Nov 9, 2022 | Volume 12 - Issue 3
Michael T. Kalkbrenner, Gabriella Miceli
Meeting the mental health needs of students enrolled in science, technology, engineering, and mathematics (STEM) majors is particularly challenging for professional counselors who work in college settings, as STEM students are a subgroup of college students that face unique risks for developing mental health issues. The scarcity of literature on STEM student mental health coupled with their reticence to seek counseling is concerning. An important next step in this line of research is understanding why STEM students are reticent to seek counseling. Accordingly, the present investigators validated STEM students’ scores on the Revised Fit, Stigma, and Value (RFSV) Scale, a screening tool for measuring barriers to seeking counseling. Results also established the capacity of STEM students’ RFSV scores to predict peer-to-peer referrals to the counseling center and revealed demographic differences in barriers to counseling. Findings have implications for enhancing professional counselors’ efforts to support STEM students’ mental health.
Keywords: Revised Fit, Stigma, and Value Scale; STEM; student mental health; barriers to counseling; peer-to-peer referrals
The frequency and complexity of college students presenting with mental health issues is a notable concern for professional counselors who work in university settings (Al-Maraira & Shennaq, 2021; Hong et al., 2022). Students enrolled in science, technology, engineering, and mathematics (STEM) majors are a distinctive group of college students who face unique risks for developing mental health issues (Daker et al., 2021; Kalkbrenner, James, & Pérez-Rojas, 2022; Lipson et al., 2016; Shapiro & Sax, 2011). When compared to their non-STEM counterparts, STEM students are less likely to recognize warning signs of mental distress, and they access mental health support services at lower rates than their peers. In addition, the harsh and competitive academic environment in STEM majors can exacerbate students’ risk for mental health distress (Lipson et al., 2016; Shapiro & Sax, 2011). Moreover, Rice et al. (2015) demonstrated that STEM students exhibit higher levels of maladaptive perfectionism, which is associated with higher levels of mental distress.
Whereas substantial academic and financial resources exist to support STEM students (U.S. Department of Education, 2020), there is a dearth of literature on supporting STEM students’ mental health, which is essential for retaining students and ensuring their success both in and out of the classroom (Kivlighan et al., 2021; Schwitzer et al., 2018). This gap in the literature is concerning, as STEM students are at risk for mental health issues, which can lead to attrition, isolation, and suicide (Daker et al., 2021; Kalkbrenner, James, & Pérez-Rojas, 2022; Lipson et al., 2016). As just one example, academic mental health distress is a significant predictor of lower enrollment and completion rates in STEM fields (Daker et al., 2021). Moreover, Muenks et al. (2020) found that higher levels of psychological vulnerability among STEM students was a significant predictor of lower class attendance, higher dropout intentions, and less class engagement.
The literature is lacking research on why STEM students tend to seek counseling at lower rates than non-STEM students. One of the first steps in supporting STEM students’ mental health is validating scores on a screening tool for identifying barriers to accessing mental health support services among STEM students. Although screening tools that appraise barriers to counseling exist, none of them have been validated with STEM students. The Revised Fit, Stigma, and Value (RFSV) Scale is a screening tool for appraising barriers to counseling that has been normed with non–college-based populations (e.g., adults in the United States; Kalkbrenner & Neukrug, 2018) and college students with mental health backgrounds (e.g., graduate counseling students; Kalkbrenner & Neukrug, 2019), as just a few examples. When compared to the existing normative RFSV Scale samples, STEM students are a distinct college student population who utilize counseling services at lower rates than students in mental health majors (e.g., psychology; Kalkbrenner, James, & Pérez-Rojas, 2022). The psychometric properties of instrumentation can fluctuate significantly between different populations, and researchers and practitioners have an ethical obligation to validate scores on instruments before interpreting the results with untested populations (Mvududu & Sink, 2013). Accordingly, the primary aims of the present study were to validate STEM students’ scores on the RFSV Scale (Kalkbrenner & Neukrug, 2019), test the capacity of RFSV scores for predicting referrals to the counseling center, and investigate demographic differences in STEM students’ RFSV scores.
