May 22, 2024 | Volume 14 - Issue 1
Ashley Ascherl Pechek, Kristin A. Vincenzes, Kellie Forziat-Pytel, Stephen Nowakowski, Leandrea Romero-Lucero
In counselor education programs, students acquire clinical experience through both practicum and internship; this time frequently marks students’ first counseling experiences working with suicide in a clinical context. Often, students in practicum or internship working with clients who may be experiencing suicidal ideations do not feel properly equipped to deal with suicide. This study aimed to develop a practice model for online counselor education programs that increases counseling students’ self-efficacy to work with clients who may present with suicidal ideations. Sixty online graduate-level clinical mental health counseling students completed a pre- and posttest self-efficacy assessment. Findings showed that students’ self-efficacy increased due to taking the online basic counseling skills class that included teaching activities related to suicide screening, assessment, and intervention.
Keywords: self-efficacy, suicide, assessment and intervention, online counselor education, practice model
Despite a growing body of research and evidence-based interventions, suicide remains the 11th leading cause of death in the United States (Centers for Disease Control and Prevention [CDC], 2021). A 2014 World Health Organization report (WHO; 2014) estimated that more lives were lost to suicide than to war, conflict, and natural disasters combined. More recently, the American Foundation for Suicide Prevention (AFSP; 2023) estimated that in 2021 there were 1.7 million suicide attempts; more than 48,000 Americans died by suicide. In 2023, trends showed about 130 suicides per day (AFSP, 2023).
To address the ongoing concern of suicide risk, counselor education programs are expected to prepare students for work with diverse clients who experience suicidal ideations (Wachter Morris & Barrio Minton, 2012). Specifically, the Council for the Accreditation of Counseling and Related Educational Programs (CACREP; 2023) requires counseling programs to provide counselors-in-training (CITs) with skills in crisis intervention, suicide prevention, and response models and strategies, as well as proper assessment and management of suicidal ideations. There are no consistent suicide prevention or intervention training standards or models among counselor education programs. Organizations such as the American Association of Suicidology have recommended that suicide knowledge and assessment be at the forefront of health care by having (a) graduate programs require suicide knowledge and skills acquisition in their curriculum, (b) state licensure boards require suicide-specific education for renewal of licenses, (c) government-funded health care systems and hospitals require staff training in suicide assessment and management, and (d) staff appropriately trained to assess, manage, or treat patients who experience suicidal thoughts (Schmitz et al., 2012).
The current study aimed to determine if a practice model used in an online basic counseling skills course was effective at increasing counseling students’ self-efficacy when working with clients who present with suicidal ideations. Results from the study were used to determine if the skills-based online course effectively taught suicide assessment and intervention skills to graduate students. Discussion and implications regarding the need to establish best practices in prevention and intervention training for CITs are included. Additional considerations are given for both online and brick-and-mortar counseling programs.
Competencies and Principles
To assist counselor educators with how to best address the ongoing concern of suicide risk in clients, the Suicide Prevention Resource Center (2006) identified several core competencies and skills needed to assess and manage individuals at risk for suicide. These competencies can be used as a framework for extensive suicide training (Granello, 2010). Other models, such as a core competency–based training workshop in suicide screening, assessment, and management, have been developed to assess the effectiveness of suicide training, including pre- and post-workshop self-assessments, evidence-based instruction, role-playing, expert demonstration, group discussions, and video-recorded risk assessments of trainees intended to provide feedback (Cramer et al., 2017). Together, these competencies and principles can be used to develop a practice model in graduate counselor education programs and to better assist CITs in preparing to work with a client experiencing suicidal thoughts.
Despite the Suicide Prevention Resource Center (2006) identifying core competencies and skills needed to properly assess and manage individuals for risk of suicide, the research from counseling graduate programs on the implementation of suicide training remains sparse (Wasylko & Stickley, 2007). Therefore, we looked at other graduate programs of similar disciplines (e.g., social work, school psychology, and school counseling) to gain a better idea of best practices in related fields. Unfortunately, literature related to best practices within graduate programs of similar disciplines also demonstrates a lack of training in suicide risk assessment and intervention (Becnel et al., 2021; LeCloux, 2021; Liebling-Boccio & Jennings, 2013). This expanded look into other mental health professions further supports the notion that limited research exists regarding training in suicide screening, assessment, and intervention at the graduate level; thus, more attention is needed in these areas.
Suicide Training in Graduate Programs
Graduates of other counseling programs have indicated that there were limitations in the suicide prevention training that they received (Wakai et al., 2020). In a national sample of American School Counselor Association members, Becnel et al. (2021) found that 38% of school counselors (N = 226) did not receive suicide prevention training during their graduate programs and 37% received no training in crisis intervention. Similar results were found in a study of 193 professional counselors; over a third reported no classroom training in crisis preparation, and 30% reported no or minimal preparation in suicide assessment (Wachter Morris & Barrio Minton, 2012).
Schmidt (2016) evaluated the confidence and preparedness of 339 mental health practitioners (i.e., professional counselors, school counselors, social workers, psychologists). Results indicated that 52% of participants had graduate course work in suicide intervention and assessment, but 19% reported feeling not very confident in working with clients who had suicidal ideations. Conversely, Binkley and Leibert (2015) found that students who received training before their practicum working with clients who experience suicidal thoughts had lower anxiety and a greater level of confidence in addressing those issues compared to those who did not receive training.
The results of these studies look at counselor training and confidence or preparedness, to support the need for additional training in this area and research on best practices in preparing CITs to work with clients who present with suicidal ideation. Studies report training levels associated with practice outcomes (e.g., confidence), but there is a lack of literature explaining how suicide assessment and intervention training occurs in counselor education programs. Although there is literature that demonstrates that self-efficacy directly influences a counselor’s development (Barbee et al., 2003; Barnes, 2004; Kozina et al., 2010; Lent et al., 2003; Pechek, 2018; Vincenzes et al., 2023), literature that specifically addresses self-efficacy as it relates to working with a client who experiences suicidal ideation is sparse. However, the literature supports that additional training is needed on this topic and that self-efficacy is an important concept to consider when developing training protocols for CITs.
Self-Efficacy
Self-efficacy is dynamic and plays a significant role in counselor training and skill development. Bandura (1986) first introduced self-efficacy as an individual’s judgment on their capabilities to execute an action to achieve a certain performance or goal. Later the term was linked to behavioral motivation in the academic setting and was defined as a student’s belief in their ability to accomplish and succeed on an academic-related task (Bandura, 1989). Bandura (1997) also found that self-efficacy beliefs can be altered through four primary sources: (a) personal performance accomplishments, (b) vicarious learning, (c) social persuasion, and (d) physiological and affective states. While self-efficacy is dynamic (Lent, 2020) and can be impacted by personal interpretation of these primary sources (Lent & Brown, 2006), research has found that self-efficacy is an important factor in counselor competency (Barbee et al., 2003; Barnes, 2004; Kozina et al., 2010; Pechek, 2018; Vincenzes et al., 2023). More specifically, Lent et al. (2003) found that CITs’ initial clinical work and experience with more difficult skills (e.g., managing a session, handling the role of the counselor) increased counselor self-efficacy (Kozina et al., 2010).
Self-Efficacy in Suicide Training
Counselors who lack self-efficacy in their ability to work with a client who is experiencing suicidal thoughts may conduct suicide screening, assessments, and interventions ineffectively (Douglas & Wachter Morris, 2015; Jahn et al., 2016). In addition, counselors with low self-efficacy are more likely to subconsciously choose not to see suicide warning signs (Douglas & Wachter Morris, 2015) or avoid the topic of suicide altogether (Jahn et al., 2016). It is important that CITs are exposed to the topic of suicide and that they gain more counseling experience involving this issue during their training so that they will feel more confident working with a client experiencing suicidal thoughts. More exposure to this topic leaves CITs feeling better equipped to address suicide in sessions and is also likely to increase their self-efficacy (Elliott & Henninger, 2020; Pechek, 2018; Sawyer et al., 2013; Shea & Barney, 2015).
Clear evidence of the positive effects of including training on suicide within counselor education programs has been documented, demonstrating a reduction of fear and more success in helping clients manage suicide-related issues (Jahn et al., 2016). CITs who had prior training in suicide experienced lower levels of anxiety and higher levels of confidence in working with a client with suicidal thoughts (Binkley & Leibert, 2015). Similarly, professional counselors who expressed confidence in their academic training on suicide experienced lower levels of fear related to negative client outcomes and had higher levels of confidence in their skills and abilities (Jahn et al., 2016).
Self-Efficacy in Suicide Training for Online Learning. Although the topic of self-efficacy in counselor education has been studied (Barbee et al., 2003; Barnes, 2004; Conteh et al., 2018; Fakhro et al., 2023; Kozina et al., 2010; Pechek, 2018; Suh et al., 2018; Vincenzes et al., 2023), the literature does not focus on how best to teach for improved self-efficacy related to suicide assessment and intervention in the online setting. Specifically, it is not clear how counselor educators can best teach suicide screening, assessment, or intervention skills online. Two recent studies in counselor education programs have tried to better explain self-efficacy in suicide training during online learning (Elliott & Henninger, 2020; Gallo et al., 2019).
Elliott and Henninger (2020) showed that different online teaching strategies (e.g., a combination of a written module, role-plays/observations, and a facilitated discussion) in an online counselor education program showed no between-group differences, while all teaching strategies showed significant improvements in self-efficacy of CITs. Another study found that a 15-hour youth suicide prevention course that included didactic and experiential activities in a master’s counseling program increased participants’ knowledge and perceived ability to help clients who experienced suicidal ideations, as well as increased their self-efficacy in screening, assessment, and intervention (Gallo et al., 2019).
Purpose of the Study
With the influx of online counselor education programs, it is essential to determine how to improve suicide training and intervention skills (Allen & Seaman, 2014) so that CITs are better prepared to address the topic of suicide. The current quantitative study examined the influence of an online counseling practice model on CITs’ self-efficacy when it came to the utilization of suicide assessment and intervention with clients. The research question was: Do CITs’ perceived levels of self-efficacy in suicide assessment and intervention change because of practicing these skills through role-plays in an online counseling course? By better understanding these findings, implications can be made for how counselor educators can teach suicide screening, assessment, and intervention skills online.
Method
Procedures
Prior to beginning this study, our research team received full approval from the IRB. Participants were then recruited from an online clinical mental health counseling program. Only students enrolled in the online basic counseling skills course were recruited to ensure that all participants were at the same place in the program regarding knowledge and skills learned. An electronic announcement was posted in the 10 online basic skill course shells. The announcement included a hyperlink directing participants to an informed consent document, which detailed their requirements and rights and allowed them to indicate their consent to participate. Before completing any survey questions, the participants created a username for data comparison in the pre- and posttests, which was also an avenue for dropping participants if they requested to leave the study. After providing their username, participants completed a brief demographic questionnaire and the Counselor Suicide Assessment Efficacy Survey (CSAES; Douglas & Wachter Morris, 2015). To protect participant anonymity, no additional identifying information was collected.
Structure of the Basic Skills Class
Once students completed the pretest consent form, demographic questionnaire, and assessment, the counselor educators (i.e., faculty) started the class by providing participants with a variety of technology-assisted counseling experiences and activities (e.g., role-play demonstrations, best practices in telemental health counseling, lecture videos on specific counseling skills, guidelines for a preferred topic for the role-plays). To ensure consistency of content across courses, the faculty made sure to include the same teaching resources in each section of the class and continuously consulted each other to make sure that the classes were taught as similarly as possible. In addition, they decided that all students should receive the same training and teaching activities, ensuring that they were equally prepared to address the topic of suicide during their clinical courses and after graduation.
The topic of self-care was addressed with participants, as this was the first opportunity students had to practice counseling skills within the program. This focus on self-care was an important step toward decreasing the potential of significant deep-rooted issues surfacing without sufficient time or training to properly address them. Students would learn about a new basic counseling skill each week and were instructed to incorporate that skill into the week’s role-play. In addition to reading about the skill in the course textbook, students were required to view weekly lecture videos and role-plays that specifically explained and demonstrated the skill that the students would be practicing that week during their role-play. For role-plays, participants were randomly paired with other participants within the same basic counseling skills course to practice basic foundational counseling skills. Each pair of students participated in five weekly role-plays as both the counselor and the client. Two of these role-plays occurred during class and three occurred outside of class. Each role-play occurred via Zoom and lasted approximately 10–15 minutes during class or 30 minutes when completed outside of class. For in-class role-plays, participants utilized breakout rooms in Zoom. Faculty provided each participant in the counselor role with feedback at the end of each role-play. Role-plays outside of the class required participants to send their partner a Zoom link and password. The role-plays were recorded in Zoom. Participants identified one role-play to submit to the instructor for formal assessment of their basic counseling skills and to provide formative feedback to each participant when acting in the counselor role.
Preparation for Suicidal Ideation Role-Plays
After the initial five role-plays were completed, participants prepared for role-plays that focused on crisis counseling. They read a chapter from their textbook on crisis counseling and various supplemental articles on working with a client with suicidal ideations. In addition, they viewed pre-recorded role-plays on suicide assessment created by faculty in the program. Participants remained in the same randomly assigned pairs from earlier in the semester and then completed an additional five role-plays (one weekly), which allowed for them to gain experience working with a client with suicidal ideations.
Suicidal Ideation Role-Plays
Prior to beginning the role-plays, participants were provided with a brief synopsis for the topic of suicide and were also given the instructor’s phone number in case they needed immediate support or guidance. Like the previous role-plays, each of these lasted approximately 10–15 minutes during online classes or 30 minutes outside of class. Again, role-plays completed outside of class were recorded so that faculty could provide detailed feedback to students. The first in-class role-play was completed in a fishbowl format, allowing students in the class to observe. Instead of utilizing multiple breakout rooms, students remained in one room and observed one role-play at a time. This allowed students to learn vicariously from one another and to observe the ways that suicide screening, assessment, and intervention skills were demonstrated. The initial role-play also served as a way for participants in the counselor role to gain experience completing a suicide assessment while practicing other basic counseling skills. Four additional role-plays occurred and offered an opportunity for participants to continually reassess the risk of suicide of their partners, develop a safety plan, establish treatment goals, and practice other basic counseling skills. During the last role-play, participants in the counselor role conducted a termination session in which the counselor reviewed the client’s safety and treatment plans. Additionally, they reviewed the client’s goals and objectives and provided time for the client to reflect on the counseling experience.
Faculty Supervision and Learning Activities
During the semester, faculty supervision was an essential component of the process. If additional support or guidance was needed for participants, faculty were available via phone between 8 am–8 pm, Monday through Friday. Faculty were available to all role-play participants regardless of their role (i.e., counselor, client, or observer). While supervision can look different for each instructor, the counselor educators in this study regularly consulted with one another to ensure that they were conveying the same expectations to the students enrolled in the courses. This extended to making sure they discussed similar topics at the same time during the course; included the same teaching activities, readings, and assignments; and consulted with one another when a concern arose that may have changed course plans.
In addition to completing the virtual role-plays during the semester, participants completed a variety of activities and assignments that were intended to prepare them for realistic experiences needed upon graduation. For example, participants completed components of a treatment plan after each counseling session which were submitted to the instructor immediately following the role-play. Additionally, they submitted video tapes of role-plays for faculty feedback. Finally, participants transcribed one 30-minute role-play. This assignment allowed them to identify and reflect on specific foundational skills that they used when working with a client reporting suicidal ideations. At the conclusion of the semester, participants were asked to complete the posttest using the same username they created at the beginning of the semester. The posttest included the same assessment as the pretest (CSAES).
Participants
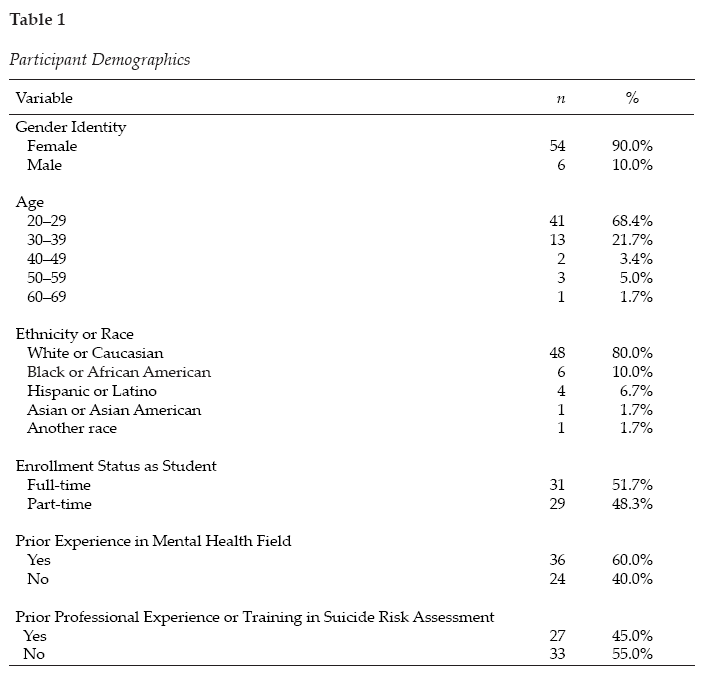
A convenience sample was used for this study. Master’s-level counseling students enrolled in the spring 2021 and spring 2022 counseling skills courses (10 sections total) in an online clinical mental health counseling graduate program were recruited via news announcements and emails to participate in this study. A total of 120 students were invited to participate in the study; however, only 60 were included because they completed both the pretest and posttest self-efficacy assessment. Included students’ ages ranged from 21–61 years old. The average age of participants was 29.03 (SD = 8.49). The sample consisted of the following racial identities: 80.0% White or Caucasian (n = 48), 10.0% Black or African American (n = 6), 6.7% Hispanic or Latino (n = 4), 1.7% Asian or Asian American (n = 1), and 1.7% did not indicate their racial identities (n = 1). Most participants identified as female (90%, n = 54) and were enrolled in the mental health counseling program full-time (51.7%, n = 31). When asked about prior experience in the mental health field, 60% (n = 36) had this experience; however, only 45% (n = 27) had prior professional experience or training in suicide risk assessment. Table 1 contains all participant demographics.
Measure
The study participants completed the CSAES (Douglas & Wachter Morris, 2015). The CSAES measures self-efficacy in suicide assessment and intervention. According to the developers (Douglas & Wachter Morris, 2015), the CSAES is comprised of 25 items that may make suicide assessment or intervention difficult for a counselor. These items are rated on a confidence scale that ranges from 1 (not confident) to 5 (highly confident). The confidence items are organized into four subscales:
- General Suicide Assessment, which has seven items and a maximum score of 35
- Assessment of Personal Characteristics, which has 10 items and a maximum score of 50
- Assessment of Suicide History, which has three items and a maximum score of 15
- Suicide Intervention, which has five items and a maximum score of 25
Sample items include the following: Q1 “I can effectively inquire if a student has had thoughts of killing oneself” (General Suicide Assessment); Q11 “I can effectively ask a student about his or her history of mental illness” (Assessment of Personal Characteristics); Q18 “I can effectively ask a student about his or her previous suicide attempts” (Assessment of Suicide History); and Q25 “I can appropriately intervene if a student is at imminent risk for suicide” (Suicide Intervention).
Table 1
Participant Demographics
The total score for the scale is 125, with higher scores representing higher levels of self-efficacy associated with suicide assessment and intervention (Douglas & Wachter Morris, 2015). The CSAES can be scored two ways. First, the assessment can be scored individually for a more detailed understanding of what differences, if any, in self-efficacy exist between differing aspects of suicide assessment. The second way is to calculate the total sum of the assessment-related subscales and the intervention subscale. In doing so, each subscale would have a mean for the individual scale (Douglas & Wachter Morris, 2015).
The assessment developers have reported internal reliability for the CSAES as a calculation for each of the four subscales and the second-order factor of Suicide Assessment using Cronbach’s α: General Suicide Assessment α = .882, Assessment of Personal Characteristics α = .88, Assessment of Suicide History α = .81, Suicide Intervention α = .83, and Suicide Assessment α = .93 (Douglas & Wachter Morris, 2015).
The CSAES was noted for showing “structural aspects of validity and sensitivity to detect differing levels of self-efficacy” (Douglas & Wachter Morris, 2015) based on the utilization of a four-factor model that was cross-validated. The scale was validated with a total of 324 participants. Of the participants, 258 (79.63%) were female. Unfortunately, a limitation of the instrument is that the diversity of participants was unknown due to ethnicity inadvertently being left off the demographic questionnaire while it was being developed (Douglas & Wachter Morris, 2015).
The current study assessed the internal reliability of the CSAES using Cronbach’s α and omega (ω) using test-retest reliability because the measure of consistency was between two measurements of the same construct to the same group at two different times. The overall CSAES has strong reliability (α = .978; ω = .978), and each subscale had the following reliability scores: General Suicide Assessment (α = .943; ω = .946); Assessment of Personal Characteristics (α = .947; ω = .947); Assessment of Suicide History (α = .896; ω = .890); and Suicide Intervention (α = .920; ω = .915). All subscale reliability coefficients were high when looking at both α and ω, meaning that good internal consistency was found among items of the scale (Green & Salkind, 2014).
Data Analysis
Before running any analyses, we screened the data using SPSS version 26.0.0.1 software to check for (a) missing data, (b) average expected scores per the outcome variables, (c) standard deviations within range, and (d) normality of data (Green & Salkind, 2014). The initial sample included 108 surveys; however, only 60 of these could be paired with posttest data, using the username data point. Therefore, individuals with their missing pair were deleted along with any others that included missing data (i.e., listwise deletion). The final sample included 60 respondents. A power analysis using a statistical power analysis program (G*Power 3.1) for paired t-test showed an N of 54 was needed for 95% power with an alpha level of .05 and a moderate effect size of .5. Next, scales were computed, and univariate testing occurred. Data met all assumptions for conducting a paired t-test (i.e., dependent variable was continuous, normally distributed, and without outliers and the observations were independent of one another). The paired t-test was used to test the effectiveness of training for suicide assessment and intervention in a basic skills class using a single-group (pretest/posttest) design, including demographics and the CSAES. To ensure that all students received the same teaching activities and assignments, we decided not to utilize a control group. We wanted to ensure that all students were equally prepared and trained to address the topic of suicide upon entering their clinical courses and upon graduation.
