Anthony Hartman, Hope Schuermann, Jovanna Kenney
Despite efforts to boost mental health treatment-seeking behaviors by combat veterans, rates have improved relatively little since 2004. Previous work suggests that trust and confidence in the mental health community may be a significant factor. This study explored how professional titles may impact trust and confidence among active-duty U.S. Army soldiers (n = 32). Consistent with previous research, eight vignettes were used to solicit ordinal (ranked) trust and confidence scores for mental health professionals. Highest confidence and trust were seen in clinical psychologists and licensed professional counselors, followed by psychiatrists, licensed clinical social workers, and marriage and family therapists; however, deviations were seen for each individual vignette and the manifested symptoms depicted. Scores for trust and confidence were strongly correlated and both appear to impact soldiers’ treatment-seeking decisions.
Keywords: soldiers, mental health professionals, licensed professional counselors, trust, confidence
The U.S. Army Medical Command’s Department of Behavioral Health provides the following vision: “Our efforts in education, prevention, and early treatment are unprecedented. Our goal is to ensure that every deployed and returning soldier receives the health care they need” (U.S. Army Medical Department, 2016). In 2004, a landmark study by Hoge and colleagues found that only 13–27% of soldiers meeting screening criteria for mental health disorders sought treatment from a mental health professional in the previous year. The researchers concluded that the primary reason for such underutilization was perhaps “concern about how a soldier will be perceived by peers and by the leadership” (Hoge et al., 2004, p. 20). Subsequently, the Army has taken significant actions to reduce negative perceptions toward mental health care and increase confidentiality for those seeking treatment.
Despite substantial efforts to reduce negative stigmas, the number of soldiers seeking mental health care seems to remain significantly low. In a population of soldiers with probable post-traumatic stress disorder (PTSD) or major depression, Schell and Marshall (2008) found that “only 30 percent had received any type of minimally adequate treatment” (p. 101). Specifically, only 18% received minimally adequate talk therapy treatment. Of a sample population of National Guard and Reserve service members reporting psychological problems, Britt et al. (2011) found that only 42% had sought treatment. Most recently, Britt, Jennings, Cheung, Pury, and Zinzow (2015) found that only 40% of soldiers who acknowledged having a mental health issue sought treatment in the last year. Although the percentages of soldiers seeking treatment seem to be improving, the current literature continues to show less than half of those in need seek even a first visit with a mental health care provider. Thus, other significant deterrents to seeking treatment remain beyond the perceptions of leadership and peers.
Research studies indicate that one possible reason for this underutilization of mental health care services could be soldiers’ lack of trust or confidence in the quality of their providers or treatments. When surveyed, one in four soldiers recently returning from deployment indicated a lack of trust in mental health care practitioners (Kim, Britt, Klocko, Riviere, & Adler, 2011). Similarly, in a different sample of soldiers and Marines screening positively for mental health disorders, 38% indicated a lack of trust in mental health providers, while one in four of the same sample indicated a belief that mental health treatments were not effective (Hoge et al., 2004). Further hinting at a lack of trust for mental health care professionals and confidence in treatment, many soldiers would prefer to address their mental health issues with family, friends, or clergy (Schell & Marshall, 2008). Recently, the statement “Marines don’t trust mental health professionals” was rated as one of the top perceptions that mark barriers to care by a sample of enlisted Marine Corps leaders (VanSickle et al., 2016, p. 1022). Ultimately, there seems to be a trend of distrust and a lack of confidence in mental health care treatments and professionals among military populations.
Mental Health Practitioners and Military Treatment
Considering that there are numerous types of mental health professionals (e.g., psychiatrists, mental health counselors), it is possible that soldiers’ perceptions and knowledge of mental health professionals may vary depending on the specific type of provider. This study aims to distinguish soldiers’ perceptions between distinct mental health professionals: psychiatrists, clinical psychologists, licensed clinical social workers (LCSWs), licensed marriage and family therapists (LMFTs), and licensed professional counselors (LPCs). Psychiatrists are distinct in that they must have earned a doctorate in medicine (i.e., MD or DO) and have the nearly exclusive privilege of prescribing pharmaceutical medications for the treatment of mental disorders. Clinical psychologists also must be educated at the doctoral level (i.e., PhD or PsyD) and maintain a licensure in order to practice, but they cannot prescribe medications in most states. LCSWs, LMFTs, and LPCs are educated at least at the master’s level by an institution accredited for their respective field, and must complete respective licensing requirements that include supervised clinical experience following degree completion.