The Revised Fit, Stigma, and Value (RFSV) Scale
Neukrug et al. (2017) developed and validated scores on the original version of the Fit, Stigma, and Value (FSV) Scale for appraising barriers to counseling among a large sample of human services professionals. The FSV Scale contains the three following subscales or latent traits behind why one would be reluctant to seek personal counseling: Fit, Stigma, and Value. Kalkbrenner et al. (2019) validated scores on a more concise version of the FSV Scale, which became known as the RFSV Scale, which includes the same three subscales as the original version. Building on this line of research, Kalkbrenner and Neukrug (2019) found a higher-order factor, the Global Barriers to Counseling scale. The Global Barriers to Counseling scale is composed of a total composite score across the three single-order subscales (Fit, Stigma, and Value). Accordingly, the Fit, Stigma, and Value subscales can be scored separately and/or users can compute a total score for the higher-order Global Barriers to Counseling scale.
Scores on the RFSV Scale have been validated with a number of non-college populations, including adults in the United States (Kalkbrenner & Neukrug, 2018), professional counselors (Kalkbrenner et al., 2019), counselors-in-training (Kalkbrenner & Neukrug, 2019), and high school students (Kalkbrenner, Goodman-Scott, & Neukrug, 2020). If scores are validated with STEM students, the RFSV Scale could be used to enhance professional counselors’ mental health screening efforts to understand and promote STEM student mental health. Specifically, campus-wide mental health screening has implications for promoting peer-to-peer mental health support. For example, college counselors are implementing peer-to-peer mental health support initiatives by training students to recognize warning signs of mental distress in their peers and, in some instances, refer them to college counseling services (Kalkbrenner, Sink, & Smith, 2020).
Peer-to-Peer Mental Health Support
College students tend to discuss mental health concerns with their peers more often than with a faculty member or student affairs professional (Wawrzynski et al., 2011; Woodhead et al., 2021). To this end, the popularity and utility of peer-to-peer mental health support initiatives has grown in recent years (Kalkbrenner, Lopez, & Gibbs, 2020; Olson et al., 2016). The effectiveness of these peer-to-peer support initiatives can be evaluated by test scores (e.g., scores on mental distress and well-being inventories) as well as non-test criteria (e.g., increases in the frequency of peer-to-peer mental health referrals). For example, Olson et al. (2016) found that college students who attended a Recognize & Refer workshop were significantly more likely to refer a peer to counseling when compared to students who did not attend the workshop. Similarly, Kalkbrenner, Lopez, and Gibbs (2020) found that increases in college students’ awareness of warning signs for mental distress were predictive of substantial increases in the odds of making peer-to-peer referrals to the counseling center.
Peer-to-peer mental health support also has implications for improving college student mental health (Bryan & Arkowitz, 2015; Byrom, 2018; Caporale-Berkowitz, 2022). For example, Bryan and Arkowitz (2015) found that peer-run support programs for depression were associated with significant reductions in depressive symptoms. In addition, Byrom (2018) demonstrated that peer support interventions were associated with increases in college students’ well-being. The synthesized results of the studies cited in this section suggest that peer-to-peer mental health support has utility for promoting mental health among general samples of undergraduate college students. However, to the best of our knowledge, the literature is lacking research on peer-to-peer mental health support with STEM majors, a subgroup of college students with unique mental health needs (Daker et al., 2021; Lipson et al., 2016; Shapiro & Sax, 2011).