Results
The purpose of the study was to compare counseling students’ pretest and posttest self-efficacy assessments when taking a basic skills course that highly emphasized skills related to suicide training and assessment. The results of a paired-samples t-test on the General Suicide Assessment subscale indicate that on average, students scored significantly higher (Mpost = 28.57, SD = 4.80) after taking the basic skills class (Mpre = 21.20, SD = 7.80), t(59) = −9.15, p < .001. A large effect was found (d = 1.182, 95% CI [−1.51, −.85]). The results of a paired-samples t-test on the Assessment of Personal Characteristics subscale indicate that on average, students scored significantly higher (Mpost = 41.17, SD = 6.59) after taking the basic skills class (Mpre = 33.80, SD = 8.75), t(59) = −8.77, p < .001. A large effect was found (d = 1.133, 95% CI [−1.46, −.81]). The results of a paired-samples t-test on the Suicide History Assessment subscale indicate that on average, students scored significantly higher (Mpost = 13.07, SD = 2.22) after taking the basic skills class (Mpre = 9.95, SD = 3.33), t(59) = −8.38, p < .001. A large effect was found (d = 1.081, 95% CI [−1.40, −.76]). The results of a paired-samples t-test on the Suicide Intervention subscale indicate that on average, students scored significantly higher (Mpost = 19.00, SD = 4.32) after taking the basic skills class (Mpre = 14.63, SD = 5.46), t(59) = −7.21, p < .001. A large effect was found (d = .931, 95% CI [−1.23, −.63]). In summary, students’ level of self-efficacy related to suicide assessment and intervention increased in all areas as a result of taking the basic counseling skills class.
Because this study had a small sample size, the risk increases that at least one test is statistically significant just by chance. Therefore, a Bonferroni correction was applied to adjust the significance levels: Bonferroni correction = .05/4 = .0125 (.05 = acceptable significance level; 4 = number of subscales of CSAES). Therefore, the familywise error value is .0125. Because the above results are looking at significance at the p <.001 value, all results remain significant.
Discussion
The initial research question was: Do CITs’ perceived levels of self-efficacy in suicide assessment and intervention change because of practicing these skills through role-plays in an online counseling course? According to the results of the current study, on average, students felt significantly more prepared and confident in their ability to counsel someone experiencing suicidal ideations after practicing the skills in their basic counseling skills online course. Prior research indicated that many students were either not taught these skills (Becnel et al., 2021) or did not feel prepared to address these issues in counseling (Schmidt, 2016). The current study points to the vitality of both teaching students about suicide screening and assessment, as well as providing them with a safe space to practice the skills. By offering students opportunities to practice suicide screening, assessment, and intervention skills, instructors could help reduce their students’ anxiety in addressing the topic during their clinical courses, which Binkley and Leibert (2015) found to be a significant student concern.
Furthermore, it is important for counselor educators to observe and provide students with feedback regarding these essential skills. Past research points to the concern that students are not adequately conducting suicide screening, assessments, and interventions (Jahn et al., 2016); therefore, it would behoove counselor educators to infuse various opportunities throughout the curriculum to strengthen these skills. In turn, feedback and practice opportunities combined may help to enhance students’ levels of self-efficacy (Elliott & Henninger, 2020; Gallo et al., 2019), thus helping them to address the issues with clients in a timely and direct manner.
Implications for Training
While CACREP (2023) requires counselor educators to prepare students to work with clients who present with suicidal ideations, there is no clear criteria as to the best way of preparing students to work with these clients. Research on the topic is limited; however, the results of this study can provide a framework for helping to inform key training areas in counselor education and future research.
As counselor educators continue to expand on the didactic knowledge of suicide screening, assessment, and intervention, more intentional efforts need to be embedded throughout the curriculum to continuously expose students to experiential opportunities for practicing these skills. This idea coincides with the recommendation from the American Association of Suicidology that proposes suicide knowledge and assessment be at the forefront of graduate program curricula (Schmitz et al., 2012). First, in foundational courses, students could become more comfortable with the topic of suicide. These courses could help break down barriers and possibly calm nerves that tend to surround the topic of suicide. In assessment courses, students could role-play giving a partner various suicide screenings and assessments and gain experience interpreting the results. These role-plays could occur during class or be recorded for faculty feedback. In skills courses, students could practice suicide intervention by broaching the topic with their classmate-clients to help them feel more comfortable with directly asking clients if they are experiencing suicidal ideations. In addition, it may be helpful if a trauma and crisis counseling course was required within the core curriculum. This course could have content devoted to suicide screening, assessment, and intervention, including both didactic and experiential opportunities. By offering these opportunities throughout the curriculum, similar to ethical and cultural considerations, students may feel more comfortable and confident as they enter their clinicals (Binkley & Leibert, 2015; Guillot Miller et al., 2013). This intentional, consistent exposure to practicing these skills could help more students gain foundational knowledge and experience with this topic. In turn, as their self-efficacy and comfort levels increase, they may be more confident addressing this topic with clients. Ultimately, this may increase client welfare by ensuring effective assessment and treatment of client needs.
Implications for Counselor Education Training Research
The topic of suicide screening, assessment, and intervention in counselor education and supervision could benefit significantly from continued outcome-based research. For example, longitudinal studies could track students’ perceived levels of self-efficacy on suicide screening, assessment, and intervention as they go through a counseling program. This may help educators become more intentional about when and how the topic is infused within the curriculum. In addition, research could compare different types of teaching methods (e.g., role-play versus lecture) that expose students to the topic and assess which methods are more influential in building students’ skills and self-efficacy. Finally, researchers could interview current mental health therapists to identify knowledge and skill gaps to help educators teach students about crisis counseling more intentionally.
Limitations
There are a few limitations to the current study that are important to discuss. First is the variability in teaching and supervision styles across different instructors, which may impact the students’ overall feelings of self-efficacy. Although the same procedures were followed, educators inevitably have different styles of giving feedback. How the feedback is perceived by the student may impact their confidence in using the acquired skills.
Another limitation involves the notion of social desirability bias. The participants in the current study were students in the program; therefore, they may have felt pressured to identify increases in their self-efficacy around suicide assessment and intervention. This pressure may have been experienced because some of their current professors also served as researchers in the study and the students may have wanted to gain favor with them.
With regard to external validity, there are a few limitations. First, our research team did not account for prior experience in suicide screening, assessment, or intervention; thus, the results could have been impacted by external experiences versus the sole experience of the course activities. Additionally, there was a large portion of the data that could not be used because the pre- and post- surveys could not be aligned. Although the current study had 60 viable pre- and post- surveys, the data could have been more reliable and generalizable with a larger dataset. Furthermore, there was a lack of diversity in the research sample. Because the participants were primarily White females, the results may be limited in its generalizability to other cultures and genders.
Future studies should attempt to better isolate these variables (i.e., teaching styles, feedback, participant recruitment, prior experience in suicide training, cultural background) and find ways to improve response rates. In addition, it would be beneficial to have a comparison course or data from other counseling programs’ basic skills classes to further determine if this practice-based model was effective. Results could be linked to more general self-efficacy increases because of growing more comfortable with learning and using interviewing skills (Holladay & Quiñones, 2003).
One final limitation worth noting is the effect size estimates of the pre- and posttest scores. All effect sizes are large. Some reasons why the effect sizes may be large in the paired-samples t-tests include: (a) large differences between paired observations (the mean scores between the pre- and posttest scores were extremely different), and (b) small within-group variability (if the within-group variability is small, then even small differences between the paired observations could result in a large effect size).
Conclusion
As counselor educators prepare students for the profession, intentional inclusion of suicide screening, assessment, and intervention skills is vital to increasing students’ confidence and preparation to address this topic with their future clients. But it is not enough for students to learn about screening, assessment, and interventions; they need experiential opportunities to practice and develop these skills. In turn, feedback and practice will increase their comfort levels to directly and adequately support their clients’ needs.
Conflict of Interest and Funding Disclosure
The authors reported no conflict of interest
or funding contributions for the development
of this manuscript.
References
Allen, I. E., & Seaman, J. (2014). Grade change: Tracking online education in the United States. The Sloan Consortium. Sloan-C. http://www.onlinelearningsurvey.com/reports/gradechange.pdf
American Foundation for Suicide Prevention. (2023). Suicide statistics. https://afsp.org/suicide-statistics
Bandura, A. (1986). Social foundations of thought and action: A social cognitive theory. Prentice-Hall.
Bandura, A. (1989). Human agency in social cognitive theory. American Psychologist, 44(9), 1175–1184. https://doi.org/10.1037/0003-066X.44.9.1175
Bandura, A. (1997). Self-efficacy: The exercise of control. W. H. Freeman.
Barbee, P. W., Scherer, D., & Combs, D. C. (2003). Prepracticum service-learning: Examining the relationship with counselor self-efficacy and anxiety. Counselor Education and Supervision, 43(2), 108–119. https://doi.org/10.1002/j.1556-6978.2003.tb01835.x
Barnes, K. L. (2004). Applying self-efficacy theory to counselor training and supervision: A comparison of two approaches. Counselor Education and Supervision, 44(1), 56–69. https://doi.org/10.1002/j.1556-6978.2004.tb01860.x
Becnel, A. T., Range, L., & Remley, T. P., Jr. (2021). School counselors’ exposure to student suicide, suicide assessment self-efficacy, and workplace anxiety: Implications for training, practice, and research. The Professional Counselor, 11(3), 327–339. https://doi.org/10.15241/atb.11.3.327
Binkley, E. E., & Leibert, T. W. (2015). Prepracticum counseling students’ perceived preparedness for suicide response. Counselor Education and Supervision, 54(2), 98–108. https://doi.org/10.1002/ceas.12007
Centers for Disease Control and Prevention. (2021, February 20). Web-based injury statistics query and reporting system (WISQARS) fatal injury reports. https://wisqars.cdc.gov/fatal-leading
Conteh, J. A., Mariska, M. A., & Huber, M. J. (2018). An examination and validation of personal counseling and its impact on self-efficacy for counselors-in-training. Journal of Counselor Practice, 9(2), 109–138.
https://www.journalofcounselorpractice.com/uploads/6/8/9/4/68949193/jac902111_jcp_vol_9_issue_2.pdf
Council for the Accreditation of Counseling and Related Educational Programs. (2023). 2024 CACREP standards. https://www.cacrep.org/wp-content/uploads/2023/06/2024-Standards-Combined-Version-6.27.23.pdf
Cramer, R. J., Bryson, C. N., Eichorst, M. K., Keyes, L. N., & Ridge, B. E. (2017). Conceptualization and pilot testing of a core competency-based training workshop in suicide risk assessment and management: Notes from the field. Journal of Clinical Psychology, 73(3), 233–238. https://doi.org/10.1002/jclp.22329
Douglas, K. A., & Wachter Morris, C. A. (2015). Assessing counselors’ self-efficacy in suicide assessment and intervention. Counseling Outcome Research and Evaluation, 6(1), 58–69.
https://doi.org/10.1177/2150137814567471
Elliott, G. M., & Henninger, J. (2020). Online teaching and self-efficacy to work with suicidal clients. Counselor Education and Supervision, 59(4), 283–296. https://doi.org/10.1002/ceas.12189
Fakhro, D., Rujimora, J., Zeligman, M., & Mendoza, S. (2023). Counselor self-efficacy, multicultural competency, and perceived wellness among counselors in training during COVID-19: A pre- and peri-analysis. Journal of Counselor Leadership and Advocacy, 10(2), 99–111. https://doi.org/10.1080/2326716X.2023.2229323
Gallo, L. L., Doumas, D. M., Moro, R., Midgett, A., & Porchia, S. (2019). Evaluation of a youth suicide prevention course: Increasing counseling students’ knowledge, skills, and self-efficacy. Journal of Counselor Preparation and Supervision, 12(3), 1–23. https://digitalcommons.sacredheart.edu/jcps/vol12/iss3/9
Granello, D. H. (2010). The process of suicide risk assessment: Twelve core principles. Journal of Counseling & Development, 88(3), 363–370. https://doi.org/10.1002/j.1556-6678.2010.tb00034.x
Green, S. B., & Salkind, N. J. (2014). Using SPSS for Windows and Macintosh: Analyzing and understanding data (7th ed.). Pearson.
Guillot Miller, L., McGlothlin, J. M., & West, J. D. (2013). Taking the fear out of suicide assessment and intervention: A pedagogical and humanistic practice. The Journal of Humanistic Counseling, 52(1), 106–121. https://doi.org/10.1002/j.2161-1939.2013.00036.x
Holladay, C. L., & Quiñones, M. A. (2003). Practice variability and transfer of training: The role of self-efficacy generality. Journal of Applied Psychology, 88(6), 1094–1103. https://doi.org/10.1037/0021-9010.88.6.1094
Jahn, D. R., Quinnett, P., & Ries, R. (2016). The influence of training and experience on mental health practitioners’ comfort working with suicidal individuals. Professional Psychology: Research and Practice, 47(2), 130–138. https://doi.org/10.1037/pro0000070
Kozina, K., Grabovari, N., De Stefano, J., & Drapeau, M. (2010). Measuring changes in counselor self-efficacy: Further validation and implications for training and supervision. The Clinical Supervisor, 29(2), 117–127. https://doi.org/10.1080/07325223.2010.517483
LeCloux, M. (2021). Efficient, yet effective: Improvements in suicide-related knowledge, confidence, and preparedness after the deployment of a brief online module on suicide in a required MSW course. Journal of Teaching in Social Work, 41(4), 389–407. https://doi.org/10.1080/08841233.2021.1954577
Lent, R. W. (2020). Career development and counseling: A social cognitive framework. In S. D. Brown & R. W. Lent (Eds.), Career development and counseling: Putting theory and research to work (3rd ed., pp. 129–164). Wiley.
Lent, R. W., & Brown, S. D. (2006). Integrating person and situation perspectives on work satisfaction: A social-cognitive view. Journal of Vocational Behavior, 69(2), 236–247. https://doi.org/10.1016/j.jvb.2006.02.006
Lent, R. W., Hill, C. E., & Hoffman, M. A. (2003). Development and validation of the Counselor Activity Self-Efficacy Scales. Journal of Counseling Psychology, 50(1), 97–108. https://doi.org/10.1037/0022-0167.50.1.97
Liebling-Boccio, D. E., & Jennings, H. R. (2013). The current status of graduate training in suicide risk assessment. Psychology in the Schools, 50(1), 72–86. https://doi.org/10.1002/pits.21661
Pechek, A. A. (2018). Counselor education learning modalities: Do they predict counseling self-efficacy in students? (Publication No. 10785997) [Doctoral dissertation, Adams State University]. ProQuest Dissertations Publishing.
Sawyer, C., Peters, M. L., & Willis, J. (2013). Self-efficacy of beginning counselors to counsel clients in crisis. Journal of Counselor Preparation and Supervision, 5(2), 30–43. https://digitalcommons.sacredheart.edu/jcps/vol5/iss2/3/
Schmidt, R. C. (2016). Mental health practitioners’ perceived levels of preparedness, levels of confidence and methods used in the assessment of youth suicide risk. The Professional Counselor, 6(1), 76–88.
https://doi.org/10.15241/rs.6.1.76
Schmitz, W. M., Jr., Allen, M. H., Feldman, B. N., Gutin, N. J., Jahn, D. R., Kleespies, P. M., Quinnett, P., & Simpson, S. (2012). Preventing suicide through improved training in suicide risk assessment and care: An American Association of Suicidology Task Force report addressing serious gaps in U.S. mental health training. Suicide and Life-Threatening Behavior, 42(3), 292–304. https://doi.org/10.1111/j.1943-278X.2012.00090.x
Shea, S. C., & Barney, C. (2015). Teaching clinical interviewing skills using role-playing: Conveying empathy to performing a suicide assessment: A primer for individual role-playing and scripted group role-playing. Psychiatric Clinics of North America, 38(1), 147–183. https://doi.org/10.1016/j.psc.2014.10.001
Suicide Prevention Resource Center. (2006). Core competencies in the assessment and management of suicide risk.
Suh, S., Crawford, C. V., Hansing, K. K., Fox, S., Cho, M., Chang, E., Lee, S., & Lee, S. M. (2018). A cross-cultural study of the self-confidence of counselors-in-training. International Journal for the Advancement of Counselling, 40(3), 255–266. https://doi.org/10.1007/s10447-018-9324-4
Vincenzes, K., Pechek, A., & Sprong, M. (2023). Counselor trainees’ development of self-efficacy in an online skills course. Journal of Counselor Preparation and Supervision, 17(1). https://digitalcommons.sacredheart.edu/jcps/vol17/iss1/1
Wachter Morris, C. A., & Barrio Minton, C. A. (2012). Crisis in the curriculum? New counselors’ crisis preparation, experiences, and self-efficacy. Counselor Education and Supervision, 51(4), 256–269.
https://doi.org/10.1002/j.1556-6978.2012.00019.x
Wakai, S., Schilling, E. A., Aseltine, R. H., Blair, E. W., Bourbeau, J., Duarte, A., Durst, L. S., Graham, P., Hubbard, N., Hughey, K., Weidner, D., & Welsh, A. (2020). Suicide prevention skills, confidence, and training: Results from the Zero Suicide Workforce Survey of behavioral health care professionals. SAGE Open Medicine, 8, 1–12. https://doi.org/10.1177/2050312120933152
Wasylko, Y., & Stickley, T. (2007). Promoting emotional development through using drama in mental health education. In T. Stickley & T. Basset (Eds.), Teaching mental health (pp. 297–309). Wiley.
https://doi.org/10.1002/97804470713617.ch25
World Health Organization. (2014). Preventing suicide: A global imperative. https://www.who.int/publications/i/item/9789241564779
Ashley Ascherl Pechek, PhD, NCC, ACS, LPC, is an associate professor at Commonwealth University of Pennsylvania. Kristin A. Vincenzes, PhD, NCC, ACS, BC-TMH, LPC, is a professor at Commonwealth University of Pennsylvania. Kellie Forziat-Pytel, PhD, NCC, ACS, LPC, is an assistant professor at Commonwealth University of Pennsylvania. Stephen Nowakowski is a graduate student at Commonwealth University of Pennsylvania. Leandrea Romero-Lucero, PhD, ACS, LPCC, CSOTS, is an associate professor and Clinical Mental Health Counseling Program Director at Commonwealth University of Pennsylvania. Correspondence may be addressed to Ashley Ascherl Pechek, 401 N. Fairview Street, Lock Haven, PA 17745, aap402@commonwealthu.edu.
Aug 20, 2021 | Volume 11 - Issue 3
Alexander T. Becnel, Lillian Range, Theodore P. Remley, Jr.
In a national sample of current school counselors with membership in the American School Counselor Association (N = 226), we examined the prevalence of suicide training among school counselors as well as differences in suicide assessment self-efficacy and workplace anxiety between school counselors who were exposed to student suicide and those who were not. The results indicate that 38% of school counselors were not prepared for suicide prevention during graduate training. Although school counselors’ exposure to suicide was not related to their workplace anxiety, those who were exposed to a student suicide attempt had higher suicide assessment self-efficacy scores than those who were not. This study demonstrates the impact of suicide exposure on school counselors and the need for additional suicide assessment training.
Keywords: school counselors, suicide, suicide assessment, self-efficacy, workplace anxiety
Suicide continues to be a growing concern for young people in the United States. Suicide is the second leading cause of death among children between the ages of 11 and 18, claiming the lives of 2,127 middle school– and high school–aged children in 2019 alone (Centers for Disease Control and Prevention [CDC], 2021). In 2019, a nationwide survey found that 18.8% of high school students reported seriously considering attempting suicide, 15.7% reported making a plan to attempt suicide, and 8.9% reported attempting suicide (Ivey-Stephenson et al., 2019). As youth suicide rates continue to rise (National Institute of Mental Health [NIMH], 2019), it is becoming increasingly important to understand how school counselors are prepared to work with suicidal youth, as well as the impact of suicidality on them.
Children and adolescents spend significant amounts of time at school, making school counselors the primary suicide and risk assessors for this population (American School Counselor Association [ASCA], 2020b). School counselors are more likely to assess youth for suicide risk than any other mental health professional (Schmidt, 2016). In 2002, a national study of ASCA members found that 30% of professional school counselors experienced a suicide-related crisis event while they were graduate student interns (Allen et al., 2002). In a more recent study, about two thirds of school counselors reported that they were conducting multiple suicide assessments each month (Gallo, 2018). Stickl Haugen et al. (2021) found that 79.8% of school counselors worked with a student who had previously attempted suicide and 36.7% experienced a student’s death by suicide. As school counselors become more frequently exposed to student suicide, it is important to understand their preparation for this role and the impact of these events on the school counselors themselves.
School Counselor Suicide and Crisis Training
Although school counselors are often exposed to student suicide, many school counselors lack appropriate crisis intervention and suicide assessment training (Allen et al., 2002; Springer et al., 2020; Wachter Morris & Barrio Minton, 2012) and lack confidence in their ability to assess students for suicide risk (Gallo, 2018; Schmidt, 2016). About 20 years ago, one third of school counselors entered the field without any formal crisis intervention coursework and nearly 60% did not feel adequately prepared to handle a school crisis event (Allen et al., 2002). Ten years later, school counselors did not fare any better, with less than a quarter of school counselors reporting that they completed a course in crisis intervention and nearly two thirds reporting that a crisis intervention course was not even offered during their master’s program (Wachter Morris & Barrio Minton, 2012). Not surprisingly, therefore, school counselors feel unprepared. In a national survey, 44% of school counselors reported being unprepared for a student suicide attempt, and 57% reported being unprepared for a student’s death by suicide (Solomonson & Killam, 2013). In another national survey, Gallo (2018) found that only 50% of school counselors thought that their training adequately prepared them to assess suicidal students, and only 59% felt prepared to recognize a student who was at risk. These results are especially troubling considering that the Council for Accreditation of Counseling and Related Educational Programs (CACREP) requires school counselor education programs to provide both suicide prevention and suicide assessment training (CACREP, 2015).