While the educational experience and licensing protocol can easily be distinguished, the mental health professions also have evolved somewhat distinct professional identities in terms of their approaches to mental health treatment. While psychiatrists are trained in various psychotherapeutic modalities, trends indicate the majority of current and future psychiatrists plan to rely more heavily on pharmacological treatments than on talk therapies (Clemens, Plakun, Lazar, & Mellman, 2014; Zisook et al., 2011). As for clinical psychologists, a review of 50 years of literature surrounding this occupation revealed trends around specializing in one particular aspect of the field (i.e., psychotherapy, assessment, research) and one or two treatment modalities (e.g., psychodynamic therapy, cognitive-behavioral therapy), and a prevalence of cognitive therapies (Norcross & Karpiak, 2012). Generally speaking, LCSWs are likely to conduct therapy from a holistic approach that heavily considers the social impacts on a person while pursing social justice and equality agendas, such as helping underprivileged groups (Bradley, Maschi, O’Brien, Morgen, & Ward, 2012). While LMFTs are often exposed to or trained in a wide variety of therapeutic paradigms and techniques, they are likely to emphasize a collective rather than individual treatment approach, often marked by working with families and couples to identify and improve systemic or transactional issues between the members (Imber-Black, 2014). As LPCs’ professional identity continues to develop and stabilize (Mellin, Hunt, & Nichols, 2011; Reiner, Dobmeier, & Hernández, 2013), professional counselors train in a variety of treatment modalities and provide a variety of services in the mental health field, including “the diagnosis and treatment of mental and emotional disorders, including addictive disorders; psychoeducational techniques aimed at the prevention of such disorders; consultation to individuals, couples, families, groups, and organizations; and research into more effective therapeutic treatment modalities” (American Counseling Association, 2011, para. 4).
Although the average client may not know or fully understand the distinctions between mental health professionals, the literature suggests clients do exhibit some bias when selecting mental health professionals. Over the past 30 years, researchers have shown a consistent trend of professional titles or education levels impacting perceptions of mental health professionals. Warner and Bradley (1991) and Wollersheim and Walsh (1993) established that both perceptions of and confidence in mental health therapies were impacted by the title and education level of the mental health professional; generally, participants in these studies indicated a lack of confidence and knowledge about clinical psychologists and a preference for treatment from counselors. In a study examining public confidence in mental health professionals, Fall, Levitov, Jennings, and Eberts (2000) found significant differences in confidence based upon their title as well as their education level (i.e., master’s vs. doctoral level); participants mostly favored doctoral-level education and preferred counselors, except when presented with “serious psychiatric disorders” (p. 122). This study was repeated in 2005 with an African American sample that provided similar findings (Fall, Levitov, Anderson, & Clay, 2005). While specific attitudes and perceptions may have changed or evolved over the past three decades, these studies show that distinct perceptions or even biases toward professional titles do exist among civilian populations. This led the researchers to question if similar trends exist in military populations, which may be influencing the treatment-seeking decisions of service members.
To summarize, soldiers’ confidence in treatment for and trust in mental health professionals might be significantly impacting treatment-seeking decisions. In multiple studies, service members have repeatedly indicated relatively low levels of trust and confidence in mental health providers and treatments. Also, researchers have consistently shown that a professional title can impact patient or public perceptions with respect to general confidence in the professional’s abilities. To date, no known research is published on military members’ perceptions and levels of confidence or trust with differing mental health professionals. Thus, the purpose of this study was to explore soldiers’ relative levels of trust for and confidence in mental health professionals based solely upon their title and a presenting issue, in an effort to better understand what may be influencing treatment-seeking decisions among U.S. Army soldiers.
Method
The researchers for this study received approval from the Institutional Review Board of their university, and the survey was approved for distribution to active-duty soldiers by Army public affairs representatives. Sample size was determined by following similar confidence in mental health professional studies that used Friedman non-parametric tests (e.g., Fall et al., 2000; Fall et al., 2005). Participants were surveyed via the online metrics program Qualtrics, ensuring anonymity.
Participants
Active-duty soldiers serving in the U.S. Army were recruited using snowball sampling initiated by public affairs representatives at various Army installations. Each potential participant received a generalized email invitation that included an information sheet about the research and a link to complete an online survey. Participants were encouraged to forward the invitation to others who also met the inclusion criteria, which limited participation to those currently serving on active duty in the U.S. Army with more than 2 years of active-duty service or the National Guard/Army Reserve equivalent. Upon completion of the survey, participants were offered the opportunity to enroll in a raffle drawing to win one of two prizes: a $100 or a $50 gift card.
