (Varshney et al., 2016), future researchers might identify demographic and background differences (particularly mental health stigma) among participants’ MDRS scores.
Summary and Conclusion
Mental health outreach and screening are essential components in the practice of college counselors, including training referral agents to recognize and refer students who might be struggling with mental health distress to support services (Golightly et al., 2017). Taken together, the results of the present study indicate that the MDRS and its dimensions were estimated sufficiently with a sample of faculty members. Our findings confirmed the two-dimensional hypothesized model for the types of responses that faculty might have when encountering a student showing signs of mental distress. In particular, the results of a CFA provided support for the MDRS and its dimensions, confirming a two-dimensional construct for the types of responses (approach/encourage and diminish/avoid) that faculty members might have when encountering a student in mental distress. Considering the utility of faculty members as gatekeepers and referral agents (Hodges et al., 2017; Kalkbrenner, 2016), researchers, practitioners, and policymakers may find the MDRS a useful screening tool for identifying the ways in which faculty members are likely to respond when encountering a student in mental distress. Results can be used to inform the content of mental health awareness initiatives and gatekeeper training programs aimed at promoting approach/encourage responses to connect students who need mental health support to the appropriate resources.
Conflict of Interest and Funding Disclosure
The authors reported no conflict of interest
or funding contributions for the development
of this manuscript.
References
Albright, G. & Schwartz, V. (2017). Are campuses ready to support students in distress?: A survey of 65,177 faculty, staff, and students in 100+ colleges and universities. https://www.jedfoundation.org/wp-content/uploads/2017/10/Kognito-JED-Are-Campuses-Ready-to-Support-Students-in-Distress.pdf
Auerbach, R. P., Alonso, J., Axinn, W. G., Cuijpers, P., Ebert, D. D., Green, J. G., Hwang, I., Kessler, R. C., Liu, H., Mortier, P., Nock, M. K., Pinder-Amaker, S., Sampson, N. A., Aguilar-Gaxiola, S., Al-Hamzawi, A., Andrade, L. H., Benjet, C., Caldas-de-Almeida, J. M., Demyttenaere, K., . . . Bruffaerts, R. (2016). Mental disorders among college students in the World Health Organization World Mental Health Surveys. Psychological Medicine, 46, 2955–2970. https://doi.org/10.1017/S0033291716001665
Barrett, D. (2014, September 24). Mass shootings on the rise, FBI says. The Wall Street Journal. http://online.wsj.com/articles/mass-shootings-on-the-rise-fbi-says-1411574475
Brockelman, K. F., & Scheyett, A. M. (2015). Faculty perceptions of accommodations, strategies, and psychiatric advance directives for university students with mental illnesses. Psychiatric Rehabilitation Journal, 38, 342–348. https://doi.org/10.1037/prj0000143
Brunner, J. L., Wallace, D. L., Reymann, L. S., Sellers, J.-J., & McCabe, A. G. (2014). College counseling today: Contemporary students and how counseling centers meet their needs. Journal of College Student Psychotherapy, 28, 257–324. https://doi.org/10.1080/87568225.2014.948770
Byrne, B. M. (2016). Structural equation modeling with AMOS: Basic concepts, applications, and programming (3rd ed.). Routledge.
Credé, M., & Harms, P. D. (2015). 25 years of higher-order confirmatory factor analysis in the organizational sciences: A critical review and development of reporting recommendations. Journal of Organizational Behavior, 36, 845–872. https://doi.org/10.1002/job.2008
Downs, M. F., & Eisenberg, D. (2012). Help seeking and treatment use among suicidal college students. Journal of American College Health, 60, 104–114. https://doi.org/10.1080/07448481.2011.619611
Eells, G. T., & Rockland-Miller, H. S. (2011). Assessing and responding to disturbed and disturbing students: Understanding the role of administrative teams in institutions of higher education. Journal of College Student Psychotherapy, 25, 8–23. https://doi.org/10.1080/87568225.2011.532470
Faul, F., Erdfelder, E., Lang, A.-G., & Buchner, A. (2007). G*Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behavior Research Methods, 39, 175–191. https://doi.org/10.3758/BF03193146
Field, A. (2018). Discovering statistics using IBM SPSS Statistics (5th ed.). SAGE.
Futo, J. (2011). Dealing with mental health issues on campus starts with early recognition and intervention. Campus Law Enforcement Journal, 41, 22–23.
Gallagher, R. P. (2015). National survey of college counseling centers 2014. http://d-scholarship.pitt.edu/id/eprint/28178
Golightly, T., Thorne, K., Iglesias, A., Huebner, E., Michaelson-Chmelir, T., Yang, J., & Greco, K. (2017). Outreach as intervention: The evolution of outreach and preventive programming on college campuses. Psychological Services, 14, 451–460. https://doi.org/10.1037/ser0000198
Haines, A., Brown, A., McCabe, R., Rogerson, M., & Whittington, R. (2017). Factors impacting perceived safety among staff working on mental health wards. BJPsych Open, 3, 204–211.
https://doi.org/10.1192/bjpo.bp.117.005280
Hodges, S. J., Shelton, K., & King Lyn, M. M. (2017). The college and university counseling manual: Integrating essential services across the campus. Springer.