Exposure to Suicide and Self-Efficacy
Mental health professionals often question their professional judgment following an exposure to suicide (Sherba et al., 2019; Thomyangkoon & Leenars, 2008). Consequently, it is imperative to explore school counselor self-efficacy in the aftermath of a student suicide. Self-efficacy is the degree to which individuals believe that that they can achieve self-determined goals, and individuals are more likely to be successful in achieving those goals simply by belief in their success (Bandura, 1986). Counselor self-efficacy is defined as counselors’ judgment of their ability to provide counseling to their clients (Larson et al., 1992). As counselors spend more years in practice, their self-efficacy increases (Goreczny et al., 2015; Kozina et al., 2010; Lent et al., 2003). Further, counselor education faculty have significantly higher levels of suicide assessment self-efficacy than their students (Douglas & Wachter Morris, 2015). The relationship between counselor self-efficacy and work experience is well documented, so it is imperative to control for years of counseling experience as a potential covariate when studying other factors that can affect counselor self-efficacy.
Although the literature regarding school counselors’ exposure to suicide is sparse, more studies have focused on the experiences of related professions, such as clinical counselors, social workers, psychiatrists, and psychologists. In a national survey, 23% of clinical counselors experienced a client’s death by suicide at some point in their career (McAdams & Foster, 2002). In the aftermath of their clients’ deaths by suicide, those counselors reported a loss of self-esteem and an increase of intrusive thoughts. They increased referrals for hospitalization for clients at risk, gave increased attention to signs for suicide, and increased their awareness of legal liabilities in their practices. In a study of community-based mental health professionals who experienced a client death by suicide, one third considered changing careers and about 15% considered early retirement in the aftermath of the suicide (Sherba et al., 2019). Psychologists who felt responsible for the death were more likely to experience a sense of professional incompetence (Finlayson & Graetz Simmonds, 2018). Among psychiatrists, those who experienced a patient’s suicidal death were more likely in the future to suggest hospitalization for patients who showed risk signs for suicide (Greenberg & Shefler, 2014). Additionally, 20% of the psychiatrists in Thomyangkoon and Leenars’s (2008) study considered changing professions after experiencing a patient death by suicide. Given the similarities in these professions, it is reasonable to suggest that school counselors may feel more anxious about their jobs following a suicide exposure.
To date, there are only three published studies that explore suicide exposures among school counselors (Christianson & Everall, 2008; Gallo et al., 2021; Stickl Haugen et al., 2021). In a qualitative study, high school counselors felt a lack of personal support from their fellow staff members and noted the importance of self-care in the aftermath of a student death by suicide. Additionally, those who lost students to suicide thought that a lack of practice standards made it difficult to navigate these difficult situations (Christianson & Everall, 2008). In another qualitative study, elementary school counselors who worked with suicidal students recognized their important work in preventing suicide but also reported a lack of suicide prevention training opportunities tailored toward working with young children (Gallo et al., 2021). In a quantitative study, most school counselors thought that a student’s death by suicide left both personal and professional impacts on their lives. These school counselors most often reported low mood, a sense of guilt or responsibility, and preoccupation with the incident as personal impacts. They also identified heightened awareness of suicide risk, more professional caution around suicide, and seeking additional training as professional impacts. The researchers suggested that future studies should determine if the number of student deaths by suicide influences the impact of the suicide exposure (Stickl Haugen et al., 2021). However, this study did not examine anxiety, an important personal impact, nor did it examine self-efficacy in dealing with suicide attempts, a more likely occurrence than suicide deaths.
Research Questions
The following research questions guided this study:
- What is the prevalence of graduate and postgraduate training in suicide prevention, crisis intervention, and suicide postvention among current school counselors?
- Are there differences in suicide assessment self-efficacy between school counselors exposed and not exposed to student deaths by suicide and suicide attempts, controlling for years of school counseling experience as a covariate?
- Does the number of suicide exposures relate to school counselors’ level of suicide assessment self-efficacy when controlling for years of school counseling experience as a covariate?
- Are there differences in workplace anxiety between school counselors exposed and not exposed to student deaths by suicide and suicide attempts, controlling for years of school counseling experience as a covariate?
Method
Procedure
We obtained approval from our university’s Human Subjects Protection Review Committee prior to conducting this study. Using a random number generator, we randomly selected 5,000 members from the ASCA member directory to receive a link to the survey. When potential participants clicked the link, they viewed and agreed to an informed consent statement before they were permitted to view the survey. This statement also informed participants that they could stop participation or withdraw their participation at any time. Upon agreement to the informed consent statement, participants were directed to the survey. This online survey was administered via Qualtrics, which allowed them to respond anonymously.
Participants
From the 5,000 potential participants, 422 began the survey. From these participants, 101 opened the survey and did not answer any questions, 5 did not agree to the informed consent statement, 29 reported that they were not current school counselors, and 60 did not complete the survey. Thus, 226 of the 5,000 ASCA members completed the survey (4.52%). An a priori power analysis (Cohen, 1992) with a power of .8, a medium effect size, and α = .05 determined that the required sample size for our most robust test was 175.
Participants were 226 current school counselors (201 women, 88.9%; 25 men, 11.1%). The racial categories included 192 White (85%), nine Black or African American (4%), eight “other” races (3.5%), six Asian (2.7%), five biracial or multiracial (2.2%), three American Indian or Alaska Native (1.3%), and three not reporting race (1.3%). The ethnicity categories included 210 participants (92.9%) who were not of Hispanic or Latino or Spanish origin and 16 (7.1%) who were of Hispanic or Latino or Spanish origin. The mean age was 39 years (SD = 10.68), and the mean years of experience working as a school counselor was 7 (SD = 6.98). With regard to school setting, 52 school counselors worked in an elementary or primary school (23%), 58 worked in a middle or junior high school (25.7%), 81 worked in a high school (35.8%), 19 worked in a K–12 school (8.4%), and 16 worked in another type of school not listed (7.1%). Although ASCA does not provide demographic information about their members, this sample is similar in its demographic makeup to the sample in Gilbride et al.’s (2016) study, which sought to describe the demographic identity of ASCA’s membership.
Instrumentation
The survey packet consisted of three instruments: the demographic questionnaire, the Counselor Suicide Assessment Efficacy Survey (CSAES; Douglas & Wachter Morris, 2015), and the Workplace Anxiety Scale (WAS; McCarthy et al., 2016).
Demographic Questionnaire
Using a demographic questionnaire, we asked participants to identify the following information: sex, race, ethnicity, age, years of school counseling experience, and school type (e.g., high school, middle school). Additionally, we asked participants to identify the types of suicide exposures that they have encountered in their school counseling careers. If they reported exposure to either deaths by suicide or suicide attempts, the survey followed up with additional questions about the number of exposures, the amount of time since the first suicide exposure, and the amount of time since the most recent suicide exposure. We asked participants if their schools had crisis plans or crisis teams. We also asked participants if they had training in suicide prevention, crisis intervention, and suicide postvention during graduate school and the number of postgraduate training hours in each of these areas.
CSAES
The CSAES evaluates counselors’ confidence in their ability to assess clients for suicide risk and intervene with a client at risk of suicide. It includes 25 items in four subscales: General Suicide Assessment, Assessment of Personal Characteristics, Assessment of Suicide History, and Suicide Intervention. Each item is rated on a 5-point Likert scale from 1 (not confident) to 5 (highly confident). High scores indicate high self-efficacy. Among school counselors in the original study, each subscale had good internal consistency (α = .88–.81) and acceptable goodness of fit. As suggested by Douglas and Wachter Morris (2015), we scored each subscale separately and averaged each score. This process created four comparable subscale scores.
WAS
The WAS measures participants’ job-related anxiety. This scale asks participants to rate eight items such as “I worry that my work performance will be lower than that of others at work” on a 5-point scale from 1 (strongly disagree) to 5 (strongly agree). High scores on the WAS indicate higher levels of job-related anxiety. The WAS demonstrated good internal consistency (α = .94) and acceptable goodness of fit (McCarthy et al., 2016).
Data Analysis
To address our first research question, we used descriptive statistics to examine the prevalence of training among the participants. We used analysis of covariance (ANCOVA) to detect differences in both suicide assessment self-efficacy (CSAES scores) and workplace anxiety (WAS scores) while controlling for years of school counseling experience between school counselors who were exposed to student suicide and those who were not. We considered exposure to deaths by suicide and exposure to suicide attempts as different types of exposure. Therefore, we performed a total of four ANCOVAs: (a) differences in CSAES scores between school counselors exposed to deaths by suicide and those not exposed, (b) differences in CSAES scores between school counselors exposed to suicide attempts and those not exposed, (c) differences in WAS scores between school counselors exposed to deaths by suicide and those not exposed, and (d) differences in WAS scores between school counselors exposed to suicide attempts and those not exposed. We also used analysis of variance (ANOVA) to determine the difference in years of school counseling experience between those exposed to suicide and those not exposed. To determine the relationship between the number of suicide exposures and counselor suicide assessment self-efficacy, we also completed two partial correlations between the number of exposures to student death by suicide and CSAES scores, and the number of exposures to student suicide attempts and CSAES scores.
Results
A total of 64 school counselors reported that they experienced a student death by suicide during their school counseling experience (28.3%), with a mean of 2.11 deaths (SD = 2.21). On average, their first suicide death was 6.72 years ago (SD = 5.87), and the most recent suicide death was 3.84 years ago (SD = 3.88). A total of 124 participants experienced a student suicide attempt during their school counseling experience (54.9%), with a mean of 5.36 attempts (SD = 10.54). On average, the first suicide attempt was 5.91 years ago (SD = 6.07), and the most recent attempt was 1.82 years ago (SD = 2.10). Of all 226 school counselors, 195 worked in schools that have crisis plans (86.3%), and 170 worked in schools that have crisis teams (75.2%).
Suicide Training
Regarding suicide prevention training during their graduate program, 140 (62%) received some training, but 86 (38%) received no training. Regarding crisis intervention training during their graduate program, 142 (63%) received some, but 84 (37%) received none. Regarding suicide postvention, only 87 (38.5%) received some, but 139 (61.5%) received none. The number of postgraduate training hours varied widely for each preparation type. For suicide prevention, training hours averaged 12.20 (SD = 28.61); for crisis intervention, training hours averaged 9.04 (SD = 15.51); and for suicide postvention, training hours averaged 6.45 (SD = 18.14). We removed one participant’s postgraduate training data that was more than 3 standard deviations higher than the mean. In order to better illustrate the distribution of postgraduate training hours, we grouped the number of training hours into four categories: 0 hours, 1–10 hours, 11–50 hours, and more than 50 hours of postgraduate training. Nearly a quarter of the participants (24.3%) received no postgraduate training in suicide prevention, about a third of the participants (30.5%) received no postgraduate training in crisis intervention, and half (50.4%) received no postgraduate training in suicide postvention.
To further demonstrate the disparity of suicide training, cross-tabulation was performed between graduate training and the number of postgraduate training hours. We reported this data in Table 1. Most surprisingly, 25 school counselors (11.1%) received no graduate training in suicide prevention, nor any postgraduate hours of training in suicide prevention; another 45 (19.9%) received no graduate training and only 10 or fewer hours of postgraduate training in suicide prevention, making nearly 1 in 3 school counselors unprepared to provide suicide prevention services. Crisis intervention fared similarly with 26 school counselors (11.5%) reporting no graduate training and no postgraduate training hours and 41 school counselors (18.1%) reporting no graduate training and 10 or fewer postgraduate training hours. Again, nearly 1 in 3 school counselors were not adequately prepared to provide this important service. Crisis postvention fared the worst, with 80 school counselors (35.4%) reporting that they received no graduate training and no postgraduate training hours, and 46 school counselors (20.4%) reporting no graduate training and fewer than 10 hours of postgraduate training. More than half of the school counselors surveyed are unprepared to face the aftermath of a suicide.
Table 1
Graduate Training and Postgraduate Training Hours
| Number of postgraduate training hours |
Received graduate training |
Did not receive graduate training |
|
Frequency |
Percentage |
Frequency |
Percentage |
| Suicide Prevention |
|
|
|
|
| 0 hours |
30 |
13.3 |
25 |
11.1 |
| 1–10 hours |
73 |
32.3 |
45 |
19.9 |
| 11–50 hours |
29 |
12.8 |
15 |
6.6 |
| 50 or more hours |
8 |
3.6 |
1 |
0.4 |
| Total |
140 |
62.0 |
86 |
38.0 |
|
|
|
|
|
| Crisis Intervention |
|
|
|
|
| 0 hours |
43 |
19.0 |
26 |
11.5 |
| 1–10 hours |
69 |
30.5 |
41 |
18.1 |
| 11–50 hours |
26 |
11.5 |
16 |
7.0 |
| 50 or more hours |
4 |
1.8 |
1 |
0.4 |
| Total |
142 |
63.0 |
84 |
37.0 |
|
|
|
|
|
| Suicide Postvention |
|
|
|
|
| 0 hours |
34 |
15.0 |
80 |
35.4 |
| 1–10 hours |
37 |
16.4 |
46 |
20.4 |
| 11–50 hours |
12 |
5.3 |
11 |
4.8 |
| 50 or more hours |
4 |
1.8 |
2 |
0.9 |
| Total |
87 |
38.5 |
139 |
61.5 |
Suicide Exposure and Suicide Assessment Self-Efficacy
An ANOVA indicated that school counselors exposed to a student death by suicide had significantly more years of school counseling experience (M = 11.9, SD = 7.87) than school counselors not exposed to a student death by suicide (M = 5.1, SD = 5.56): F(1, 224) = 21.512, p < .001. Controlling for years of school counseling experience as a covariate, an ANCOVA indicated that there was no significant difference between these two groups in General Suicide Assessment, F(1, 223) = .316, p = .574; Assessment of Personal Characteristics, F(1, 223) = .156, p = .694; Suicide Intervention, F(1, 223) = .028, p = .867; or Assessment of Suicide History, F(1, 223) = 1.095, p = .133.
Similarly, results of an ANOVA indicated that school counselors exposed to student suicide attempts had significantly more years of school counseling experience (M = 8.8, SD = 7.31) than counselors not exposed (M = 4.9, SD = 5.94): F(1, 224) = 8.055, p = .005. Controlling for years of school counseling experience, an ANCOVA indicated significant differences between the two groups in General Suicide Assessment, F(1, 223) = 6.014, p = .015; Assessment of Personal Characteristics, F(1, 223) = 7.140, p = .008; and Suicide Intervention, F(1, 223) = 6.671, p = .010; but not Assessment of Suicide History, F(1, 223) = .763, p = .383. Overall, effect sizes were small.
Number of Exposures and Self-Efficacy
A partial correlation between the number of suicide exposures and CSAES scores while controlling for years of school counseling experience was not statistically significant. There was no significant relationship between the number of death by suicide exposures and General Suicide Assessment, r(61) = .137, p = .285; Assessment of Suicide History, r(61) = .207, p = .104; Assessment of Personal Characteristics, r(61) = .170, p = .184; or Suicide Intervention, r(61) = .077, p = .551. Likewise, there was also no significant relationships between the number of suicide attempt exposures and General Suicide Assessment, r(121) = −.028, p = .762; Assessment of Suicide History, r(121) = .087, p = .336; Assessment of Personal Characteristics, r(121) = .131, p = .150; or Suicide Intervention, r(121) = .076, p = .401. We reported data regarding the frequency of suicide exposure in Table 2.
Suicide Exposure and Workplace Anxiety
In WAS scores, an ANCOVA revealed that there were no significant differences between school counselors exposed and not exposed to a student death by suicide when controlling for years of school counseling experience: F(1, 223) = .412, p = .522. Likewise, an ANCOVA revealed that there was no significant difference in WAS scores between school counselors exposed and not exposed to student suicide attempts when controlling for years of school counseling experience: F(1, 223) = .238, p = .626. To further illustrate the relationship between years of school counseling experience and workplace anxiety, a correlation coefficient indicated that these measures were significantly related, r(224) = −.260, p < .001.
Discussion
Among these school counselors, more than a quarter experienced a student’s death by suicide and over half experienced a student’s suicide attempt. These results are consistent with previous studies indicating that many school counselors will eventually be exposed to a student suicide during their careers (Allen et al., 2002; Gallo, 2018; Schmidt, 2016; Stickl Haugen et al., 2021). Given how common suicide experiences are, school counselors need to be trained to manage suicide-related crises.
Training
A surprising result in our study was the overall lack of suicide and crisis training reported. As seen in Table 1, nearly 2 in 5 school counselors (38%) reported that they received no suicide prevention training during their graduate education. Additionally, a quarter of the school counselors in this study reported that they received no postgraduate training in suicide prevention, and half reported between 1 and 10 hours. Thus, a sizeable portion of these school counselors were not adequately trained to incorporate suicide prevention programs into their school counseling practice. This finding echoes Gallo (2018), who reported that only 60% of school counselors felt prepared to identify students at risk for suicide. These rates are poor considering that CACREP requires suicide assessment and suicide prevention training as a standard of all counselor education programs (CACREP, 2015). Further, ASCA states that school counselors are responsible for identifying students at risk for suicide and ensuring that suicide prevention programs are in place in schools (ASCA, 2020a). The lack of training reported in this study is particularly troubling given that all of the participants in this study were members of ASCA.
Table 2
Frequency of Student Suicide Exposure
| Variable |
Frequency |
Percentage |
| Number of student deaths by suicide (n = 64) |
|
|
| 1 |
37 |
57.8 |
| 2 |
15 |
23.4 |
| 3–5 |
8 |
12.5 |
| > 5 |
4 |
6.3 |
| Years since first death by suicide (n = 64) |
|
|
| Within 1 year |
12 |
18.8 |
| 1 and 5 years |
25 |
39.0 |
| 6 and 10 years |
12 |
18.8 |
| More than 10 years |
15 |
23.4 |
| Years since most recent death by suicide (n = 64) |
|
|
| Within 1 year |
23 |
35.9 |
| Between 1 and 5 years |
26 |
40.6 |
| Between 6 and 10 years |
11 |
17.2 |
| More than 10 years |
4 |
6.3 |
| Number of student suicide attempts (n = 124) |
|
|
| 1 |
29 |
23.4 |
| 2 |
29 |
23.4 |
| 3–5 |
44 |
35.5 |
| > 5 |
22 |
17.7 |
| Years since first student attempt (n = 124) |
|
|
| Within 1 year |
30 |
24.2 |
| Between 1 and 5 years |
51 |
41.1 |
| Between 6 and 10 years |
21 |
17.0 |
| More than 10 years |
22 |
17.7 |
| Years since most recent attempt (n = 124) |
|
|
| Within 1 year |
84 |
67.7 |
| Between 1 and 5 years |
33 |
26.6 |
| Between 6 and 10 years |
6 |
4.8 |
| More than 10 years |
1 |
0.8 |
Crisis intervention training among school counselors also was poor. Comparable to the finding on suicide prevention training, a third of these school counselors reported no graduate training in crisis intervention. Further, more than a third reported that they did not receive postgraduate training hours in crisis intervention, and nearly half received between 1 and 10 hours of postgraduate training. A significant portion of these school counselors were not adequately prepared to respond to crises in their schools. These findings are slightly worse than the findings from 20 years ago when one third of a sample of school counselors reported that they entered the field with no formal crisis intervention coursework (Allen et al., 2002). However, these findings are much better than Wachter Morris and Barrio Minton’s (2012) study in which only 20% of school counselors completed a course in crisis intervention during their master’s degree program. Although preparation has increased, crisis preparation for school counseling students must continue to improve given that school counselors regularly experience crises (Wachter, 2006) and school counseling students often experience crises while still in graduate school completing their practicum or internship (Wachter Morris & Barrio Minton, 2012). The number of school counselors who experienced a student suicide event in the current study also supports the notion that school counselors regularly experience crises.
Most of these school counselors (61.5%) were not trained in their graduate programs for suicide postvention. Half of the surveyed school counselors reported that they received no postgraduate training hours in suicide postvention, with an additional 38% reported having received between 1 and 10 hours of postgraduate training. These results demonstrate that the vast majority of school counselors are not prepared to respond to a student’s suicidal death. This finding is distressing because school counselors play a vital role in the aftermath of a student suicide (Maples et al., 2005; Substance Abuse and Mental Health Services Administration [SAMHSA], 2016).
Suicide Assessment Self-Efficacy
Among these counselors, exposure to suicide alone did not make a difference with their suicide assessment self-efficacy or workplace anxiety. Years of school counseling experience appears to have a much more important role in suicide assessment self-efficacy and reduced anxiety than experiencing a student’s death by suicide. This result supports previous studies that found that years of experience has a positive relationship with self-efficacy (Douglas & Wachter Morris, 2015; Kozina et al., 2010; Lent et al., 2003). It also parallels the previous finding that the impact of a client’s suicidal death on a mental health practitioner decreases as the practitioner gains years of experience (McAdams & Foster, 2002). This result is different from Stickl Haugen et al.’s (2021) finding that school counselors who were exposed to a student death had higher levels of suicide assessment self-efficacy than those not exposed. However, Stickl Haugen et al. did not control for years of school counseling experience.