The sample included 32 active-duty soldiers, 26 males and six females, between the ages of 25 and 50 years (M = 33.3, SD = 7.0). Ethnic identities included 25 non-Hispanic Whites, two Hispanic or Latinos, one African American, one Filipino, one Native American, one White/Korean, and one White/Hispanic. Most of the participants (26) were married, while three were divorced and three had never married. Nearly two-thirds of the sample indicated current responsibility for children in their homes; there was an average of 1.85 children (SD = 1.5) reported by these 20 participants. Thirteen of the soldiers had seen at least one mental health professional (MHP) prior to completing the survey; respondents had seen all five MHPs included in this study. Participants were allowed to list multiple MHPs if applicable, and the MHPs were identified as follows: clinical psychologist, seven times; psychiatrist, five times; LPC, four times; LCSW, three times; LMFT, three times; and “other” or “unsure,”five times.
Regarding military experience, the sample included 18 officers, 11 non-commissioned officers, and three junior-enlisted (i.e., rank of E1–E4) soldiers. Twenty participants had a military occupational specialty (MOS) considered as Combat Arms in the U.S. Army. In the military, not all service members are equally likely to fight in combat; certain MOSs are combat-related while others are supportive in nature (e.g., administrative personnel, mechanics, logisticians). Of our 32 qualifying participants, we had a good mix of combat and non-combat MOSs. To the reader, this may seem to be either irrelevant or not particularly noteworthy information; however, this data can be quite important when forming conclusions about the study. On average, military service was 11.4 years (SD = 7.2), with 17 months (SD = 11.5) deployed to either Iraq or Afghanistan; only two participants had not been deployed to these countries. Seventy-five percent of the sample reported direct exposure to combat, and 59% reported having never seen an MHP for even one visit throughout their life.
Materials
Demographic questionnaire. In order to provide some description of the sample population, a demographics survey of 15 questions regarding age, sex, ethnicity, marital background, parental status, military rank, deployment and combat experience, and previous experience with mental health care providers was collected from participants. Most questions were multiple-choice but offered the options to not respond or provide a unique response if desired. The remaining questions were free-response.
Vignettes. Brief vignettes were used to depict the selected mental health diagnoses or mental health issues of eight fictional soldiers recently returning from a combat deployment. The vignettes were limited in length to approximately half of a standard printed page and were written with the goal of depicting diagnostic criteria in a manner that one might see them manifested by the soldier in the vignette. Authors specifically avoided using the exact clinical terms that an MHP may use while ensuring that enough diagnostic criteria were included to suggest the intended diagnoses may be warranted.
Each vignette was followed immediately by two questions. These questions asked the participant to rank the five MHPs in order according to the participant’s preference for (1) confidence in the MHPs in providing treatment for the soldier in the vignette, and (2) their own personal trust for the professionals if they were experiencing the symptoms described in the vignette. Because both questions were worded similarly, keywords such as trust and confident were bolded or underlined in order to highlight the intent of the question.
Development and validation of the vignettes.
The vignettes and questions were originally drafted by the lead researcher to explore how soldiers may rank MHPs under the two stated conditions (i.e., confidence and trust questions). The four mental health diagnoses selected were PTSD, anxiety disorders, depression, and substance use disorders, as these were identified by Seal, Bertenthal, Miner, Sen, and Marmar (2007) to be the most prevalent for soldiers returning from Iraq. The four common issues were suicide, marital problems, parenting difficulties, and sleep problems; these were selected from the Military Health System’s “After Deployment” (2015) website because they were depicted as common problems faced by soldiers and contributed to the breadth of issues explored in the study. Vignettes were modeled after previous studies using similar metrics to measure populations’ trust of MHPs (e.g., Fall et al., 2000; Fall et al., 2005).
After review and editing within the research team, faculty with extensive clinical and teaching expertise in the area of diagnosis reviewed the vignettes. Based on their recommendations, specific diagnostic labels, such as PTSD and depression, were removed in order to reduce the impact of these labels on participants’ responses, and the keywords trust and confidence were included and bolded in the survey questions. Their input also resulted in the refining of the vignettes to more accurately depict the intended issues based upon their clinical experience and expertise.
Procedures
From January to June of 2017, surveys were administered via Qualtrics software on an electronic device of the participant’s choosing. Respondents were requested to complete the surveys at a location and time presenting minimal distractions. After being provided information about the study and consenting to continue, participants were presented with the demographics survey followed by the vignettes. The survey would not advance to the next page unless a response was recorded to all questions on the previous page. Upon completion of the demographics portion, participants advanced to the vignettes depicting soldiers facing issues upon returning from a combat deployment.