Hooper, D., Coughlan, J., & Mullen, M. R. (2008). Structural equation modelling: Guidelines for determining model fit. The Electronic Journal of Business Research Methods, 6, 53–60.
Iarussi, M. M. (2013). Examining how motivational interviewing may foster college student development. Journal of College Counseling, 16(2), 158–175. https://doi.org/10.1002/j.2161-1882.2013.00034.x
Kalkbrenner, M. T. (2016). Recognizing and supporting students with mental health disorders: The REDFLAGS Model. Journal of Education and Training, 3, 1–13. https://doi.org/10.5296/jet.v3i1.8141
Kalkbrenner, M. T. (2019). Peer-to-peer mental health support on community college campuses: Examining the factorial invariance of the Mental Distress Response Scale. Community College Journal of Research and Practice. https://doi.org/10.1080/10668926.2019.1645056
Kalkbrenner, M. T., & Carlisle, K. L. (2019). Faculty members and college counseling: Utility of The REDFLAGS Model. Journal of College Student Psychotherapy. https://doi.org/10.1080/87568225.2019.1621230
Kalkbrenner, M. T., & Flinn, R. F. (2020). Development, validation, and cross-validation of the Mental Distress Reaction Scale (MDRS). Journal of College Student Development.
Kalkbrenner, M. T., & Sink, C. A. (2018). Development and validation of the College Mental Health Perceived Competency Scale. The Professional Counselor, 8, 175–189. https://doi.org/10.15241/mtk.8.2.175
Kleinfield, N. R. (2007, April 22). Before deadly rage, a life consumed by a troubling silence. The New York Times. http://www.nytimes.com/2007/04/22/us/22vatech.html?pagewanted=all
Lynch, R. J., & Glass, C. R. (2019). The development of the Secondary Trauma in Student Affairs Professionals Scale (STSAP). Journal of Student Affairs Research and Practice, 56, 1–18.
https://doi.org/10.1080/19496591.2018.1474757
Margrove, K. L., Gustowska, M., & Grove, L. S. (2014). Provision of support for psychological distress by university staff, and receptiveness to mental health training. Journal of Further and Higher Education, 38, 90–106. https://doi.org/10.1080/0309877X.2012.699518
Mvududu, N. H., & Sink, C. A. (2013). Factor analysis in counseling research and practice. Counseling Outcome Research and Evaluation, 4, 75–98. https://doi.org/10.1177/2150137813494766
Reetz, D. R., Bershad, C., LeViness, P., & Whitlock, M. (2016). The Association for University and College Counseling Center Directors annual survey. https://www.aucccd.org/assets/documents/aucccd%202016%
20monograph%20-%20public.pdf
Resnicow, K., & McMaster, F. (2012). Motivational interviewing: Moving from why to how with autonomy support. International Journal of Behavioral Nutrition and Physical Activity, 9, 19.
https://doi.org/10.1186/1479-5868-9-19
Reynolds, A. L. (2013). College student concerns: Perceptions of student affairs practitioners. Journal of College Student Development, 54, 98–104. https://doi.org/ 10.1353/csd.2013.0001
Shuchman, M. (2007). Falling through the cracks—Virginia Tech and the restructuring of college mental health services. The New England Journal of Medicine, 357, 105–110. https://doi.org/10.1056/NEJMp078096
Vanderhart, D., Johnson, K., & Turkewitz, J. (2015, October 2). Oregon shooting at Umpqua College kills 10, sheriff says. The New York Times. https://www.nytimes.com/2015/10/02/us/oregon-shooting-umpqua-community-college.html?smid=pl-share
Varshney, M., Mahapatra, A., Krishnan, V., Gupta, R., & Deb, K. S. (2016). Violence and mental illness: What is the true story? Journal of Epidemiology & Community Health, 70, 223–225.
https://doi.org/10.1136/jech-2015-205546
Vieselmeyer, J., Holguin, J., & Mezulis, A. (2017). The role of resilience and gratitude in posttraumatic stress and growth following a campus shooting. Psychological Trauma: Theory, Research, Practice, and Policy, 9, 62–69. https://doi.org/10.1037/tra0000149
Warne, R. T. (2014). A primer on multivariate analysis of variance (MANOVA) for behavioral scientists. Practical Assessment, Research & Evaluation, 19(17), 1–10.
Michael T. Kalkbrenner, PhD, NCC, is an assistant professor at New Mexico State University. Correspondence can be addressed to Michael Kalkbrenner, 1220 Stewart St., OH202B, NMSU, Las Cruces, NM 88001, mkalk001@nmsu.edu.