In contrast, exposure to suicide attempts did make a difference in suicide assessment self-efficacy. Even after controlling for years of experience, counselors with suicide attempt experience reported more efficacy in three of four subscales: General Suicide Assessment, Assessment of Personal Characteristics, and Suicide Intervention. One explanation for this outcome is that a student suicide attempt experience might motivate school counselors to learn about suicide and the risk factors associated. This explanation echoes Wagner et al.’s (2020) finding that counselors found additional training in the aftermath of a suicide very helpful. Many of the school counselors in the current study received no formal training, so it is possible that these experiences helped them fill in knowledge gaps, which in turn increased their self-efficacy. Training increases self-efficacy (Al-Darmaki, 2004; Mirick et al., 2016; Wachter Morris & Barrio Minton, 2012), so it is also possible that this experience worked as an in vivo training for these school counselors, increasing their self-efficacy.
Workplace Anxiety
Although mental health clinicians often experience symptoms of anxiety in the wake of a student suicide (McAdams & Foster, 2002; Sherba et al., 2019), present results suggest that a student’s death or suicide attempt does not have an impact on school counselors’ workplace anxiety. One explanation for this finding is the relationship between self-efficacy and anxiety. Overall, these school counselors had high self-efficacy scores in each of the four subscales. Previous research indicated that as self-efficacy increases, anxiety decreases (Bodenhorn & Skaggs, 2005; Gorecnzy et al., 2015; Larson et al., 1992). The death by suicide experience might not have impacted the counselors’ anxiety in this study because of their overall high self-efficacy. Another explanation is that the school counselors in this study had on average several years of experience (M = 7.05). Workplace anxiety levels decrease as school counselors spend more time on the job.
Implications
These results have several implications for school counselors and school counselor educators. First, school counselor educators and school counseling graduate programs should be aware of both the overall disparity of graduate-level suicide and crisis training as well as the benefits that training can provide to future school counselors. Regarding suicide prevention, crisis intervention, and suicide postvention, there are far too many untrained school counselors among the current body of school counselors. School counseling students are a vulnerable group when it comes to suicide assessment self-efficacy (Douglas & Wachter Morris, 2015), so it is imperative to support their professional development. School counseling graduate programs must increase their efforts to adequately train and prepare school counselors for suicide prevention, assessment, and intervention.
Second, school counselors should prepare to face the probability of having to deal with student suicide attempts and student deaths by suicide. If school counselors do not receive this training during their graduate programs, then they must seek continuing education opportunities that address suicide prevention, crisis intervention, and suicide postvention. Suicide and crisis training increases counselor self-efficacy (Mirick et al., 2016; Wachter Morris & Barrio Minton, 2012), making appropriate preparation vital. Additionally, school counselors could consider clinical supervision as a supplemental layer of support. School counselors receive supervision at much lower rates than their clinical counterparts (Perera-Diltz & Mason, 2012) even though many school counselors desire more supervision (Cook et al., 2012). Given that school counseling–focused supervision can increase self-efficacy (Tang, 2019) and school counselors feel a lack of personal support in the aftermath of a suicide (Christianson & Everall, 2008), school counselors must seek clinical supervision.
Finally, school counselor educators should consider training efforts that focus specifically on student suicide attempts. In the current study, school counselors exposed to a suicide attempt were more efficacious than school counselors not exposed to a student suicide attempt. Modeling these experiences through the use of specific role plays could help school counseling students feel more confident about their suicide assessment capabilities. Although CACREP does not require counselor education programs to provide suicide postvention training (CACREP, 2015), perhaps standards should adapt to include this important training area. Regardless, programs should also emphasize this training to best prepare school counselors.
Limitations and Suggestions for Future Research
Some factors limited this study. Although we had a national sample, we surveyed only current members of ASCA. It is possible that school counselors who are not members of ASCA might have responded differently. The study also had a low response rate (4.64%). Those school counselors who responded may be uniquely interested in this area, so the results may not reflect all school counselors. This study also did not limit the types of school counselors who could participate. It is possible that school counselors who work with younger children, such as elementary and primary school counselors, have less familiarity with suicide assessment and intervention than those school counselors who work with older children. The inclusion of these counselors could have affected the results of this study. Finally, this study did not ask participants if they graduated from a CACREP-accredited program. Because suicide prevention and assessment training are required components of CACREP-accredited programs, it is possible that school counselors who graduated from these programs may have different levels of training and self-efficacy than those trained in unaccredited programs.
For future studies, researchers should consider limiting their samples to specific levels of schooling such as elementary, middle, or high school. This change would help illustrate the nuanced differences among school counselors in different academic environments as well as increase focus on the school counselors who most often work with suicidal students. Future studies should also consider surveying a sample that includes all school counselors, not just ASCA members. Researchers should also differentiate between school counselors who graduated from CACREP-accredited programs and those who did not. Collecting this data would allow researchers to detect if there are any differences in suicide assessment training and self-efficacy between these two groups. Finally, future researchers should consider designing a study that seeks to identify the factors that most impact suicide assessment self-efficacy. Although this study showed that a suicide attempt experience could impact suicide assessment self-efficacy, other factors, such as self-confidence, could have a larger influence.
Suicide continues to be understudied in school counseling. Even though this study demonstrates the high likelihood that a school counselor will experience a student suicide, school counselors continue to report a lack of preparation in suicide prevention, crisis intervention, and suicide postvention. Although school counselors who experienced a student suicide attempt appeared to gain self-efficacy from their experiences, additional training in counseling suicidal students might help school counselors feel prepared before they face such serious situations. If additional training can help school counselors save students from suicide, then efforts must be made to adequately prepare them.
Conflict of Interest and Funding Disclosure
The authors reported no conflict of interest
or funding contributions for the development
of this manuscript.
References
Al-Darmaki, F. R. (2004). Counselor training, anxiety, and counseling self-efficacy: Implications for training psychology students from the United Arab Emirates University. Social Behavior and Personality: An International Journal, 32(5), 429–439. https://doi.org/10.2224/sbp.2004.32.5.429
Allen, M., Burt, K., Bryan, E., Carter, D., Orsi, R., & Durkan, L. (2002). School counselors’ preparation for and participation in crisis intervention. Professional School Counseling, 6(2), 96–102.
American School Counselor Association. (2020a). The school counselor and suicide risk assessment. https://schoolcounselor.org/Standards-Positions/Position-Statements/ASCA-Position-Statements/The-School-Counselor-and-Suicide-Risk-Assessment
American School Counselor Association. (2020b). The school counselor and student mental health. https://schoolcounselor.org/Standards-Positions/Position-Statements/ASCA-Position-Statements/The-School-Counselor-and-Student-Mental-Health
Bandura, A. (Ed.). (1986). Social foundations of thought and action: A social cognitive theory. Prentice Hall.
Bodenhorn, N., & Skaggs, G. (2005). Development of the School Counselor Self-Efficacy Scale. Measurement and Evaluation in Counseling and Development, 38(1), 14–28. https://doi.org/10.1080/07481756.2005.11909766
Centers for Disease Control and Prevention. (2021). Injury center: Violence prevention: Suicide prevention. https://webappa.cdc.gov/sasweb/ncipc/leadcause.html
Christianson, C. L., & Everall, R. D. (2008). Constructing bridges of support: School counsellors’ experiences of student suicide. Canadian Journal of Counselling, 42(3), 209–221.
Cohen, J. (1992). A power primer. Psychological Bulletin, 112(1), 155–159. https://doi.org/10.1037//0033-2909.112.1.155
Cook, K., Trepal, H., & Somody, C. (2012). Supervision of school counselors: The SAAFT model. Journal of School Counseling, 10(21). https://files.eric.ed.gov/fulltext/EJ981202.pdf
Council for Accreditation of Counseling and Related Educational Programs. (2015). 2016 CACREP standards. http://www.cacrep.org/wp-content/uploads/2017/08/2016-Standards-with-citations.pdf
Douglas, K. A., & Wachter Morris, C. A. (2015). Assessing counselors’ self-efficacy in suicide assessment and intervention. Counseling Outcome Research and Evaluation, 6(1), 58–69. https://doi.org/10.1177/2150137814567471
Finlayson, M., & Graetz Simmonds, J. (2018). Impact of client suicide on psychologists in Australia. Australian Psychologist, 53(1), 23–32. https://doi.org/10.1111/ap.12240
Gallo, L. L. (2018). The relationship between high school counselors’ self-efficacy and conducting suicide risk assessments. Journal of Child and Adolescent Counseling, 4(3), 209–225. https://doi.org/10.1080/23727810.2017.1422646
Gallo, L. L., Rausch, M. A., Beck, M. J., & Porchia, S. (2021). Elementary school counselors’ experiences with suicidal students, Journal of Child and Adolescent Counseling, 7(1), 26–41. https://doi.org/10.1080/23727810.2020.1835419
Gilbride, D. D., Goodrich, K. M., & Luke, M. (2016). The professional peer membership of school counselors and the resources used within their decision-making. The Journal of Counselor Preparation and Supervision, 8(2). https://repository.wcsu.edu/jcps/vol8/iss2/4
Goreczny, A. J., Hamilton, D., Lubinski, L., & Pasquinelli, M. (2015). Exploration of counselor self-efficacy across academic training. The Clinical Supervisor, 34(1), 78–97. https://doi.org/10.1080/07325223.2015.1012916
Greenberg, D., & Shefler, G. (2014). Patient suicide. Israel Journal of Psychiatry & Related Sciences, 51(3), 193–198.
Ivey-Stephenson, A. Z., Demissie, Z., Crosby, A. E., Stone, D. M., Gaylor, E., Wilkins, N., Lowry, R., & Brown, M. (2019). Suicidal ideation and behaviors among high school students — Youth Risk Behavior Survey, United States, 2019. Morbidity and Mortality Weekly Report, Supplement 69(1), 47–55. https://doi.org/10.15585/mmwr.su6901a6
Kozina, K., Grabovari, N., De Stefano, J., & Drapeau, M. (2010). Measuring changes in counselor self-efficacy: Further validation and implications for training and supervision. The Clinical Supervisor, 29(2), 117–127. https://doi.org/10.1080/07325223.2010.517483
Larson, L. M., Suzuki, L. A., Gillespie, K. N., Potenza, M. T., Bechtel, M. A., & Toulouse, A. L. (1992). Development and validation of the Counseling Self-Estimate Inventory. Journal of Counseling Psychology, 39(1), 105–120. https://doi.org/10.1037/0022-0167.39.1.105
Lent, R. W., Hill, C. E., & Hoffman, M. A. (2003). Development and validation of the Counselor Activity Self-Efficacy Scales. Journal of Counseling Psychology, 50(1), 97–108. https://doi.org/10.1037/0022-0167.50.1.97
Maples, M. F., Packman, J., Abney, P., Daugherty, R. F., Casey, J. A., & Pirtle, L. (2005). Suicide by teenagers in middle school: A postvention team approach. Journal of Counseling & Development, 83(4), 397–405. https://doi.org/10.1002/j.1556-6678.2005.tb00361.x
McAdams, C. R., III., & Foster, V. A. (2002). An assessment of resources for counselor coping and recovery in the aftermath of client suicide. Journal of Humanistic Counseling, Education and Development, 41(2), 232–242.
McCarthy, J. M., Trougakos, J. P., & Cheng, B. H. (2016). Are anxious workers less productive workers? It depends on the quality of social exchange. Journal of Applied Psychology, 101(2), 279–291. https://doi.org/10.1037/apl0000044
Mirick, R. G., Bridger, J., McCauley, J., & Berkowitz, L. (2016). Continuing education on suicide assessment and crisis intervention for social workers and other mental health professionals: A follow-up study. Journal of Teaching in Social Work, 36(4), 363–379. https://doi.org/10.1080/08841233.2016.1200171
National Institute of Mental Health. (2019). Mental health information: Statistics: Suicide. https://www.nimh.nih.gov/health/statistics/suicide.shtml
Perera-Diltz, D. M., & Mason, K. L. (2012). A national survey of school counselor supervision practices: Administrative, clinical, peer, and technology mediated supervision. Journal of School Counseling, 10, 1–34. https://files.eric.ed.gov/fulltext/EJ978860.pdf
Substance Abuse and Mental Health Services Administration. (2016). Preventing suicide: A toolkit for high school. Center for Mental Health Services, Substance Abuse and Mental Health Services Administration. https://store.samhsa.gov/product/Preventing-Suicide-A-Toolkit-for-High-Schools/SMA12-4669
Schmidt, R. C. (2016). Mental health practitioners’ perceived levels of preparedness, levels of confidence and methods used in the assessment of youth suicide risk. The Professional Counselor, 6(1), 76–88. https://doi.org/10.15241/rs.6.1.76
Sherba, R. T., Linley, J. V., Coxe, K. A., & Gersper, B. E. (2019). Impact of client suicide on social workers and counselors. Social Work in Mental Health, 17(3), 279–301. https://doi.org/10.1080/15332985.2018.1550028
Solomonson, L. L., & Killam, W. (2013). A national study on crisis intervention: Are school counselors prepared to respond? Ideas and Research You Can Use: VISTAS 2013. https://www.counseling.org/docs/default-source/vistas/a-national-study-on-crisis-intervention.pdf?sfvrsn=b3b9af05_11
Springer, S., Paone, C. H., Colucci, J., & Moss, L. J. (2020). Addressing suicidality: Examining preservice school counselors’ perceptions of their training experiences. Journal of Child and Adolescent Counseling, 6(1), 18–36. https://doi.org/10.1080/23727810.2018.1556990
Stickl Haugen, J., Waalkes, P. L., & Lambie, G. W. (2021). A national survey of school counselors’ experiences with student death by suicide. Professional School Counseling, 25(1), 1–11. https://doi.org/10.1177/2156759X21993804
Tang, A. (2019). The impact of school counseling supervision on practicing school counselors’ self-efficacy in building a comprehensive school counseling program. Professional School Counseling, 23(1), 1–11. https://doi.org/10.1177/2156759X20947723
Thomyangkoon, P., & Leenars, A., (2008). Impact of death by suicide of patients on Thai psychiatrists. Suicide & Life-Threatening Behavior, 38(6), 728–740. https://doi.org/3994/10.1521/suli.2008.38.6.728
Wachter, C. A. (2006). Crisis in the schools: Crisis, crisis intervention training, and school counselor burnout (Publication No. 3221458). [Doctoral dissertation, University of North Carolina at Greensboro]. ProQuest Dissertations Publishing.
Wachter Morris, C. A., & Barrio Minton, C. A. (2012). Crisis in the curriculum? New counselors’ crisis preparation, experiences, and self-efficacy. Counselor Education and Supervision, 51(4), 256–269. https://doi.org/10.1002/j.1556-6978.2012.00019.x
Wagner, N. J., Grunhaus, C. M. L., & Tuazon, V. E. (2020). Agency responses to counselor survivors of client suicide. The Professional Counselor, 10(2), 251–265. https://doi.org/10.15241/njw.10.2.251
Alexander T. Becnel, PhD, NCC, LPC, is a doctoral candidate at the University of Holy Cross. Lillian Range, PhD, is a professor at the University of Holy Cross. Theodore P. Remley, Jr., JD, PhD, NCC, is a professor at the University of Holy Cross. Correspondence may be addressed to Alexander T. Becnel, 4123 Woodland Drive, New Orleans, LA 70131, abecnel2@uhcno.edu.
Apr 1, 2021 | Author Videos, Volume 11 - Issue 2
Rebekah F. Cole, Rebecca G. Cowan, Hayley Dunn, Taryn Lincoln
Newly released data from the U.S. Department of Defense shows military spouse suicide to be an imminent concern for the U.S. military. Currently, there is an absence of research in the counseling profession related to suicide prevention and intervention for this population. Therefore, this qualitative phenomenological study explored the perceptions of military spouses regarding suicide within their community. Ten military spouses were interviewed twice and were asked to provide written responses to follow-up questions. Six main themes emerged: (a) loss of control, (b) loss of identity, (c) fear of seeking mental health services, (d) difficulty accessing mental health services, (e) the military spouse community as a protective factor, and (f) desire for better communication about available mental health resources. Implications for practicing counselors and military leadership in helping to prevent military spouse suicide as well as recommendations for future research regarding ways to support military spouse mental health and prevent suicide in this community are included.
Keywords: military spouse, suicide, prevention, intervention, phenomenological
In 2018, there were 624,000 active-duty military spouses in the United States, 92% of whom were female (U.S. Department of Defense [DOD], 2018). Recent data also noted that the average age of a military spouse was 31.5 years and 88% of spouses had postsecondary education (U.S. Chamber of Commerce, 2017). Twenty-four percent of spouses were unemployed (DOD, 2018) and 35%–40% were underemployed (U.S. Chamber of Commerce, 2017). Further, 74% of military spouses had children under the age of 18 and often acted as single parents because of the responsibilities of the service member (Institute for Veterans and Military Families, 2016). And of particular note, the Substance Abuse and Mental Health Services Administration (SAMHSA; 2015) reported that 29.1% of military spouses have had a mental illness, with 11.8% having had at least one major depressive episode, and 6.5% having had a major depressive episode with severe impairment.
Military Lifestyle and Spousal Mental Health
Military spouses do not serve in combat as service members do, but they are subject to many stressors brought on by the military lifestyle that may affect their mental health (Cole, 2014). One of the primary stressors of the military lifestyle is frequent moving (Tong et al., 2018). Military families move every 2–3 years to a new location (Burke & Miller, 2016), which they may not have adequate time to prepare for, adding to the stress of the relocation process (Tong et al., 2018). Military spouses may feel isolated after moving, as 70% of military families live in civilian communities rather than in military housing (Blue Star Families, 2019). Although social support has been found to be key in ameliorating mental health issues in military spouses (Ross et al., 2020), this support is lost and must be rebuilt when the family moves to a new duty station.
Because of these frequent moves, military spouses are often unable to build consistent careers or finish their education (Institute for Veterans and Military Families, 2016). Relocating spouses may experience difficulty finding a new job or utilizing their professional license or certification in their new home state or country (DOD, 2020b). As a result of these lifestyle challenges, 24% of military spouses are unemployed (DOD, 2018) and 77% of employed spouses have been underemployed at least once (Blue Star Families, 2019). These employment challenges often result in anxiety and depression among military spouses (Linn et al., 1985). In addition, the inability to find work may result in financial stress for the family and often affects spousal mental and behavioral health (Blue Star Families, 2019; Center for the Study of Traumatic Stress, 2020).
In addition to stressful relocations and career disruption, spouses also face frequent deployments of their partners (Allen et al., 2011). These deployments result in increased depression and anxiety in spouses (Baer, 2019; Eaton et al., 2008; O’Keefe, 2016), with 92% of spouses reporting increased stress during a deployment, and 85% reporting that they feel anxious or depressed during a deployment (Romo, 2019). This deployment stress may be amplified when the spouse lives overseas and is away from their friends and family in an unfamiliar culture (McNulty, 2003). When their service member is deployed, military spouses have to take on new roles and responsibilities in the home, which may contribute to these high stress levels (Eaton et al., 2008). In addition, they may live in constant fear for their service member’s physical safety, as they are unable to contact their spouse regularly, or communication may be limited to social media with inherent limits to tone or context that prove to be anxiety-inducing (Allen et al., 2011; O’Keefe, 2016).
Military Spouses and Mental Health Treatment
Although military spouses are under constant stress in their everyday lives (Cole, 2012; Eaton et al., 2008; Mailey et al., 2018), they often resist seeking mental health treatment (Lewy et al., 2014). Past studies have revealed that spouses often do not seek therapy because they cannot locate a counselor they trust or who understands their culture, they are concerned that someone will find out they are seeking counseling, or they do not know where to find counseling services (Lewy et al., 2014). The stigma that military spouses fear regarding mental health treatment affecting their service member’s career progression mirrors that of the active-duty service member population (Britt et al., 2015). In addition, the pressure that spouses feel to take care of their families without their service member’s support and the sense that they must prioritize their families before themselves has led them to resist receiving mental health help for themselves (Mailey et al., 2018). When they do seek mental health services, spouses are likely to visit their primary care doctor at a military care facility; however, these facilities are not equipped to meet spouses’ mental health needs because of lack of personnel and resources for specialized mental health services (Eaton et al., 2008; Lewy et al., 2014).
Military Spouses and Suicide
Although many of these studies have focused on risk factors and barriers for military spouse mental health treatment, no research has focused on the consequences of these barriers, including suicide in this population. Although much focus has been placed on researching service member and veteran suicide (Blosnich et al., 2010), statistics regarding military spouse suicide were recently tracked for the first time and released to the public in September 2019 (DOD, 2019). In 2018, 128 military spouses died by suicide, with a suicide rate of 12.1 deaths per 100,000 individuals (DOD, 2020a). Of those who committed suicide, 57.8% were female and 85.1% were under the age of 40. Given the alarming numbers of spousal suicide outlined in the DOD report, it is essential that pioneering research be done to investigate suicidality in the military spouse population. This study, therefore, explored the perceptions of military spouses related to suicide in this population by interviewing military spouses themselves, who are the experts on the military spouse lifestyle and experience (Sargeant, 2012). The purpose of this study was not to focus on the experiences of spouses who have themselves attempted suicide, but rather how members of the military spouse population made meaning of suicide within their community. Thus, a qualitative phenomenological design was appropriate for exploring this meaning making (Christensen et al., 2017; Creswell & Poth, 2017). As experts on their own community and experiences, the participants provided perceptions that proved valuable in understanding the causes and risk factors associated with suicide in this population.
Purpose Statement and Research Questions
The purpose of this qualitative phenomenological study was to explore the perceptions of military spouses related to military spouse suicide and how these spouses made meaning of suicide within the military spouse community. Based on the perceptions and recommendations of the participants, this study makes suggestions to the civilian and military communities regarding best practices for preventing suicide in and providing mental health services for this population. This study was guided by the following research questions:
- What are the perceptions of military spouses of suicide in the military spouse community?