During the vignette portion of the survey, respondents ranked the list of mental health practitioners for both the confidence and trust conditions; see the Appendix for the vignettes presented to participants. The survey would not allow duplicate ranks (i.e., MHPs could not “tie”) for either condition. The vignettes were randomized, with both the trust and confidence questions presented together on the same screen, and the listed order of the MHPs was randomized for each vignette as well.
Analysis
Data analysis focused on three main themes: the mean ranks for trust of the MHPs across the vignettes, the mean ranks for confidence in the MHPs across the vignettes, and potential correlation between trust and confidence. Consistent with the Fall et al. (2005) analysis, Friedman non-parametric tests and Wilcoxon matched-pairs tests were used to determine significant findings in the mean ranks for MHPs in each vignette with respect to both the confidence and trust conditions separately. These tests were completed 16 times—once for each of the eight vignettes for both the trust and confidence questions. Afterward, the data was aggregated separately for both the trust and confidence questions to allow an overall assessment of the mean ranks for each MHP without concern for the particular vignette presented. Both the Friedman and Wilcoxon tests were completed again on the aggregated data. Finally, a Goodman and Kruskall’s gamma test was used to determine the correlation between trust and confidence ranking for each MHP.
Results
For all eight vignettes, significant differences (n = 32, df = 4, p <= .002) were found for mean rankings in both confidence and trust conditions. Subsequently, Wilcoxon matched-pairs tests identified statistically significant differences within groups for each of the 16 conditions; see Table 1 for specific results. Figures 1 and 2 display inverted mean rankings for each MHP by vignette for the confidence and trust questions respectively; higher scores indicate a more favorable ranking.
In both the confidence and trust conditions, the data from each vignette allowed for the separation of the five MHPs into either two or three distinct groups in terms of their rankings. In some instances, some MHPs could be grouped with both the higher- and lower-ranking adjacent MHP; in this case, the MHP was placed in both groups. For example, in Table 1 under the Aggregate Rank column for the confidence condition, there was no significant difference between LPCs and psychiatrists (N = 256, p = .202), or LPCs and psychologists (N = 256, p = .336), but there was a significant difference between psychologists and psychiatrists (N = 256, p = .011).
Lastly, scores from all eight vignettes were aggregated for each MHP to allow an overall measure of the MHP’s ranking for both confidence and trust. Table 1 includes the associated statistically significant grouping, and Figure 3 depicts the aggregated inverted mean ranking for both conditions for each MHP. Using a Goodman and Kruskall’s gamma test on the aggregated data, a strong positive correlation was found between confidence and trust ratings for all five MHPs with G values ranging from 0.72 to 0.88 (N = 256, p < .0005).
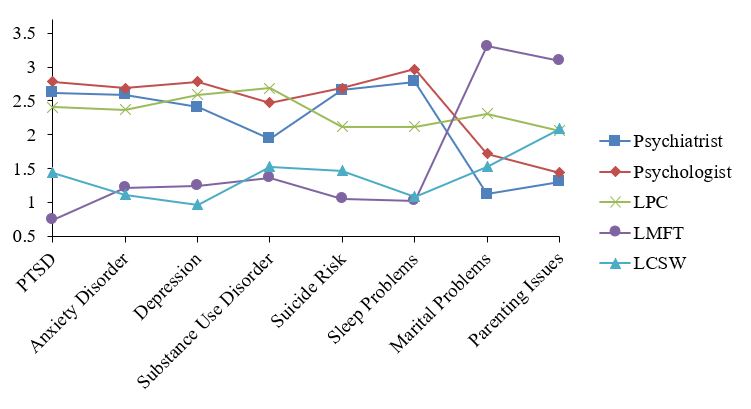
Figure 1. Inverted Mean Ranks for Confidence Question Plotted by Type of Mental Health Professional and Vignette. Higher mean rank equates to higher confidence.