- What are the perceptions of military spouses regarding resources to prevent military spouse suicide?
Method
Our research team utilized the descriptive phenomenological tradition in qualitative inquiry, in which the researcher explores the participants’ meaning-making experience and how they translate this experience into their consciousness (Christensen et al., 2017; Creswell & Poth, 2017). In order to gather information and perspective regarding suicide within the military spouse community, Rebekah F. Cole, our team’s principal investigator, interviewed 10 spouses of active-duty service members, using a semi-structured interview, to explore their experiences in-depth and to understand how they make meaning of suicide within the military spouse community. A qualitative researcher does not aim to generalize but to draw out depth of insight from participants; hence, a small sample size was appropriate and justified with the aim of collecting a wealth of information from each participant (Creswell & Poth, 2017). Cole interviewed each spouse two times for approximately 30 minutes over the course of 4 weeks and then sent each participant an email with follow-up reflection questions (e.g., “What was it like for you to participate in this study?”) and demographic questions regarding the participants’ age group, gender, race/ethnicity, military branch, years as a spouse, and spouse’s rank.
Participants
We selected the participants based on their status as active-duty spouses as well as their willingness and availability to participate in two interviews and complete the follow-up questions. We identified and recruited participants via purposeful sampling following approval by the IRB at our university (Creswell & Poth, 2017). Cole made a posting on a military spouse Facebook page explaining the nature and purpose of the study and asking for volunteers who were married to an active-duty service member. We offered each participant a $250 Target gift card to participate in the study, given to them upon completion of the two interviews and return of the emailed follow-up questions. We selected the first 10 volunteers who responded to the Facebook post as the 10 participants in this study. Once they showed interest in participating in the study, Cole contacted each participant via email to explain the nature and goals of the study and provide the participants with the informed consent document to sign and return.
The participants in this study were all spouses of active-duty service members (see Appendix A for a demographic chart). Three of the participants were Army spouses, three were Air Force spouses, three were Navy spouses, and one was a Coast Guard spouse. Two of the spouses were in the 18–29 age range, five were in the 30–39 age range, and three were in the 40–49 age range. The time spent as a spouse ranged from 1–20 years with a mean of 9.5 years. Eight of the spouses identified as White or having a European heritage and two of the spouses identified as having Asian or Pacific Islander heritage. All of the spouses identified as female. The participants were assigned numbers (Participant 1, Participant 2, etc.) to protect their confidentiality throughout the study.
Research Team
The research team in this study consisted of Cole and two school counseling graduate students, Hayley Dunn and Taryn Lincoln. These students had been trained in research methodology and were familiar with the qualitative data analysis process. Lincoln is a 35-year-old White female whose husband is a retired service member. Dunn is a 33-year-old White female with no military connections. Cole worked closely with Dunn and Lincoln to review the transcriptions of the interviews, develop a comprehensive codebook, and discuss the themes and patterns that emerged from the data.
Data Collection
Cole conducted and recorded the interviews via phone. She transcribed the interviews using an automated transcription service and reviewed each transcription word-by-word to verify the accuracy and reliability of the transcription (Creswell & Creswell, 2018; Creswell & Poth, 2017). In each interview, Cole asked questions related to suicide in the spouse population (see Appendix B). She also utilized probing follow-up questions (e.g., “Can you tell me more about that?” or “Why do you think that is?”) to gather additional information throughout the interviews (Creswell & Creswell, 2018). Finally, Cole sent a follow-up email consisting of process questions related to the interview experience (see Appendix B) as well as demographic questions.
Data Analysis
We analyzed the data in a step-by-step process: 1) organizing the data, 2) looking over all of the data, 3) coding the data, 4) generating a description of themes, and 5) presenting the description of themes (Creswell & Creswell, 2018). Cole first organized the data, sorting each participant’s file and memoing ideas that began to emerge from the data (Creswell & Creswell, 2018; Creswell & Poth, 2017). We then each reviewed the transcripts and email responses in detail. After reviewing the data, we coded the interviews and follow-up questions. Cole compiled the codes that we generated into a codebook. We then identified and defined themes and patterns that emerged from the study. This collaboration continued until we decided that no additional themes and patterns were emerging from the data. Cole then sent the codebook, as well as the themes and patterns, to the external auditor of the study, Rebecca G. Cowan, who confirmed the findings of the research team. Cole then wrote a detailed narrative of the themes, which are presented in the Findings section of this article.
Strategies to Increase Trustworthiness
In order to increase trustworthiness of the study, Cole, the key data collector in this study, engaged in reflexivity and self-analysis throughout the study (Creswell & Creswell, 2018; Darawsheh, 2014; Meyer & Willis, 2019). As a military spouse and professional counselor, Cole inherently has her own thoughts and feelings related to spousal mental health. Thus, it was important to bracket these thoughts and feelings to prevent them from interfering with the data collection and analysis process. Cole used reflective journaling throughout the study to engage in self-reflection and to increase her self-awareness of her reactions to the participants’ perspectives (Malacrida, 2007; Meyer & Willis, 2019). She also discussed these thoughts and feelings with the research team to explore her position as the researcher in the context of this study (Barrett et al., 2020).
In addition to this reflexivity, Cole kept an audit trail throughout the study, which included the transcriptions of the interviews, the participants’ emailed responses, the codebook, reflexive journal entries, and the notes from the research team (Creswell & Creswell, 2018; Creswell & Poth, 2017). Cowan, an auditor with a PhD in counselor education who has been a counselor and counselor educator for the past 10 years, reviewed the study in full to verify the data collection and analysis process (Creswell & Creswell, 2018) as well as the rigor of the study (Patton, 2002).
To triangulate the study’s data and increase the validity of the study’s results, data were collected through two individual interviews as well as through an email questionnaire, both open-ended forms of data collection (Creswell & Creswell, 2018). Prolonged engagement assisted with the development of trust and rapport (Korstjens & Moser, 2018). Additionally, through the collection of both verbal and written data, the study’s themes gained more credibility, as they emerged from both data sources (Creswell & Creswell, 2018).
Finally, we used member checking (Creswell & Creswell, 2018) to request the participants’ feedback on the credibility of the data (Creswell & Poth, 2017). Member checking allows the study’s participants to become actively involved in and make additions to the data review process (Birt et al., 2016). Cole emailed the participants transcriptions of their interviews and asked them to review and make any additions or changes they would like to the transcriptions, allowing them ownership of their thoughts and words and increasing the trustworthiness of the data (Birt et al., 2016). In addition, Cole discussed the findings of the study with the participants as the themes and patterns emerged (Shenton, 2004).
Results
The study’s data yielded six main themes: (a) loss of control, (b) loss of identity, (c) fear of seeking mental health services, (d) difficulty accessing mental health services, (e) the military spouse community as a protective factor, and (f) desire for better communication about available mental health resources.
Theme 1: Loss of Control
Each of the 10 participants perceived their circumstances as a military spouse to be out of their control. For example, all of the participants mentioned deployments, especially those on short notice, to be a risk factor for suicide. One spouse described how her active-duty husband “might be home on Thursday and then he’s gone the next day. He finds out on such short notice, that’s really tricky, and a lot of my friends are constantly, you’re just so constantly anxious all the time.”
Four of the participants described how they fear for their spouse’s safety during these deployments, which impacts their mental health. One spouse, for example, described how she lives “just constantly not knowing what’s happening, but then being fearful for the significant other as well.” Another spouse explained how spouses live with a “constant fear of whether or not your spouse will return.” One participant discussed how military spouses are thus more prone to mental health issues:
[T]he stress of your life and the stress you have over your spouse’s military career, whether they’re in danger or not, worrying about their mental health . . . probably aggravates all of the mental disorders that anyone could experience, but just magnifies them if you’re a military spouse.
Participants also felt like they lacked control because of frequently relocating. All 10 participants described the stress involved with moving unpredictably. One spouse described how “you’re always worried about what’s coming next and what you can plan for and what you can’t plan for.” Another participant mirrored this same sentiment: “It’s that ‘Where are we going to be next? We just moved here, but I know in two years we’re going to move again’ type deal . . . always just kind of being on your toes and not knowing what to expect.” Another spouse expressed similar thoughts: “I hope for the best but expect the worst, which is kind of sad, but that is the kind of mentality I’ve had to live by because of how unpredictable this lifestyle is.”
As a result of these constant relocations, spouses are separated and isolated from family and friends, or their “network of support” in the words of one participant. All of the participants recognized the risk of losing this support with regard to their mental health. One spouse, for example, explained the danger of not having “long-standing relationships where you could say like, ‘Wow that person really seems like they’re going through something.’”
Theme 2: Loss of Identity
All 10 participants struggled with a loss of their identity, especially regarding their careers. Many participants described how career struggles and finding purpose are related to spousal mental health. One spouse explained how “not having that career is part of the anxiety and depression. And not having a purpose in life.” Another spouse described the struggle to maintain a career: “Eventually, it kind of weighs on you and eventually your mind can play tricks on you and you feel like you’re not worthy.” One participant summed up these career struggles in these words: “Part of being a military spouse is sacrificing your own life . . . there’s a lot of hurt and loneliness and sacrifice.”
In addition to this struggle for career identity and purpose, five of the participants described how the military fails to recognize their value. One spouse described how spousal suicide “is definitely brushed under the rug because people are kind of like, ‘You’re not going to war, you’re not doing any of these things.’” Another participant described her own experiences: “We’ve had situations where wives were struggling, but . . . he couldn’t get off that day, he had to report in because she’s not at the hospital . . .it’s not serious.” Another explained how “the military in general, they’re so focused on their job that they kind of forget that we’re all humans and that we are people.” One participant said that “spouses get beat down and they just kind of feel like there’s the whole ‘If the military wanted you to have a family, they would have issued you one.’”
The participants also described the military spouse’s tendency to prioritize family and the military over oneself and the impact of this inclination on spouses’ mental health. “So much of the burden of the family falls onto the military spouse, I think it’s easy for the spouse to not consider their own mental health a priority, and therefore the risk factors may go undetected or untreated.” Another described how spouses “go through this constant cycle that’s always churning. You move to a new place, you try to get settled . . . then we hit the point of going, ‘Ok, now what about me?’ If we ever get to that point.” One spouse described that after each of the moves and deployments, “I feel like we lose a sense of ourselves too . . . it’s like having a new baby all of the time. . . . You kind of reach a point where you’re like, ‘Where am I? What the heck am I doing?’”
As a result of prioritizing family and the military over themselves, spouses feel unworthy of receiving mental health services and feel guilty for suffering, as described by eight of the participants. One spouse explained that “spouses can feel weak or feel like they’re not holding up their end of the bargain if they get help.” Another participant noted that spouses “consider themselves less worthy of getting treatment or that their problems [are] not as important.” Finally, a spouse explained that there is a “weird mentality, I think, in the military spouse community, where you don’t complain because someone else has it worse. . . . If you’re an Air Force spouse, maybe the Army deployments are longer, so you just don’t want to complain.”
Theme 3: Fear of Seeking Mental Health Services
Despite these challenges that military spouses face, eight of the participants described a fear of seeking out mental health services. Five of the participants, for example, said that spouses fear appearing to be unstable or, as one spouse described, a “fear of being ostracized, or the fear of having people talk behind your back, or embarrassment.” One spouse explained how mental health issues are viewed as, “Oh, she was a crazy spouse. Oh, she got everything that she needed . . . so she was just kind of crazy.” Another participant described how a spouse was viewed after verbalizing her mental health struggles: “I’ve been told by other spouses not to go hang out with her in group settings because she’s batshit crazy.” One spouse noted that “there’s still that stigma of reaching out and being known to have the mental health issue.” Finally, spouses may fear being honest with their medical providers for this same reason. One participant described her own perception of this fear of being transparent with the doctor regarding a suicidal assessment: “If you answer it honestly, sometimes you’re like ‘They’re going to put me in a padded room if I really tell you what my last 2 weeks has been like.’”
In addition to appearing unstable, seven of the participants described how military spouses fear that seeking mental health services would negatively impact or bring “backlash” on their service member’s career. One participant noted: “People keep it quiet because they don’t want their spouse, their military member, to not get promoted or not get more responsibility and stuff like that because they’re not keeping it together.” Another participant stated that often “you run into people who are kind of skittish about going just because of the stigma.” She further explained that “you don’t want to hurt your husband’s career, and that’s what you’ve heard for a long time. He looks like he can’t handle the situations at home.’”
Theme 4: Difficulty Accessing Mental Health Services
Spouses who do decide to seek help for their mental health may experience difficulties in securing an appointment, as described by six of the participants in this study. Each of these spouses expressed difficulties with finding a mental health provider in the community or accessing mental health treatment at a military facility. One participant explained that “the reality is they can’t guarantee that the local community and local providers will be able to provide everything we need when we need it.” Another spouse expressed frustration that “TRICARE can sometimes be a pain when you’re trying to schedule something, and it will make you schedule at 6 weeks out because that’s the first available.” One participant described her experience with trying to find a counselor covered by TRICARE. She stated, “You hope that you get an appointment and hope you can jive with whoever you called because you may have to wait another month or two to try to find someone else.” Three spouses in the study also expressed concern about the consistency of care due to frequent relocations. One participant explained the need to streamline mental health services at each duty station “so that if [spouses] are seeing a psychiatrist in one place and they go to the next place, they’re not waiting for 2 or 3 months before they can get in to see a new psychiatrist.”
Five of the study’s participants also expressed concern over not having access to a mental health specialist. For example, one spouse shared that “the person I did see, who was a social worker, I just don’t feel was very equipped to talk to me about the things I wanted to talk about.” Another spouse described her perception of military family life consultants’ work with spouses on military bases:
They just kind of give them the same spiel, like you should exercise, make sure you’re eating well, getting enough sleep, instead of saying, “You know what? This is outside of the realm of what I can handle, let’s get you in to the type of professional that you need.”
Theme 5: The Military Spouse Community as a Protective Factor
In the midst of these mental health challenges and difficulty seeking and accessing mental health services, seven of the participants described the military spouse community as a protective factor against suicidal ideation. As one participant explained, “Anyone can try to take their own life, but if they have people around them who are looking out for them, who are with them physically and emotionally, it’s harder to do.” In addition, one participant pointed out that the spouse community can offer a sense of shared understanding: “Someone else probably very close by has gone through the same thing that you have . . . and you’re not the first person to go through this and someone might be able to help lighten your load.” The participants emphasized the need to create “a friendly, inclusive environment where spouses can network and establish relationships” as well as establish a “connection and feeling of belonging.” One participant noted that within this environment and community, it is important to normalize conversations about mental health in order to decrease the stigma attached to it. “Letting people see that while we might post pretty pictures on Facebook and someone looks all together when they’re at that unit function, we’ve all had to reach out for help, and looking at that as being strong.”
To increase this protective factor as a community, six spouses described the importance of training for spouses geared toward suicide prevention so they could recognize the signs of suicide in others. One spouse said that training in “prevention measures of how to spot suicide, signs of suicide, or who to talk to, where to go, what to say” would be helpful “because spouses are probably already witnessing all of these signs in their homes or in their neighbors or in their friend groups of depression and suicidality.” Another participant described how “spouses could be looking out for friends, if they know some warning signs or give friends resources to go to so their friend could find it if they need help.”
Theme 6: Desire for Better Communication About Available Mental Health Resources
Each of the 10 participants expressed the need for the military to communicate more with them about mental health resources. One spouse, for example, pointed out that such “information needs to be put out there clearly at military hospitals, on military bases. . . . So I think the military could make it more clear, destigmatize it, and just make the programs more widely available and advertised.” In this proposed advertisement, the spouses would want to know “what kind of help we can get, what it costs, where we can get help, and will it matter to our spouse’s career?”
In addition to this suggested advertising, six of the participants said they would like the military leadership to communicate with them directly regarding available mental health resources specifically designed for spouses. One participant described how “it’s harder for the spouse to get that information . . . if they had information sent directly to them, I think they would be more willing to seek it out and use those resources.” Another spouse noted that “military spouses need to be presented with the resources available for their mental health directly instead of solely relying on the service member to relay the information.” As a result of receiving this information on resources available specifically for them, one participant explained that “the military spouse wouldn’t have to consider themselves less worthy of getting treatment or that their problems [were] not as important.”
Finally, six of the spouses suggested that the check-in process for each duty station could be a key opportunity to provide spouses with resources and preventative services. One spouse noted: “I think that when you move somewhere new there should be someone checking to make sure you’re okay and you’re not alone all the time. I think it’s the military’s responsibility to make sure there’s a process in place.” Another spouse proposed this check-in process as being “part of the standard procedure to make sure the spouse maybe is brought in and made aware of all of the programs that are available to them.”
Discussion
In this study, all of the military spouse participants described how spouses’ loss of control and loss of identity may contribute to their increased risk for suicide. These feelings resulted from continually moving to new duty stations (often unexpectedly), being isolated and separated from their support systems, fearing for their spouse’s safety during deployments, and struggling to maintain a sense of self and a career while making their families and the military their priority. Although they were committed to prioritizing the military lifestyle and their spouses’ career, these spouses did not feel that their needs were prioritized by the military in turn.
Each of these challenges for military spouses has been previously addressed in the professional literature (Eaton et al., 2008; Lewy et al., 2014; Mailey et al., 2018), although their direct correlation to suicidality has not yet been explored. Because increased levels of suicidality have been found in other populations when social isolation increases (Calati et al., 2019; Heuser & Howe, 2019; Pompili et al., 2007) or stressful life transitions or events occur (Oquendo et al., 2014; Paul, 2018), it is important to continue to consider how these risk factors impact military spouses’ suicidality.
Most of the participants likewise described the tendency of spouses to feel guilty for suffering, as they are not the ones on the battlefield, a new phenomenon not yet explored in the professional literature. One participant concluded that these feelings of guilt may lead to spouses feeling they are unworthy of using mental health resources intended for active-duty service members. To address these feelings of guilt, one spouse described the need to normalize the conversation about mental health among spouses, which would ameliorate these feelings of unworthiness and increase spouses’ use of resources. Finally, all of the participants felt that provision and advertisement of mental health and suicide prevention programs and services specifically for spouses would help them feel more confident in utilizing these services.
When speaking about risk factors associated with suicide, most spouses described their fears of the stigma associated with accessing mental health services and the struggles associated with finding mental health providers qualified to help them when they did decide to seek help. These fears and struggles directly correspond to results in past quantitative and mixed-methods research regarding barriers to treating military spouse mental health (Eaton et al., 2008; Lewy et al., 2014). The participants in this study likewise described their frustration with not being able to get an appointment with military or community providers. These struggles echo the results of previous research describing the challenges of spouses to access mental health services (Lewy et al., 2014), highlighting the consistency of this issue.
Although the participants’ struggles with mental health and mental health providers confirm the findings of existing studies, their suggestions for preventing suicide within the military spouse community are new ideas generated from this study. Primarily, the participants focused on the community itself as a protective factor against suicide. They described how building a strong spousal community prevents feelings of isolation, as spouses can care for each other because they share common experiences of the military lifestyle. This sense of connection is especially important, as spouses are separated from their support systems when relocating from one duty station to the next (Ross et al., 2020). In order to strengthen the protective factor of their community, the spouses discussed how they wanted more training from military leadership in the areas of suicide prevention and intervention so that they can help others around them. Interestingly, contradictory themes arose in this study’s findings regarding the spouse community shunning those who were struggling with mental health issues and the spouse community serving as a much-needed protective factor. Perhaps the participants’ suggestions of focusing on normalizing mental health support within their community would help to reduce the current tendency to shun and would increase the tendency to support.
In addition to focusing on increasing the protective factor of the spouse community itself, all of the participants stated that they desired increased communication from the military regarding mental health services and programs available specifically to them. Some of the spouses suggested that a direct line of communication from military leadership to spouses would be helpful for finding out about mental health resources available to them, as well as to their spouses. This communication would involve more strategic and widely spread advertising about suicide prevention resources and mental health services in places that spouses often frequent, such as military hospitals or on-base/on-post facilities.
Finally, several spouses suggested an innovative, structured check-in process at each duty station that would promote spousal awareness and understanding of the resources available to them. They explained that this check-in would provide an immediate sense of connection and community for the spouse and a way to formally network with other spouses in the area. This formalized check-in process carried out by the administration at the new duty station may be especially helpful for newer spouses who may not be familiar with the military’s mental health resources or health care system or who may be hesitant to reach out on their own to make connections with others, a pattern noticed by three of the most senior spouses in this study.
Implications for Future Training and Practice
Both the military community and the mental health counseling profession are called to recognize the mental health struggles that military spouses face in order to help prevent suicide in this population. Military leadership should strategize ways to provide easier access to mental health services for spouses, including suicide prevention programs designed specifically for this population. In addition, suicide education programs for spouses may help them identify warning signs in others, ultimately strengthening the protective factor of the military spouse community. Military leadership should also work to reduce the stigma of receiving mental health services, not only for active-duty service members, but for their family members as well. Military leaders may likewise consider the participants’ suggestions regarding direct communication between military leadership and spouses, including a formalized check-in process for each duty station. Each of these suggestions offers a solution to the challenges outlined by both the professional literature and the spouse participants in this study regarding the mental health challenges faced by spouses and the risk factors of military spouse suicide.
Next, mental health counselors are called to be aware of and screen for the risk factors for suicide in the military spouse population that may be correlated to the inherent challenges that the military lifestyle brings. As prevention is a primary focus within the counseling profession (Sale et al., 2018), counselors might create preventative, psychoeducational groups for spouses to enhance their sense of connectedness and wellness. These groups would serve to identify spouses who may need additional supportive services to mitigate risk of depression and anxiety as well as other mental health issues. Additionally, when relocations occur, counselors should consider connecting their military spouse clients with mental health services in their new location and, with the permission of the client, reach out to those providers to ensure continuity of care. Finally, mental health counselors should actively seek out and build partnerships with military leadership in order to develop evidence-based resources specific to preventing suicide in the spouse population and to reduce the mental health stigma present in both active-duty service members and spouse communities.
Limitations
Several limitations to this study exist related to the nature of qualitative methodology. First, in qualitative research, the researcher is the primary source of data collection and analysis. Thus, inherent biases exist throughout this data collection and analysis process (Anderson, 2010). However, bracketing and reflexivity reduced the potential impact of this limitation. Additionally, because mental health stigma exists within the military community, it is possible that participants were guarded during their interviews. Prolonged engagement assisted with mitigating this limitation. Finally, because of the nature of qualitative research, the sample size of the study is small (Atieno, 2009). For instance, the sample in this study did not include the perspectives of any male spouses or spouses who are African American or Hispanic. Additionally, although the sample includes Army, Navy, Air Force, and Coast Guard spouses, no Space Force or Marine Corps spouses are represented. Because of these limitations in gender, ethnicity, and branches, the sample is not representative of the military spouse community as a whole.
Implications for Future Research
Given these limitations of qualitative research, future quantitative research might focus on specific causes of suicide among military spouses. For example, studies might look at the characteristics of spouses who have committed suicide to detect any patterns or correlations that may exist. There should be particular focus on exploring any ethnic, racial, sexual minority, or gender identity disparities. Future researchers could pilot training programs in the military aimed at preventing military spouse suicide to develop best practices in this area. Finally, future qualitative studies should focus on the experiences of male military spouses. This is critical as the male military spouse suicide rate was recently found to be statistically higher than the overall male suicide rate in the U.S. population (40.9 per 100,000 and 28.4 per 100,000, respectively; DOD, 2020a).
Conclusion
Overall, the military spouses’ perceptions of risk factors for suicide in this study align with previous studies regarding military spouse mental health that have been conducted throughout the past 12 years. With a new knowledge of the number of spouses that are committing suicide, it is imperative that both the counseling profession and military leadership continue to work toward solutions for spousal mental health. These stakeholders are called to recognize the inherent risk factors of the military lifestyle and provide military spouses with the resources, training, and services that they need (and want) to address and prevent suicide within their community.
Disclosure and Disclaimer Statements
This research was partially funded by a faculty research grant from Arkansas State University.
The opinions and assertions expressed herein are those of the author(s) and do not necessarily reflect the official policy or position of the Uniformed Services University or the Department of Defense.
This research protocol was reviewed and approved by the Arkansas State University Institutional Review Board (IRB) in accordance with all applicable Federal regulations governing the protection of human subjects in research.
Neither the authors nor their family members have a financial interest in any commercial product, service, or organization providing financial support for this research.
References
Allen, E. S., Rhoades, G. K., Stanley, S. M., & Markman, H. J. (2011). On the home front: Stress for recently deployed Army couples. Family Process, 50(2), 235–247. https://doi.org/10.1111/j.1545-5300.2011.01357.x
Anderson, C. (2010). Presenting and evaluating qualitative research. American Journal of Pharmaceutical Education, 74(8), 141. https://doi.org/10.5688/aj7408141
Atieno, O. P. (2009). An analysis of the strength and limitation of qualitative and quantitative research paradigms. Problems of Education in the 21st Century, 13, 13–18. http://www.scientiasocialis.lt/pec/files/pdf/Atieno_Vol.13.pdf
Baer, M. D. (2019). The experiences of spouses/partners of military RPA pilots and sensor operators: A generic qualitative study (Order No. 27666760). Available from ProQuest Dissertations & Theses Global. (2331474736).
Barrett, A., Kajamaa, A., & Johnston, J. (2020). How to . . . be reflexive when conducting qualitative research. The Clinical Teacher, 17(1), 9–12. https://doi.org/10.1111/tct.13133
Birt, L., Scott, S., Cavers, D., Campbell, C., & Walter, F. (2016). Member checking: A tool to enhance trustworthiness or merely a nod to validation? Qualitative Health Research, 26(13), 1802–1811. https://doi.org/10.1177/1049732316654870
Blosnich, J. R., Montgomery, A. E., Dichter, M. E., Gordon, A. J., Kavalieratos, D., Taylor, L., Ketterer, B., & Bossarte, R. M. (2010). Social determinants and military veterans’ suicide ideation and attempt: A cross-sectional analysis of electronic health record data. Journal of General Internal Medicine, 35(6), 1759–1767. https://doi.org/10.1007/s11606-019-05447-z
Blue Star Families. (2019). 2019 Military Family Lifestyle Survey executive summary. https://bluestarfam.org/wp-content/uploads/2020/03/BSF-2019-Survey-Exec-Summary-Digital-rev200305v2.pdf
Britt, T. W., Jennings, K. S., Cheung, J. H., Pury, C. L. S., & Zinzow, H. M. (2015). The role of different stigma perceptions in treatment seeking and dropout among active duty military personnel. Psychiatric Rehabilitation Journal, 38(2), 142–149. https://doi.org/10.1037/prj0000120
Burke, J., & Miller, A. (2016). The effect of military change-of-station moves on spousal earnings. https://www.rand.org/pubs/research_briefs/RB9920.html
Calati, R., Ferrari, C., Brittner, M., Oasi, O., Olié, E., Carvalho, A. F., & Courtet, P. (2019). Suicidal thoughts and behaviors and social isolation: A narrative review of the literature. Journal of Affective Disorders, 245, 653–667. https://doi.org/10.1016/j.jad.2018.11.022
Center for the Study of Traumatic Stress. (2020). Financial stress and behavioral health in military servicemembers report. https://www.cstsonline.org/resources/resource-master-list/financial-stress-form-report
Christensen, M., Welch, A., & Barr, J. (2017). Husserlian descriptive phenomenology: A review of intentionality, reduction and the natural attitude. Journal of Nursing Education and Practice, 7(8), 113–118. https://doi.org/10.5430/jnep.v7n8p113
Cole, R. F. (2012). Professional school counselors’ role in partnering with military families during the stages of deployment. Journal of School Counseling, 10(7). http://www.jsc.montana.edu/jsc_2011-2015.html#2012
Cole, R. F. (2014). Understanding military culture: A guide for professional school counselors. The Professional Counselor, 4(5), 497–504. https://doi.org/10.15241/rfc.4.5.497
Creswell, J. W., & Creswell, J. D. (2018). Research design: Qualitative, quantitative, and mixed methods. (5th ed.). SAGE.
Creswell, J. W., & Poth, C. N. (2017). Qualitative inquiry and research design: Choosing among five approaches (4th ed.). SAGE.
Darawsheh, W. (2014). Reflexivity in research: Promoting rigour, reliability and validity in qualitative research. International Journal of Therapy and Rehabilitation, 21(12), 560–568. https://doi.org/10.12968/ijtr.2014.21.12.560
Eaton, K. M., Hoge, C. W., Messer, S. C., Whitt, A. A., Cabrera, O. A., McGurk, D., Cox, A., & Castro, C. A. (2008). Prevalence of mental health problems, treatment need, and barriers to care among primary care-seeking spouses of military service members involved in Iraq and Afghanistan deployments. Military Medicine, 173(11), 1051. https://doi.org/10.7205/milmed.173.11.1051
Heuser, C., & Howe, J. (2019). The relation between social isolation and increasing suicide rates in the elderly. Quality in Ageing and Older Adults, 20(1), 2–9. https://doi.org/10.1108/qaoa-06-2018-0026
Institute for Veterans and Military Families. (2016). The force behind the force. https://ivmf.syracuse.edu/wp-content/uploads/2016/07/The-Force-Behind-the-Force-Infographic.pdf
Korstjens, I., & Moser, A. (2018). Series: Practical guidance to qualitative research. Part 4: Trustworthiness and publishing. European Journal of General Practice, 24(1), 120–124. https://doi.org/10.1080/13814788.2017.1375092
Lewy, C. S., Oliver, C. M., & McFarland, B. H. (2014). Brief report: Barriers to mental health treatment for military wives. Psychiatric Services, 65(9), 1170–1173. https://doi.org/10.1176/appi.ps.201300325
Linn, M. W., Sandifer, R., & Stein, S. (1985). Effects of unemployment on mental and physical health. American Journal of Public Health, 75(5), 502–506. https://doi.org/10.2105/ajph.75.5.502
Mailey, E. L., Mershon, C., Joyce, J., & Irwin, B. C. (2018). “Everything else comes first”: A mixed-methods analysis of barriers to health behaviors among military spouses. BMC Public Health, 18, 1013. https://doi.org/10.1186/s12889-018-5938-z
Malacrida, C. (2007). Reflexive journaling on emotional research topics: Ethical issues for team researchers. Qualitative Health Research, 17(10), 1329–1339. https://doi.org/10.1177/1049732307308948
McNulty, P. A. F. (2003). Does deployment impact the health care use of military families stationed in Okinawa, Japan? Military Medicine, 168(6), 465–70. https://doi.org/10.1093/milmed/168.6.465
Meyer, K., & Willis, R. (2019). Looking back to move forward: The value of reflexive journaling for novice researchers. Journal of Gerontological Social Work, 62(5), 578–585.
https://doi.org/10.1080/01634372.2018.1559906
O’Keefe, P. H. (2016). Using Facebook to communicate with husbands while deployed: A qualitative study of Army wives’ experiences (Order No. 10196383). Available from ProQuest Central; ProQuest Dissertations & Theses Global. (1853893200).
Oquendo, M. A., Perez-Rodriguez, M. M., Poh, E., Sullivan, G., Burke, A. K., Sublette, M. E., Mann, J. J., & Galfalvy, H. (2014). Life events: A complex role in the timing of suicidal behavior among depressed patients. Molecular Psychiatry, 19(8), 902–909. https://doi.org/10.1038/mp.2013.128
Patton, M. Q. (2002). Qualitative research and evaluation methods (3rd ed.). SAGE.
Paul, E. (2018). Proximally-occurring life events and the first transition from suicidal ideation to suicide attempt in adolescents. Journal of Affective Disorders, 241, 499–504. https://doi.org/10.1016/j.jad.2018.08.059
Pompili, M., Amador, X. F., Girardi, P., Harkavy-Friedman, J., Harrow, M., Kaplan, K., Krausz, M., Lester, D., Meltzer, H. Y., Modestin, J., Montross, L. P., Mortensen, P. B., Munk-Jørgensen, P., Nielsen, J., Nordentoft, M., Saarinen, P. I., Zisook, S., Wilson, S. T., & Tatarelli, R. (2007). Suicide risk in schizophrenia: Learning from the past to change the future. Annals of General Psychiatry, 6, 10. https://doi.org/10.1186/1744-859X-6-10
Romo, V. (2019). Military families experience high stress, anxiety and unemployment, report says. https://www.npr.org/2019/02/21/696848723/military-families-experience-high-stress-anxiety-and-unemployment-report-says
Ross, A. M., DeVoe, E. R., Steketee, G., Emmert-Aronson, B. O., Brown, T., & Muroff, J. (2020). Outcomes of a reflective parenting program among military spouses: The moderating role of social support. Journal of Family Psychology, 34(4), 402–413. https://doi.org/10.1037/fam0000637
Sale, E., Hendricks, M., Weil, V., Miller, C., Perkins, S., & McCudden, S. (2018). Counseling on Access to Lethal Means (CALM): An evaluation of a suicide prevention means restriction training program for mental health providers. Community Mental Health Journal, 54(3), 293–301. https://doi.org/10.1007/s10597-017-0190-z
Sargeant, J. (2012). Qualitative research part II: Participants, analysis, and quality assurance. Journal of Graduate Medical Education, 4(1), 1–3. https://doi.org/10.4300/JGME-D-11-00307.1
Shenton, A. K. (2004). Strategies for ensuring trustworthiness in qualitative research projects. Education for Information, 22(2), 63–75. https://doi.org/10.3233/EFI-2004-22201
Substance Abuse and Mental Health Services Administration. (2015). Spouses and children of U.S. military personnel: Substance use and mental health profile from the 2015 National Survey on Drug Use and Health. https://www.samhsa.gov/data/sites/default/files/NSDUH-MilitaryFamily-2015/NSDUH-MilitaryFamily-2015.pdf
Tong, P. K., Payne, L. A., Bond, C. A., Meadows, S. O., Lewis, J. L., Friedman, E. M., & Maksabedian Hernandez, E. J. (2018). Enhancing family stability during a permanent change of station: A review of disruptions and policies. https://www.rand.org/pubs/research_reports/RR2304.html
U.S. Chamber of Commerce. (2017). Military spouses in the workplace: Understanding the impacts of spouse unemployment on military recruitment, retention, and readiness. https://bit.ly/3gfd96N
U.S. Department of Defense. (2018). Military spouse demographics and employment information. https://bit.ly/3gmfQ5i
U.S. Department of Defense. (2019). Annual suicide report. https://bit.ly/2TVxxkx
U.S. Department of Defense. (2020a). Annual suicide report. https://bit.ly/3czBXEn
U.S. Department of Defense. (2020b). DOD releases military spouse licensure report. https://bit.ly/3gn85Mq
Appendix A
Demographics
| Participant |
Age Group |
Gender |
Race |
Military Branch |
Spouse’s Rank |
Years as Spouse |
| Participant 1 |
30–39 |
Female |
White |
Army |
Officer |
10 |
|
Participant 2 |
18–29 |
Female |
White |
Army |
Officer |
1 |
|
Participant 3 |
30–39 |
Female |
White |
Coast Guard |
Enlisted |
11 |
|
Participant 4 |
18–29 |
Female |
White |
Navy |
Officer |
3 |
|
Participant 5 |
30–39 |
Female |
Asian |
Air Force |
Officer |
2 |
|
Participant 6 |
40–49 |
Female |
White |
Army |
Officer |
20 |
|
Participant 7 |
40–49 |
Female |
Asian |
Air Force |
Officer |
20 |
|
Participant 8 |
40–49 |
Female |
White |
Air Force |
Officer |
18 |
|
Participant 9 |
30–39 |
Female |
White |
Navy |
Enlisted |
8 |
|
Participant 10 |
30–39 |
Female |
White |
Navy |
Officer |
2 |
Appendix B
Interview Protocol
First Interview
What are your perceptions of suicide in the military spouse community?
What are the risk factors for suicide in the military spouse population?
What mental health challenges do military spouses face?
What resources currently exist to help prevent military spouse suicide?
What would you like to let the civilian world know about your life as a military spouse that they might not be aware of?
Is there anything else you would like to add?
Second Interview
Do you have anything else to add from our first interview?
What do you think causes military spouses to commit suicide?
What needs to be done to prevent suicide in the military spouse community?
What might be the consequences of not addressing suicide in the military spouse community?
What type of mental health support is most needed for the military spouse community?
How would your mental health differ, if at all, if you weren’t a military spouse?
Is there anything else you would like to add?
Follow-Up Email Questions
Is there anything else you would like to add to your interview responses?
What was it like for you to participate in this study?
What is the most important resource that military spouses need to prevent future suicides?
Rebekah F. Cole, PhD, NCC, LPC, is formerly an assistant professor at Arkansas State University and is now a research associate professor at the Uniformed Services University. Rebecca G. Cowan, PhD, NCC, BC-TMH, LPC, DCMHS, is a core faculty member at Walden University. Hayley Dunn is a graduate student at Arkansas State University. Taryn Lincoln is a graduate student at Arkansas State University. Correspondence may be addressed to Rebekah Cole, Uniformed Services University of the Health Sciences, Department of Military and Emergency Medicine, 4301 Jones Bridge Rd., Bethesda, MD 20814, rebekah.cole@usuhs.edu.
Dec 9, 2015 | Article, Volume 5 - Issue 4
Lindsey Mitchell
The purpose of this study was to explore the relationship of five variables—primary appraisal, secondary appraisal, coping skills, social support and stigma—to bereavement among women whose military spouses had completed suicide. Four correlations to bereavement (primary appraisal, secondary appraisal, coping skills and stigma) were significant. Hierarchical multiple regression analysis assessed the overall relationship of bereavement (the criterion variable) to the five predictor variables, along with the unique contribution of each predictor variable. In the regression, five of six models (all except Model 4) showed significance. The dissertation on which this manuscript is based has the following practical implications: statistically significant correlations between bereavement and constructs of Lazarus’ Cognitive Model of Stress (LCMS), as well as the significance of Lazarus’ construct of primary appraisal within Model 6, indicate that LCMS holds promise for understanding symptoms of bereavement in women whose military spouses have completed suicide.
Keywords: suicide, bereavement, military, spouse, Lazarus
Reports indicate that suicides in the U.S. military surged to a record number of 349 in 2013. This figure far exceeds the 295 American combat deaths in Afghanistan in 2012 and compares with the 201 military suicides in 2011 (National Institute of Mental Health [NIMH], 2013). Some private experts predict that the trend will worsen this year (Miles, 2010).
From 2008–2010, the Army reported the highest number of suicides (n = 182) among active duty troops; whereas the Navy and Air Force reported 60 and 59 respectively (National Institute of Mental Health [NIMH], 2013). The Marine Corps had the largest percentage increase in suicides in a period of 2 years (Lamorie, 2011). U.S. veterans accounted for 20% of the more than 30,000 suicide deaths in the United States in 2009. Between 2003 and 2009, approximately 6,000 veterans committed suicide annually, an average of 18 suicides each day (Congressional Quarterly, 2010; Miles, 2010). During the 2009 fiscal year, 707 members of the veteran population committed suicide, and another 10,665 made unsuccessful suicide attempts (Miles, 2010). Certain experiences of military service members (e.g., exposure to violence, act of killing the enemy, risk of injury, exposure to trauma) increase suicidal tendencies (Zamorski, 2011).
For every person who completes suicide, an estimated 20 people experience trauma related to the death (NIMH, 2010). This suggests that from the 349 military suicides in 2013, approximately 7,000 people have experienced related trauma. Suicide survivors are family members and friends whose lives significantly change because of the suicide of a loved one (Andriessen, 2009; Jordan & McIntosh, 2011; McIntosh, 1993). Survivors of suicide may have higher risk for a variety of psychological complications, including elevated rates of complicated grief and even reactive suicide (Agerbo, 2005).
It is also important to note that suicide survivors might not differ significantly from other bereaved groups regarding general mental health, depression, post-traumatic stress disorder symptoms and anxiety (Sveen & Walby, 2008). Examining the impact of suicide on surviving military family members may provide important information on minimizing negative consequences, including possible survivor suicide.
Military deaths are often sudden, unexpected, traumatic and/or violent in nature, and the family is conditioned to anticipate these types of deaths. In contrast, death by suicide is not anticipated and might not be handled well among military families (Martin, Ghahramanlou-Holloway, Lou, & Tucciarone, 2009). Suicide within the military culture is a traumatic as well as a unique experience. Service members and their families struggle with the visible and invisible wounds of war and the aftermath that combat deaths leave for the survivors. When a service member’s trauma leads to suicide, the military community is less trained and conditioned to process the grief than when death occurs as a direct result of military service (Zhang & Jia, 2009).
Stress plays a role in the grief process within the military culture when it relates to suicide. The chief identifying feature of military culture is warfare, which in turn leads to the claiming of human lives (Siebrecht, 2011). Siebrecht argued that bereavement can only be overcome if people adopt a more rational attitude and grant death its natural place in life. Association with the military ensures that most families will have to experience some form of bereavement and many forms of loss during times of war (Audoin-Rouzeau & Becker, 2002). Military men and woman are less equipped than the general population when it comes to their culture’s acceptance of outward demonstration or sharing of the emotional experience of grief (Doka, 2005).
Stigma
Historically, the stigma of suicide has been present in society (Cvinar, 2005). The biggest obstacles that families with members who have completed suicide confront are acts of informal social disapproval. The surviving family may be suspected of being partly blameworthy in a suicide death and consequently may be subjected to informal isolation and shunning (Bleed, 2007). The stigma of suicide can be subtle. It can be manifested in overt actions taken against the survivors (i.e., placing blame on the family), as well as by omitted actions (i.e., not receiving life insurance), which are probably far more common. When people experience the untimely loss of a family member, there can be feelings of being offended, wounded or abandoned (Neimeyer & Jordan, 2002). The stigmatization experienced by survivors may complicate their bereavement process (Cvinar, 2005; Jordan, 2001; McIntosh, 1993). This complexity results in communication issues, social isolation, projection of guilt, blaming of others and scapegoating (Harwood, Hawton, Hope, & Jacoby, 2002; Lindemann & Greer, 1953). There is a lack of research in the professional literature addressing the grief of surviving military family members impacted by the death, including suicide, of a loved one (Lamorie, 2011).
Suicide and Bereavement
Jordan (2001) researched suicide bereavement and concluded that there are several underlying reasons that it differs from other types of mourning. Jordan summarized that “there is considerable evidence that suicide survivors are viewed more negatively by others and by themselves” (p. 93) and that suicide “is distinct in three significant ways: the thematic content of grief, the social processes surrounding the survivor, and the impact suicide has on family systems” (p. 91). In reviewing the social processes surrounding suicide, Jordan’s analysis supports those of Worden (1991) and Ness and Pfeffer (1990), saying that “there is considerable evidence that survivors feel more isolated and stigmatized than other mourners, and may be viewed more negatively by others in their social network” (p. 93). Most traumatic death survivors will face questions regarding their own culpability in their loved one’s decision to take his or her own life. Survivors may find themselves repeatedly pondering missed warning signs and risk factors (Parrish & Tunkle, 2005). Four primary factors that distinguish the complexities of suicide bereavement for families include stigma, questions about reasons, issues of remorse and guilt, and various logistical and legal factors unique to suicide that necessarily influence the events and processes following death (Minois,1999). The question of why often comes up given the pervasive sense that suicide is a preventable event. This line of thought can often define the grief process. Combined with factors of shock from the sudden, often violent nature of the death, these questions are virtually unavoidable. In some cases, answers to questions of why may never be forthcoming or satisfactory (Steel, Dunlavy, Stillman, & Pape, 2011). Among military families, bereavement is complex. A military death often has circumstances not normally found in the civilian world. It is most likely unexpected, potentially traumatic, occurring in another country, publicized by the media, and enveloped in the commitment to duty and country. Surviving family members of military personnel are often parents, siblings, grandparents and spouses. Military widows are young, often with young families, and are living at a duty station, far away from family and longtime friends (Katzenell, Ash, Tapia, Campino, & Glassberg, 2012).