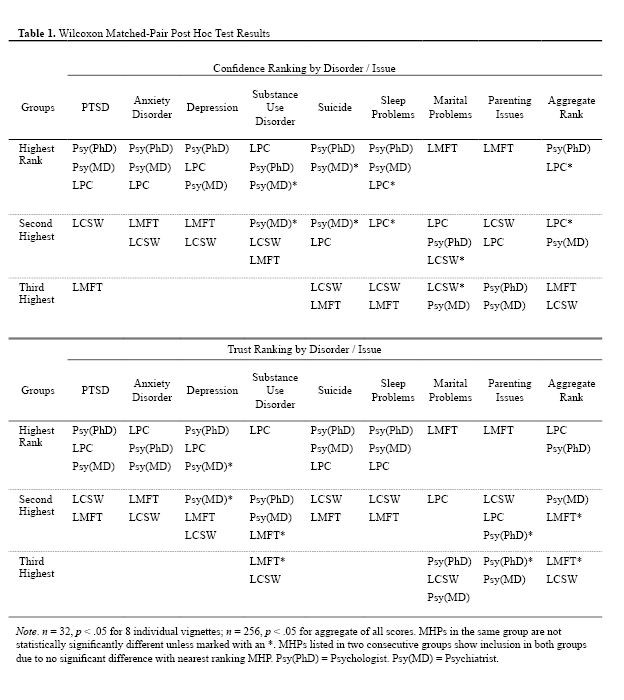
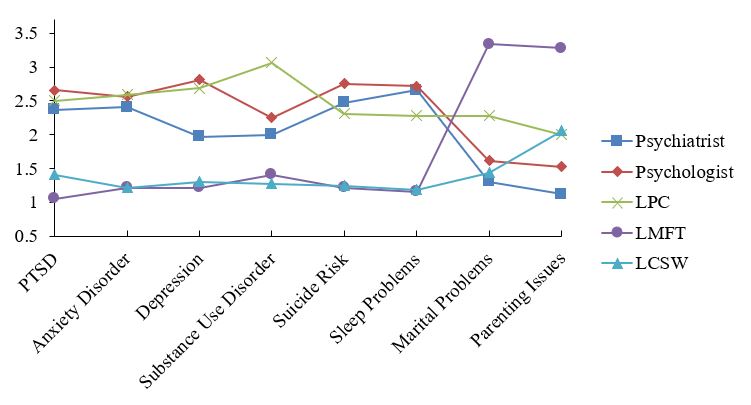
Figure 2. Inverted Mean Ranks for Trust Question Plotted by Type of Mental Health Professional and Vignette. Higher mean rank equates to higher trust.
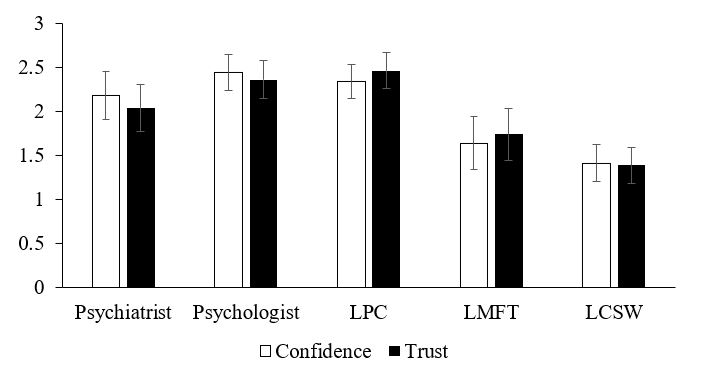
Figure 3. Aggregated Inverted Mean Ranks for Mental Health Professionals for Confidence and Trust Questions. Higher mean rank equates to higher confidence or trust. Error bars indicate standard error based on standard deviation from the mean; they do not indicate statistical significance.
Discussion
This study was designed to explore active-duty Army soldiers’ perceptions toward various mental health care providers with respect to trust and confidence in the MHP. Overall, the sample population of soldiers appears to have the highest confidence and trust in clinical psychologists and LPCs, while LCSWs and LMFTs are significantly less preferred (as seen in Table 1). Psychiatrists seem to be somewhere between each of these two groups, as they appear in both the highest and second-highest preferred groups depending on the condition (i.e., confidence or trust). The statistically significant stratification into these groups suggests that the title of available MHPs may influence a soldier’s decision to seek services. Undoubtedly, other factors are involved, but the title, and perhaps the certifications of the available professional, is likely impacting treatment-seeking behaviors in military communities.
At the heart of this study is the notion that each of the MHPs included could treat any of the soldiers in the vignettes; however, the results suggest that soldiers would seek out different professionals based on the context of the presenting symptoms rather than the type or potential efficacy of the treatment to be received. For example, the marital problems vignette (see Appendix) could arguably have been treated more effectively by a psychiatrist than an LMFT; perhaps the declining relationship was itself a symptom of biochemical issues such as vitamin or neurotransmitter deficiencies, which may be more aptly treated with medicine. Or, it also is possible that an experienced LPC or LCSW could have effectively brought to the surface some other underlying issue in the course of individual therapy rather than the marriage, couple, and family-oriented approach taken by an LMFT. Similar arguments could be made for each of the other vignettes, but the results suggest that soldiers are likely making treatment decisions based upon professional title and presumably the associated reputation. If the Army’s goal is to boost rates of treatment-seeking behaviors, professional titles and perceptions of trust and confidence should not be ignored.
Results also show a strong correlation between trust and confidence across all of the vignettes. This can best be seen by comparing the LMFTs’ rankings for the marital problems and parenting issues vignettes with their consistently lower scores on the other vignettes. The jump in scores was consistent across both conditions, demonstrating that trust and confidence for MHPs are strongly linked. Although less likely, it also is possible that the respondents might have been biased or influenced to provide similar ranks for each professional across both conditions because the survey design allowed them to see their scores for the confidence question while completing the trust question. Regardless of whether trust influences confidence or vice versa, the two should be considered in the quest to boost treatment-seeking rates among soldiers.
Implications for Service Provision
With further validating and corroborating research, the Army may be able to improve treatment-seeking rates among those in need of mental health care by adjusting services based on the perceptions of soldiers. Although LPCs were consistently favored more than LCSWs, the Army currently allows LCSWs to serve as commissioned officers in behavioral health clinics providing individual therapy to soldiers, while the LPC license does not qualify an MHP to commission and serve as an officer (U.S. Department of the Army, 2007). This means soldiers have fewer chances of seeing an LPC without some type of insurance referral because the uniformed personnel initially available will not be LPCs. This study provides evidence that LPCs may be more appropriate and effective in this role by boosting treatment-seeking rates, so it could be beneficial to make treatment with LPCs more accessible to soldiers. Likewise, incorporating the services of LMFTs following deployments could help military families, as they had the highest average trust and confidence ratings of any professional in any vignette in the study when they were the preferred MHP. Perhaps they could advocate for temporary positions following deployments or increased advertisement of their services in military communities with units returning from overseas.
Limitations and Future Research
Future research is certainly needed to further confirm the results of this study. Investigators could explore what drives trust and confidence perceptions in military communities and how prior personal experiences influence the soldiers’ views of MHPs. Studies like this one could be conducted with other branches of the military and include National Guard and Reserve forces. Exploratory qualitative research could seek to identify specific factors that build trust and confidence in the mental health community as a whole. Future studies also should continue to update the disorders or issues selected to accurately represent the issues faced by targeted populations at the time.
Limitations to this study include the sample size, delivery of the survey, and lack of consideration for gender biases. While 32 respondents can provide initial insights, a much larger sample should be surveyed before any significant policy decisions are considered. The research team also recommends administering the surveys in person rather than online with the belief that many soldiers—and people in general—may not complete the digital surveys as earnestly as a paper version following a personal interaction with the research team or a recruiter. With regards to gender, it was not considered how the names of the soldiers in the vignettes may influence the respondents’ rankings; it is possible that the scores could have varied if the soldier in the vignette was of a specific gender.
Future researchers should be cautious to ensure that voluntary participation is not influenced by environmental pressures. In military communities, the researchers recommend seeking a sample population that includes personnel from multiple units, locations, and MOSs, as culture and attitudes can be vastly different among these variables.
Although this study has limitations, the researchers believe it highlights one of the key reasons that soldiers may not seek mental health services when in need: lack of trust and confidence in the resources available. Although the military has significantly addressed other identified issues, such as the associated stigma or impact to a service member’s career, treatment-seeking rates for those in need have changed very little, which indicates other issues are contributing to the decision not to visit with an MHP. The researchers hope the results of this study are built upon and examined for alternative approaches to boost treatment-seeking rates among the military.
Conflict of Interest and Funding Disclosure
The authors reported no conflict of interest
or funding contributions for the development
of this manuscript.
References
After Deployment. (2015). After deployment: Wellness resources for the military community. Retrieved from
http://afterdeployment.dcoe.mil
American Counseling Association. (2011). Who are licensed professional counselors. Retrieved from
https://www.counseling.org/PublicPolicy/WhoAreLPCs.pdf
Bradley, C., Maschi, T., O’Brien, H., Morgen, K., & Ward, K. (2012). Faithful but different: Clinical social workers speak out about career motivation and professional values. Journal of Social Work Education, 48, 459–477. doi:10.5175/JSWE.2012.201000043
Britt, T. W., Bennett, E. A., Crabtree, M., Haugh, C., Oliver, K., McFadden, A., & Pury, C. L. S. (2011). The theory of planned behavior and reserve component veteran treatment seeking. Military Psychology, 23, 82–96. doi:10.1080/08995605.2011.534417
Britt, T. W., Jennings, K. S., Cheung, J. H., Pury, C. L. S., & Zinzow, H. M. (2015). The role of different stigma perceptions in treatment seeking and dropout among active duty military personnel. Psychiatric Rehabilitation Journal, 38, 142–149. doi:10.1037/prj0000120
Clemens, N. A., Plakun, E. M., Lazar, S. G., & Mellman, L. (2014). Obstacles to early career psychiatrists practicing psychotherapy. Psychodynamic Psychiatry, 42, 479–495. doi:10.1521/pdps.2014.42.3.479
Fall, K. A., Levitov, J. E., Anderson, L., & Clay, H. (2005). African Americans’ perception of mental health professions. International Journal for the Advancement of Counselling, 27, 47–56.