Bereavement in the Military Culture
Bereavement is a part of the military culture but is often misinterpreted as a weakness that will elicit limited outside support. Military men and women in general are uninformed about the cultural acceptability of outwardly demonstrating their grief or sharing the emotional experience of the loss (Doka, 2005). Although traditional mental health treatments predominantly encourage emotional vulnerability, the military culture values emotional toughness (Kang, Natelson, Mahan, Lee, & Murphy, 2003) and stigmatizes mental illness (Doka, 2005). These attitudes can often deter service members from seeking assistance that could help them to overcome physical and mental health issues. Military culture affects the impact of suicide on families. Each spouse and family has a different bereavement process, and this process is influenced by stigma, social support and ability to cope. In the U.S. military, these issues can be a hindrance to seeking services and can lead to feelings of isolation, which in turn are a risk factor for suicide (Christensen & Yaffe, 2012).
Conceptual Framework
The conceptual framework of Lazarus’ Cognitive Model of Stress (LCMS) was used to frame this study. The underlying construct of this model states that times of uncertainty and difficulty may assist in understanding a person’s ability and capacity to cope with the suicide of a loved one. In general, when people encounter a difficult situation, they employ strategies for dealing with and lessening perceived stress (Groomes & Leahy, 2002).
LCMS (Lazarus & Folkman, 1984) has served as a useful lens for examining the interaction between a person and situational demands. Burton, Farley, and Rhea (2009) used LCMS to frame a study of the relationship between level of perceived stress and extent of physical symptoms of stress, or somatization, among spouses of deployed versus non-deployed servicemen. Eberhardt and associates (2006) examined Lazarus and Folkman’s 1984 stress theory regarding the ways that stress mediators and perceived social support may affect anxiety (as a stress response). The above studies show the usefulness of LCMS in depicting the impact of stress and coping on perceived anxiety, acceptance, ability to lead mentally and physically satisfactory lives, and perception of social support.
LCMS includes primary appraisal, secondary appraisal, coping and perceived social support. Stress is defined as a person’s relationship to his or her environment, specifically a relationship that the person perceives as exceeding his or her resources and endangering well-being. This model supports that the person and the environment are in a dynamic, reciprocal and multidimensional relationship. This conceptualization suggests that people’s perception of stress is related to the way they evaluate, appraise and cope with difficulties.
Stress can be measured by the way an individual appraises a specific encounter. Lazarus and Folkman (1984) presented two types of appraisal. The first is primary appraisal, defined as an individual’s expressed concern in terms of harm, loss, threat or challenge. Harm and loss appraisals refer to loss or damage that has already taken place; threat appraisal refers to harm or loss that has not yet occurred (i.e., anticipatory loss); and challenge appraisal refers to the opportunity for mastery or growth (Lazarus & Folkman, 1984). The second type is secondary appraisal, defined as the focus on what the individual can do to overcome or prevent harm. Lazarus and Folkman suggested that an appraisal of threat is associated with coping resources that can mediate the relationship between stressful events (e.g., loss of spouse to suicide) and outcomes (e.g., ability to seek mental health services).
Coping resources are the personal factors that people use to help them manage situations that are appraised as stressful (Lazarus & Folkman, 1984). Coping resources can be available to the person during the grief process or can be obtained as needed. This fact suggests that the grief process following a suicide is stressful and imposes demands on coping as the bereavement process evolves. Lazarus and Folkman (1984) defined coping as “constantly changing cognitive and behavioral efforts to manage specific external or internal demands that are appraised as exceeding the resources of the person” (p. 141). Coping is a dynamic process that is called into action whenever people are faced with a situation that requires them to engage in some special effort to manage that situation (Lazarus & Folkman, 1984). The ability to cope impacts a person’s bereavement process, and the ways and ability to cope vary with each individual. Stigma and the amount of perceived social support also influence the ability to cope (Bandura, 1997). These variables impact the bereavement process, especially with the added variable of death by suicide.
Social support can strengthen an individual’s position against the stressor and reduce the level of threat (Lazarus, 1996). Research suggests there are specific reasons why survivors do not seek out social support. McMenamy, Jordan, and Mitchell (2008) identified depression and a lack of energy as substantial barriers to obtaining social support.
People who experience a traumatic event are more likely to perceive barriers and not request medical and mental health services due to this lack of energy, lack of trust in professionals and depression (Amaya-Jackson et al., 1999). Provini, Everett, and Pfeffer (2000) stated that the stigma and social isolation that survivors experience can interfere with seeking social support and the willingness of social support networks to come to the aid of the survivor. A lack of social support can increase depression, a lack of energy to complete daily tasks and isolation. Limited social support is especially common for suicide survivors. Shame and guilt surrounding a suicide can impact survivors’ ability to seek social support; however, high social support can be linked to positive mental health.
Barriers to Bereavement
Many suicide survivors struggle with questions about the meaning of life and death, report feeling more isolated and stigmatized, and have greater feelings of abandonment and anger compared with other sudden death survivors (Callahan, 2000). Moreover, the feeling of relief from no longer having to worry about the deceased may distinguish survivors of suicide from survivors of other types of sudden death (Jordan, 2001). Experiencing suicide in one’s family increases risks for family members’ mental health and family relationships (Jordan, 2001). Despite the frequency of suicide, there is limited research focusing on the needs of surviving spouses (Miers, Abbott, & Springer, 2012).
The family system in which the spouses existed as a couple is destabilized by suicide, but the survivor must continue to function. Tasks that were carried out in the relationship must now be carried out by the survivor (Murray, Terry, Vance, Battistutta, & Connolly, 2000). Cerel, Jordan, and Duberstein (2008) stated that because suicide occurs within families, the focus on the aftermath of suicide within families and the impact on the spouse are important areas to investigate in order to determine exactly how to help survivors. Helping survivors to address practical, economic and legal issues, in addition to providing information and therapeutic intervention, is important (Dyregrov, 2002; Provini et al., 2000).
Purpose of the Study
Because of the frequency of suicide in the United States, the increased number of suicides within the U.S. military, and the impact of suicide on the family, the bereavement process among female spousal survivors of military suicides deserves further exploration. The purpose of this study was to explore bereavement in female spousal survivors of military suicides. Using LCMS, the study explored the relationship of bereavement and stigma, social support, primary appraisal, secondary appraisal, and coping skills among women whose military spouse had completed suicide.
Summary of the Study and Methodology
This study investigated the linear relationship between the dependent variable of bereavement and each of five independent variables—primary appraisal, secondary appraisal, coping skills, perceived social support and stigma—among women whose military spouses had completed suicide. The following hypotheses guided the study. Hypothesis 1 stated that there would be a relationship between bereavement and stigma; this positive relationship was significant. Hypothesis 2 stated that there would be a relationship between bereavement and social support; the relationship was not statistically significant. Hypothesis 3 stated that there would be a relationship between bereavement and primary appraisal; this positive relationship was significant. Hypothesis 4 stated that there would be a relationship between bereavement and secondary appraisal; this negative relationship was significant. Hypothesis 5 stated that there would be a relationship between bereavement and coping skills; this negative relationship was significant.
Using hierarchical regression analysis, the researcher examined the relationship of five independent variables—primary appraisal, secondary appraisal, coping skills, social support and stigma—to bereavement. The relationship was statistically significant. The model was a good fit and controlled for time since death (i.e., number of years since the person completed suicide). Therefore, for this sample, the five independent variables are components of a statistically significant model.
Participants and Recruitment
The participants in this study were women aged 18 and older who had lost a military spouse to suicide. Criteria for inclusion were that (a) the service member who had completed suicide had been either on active duty or of veteran status, (b) the survivor was female and 18 years of age or older, and (c) the survivor was considered a spouse. A spouse was defined as legally married to another person or living and cohabiting with another person in a marriage-like relationship, including a marriage-like relationship between persons of the same gender. Participants were chosen from seven national organizations serving veterans. The researcher recruited participants from these organizations by explaining the study and asking for volunteers. The director or assistant director of each organization distributed study information and materials through listservs and posted them on their Web sites. Once prospective participants received an e-mail, they decided whether they wanted to participate and whether they met the eligibility requirements. If the spouses decided to participate in the study, they would complete the survey through Survey Monkey.
Variables
Demographic variables included age, race/ethnicity, length of relationship with the deceased partner, the decedent’s military status (active or retired), the decedent’s length of service, and time elapsed since death. The survey also asked about the deceased’s rank, education level, surviving children and prior suicide attempts.
A self-report online survey was constructed using the following five instruments: the Core Bereavement Items (CBI; Holland, Futterman, Thompson, Moran, & Gallagher-Thompson, 2013), the Stigma of Suicide and Suicide Survivor Scale (STOSASS; Scocco, Castriotta, Toffol, & Preti, 2012), the Coping Self-Efficacy Scale (CSES; Chesney, Neilands, Chambers, Taylor, & Folkman, 2006), the Multidimensional Scale of Perceived Social Support (MSPSS; Zimet, 1988), and the Stress Appraisal Measure (SAM; Peacock & Wong, 1990). The SAM is one measure. However, the variables of primary stress appraisal and secondary stress appraisal within it were separated, and the questions within the SAM regarding primary stress appraisal were referred to as the primary stress appraisal measure (PSAM), and the remaining questions of the SAM were referred to as the secondary stress appraisal measure (SSAM). In addition to these assessments, participants would also answer 11 demographic questions and three open-ended questions. The survey was split into seven sections.
The first section had 11 demographic questions. The second section, comprised of the MSPSS, had 12 questions regarding social support of the participant and used a 7-point Likert scale. The third section, comprised of the CBI, had 26 questions regarding the participant’s ability to cope and used a 10-point Likert scale. The fourth section, comprised of the SAM, had 19 questions regarding participant’s stress appraisal measures and used a 4-point Likert scale. The fifth section, comprised of the STOSASS, had 17 questions regarding the participant’s perceived stigma and used a 4-point Likert scale. The sixth section, comprised of the CBI, had 17 questions regarding the participant’s bereavement process and used a 4-point Likert scale. The survey included the three following open-ended questions that were derived from the Grief Evaluation Measure (GEM) and reviewed by three licensed professional counselors working in the field of suicide bereavement: (1) What do you recall about how you responded to the death of your spouse at the time?; (2) What was the most painful part of the experience to you?; and (3) How has this experience affected your view of yourself or your view of your world? To analyze the qualitative responses, the researcher identified the most commonly recurring words or phrases used by participants for each question. Three experts in the field of grief and loss were consulted and confirmed the content and face validity of the survey.
Data Analysis
The Statistical Package for the Social Sciences (SPSS), a statistical software package, generated all of the statistics for this research investigation. A Pearson correlation analysis was conducted to determine whether there was a linear relationship between primary appraisal, secondary appraisal, social support, coping skills, stigma and bereavement for women whose military spouse had completed suicide. Following this analysis, a multiple regression was used to describe the relationships of the independent or predictor variables to the dependent or criterion variable (Lussier & Sonfield, 2004). Because LCMS states that it is possible to discern the order in which a person experiences each variable with regard to a particular event, the variables were entered into the regression using the following equation: Bereavement = {time since death} + {primary appraisal} + {secondary appraisal} + {coping skills} + {perceived social support} + {perceived stigma}.
Results
Descriptive Statistics
Descriptive statistics provided simple summaries of the demographic characteristics of the sample, as well as descriptors such as means and standard deviations for these characteristics. The sample was a well-educated, racially diverse group of women who had lost their military spouses to suicide. The majority of participants were non-Hispanic White females who had attended at least some college. Most were affiliated with the Army and had been married to the military member who had completed suicide. The majority of the partners had committed suicide while on active duty. The mean age of respondents was 33.48 years (SD = 5.20; SE = .373); their ages ranged from 23–50 years. The mean number of children aged 17 or under that were a product of the relationship with the service member was 1.12 (SD = .79; SE = .064); the range was 0–4 children. The mean number of prior suicide attempts by the service member (known/confirmed by the surviving female spouse) was 1.31 (SD = 1.06; SE = .096); the range was 0–4 prior suicide attempts.
Correlation Results
Using SPSS Student Version 22.0 software, a Pearson correlation coefficient was used to measure the relationship of bereavement, primary appraisals, secondary appraisals, coping skills, social support, and stigma among women whose military spouses had completed suicide. The correlation coefficient measures the strength and direction of the relationship among variables. When conducting a correlational analysis of two co-occurring variables, the researcher can indicate whether change in one is accompanied by systematic change in the other. Examination of intercorrelations among study variables indicated statistically significant correlations between bereavement and each of four independent variables: primary appraisal, secondary appraisal, coping skill, and stigma. The results for each correlation are presented separately and summarized below as well as in Table 1.
Control variable. There was a statistically significant relationship between time since death and bereavement for women whose military spouse had completed suicide, r(194) = .277, p < .01. The shorter the amount of time elapsed, the higher the bereavement scores.
Independent variables. Primary stress appraisal, r(193) = -.309, p < .01: There is a weak negative linear relationship between bereavement and primary stress appraisal. Secondary stress appraisal, r(193) = -.309, p < .01: There is a weak negative linear relationship between secondary stress appraisal and bereavement. Coping skills, r(193) = -.174, p = .015: There is a weak negative linear relationship between coping skills and bereavement. Social support, r(193) = -.039, p = .594: There is no linear relationship between perceived social support and bereavement. Stigma, r(193) = .252, p < .01: There is a weak positive linear relationship between perceived stigma and bereavement.
Table 1
Correlations for Independent, Dependent and Control Variables
CBI TSD PSAM SSAM MSPSS CSES
1. TSD .277*
2. PSAM -.309* -.167
3. SSAM -.309* -.151 .602*
4. MSPSS -.039 .032 .379* .172*
5. CSES -.174* -.167* .494* .473* .585*
6. STOSASS .252* .095 -.196* -.221* .022 -.253
Note: N = 194; CBI = Core Bereavement Items; TSD = Time Since Death (in months);
PSAM = Primary Stress Appraisal Measure; SSAM = Secondary Stress Appraisal Measure;
CSES = Coping Self-Efficacy Scale; MSPSS = Multidimensional Scale of Perceived Social Support; STOSASS = Stigma of Suicide and Suicide Survivor Scale.
*Significant at p < .05.
Multiple Regression
Following the correlational analysis, a multiple regression was utilized. This analysis was appropriate to describe the relationships between the independent or predictor and dependent or criterion variables in an objective manner (Lussier & Sonfield, 2004). The design was appropriate because the purpose of the study was to explain the relationships between variables.
Model 1 (TSD onto bereavement) yielded R = .277, R2 = .077, F(1, 125), p < .001. The portion of the variance explained was 7%. Model 2 (TSD and primary appraisal) yielded R = .431, R2 = .186, F(2, 124), p < .001. The portion of variance explained was 18.6%. Model 3 (TSD, primary appraisal and secondary appraisal) yielded R = .454, R2 = .206, F(3, 123), p < .001. The portion of variance explained was 20.6%. Model 4 (time since death, primary appraisal, secondary appraisal and coping skills) yielded R = .455, R2 = .207, F(4, 122), p < .001. The portion of variance explained was 20.7%. Model 5 (time since death, primary appraisal, secondary appraisal, coping skills and social support) yielded R = .471, R2 = .221, F(5, 121), p < .001. The portion of variance explained was 22.1%. Model 6 (time since death, primary appraisal, secondary appraisal, coping skills, social support, and stigma) yielded R = .482, R2 = .232, F(6, 120), p < .001. The portion of variance explained was 23.2% (see Table 2).
Table 2
Hierarchical Multiple Regression
| Model |
R |
R2 |
t |
p |
B |
β |
R2 Change |
| Model 1TSD |
.277
|
.077
|
61.600
3.228
|
.000
.002
|
.049
|
.277
|
0
|
| Model 2TSDPSAM |
.431
|
.186
|
19.482
2.696
-4.074
|
.000
.008
.000
|
.039
-.406
|
.222
-.335
|
.109
|
| Model 3TSDPSAMSSAM |
.454
|
.206
|
19.646
2.618
-1.947
-1.782
|
.000
.010
.054
.077
|
.038
-.254
-.192
|
.214
-.209
-.191
|
.02
|
| Model 4TSDPSAMSSAMCSES |
.455
|
.207
|
16.971
2.622
-1.952
-1.788
.266
|
.000
.010
.053
.076
.791
|
.038
-.262
-.199
.004
|
.216
-.216
-.198
.025
|
.001
|
| Model 5TSDPSAMSSAMCSESMSPSS |
.471
|
.221
|
12.989
2.307
-2.359
-1.111
-0.710
1.505
|
.000
.023
.020
.269
.479
.135
|
.034
-.335
-.132
-.012
.091
|
.192
-.276
-.132
-.083
.167
|
.015
|
| Model 6 TSDPSAMSSAMCSESMSPSSSTOSASS |
.482
|
.232
|
9.026
2.329
-2.187
-1.105
-0.320
1.107
1.280
|
.000
.022
.031
.271
.750
.271
.203
|
.034
-.312
-.131
-.006
.069
.086
|
.194
-.257
-.131
-.039
.128
.112
|
.010
|
Note: TSD = Time Since Death (in months); PSAM = Primary Stress Appraisal Measure; SSAM = Secondary Stress Appraisal Measure; CSES = Coping Self-Efficacy Scale; MSPSS = Multidimensional Scale of Perceived Social Support; STOSASS = Stigma of Suicide and Suicide Survivor Scale.
Qualitative Component
There is a growing interest in integrating qualitative data across quantitative studies to discover patterns and common threads within a specific topic or issue (Erwin, Brotherson, & Summers, 2011). The main aim of the qualitative questions within the survey is to gain insight into the participants’ world and capture their unique experiences (e.g., naturally occurring events and/or social or human problems) and their interpretations of these experiences (Jones, 1995; Sarantakos, 1993).
A total of 55 (28.4%) participants responded to the question, “What do you recall about how you responded to the death of your spouse at the time?” Of these, 24 stated recalling “sadness” as most frequent. Fifteen participants indicated disbelief, shock, feelings of helplessness or feelings of fear. Other participants’ responses included “trying not to think about what had happened,” crying, sobbing, physical symptoms, physical pain, collapsing, fainting, being unable to forget what happened, and being unable to recall or process the event. A total of 68 (35.1%) participants responded to the question, “What was the most painful part of the experience to you?” Of these, 50 reported physical and emotional numbness and only partial recollection of learning about the death (e.g., who told them, where they were when notified, immediate responses). These participants indicated that they could recall parts of the experience but struggled with identifying feelings or emotions directly following the event. Other responses included being hospitalized, contemplating suicide, refraining from eating, and feeling that their future had been lost. Although four reported contemplating suicide following the death of their spouse, no participants reported attempting suicide at any point. A total of 36 (18.6%) participants responded to the question, “How has this experience affected your view of yourself or your view of your world?” Of these, 15 participants indicated that they no longer feared death, while seven reported having a negative reaction to relationships. Eleven participants reported that they perceived stress as more threatening than before the suicide of their spouse and were unaware of the triggers that brought on stress during the bereavement process. Ten participants indicated that their view of love had changed since the loss of their spouse. Nine participants wrote about making an effort to enjoy life after the suicide of their spouse.
Discussion
This study investigated the relationships between bereavement and primary appraisal, secondary appraisal, coping skills, perceived social support and stigma among women whose military spouses had completed suicide. There are several study findings that deserve further exploration.
First, there was a statistically significant positive relationship between stigma and bereavement, suggesting that as female survivors perceive increased stigma regarding the suicide of their spouse, they present more symptoms of bereavement. Knieper (1999) suggested that bereavement following suicide is not the same as that following natural death. He reported that stigma and avoidance continue to be central issues for suicide survivors. Psychological projection of feelings of rejection and the actual social response to the survivor interact in a complicated manner. Worden (2009) also noted a difference between suicide bereavement and other forms of bereavement, suggesting that suicide is often associated with stigma and a sense of shame. Such shame can result in the complete isolation of the bereaved during the period immediately following the suicide event. Eaton and associates (2008) examined survivors’ barriers to seeking mental health treatment after the suicide of their partners and found that spouses were 70% less likely to seek treatment following a suicide, as compared to a natural death, and that stigma was a recurrent theme in the qualitative analysis. However, Eaton et al.’s study did not directly examine the impact of stigma on bereavement. It did show that stigma is an important variable that needs to be investigated further. The present study showed similar results to Eaton et al.’s (2008) research.
The qualitative comments recorded in the open-ended question section of the survey supported the study findings. For example, one participant responded, “I blamed myself for not doing more, not being there enough, or not being there when the death happened.” Another participant noted, “Suicide is one of the most difficult and painful ways to lose someone we love, because we are left with so many unanswerable questions.” One participant expressed the following:
[I felt] anger at family members for not assisting me with my husband and anger at physicians that treated my husband and were not able to see the warning signs or provide assistance in caring for them properly. I was then left with the scars after the death and had to explain to people what happened. I felt I got blamed and it was not my fault.
Several participants expressed “numbness and isolation.” Responding to stigma, people with mental health problems often internalize public attitudes and become embarrassed or ashamed. These feelings can lead them to conceal symptoms and fail to seek treatment (President’s New Freedom Commission on Mental Health, 2003). These survey responses assist in understanding the impact of stigma upon the military spouse survivors and imply that unanswered questions, as well as guilt, are important factors to explore in the grief process following a suicide.