doi:10.1007/s10447-005-2246-y
Fall, K. A., Levitov, J. E., Jennings, M., & Eberts, S. (2000). The public perception of mental health professions: An empirical examination. Journal of Mental Health Counseling, 22, 122–134.
Hoge, C. W., Castro, C. A., Messer, S. C., McGurk, D., Cotting, D. I., & Koffman, R. L. (2004). Combat duty in Iraq and Afghanistan, mental health problems, and barriers to care. New England Journal of Medicine, 351, 13–22. doi:10.1056/NEJMoa040603
Imber-Black, E. (2014). Eschewing certainties: The creation of family therapists in the 21st century. Family Process, 53, 371–379. doi:10.1111/famp.12091
Kim, P. Y., Britt, T. W., Klocko, R. P., Riviere, L. A., & Adler, A. B. (2011). Stigma, negative attitudes about treatment, and utilization of mental health care among soldiers. Military Psychology, 23, 65–81.
doi:10.1080/08995605.2011.534415
Mellin, E. A., Hunt, B., & Nichols, L. M. (2011). Counselor professional identity: Findings and implications for counseling and interprofessional collaboration. Journal of Counseling & Development, 89, 140–147. doi:10.1002/j.1556-6678.2011.tb00071.x
Norcross, J. C., & Karpiak, C. P. (2012). Clinical psychologists in the 2010s: 50 Years of the APA Division of Clinical Psychology. Clinical Psychology: Science and Practice, 19, 1–12.
doi:10.1111/j.1468-2850.2012.01269.x
Reiner, S. M., Dobmeier, R. A., & Hernández, T. J. (2013). Perceived impact of professional counselor identity: An exploratory study. Journal of Counseling & Development, 91, 174–183.
doi:10.1002/j.1556-6676.2013.00084.x
Schell, T. L., & Marshall, G. N. (2008). Survey of individuals previously deployed for OEF/OIF. In T. Tanielian & L. H. Jaycox (Eds.), Invisible wounds of war: Psychological and cognitive injuries, their consequences, and services to assist recovery (pp. 87–115). Santa Monica, CA: RAND Health Center for Military Health Policy Research.
Seal, K. H., Bertenthal, D., Miner, C. R., Sen, S., & Marmar, C. (2007). Bringing the war back home: Mental health disorders among 103,788 US veterans returning from Iraq and Afghanistan seen at Department of Veterans Affairs facilities. Archives of Internal Medicine, 167, 476–482.
U.S. Army Medical Department. (2016). Behavioral health. Retrieved from https://armymedicine.health.mil/Behavioral-Health
U.S. Department of the Army. (2007). Army Medical Department Officer Development and Career Management: Department of the Army Pamphlet 600-4. Retrieved from http://www.apd.army.mil/epubs/DR_pubs/DR_a/pdf/web/p600_4.pdf
VanSickle, M., Werbel, A., Perera, K., Pak, K., DeYoung, K., & Ghahramanlou-Holloway, M. (2016). Perceived barriers to seeking mental health care among United States Marine Corps noncommissioned officers serving as gatekeepers for suicide prevention. Psychological Assessment, 28, 1020–1025.
doi:10.1037/pas0000212
Warner, D. L., & Bradley, J. R. (1991). Undergraduate psychology students’ views of counselors, psychiatrists, and psychologists: A challenge to academic psychologists. Professional Psychology: Research and Practice, 22, 138–140.
Wollersheim, D. M., & Walsh, J. A. (1993). Clinical psychologists: Professionals without a role? Professional Psychology: Research and Practice, 24, 171–175.
Zisook, S., McQuaid, J. R., Sciolla, A., Lanouette, N., Calabrese, C., & Dunn, L. B. (2011). Psychiatric residents’ interest in psychotherapy and training stage: A multi-site survey. American Journal of Psychotherapy, 65, 47–59.
Appendix
Vignettes Used to Depict Mental Health Diagnoses and Issues
Post-Traumatic Stress Disorder Vignette
Joe returned from deployment to Afghanistan 4 months ago. He was personally involved in combat with enemy insurgents on multiple occasions and was exposed to disfigured, dead bodies of both enemy combatants and fellow soldiers as well. He has often mentioned bad dreams about one of these times in particular and seems obviously distressed (e.g., fidgeting, faster breathing, and sometimes even sweating) whenever he speaks about it. However, when his fellow soldiers from the deployment bring up the event, he seems unwilling to participate in the conversation and has on a few occasions become angry about it. Based on these behaviors, you believe he may be struggling with traumatic experiences.
Anxiety Disorder Vignette
John returned from a combat deployment 9 months ago. Since returning, his family and coworkers have noticed changes in his behavior. He is often restless (or “on edge”), irritable, or physically tense in common, everyday situations. Plus, he has claimed poor or unsatisfying sleep for several months. These symptoms seem to be impairing his work performance and damaging personal relationships with loved ones. When asked, he hasn’t mentioned any particular traumatic events or worries that are bothering him. He simply seems much more anxious and it is affecting his well-being.
Depression Vignette
Jane returned from a combat deployment 3 months ago and has generally seemed a little bit down since coming home. Nearly every day over the past 2 weeks she has seemed to be sad or gloomy throughout the day and has shown very little interest in doing things she used to enjoy. She is clearly tired throughout the day and has mentioned feeling worthless to those around her. It seems like she is suffering greatly based on her unhappy and sad moods.
Substance Abuse Disorder Vignette
Jim returned from a combat deployment 12 months ago. Upon returning, he seemed to seamlessly reintegrate with his family, friends, and former social life. However, he soon began drinking alcohol more heavily than ever before, often binge drinking until passing out on weekdays and weekends. Although never caught in the act, he has even gone to work intoxicated and driven while drunk on multiple occasions. On two distinct occasions, he attempted to reduce his alcohol consumption but failed after only a week or two. Alcohol abuse is beginning to disrupt his work performance, family life, and physical well-being.
Sleep Problems Vignette
Joan returned from a combat deployment 4 months ago. She seems to have reintegrated very successfully into her family, social, and work environments. However, her sleep patterns have become very irregular and unsatisfactory. She rarely gets more than 4 hours of sleep consecutively and often uses her weekends to recover from a week of sleepless nights. Although her family and coworkers haven’t noticed anything wrong, Joan fears her sleep problems will soon begin disrupting her life.
Suicide Risk Vignette
James returned from a combat deployment 6 months ago. Since returning, he has outwardly seemed to have successfully reintegrated into his family, work, and social life. Although he appears to have been changed by his combat experiences, he does not seem to be generally troubled in any way (e.g., depressed, anxious, abusing drugs). However, he has jokingly mentioned “blowing his brains out” to colleagues at work and mentioned a specific plan to take his own life with his pistol. During a conversation with two friends, he has mentioned “ending it all” because he is feeling hopeless. You think James may be at risk for suicide.
Marital Problems Vignette
Jon returned from a combat deployment 5 months ago. He has rejoined his wife of 6 years, but their relationship has changed. While they used to feel very close and connected, they now both feel very distant. They do not enjoy activities together which they used to, such as hiking and dancing. They rarely hold good conversations with each other and are also less physically intimate. Jon and his wife both want their marriage to work but fear that they are nearing divorce. They are facing the most significant period of marital problems they have ever experienced.
Parenting Issues Vignette
Jerry returned from a combat deployment 10 months ago. He rejoined his wife of 16 years, their 13-year-old daughter, and their 5-year-old son. Since returning, Jerry has experienced some difficulty reassuming his role as a parent. His daughter seems to want very little to do with him. Although he thinks this is typical of a 13-year-old, it still causes him distress and he complains that he doesn’t feel like he has any influence in her life. With their son, Jerry often disagrees with his wife on discipline issues, and he can’t seem to find ways to connect with the 5-year-old. His son seems to have little interest in playing anything besides video games and always runs to his mother when Jerry attempts to discipline him. These parenting issues are significantly affecting Jerry’s mental and emotional well-being.
Anthony Hartman is a medical student at UT-Health San Antonio. Hope Schuermann is a clinical assistant professor at the University of Florida. Jovanna Kenney is a therapist at Genesis Psychiatric Center in San Antonio, TX. Correspondence can be addressed to Anthony Hartman, 7703 Floyd Curl Drive, San Antonio, TX 78229, hartmanaj@livemail.uthscsa.edu.