Second, a statistically significant relationship between primary appraisal and bereavement was reported, suggesting that survivors who perceive the death of a spouse to be stressful are more likely to experience bereavement. This result is supported by the bereavement literature (Cvinar, 2005; Jordan, 2001; McIntosh, 1993). Lazarus (2005) argued that primary appraisal shows that it is not the situation, but the way a person interprets the situation, that affects the person’s experience. The way a person appraises a situation can impact the way the person reacts to it. Primary appraisal is an important step in processing the stress of bereavement, since grieving is such an individualized experience.
The qualitative comments recorded in the open-ended question portion of the survey supported the statistical relationship between primary appraisal and bereavement. For example, one participant indicated that her worldview had changed when she responded, “My world has become gray; I have made myself closed. I live in a rain cloud and now know that good people do bad things that change lives.” The participant had changed her worldview such that her world became a smaller, more restricted place. Another stated, “This death, this loss, makes small things seem insignificant. Material things are insignificant. Relationships with people are more important. I don’t have a fear of dying and in fact, feel like I will die at a young age.” This concept of primary appraisal is based on the idea that emotional processes are dependent on a person’s expectancies about the significance and outcome of a specific event. The same event within the same community (in this case, suicide within the military) can elicit responses of different quality, intensity and duration due to individuality in experiences and personality (Krohne, Pieper, Knoll, & Breimer, 2002). The different kinds of stress identified by the primary appraisal may be embedded in specific types of emotional reactions, thus illustrating the close conjunction of the fields of stress and emotion (Lazarus & Folkman, 1984).
Third, a statistically significant negative relationship was reported between secondary appraisal and bereavement, suggesting that survivors who make a negative appraisal of their ability to control the outcomes of their spouse’s death are more likely to experience bereavement. In the future, when examining outcomes of interventions that impact coping, beliefs about a person’s ability to perform specific behaviors related to coping would need to be highlighted. This concept is known as specific coping behaviors and is also pertinent to stress, coping theory and secondary appraisal (Chesney et al., 2006). Part of secondary appraisal is the judgment that an outcome is controllable through coping; another part addresses the question of whether or not the individual believes he or she can carry out the requisite coping strategy (Chesney et al., 2006; DiClemente, 1986; Hofstetter, Sallis, & Hovell, 1990).
The qualitative comments recorded in the open-ended section of the survey supported this finding. For example, one participant indicated her appraisal of the situation by stating, “Everyone must learn to face the misfortune, because life on the road will not be smooth.” Another stated that “time can dilute all and I must face life and accept my reality;” yet another wrote, “I want to work on longer range goals to give myself some structure and direction to my life and not focus on my loss. I am only interested in rebuilding my life.” However, other participants stated that it was harder to assess the loss and to move forward after the suicide. One participant stated the following:
I often find myself complaining to God about what seems senseless or unjust and unfair. I find myself bogged down in fear and even anger at myself or the person who died and “left” me. I do not accept what happen[ed] to me and my children.
Some participants reported not knowing what to do. An example of this feeling is the statement, “I perceive stress as threatening. I feel totally helpless.” Perceived self-efficacy, defined as a belief about one’s ability to perform a specific behavior, is a salient component of this theory. It highlights the importance of personal efficacy in determining the acquisition of knowledge on which skills are founded (Bandura, 1997; Chesney et al., 2006).
Fourth, a statistically significant negative relationship between coping skills and bereavement was reported, suggesting that survivors who believe they have a low ability to cope with their spouses’ death are more likely to experience bereavement. Although it is important for survivors to become familiar with the stress appraisal process, the way they assign meaning to their spouse’s death and their past experience with death also are important in their primary appraisal to the overall coping effort. One model of this process is the transactional model of coping (Lazarus & Folkman, 1984). This model of coping implies that a person’s appraisal of his or her interaction with a difficult event naturally evokes a coping response for dealing with the situation. Experiencing a suicide or living in a social environment that hinders, stigmatizes or isolates a person who has experienced a suicidal death may cause demands to exceed his or her resources for dealing with certain situations. Few studies have examined the natural coping efforts used by suicide survivors, or have identified specific problems and needs that survivors experience following the suicide of a significant other (McMenamy et al., 2008). Interventions with suicide survivors have limited effectiveness (Jordan & McMenamy, 2004). Provini et al. (2000) presented four categories of concerns for suicide survivors: concerns related to (a) family relationships, (b) psychiatric symptoms, (c) bereavement and (d) stress. Family-related problems were the most frequently mentioned type of concerns (Provini et al., 2000). Examples of family relationship concerns included inability to maintain parenting roles, inability to maintain family routines, existence of different coping styles within the family, and inability to provide appropriate emotional support to family members.
Qualitative comments recorded in the open-ended section of the survey supported this study finding. For example, one participant stated, “I often feel distracted, forgetful, irritable, disoriented, or confused. I try to remember how I got over a death in the past, sometimes it helps and sometimes it does not.” Another participant stated, “I know I need to start to form new relationships or attachments in my life but my mind [is] telling me ‘there must be some mistake,’ or ‘this can’t be true.’ ” Regarding bereavement, one participant wrote, “Grief is perhaps the most painful companion to death.” Addressing coping, one participant stated, “I must also adjust to working or returning to work after the death. I know things can’t go back to the way they were before, very difficult and painful to deal with and I better adjust to life.” These statements support the need to further explore the relationship between one’s ability to cope with the suicide of a spouse and one’s ability to experience and acknowledge feelings and move forward with everyday life activities (e.g., employment, childcare, financial obligations). Ability to cope impacts a person’s bereavement process; the ways and ability to cope vary with the individual. Stigma and amount of perceived social support have been correlated with ability to cope (Bandura, 1997). It is important to understand the individual impacts that stigma, social support, primary appraisal, secondary appraisal and coping have on bereavement. However, it is equally important to examine the relationships of these variables within the context of a model in order to establish future interventions for bereavement within the context of a suicide.
Fifth, results indicated that the model is statistically significant in predicting bereavement outcomes and provides considerable support for using the Lazarus model as a means of understanding the relationship between stress and bereavement when placed into the equation in a particular order: CBI = TSD + PSAM + SSAM + CSES + MSPSS + STOSASS.
This study suggests that the proposed model, using LCMS and assessment of stress, identifies the constructs associated with bereavement among women whose military spouses completed suicide. Future research could further explore the assessment of primary and secondary appraisal processes, coping, stigma, and social support enhancement programs and interventions to improve the bereavement process for military spouses. When survivors can identify and address their needs, the bereavement process following a suicide can begin (Christensen & Yaffe, 2012).
Limitations
First, the majority of the sample (54.1%) were non-Hispanic White, or Euro-American. Second, there is limited representation across military branches. Third, the study collected data from a self-administered electronic survey. Fourth, although the social support measure (i.e., MSPSS) has good reliability and measures social support as a general feeling of belonging to a social network that one can turn to for advice and assistance in times of need (Uchino, 2006), it does not delineate various types of social support. Finally, most of the sample consisted of women whose spouses had completed suicide while on active duty. Active duty members typically live on base and are well connected to the military community. When the military spouse dies, these supports are often no longer available, and the stigma of a suicide could strongly affect these women.
Recommendations for Future Studies
There are several practice implications from this study. The statistically significant correlations between bereavement and four other variables (primary appraisal, secondary appraisal, coping skills and stigma), as well as the significance of the LCMS construct of primary appraisal within Model 6, indicate that LCMS holds promise for understanding symptoms of bereavement in females following the suicide of a military spouse. Primary appraisal, the most significant variable within this study, could be highlighted within bereavement research on women whose military spouses have completed suicide. When conceptualizing the responses of these women, counselors and clinicians could use LCMS, examining the three components of primary appraisal (goal relevance, goal congruence and ego involvement) and exploring the ways these components present during the client’s bereavement process. The approach would focus on the role of maladaptive cognitions during times of stress (Sudak, 2009).
The reluctance of the military community to seek mental health support contributes to an inability to move through the bereavement process in a healthy way. Within the military community, it can be quite difficult to deal with the ambiguity of bereavement that is typically associated with emotional vulnerability (Lamorie, 2011). However, the current study suggests that four constructs—primary appraisal, secondary appraisal, coping and stigma—are significant when addressing the issues of bereavement in females who have lost a military spouse to suicide. Using LCMS to address cognitions, counselors might be able to assist a population whose members have been reluctant to seek mental health services in the past. Because the components of LCMS are correlated with bereavement, clinicians could use LCMS and cognitive stress research, which together seem to be a promising direction, when assisting women who have lost a military spouse to suicide.
Conflict of Interest and Funding Disclosure
The author reported no conflict of interest
or funding contributions for the development
of this manuscript.
References
Agerbo, E. (2005). Midlife suicide risk, partner’s psychiatric illness, spouse and child bereavement by suicide or other modes of death: A gender specific study. Journal of Epidemiology and Community Health, 59, 407–412. doi:10.1136/jech.2004.024950
Amaya-Jackson, L., Davidson, J. R., Hughes, D. C., Swartz, M., Reynolds, V., George, L. K., & Blazer, D. G. (1999). Functional impairment and utilization of services associated with posttraumatic stress in the community. Journal of Traumatic Stress, 12, 709–724. doi:10.1023/A:1024781504756
Andriessen, K. (2009). Can postvention be prevention? Crisis: The Journal of Crisis Intervention and Suicide Prevention, 30, 43–47. doi:10.1027/0227-5910.30.1.43
Audoin-Rouzeau, A., & Becker, S. (2002). 14–18: Understanding the great war. New York, NY: Hill and Wang.
Bandura, A. (1997). Self-efficacy: The exercise of control. New York, NY: Worth.
Bleed, J. (2007, February 19). Howell’s life insurance payout not a sure bet. Arkansas Democrat-Gazette.
Retrieved from http://www.arkansasonline.com/
Burton, T., Farley, D., & Rhea, A. (2009). Stress-induced somatization in spouses of deployed and nondeployed servicemen. Journal of the American Academy of Nurse Practitioners, 21, 332–339. doi:10.1111/j.1745-7599.2009.00411.x
Callahan, J. (2000). Predictors and correlates of bereavement in suicide support group participants. Suicide & Life-Threatening Behavior, 30, 104–124. doi:10.1111/j.1943-278X.2000.tb01070.x
Cerel, J., Jordan, J. R., & Duberstein, P. R. (2008). The impact of suicide on the family. Crisis: The Journal of Crisis Intervention and Suicide Prevention, 29, 38–44. doi:10.1027/0227-5910.29.1.38
Chesney, M. A., Neilands, T. B., Chambers, D. B., Taylor, J. M., & Folkman, S. (2006). A validity and reliability study of the coping self-efficacy scale. British Journal of Health Psychology, 11, 421–337. doi:10.1348/135910705X53155
Christensen, B. N., & Yaffe, J. (2012). Factors affecting mental health service utilization among deployed military personnel. Military Medicine, 177, 278–283.
Congressional Quarterly. (2010). Rising military suicide: The pace is faster than combat death in Iraq and Afghanistan. Retrieved from http://www.infiniteunknown.net/2010/01/01/rising-us-military-suicides-the-pace-is-faster-than-combat-deaths-in-iraq-or-afghanistan/
Cvinar, J. C. (2005). Do suicide survivors suffer social stigma: a review of the literature. Perspectives in Psychiatric Care, 41, 14–21. doi:10.1111/j.0031-5990.2005.00004.x
DiClemente, C. C. (1986). Self-efficacy and the addictive behaviors. Journal of Social and Clinical Psychology, 4, 302–315. doi:10.1521/jscp.1986.4.3.302
Doka, K. J. (2005). Ethics, end-of-life decisions and grief. Mortality, 10, 83–90. doi:10.1080/13576270500031105
Dyregrov, K. (2002). Assistance from local authorities versus survivors’ needs for support after suicide. Death Studies, 26, 647–668. doi:10.1080/07481180290088356
Eaton, K. M., Hoge, C. W., Messer, S. C., Whitt, A. A., Cabrera, O. A., McGurk, D., . . . Castro, C. A. (2008). Prevalence of mental health problems, treatment need, and barriers to care among primary care-seeking spouses of military service members involved in Iraq and Afghanistan deployments. Military Medicine, 173, 1051–1056.
Eberhardt, B., Dilger, S., Musial, F., Wedding, U., Weiss, T., & Miltner, W. H. (2006). Short-term monitoring of cognitive functions before and during the first course of treatment. Journal of Cancer Research & Clinical Oncology, 132, 234–240. doi:10.1007/s00432-005-0070-8
Erwin, E. J., Brotherson, M. J., & Summers, J. A. (2011). Understanding qualitative metasynthesis: Issues and opportunities in early childhood intervention research. Journal of Early Intervention, 33, 186–200. doi:10.1177/1053815111425493
Groomes, D. A. G., & Leahy, M. J. (2002). The relationships among the stress appraisal process, coping disposition, and level of acceptance of disability. Rehabilitation Counseling Bulletin, 46, 15–24.
Harwood, D., Hawton, K., Hope, T., & Jacoby, R. (2002). The grief experiences and needs of bereaved relatives and friends of older people dying through suicide: A descriptive and case-control study. Journal of Affective Disorders, 72, 185–194. doi:10.1016/S0165-0327(01)00462-1
Hofstetter, C. R., Sallis, J. F., & Hovell, M. F. (1990). Some health dimensions of self-efficacy: Analysis of theoretical specificity. Social Science & Medicine, 31, 1051–1056.
Holland, J. M., Futterman, A., Thompson, L. W., Moran, C., & Gallagher-Thompson, D. (2013). Difficulties accepting the loss of a spouse: A precursor for intensified grieving among widowed older adults. Death Studies, 37, 126–144. doi:10.1080/07481187.2011.617489
Jones, R. (1995). Why do qualitative research? British Medical Journal, 311(6996), 2–3. doi:10.1136/bmj.311.6996.2
Jordan, J. R. (2001). Is suicide bereavement different? A reassessment of the literature. Suicide and Life-Threatening Behavior, 31, 91–102. doi:10.1521/suli.31.1.91.21310
Jordan, J. R., & McIntosh, J. L. (2011). Grief after suicide: Understanding the consequences and caring for the survivors. New York, NY: Routledge.
Jordan, J. R., & McMenamy, J. (2004). Interventions for suicide survivors: A review of the literature. Suicide and Life-Threatening Behavior, 34, 337–349. doi:10.1521/suli.34.4.337.53742
Kang, H. K., Natelson, B. H., Mahan, C. M., Lee, K. Y., & Murphy, F. M. (2003). Post-Traumatic stress disorder and chronic fatigue syndrome-like illness among Gulf War veterans: A population-based survey of 30,000 veterans. American Journal of Epidemiology, 157, 141–148. doi:10.1093/aje/kwf187
Katzenell, U., Ash, N., Tapia, A. L., Campino, G. A., & Glassberg, E. (2012). Analysis of the causes of death of casualties in field military setting. Military Medical Journal, 177, 1065–1068.
Knieper, A. J. (1999). The suicide survivor’s grief and recovery. Suicide and Life-Threatening Behavior, 29, 353–364. doi: 10.1111/j.1943-278X.1999.tb00530.x
Krohne, H. W., Pieper, M., Knoll, N., & Breimer, N. (2002). The cognitive regulation of emotions: The role of success versus failure experience and coping dispositions. Cognition & Emotion, 16, 217–243. doi:10.1080/02699930143000301
Lamorie, J. (2011). Operation Iraqi Freedom/Operation Enduring Freedom: Exploring wartime death and bereavement. Social Work in Health Care, 50, 543–563. doi:10.1080/00981389.2010.532050
Lazarus, A. A. (2005). Is there still a need for psychotherapy integration? Current Psychology, 24, 149–152. doi:10.1007/s12144-005-1018-5
Lazarus, A. A. (1996). Behavior therapy & beyond. New York, NY: McGraw-Hill.
Lazarus, R. S., & Folkman, S. (1984). Stress, appraisal, and coping. New York, NY: Springer.
Lindemann, E., & Greer, I. M. (1953). A study of grief: Emotional responses to suicide. Pastoral Psychology, 4, 9–13.
Lussier, R. N., & Sonfield, M. C. (2004). Family business management activities, styles and characteristics: A correlational study. Mid-American Journal of Business, 19, 47–53.
Martin, J., Ghahramanlou-Holloway, M., Lou, K., & Tucciarone, P. (2009). A comparative review of U.S. military and civilian suicide behavior: Implications for OEF/OIF suicide prevention efforts. Journal of Mental Health Counseling, 31, 101–118.
McIntosh, J. L. (1993). Control group studies of suicide survivors: A review and critique. Suicide and Life-Threatening Behavior, 23,146–161. doi:10.1111/j.1943-278X.1993.tb00379.x
McMenamy, J. M., Jordan, J. R., & Mitchell, A. M. (2008). What do suicide survivors tell us they need? Results of a pilot study. Suicide and Life-Threatening Behavior, 38, 375–389. doi:10.1521/suli.2008.38.4.375
Miers, D., Abbott, D., & Springer, P. R. (2012). A phenomenological study of family needs following the suicide of a teenager. Death Studies, 36, 118–133. doi:10.1080/07481187.2011.553341
Miles, D. (2010). VA strives to prevent veteran suicides. Retrieved from http://www.defense.gov/news/newsarticle.aspx?id=58879
Minois, G. (1999). History of suicide: Voluntary death in western culture (L. G. Cochrane, Trans.). Baltimore, MD: Johns Hopkins University Press.
Murray, J. A., Terry, D. J., Vance, J. C., Battistutta, D., & Connolly, Y. (2000). Effects of a program of intervention on parental distress following infant death. Death Studies, 24, 275–305. doi:10.1080/074811800200469
National Institute of Mental Health. (2010). Statistics. http://www.nimh.nih.gov/health/statistics/index.shtml
National Institute of Mental Health. (2013). Suicide prevention. http://www.nimh.nih.gov/health/topics/suicide-prevention/index.shtml
Neimeyer, R. A., & Jordan, J. R. (2002). Disenfranchisement as empathic failure: Grief therapy and the co-construction of meaning. In K. J. Doka (Ed.), Disenfranchised grief: New directions, challenges, and strategies for practice (pp. 95–117). Champaign, IL: Research Press.
Ness, D. E., & Pfeffer, C. R. (1990). Sequelae of bereavement resulting from suicide. American Journal of Psychiatry, 147, 279–285.
Parrish, M., & Tunkle, J. (2005). Clinical challenges following an adolescent’s death by suicide: Bereavement issues faced by family, friends, schools, and clinicians. Clinical Social Work Journal, 33, 81–102. doi:10.1007/s10615-005-2621-5
Peacock, E. J., & Wong, P. T. P. (1990). The stress appraisal measure (SAM): A multidimensional approach to cognitive appraisal. Stress Medicine, 6, 227–236. doi:10.1002/smi.2460060308
President’s New Freedom Commission on Mental Health. (2003). New freedom commission on mental health report. Retrieved from http://govinfo.library.unt.edu/mentalhealthcommission/reports/FinalReport/downloads/FinalReport.pdf
Provini, C., Everett, J. R., & Pfeffer, C. R. (2000). Adults mourning suicide: Self-Reported concerns about bereavement, needs for assistance, and help-seeking behavior. Death Studies, 24, 1–19. doi:10.1080/074811800200667
Sarantakos, S. (1993). Social research. Basingstoke, England: Macmillan.
Scocco, P., Castriotta, C., Toffol, E., & Preti, A. (2012). Stigma of Suicide Attempt (STOSA) scale and Stigma of Suicide and Suicide Survivor (STOSASS) scale: Two new assessment tools. Psychiatry Research, 200, 872–878. doi:10.1016/j.psychres.2012.06.033
Siebrecht, C. (2011). Imagining the absent dead: Rituals of bereavement and the place of the war dead in German women’s art during the First World War. German History, 29, 202–223.
Steel, J. L., Dunlavy, A. C., Stillman, J., & Pape, H. C. (2011). Measuring depression and PTSD after trauma: Common scales and checklists. Injury, 42, 288–300. doi:10.1016/j.injury.2010.11.045
Sudak, D. (2009). Training in cognitive behavioral therapy in psychiatry residency: An overview for educators. Behavior Modification, 33, 124–137. doi:10.1177/1059601108322626
Sveen, C.-A., & Walby, F. A. (2008). Suicide survivors’ mental health and grief reactions: A systematic review of controlled studies. Suicide and Life-Threatening Behavior, 38, 13–29. doi:10.1521/suli.2008.38.1.13
Uchino, B. N. (2006). Social support and health: A review of physiological processes potentially underlying links to disease outcomes. Journal of Behavior Medicine, 29, 377–387. doi:10.1007/s10865-006-9056-5
Worden, J. W. (1991). Grief counseling & grief therapy: A handbook for the mental health practitioner (2nd ed.). New York, NY: Springer.
Worden, J. W. (2009). Grief counseling and grief therapy: A handbook for the mental health practitioner (4th ed.) New York, NY: Springer.
Zamorski, M. A. (2011). Suicide prevention in military organizations. International Review of Psychiatry, 23, 173–180. doi:10.3109/09540261.2011.562186
Zhang, J., & Jia, C.-X. (2009). Attitudes toward suicide: The effect of suicide death in the family. Omega, 60, 365–382. doi:10.2190/OM.60.4.d307.
Zimet, G. D., Dahlem, N. W., Zimet, S. G., Farley, G. K. (1988). The multidimensional scale of perceived social support. Journal of Personality Assessment, 52, 30–41. doi:10.1207/s15327752jpa5201_2
Lindsey Mitchell, NCC, is the recipient of the 2015 Outstanding Dissertation Award for The Professional Counselor and a licensed counselor in both Texas and Washington, D.C. Correspondence may be addressed to Lindsey Mitchell at lmitch26@gwmail.gwu.edu.