The Present Study
College counseling services are a valuable resource for students, as attendance in counseling is associated with increases in GPA and retention rates (Kivlighan et al., 2021; Lockard et al., 2019; Schwitzer et al., 2018). Considering STEM students’ unique vulnerability to mental health distress (Daker et al., 2021; Lipson et al., 2016; Shapiro & Sax, 2011) and their reticence to seek counseling (Kalkbrenner, James, & Pérez-Rojas, 2022), professional counselors who work in university settings need screening tools with validated scores for identifying why STEM students might avoid accessing counseling services. The RFSV Scale has potential to fill this gap in the measurement literature, as a number of recent psychometric studies (e.g., Kalkbrenner, Goodman-Scott, & Neukrug, 2020; Kalkbrenner & Neukrug, 2018) demonstrated support for the psychometric properties of scores on the RFSV Scale with non-college populations. However, the literature is lacking a screening tool for appraising barriers to counseling with validated scores among STEM students. Accordingly, a score validation study with STEM students is an important next step in this line of research, as the internal structure of instrumentation can vary notably between different samples (Mvududu & Sink, 2013). The literature is also lacking research on the potential of peer-to-peer mental support (e.g., students recognizing and referring a peer to counseling) among STEM students. This is another notable gap in the literature, as college students are more likely to discuss mental health concerns with a peer than with faculty or other university personnel (Wawrzynski et al., 2011; Woodhead et al., 2021). If STEM students’ scores on the RFSV Scale are validated, we will proceed to test the capacity of scores for predicting peer-to-peer referrals to the counseling center as well as examine demographic differences in STEM students’ RFSV scores.
The findings of the present investigation have implications for campus-wide mental health screening, increasing peer-to-peer mental health support, and identifying subgroups of STEM students that might be particularly reticent to seek counseling. To this end, the following research questions (RQs) and hypotheses (Ha) guided the present investigation: RQ1: Is the internal structure of scores on the RFSV Scale confirmed with STEM students? Ha1: The dimensionality of the RFSV Scale will be confirmed with STEM students. RQ2: Are STEM students’ RFSV scores significant predictors of making at least one referral to the counseling center? Ha2: Higher RFSV scores will emerge as a statistically significant positive predictor of STEM students making one or more peer referrals to the counseling center. RQ3: Are there significant demographic differences in FSV barriers to counseling among STEM students? Ha3: Statistically significant demographic differences in STEM students’ RFSV scores will emerge.
Methods
Participants and Procedures
Following IRB approval, first author Michael T. Kalkbrenner obtained an email list from the Office of University Student Records of all students who were enrolled in a STEM major at a research-intensive university with four campus locations in three cities located in the Southwestern United States. A recruitment message was sent out to the email list via Qualtrics Secure Online Survey Platform. A total of 407 prospective participants clicked on the survey link. A response rate could not be calculated, as Qualtrics does not track inaccurate or inactive email addresses. A review of the raw data revealed 41 cases with 100% missing data. Likely, these 41 prospective participants clicked on the link to the survey and decided not to participate. Following the removal of those 41 cases, less than 20% of data were missing for the remaining 366 cases. Little’s Missing Completely at Random test indicated that the data could be treated as missing completely at random (p = .118) and expectation maximization was used to impute missing values. An investigation of standardized z-scores revealed six univariate outliers (z > ± 3.29) and Mahalanobis distances displayed eight multivariate outliers, which were removed from the data set, yielding a robust sample of N = 352.
Participants ranged in age from 18 to 63 (M = 24.29; SD = 8.59). The demographic profile for gender identity consisted of 65.1% (n = 229) female, 30.4% (n = 107) male, 2.0% (n = 7) non-binary, 1.1% (n = 4) transgender, 0.6% (n = 2) an identity not listed (“please specify”), and 0.9% (n = 3) prefer not to answer. The ethnoracial demographic profile consisted of 2.6% (n = 9) Native Indian or Alaska Native; 3.1% (n = 11) Asian or Asian American; 2.0% (n = 7) Black or African American; 48.3% (n = 170) Hispanic, Latinx, or Spanish origin; 2.0% (n = 7) Middle Eastern or North African; 3.4% (n = 12) Multiethnic; 36.6% (n = 129) White or European American; 1.1% (n = 4) Another race, ethnicity, or origin (“please specify”); and 0.9% (n = 3) preferred not to answer. The present sample was composed of notably more diverse groups of STEM students when compared to national estimates of STEM students (National Center for Educational Statistics [NCES], 2020). The NCES’s estimates revealed fewer women (33.0%, n = 263,034) and Latinx (12.3%, n = 94,927) STEM students as well as fewer White students (49.8%, n = 385,132). But the NCES’s national estimates included larger proportions of Black (7.2%, n = 55,642) and Asian (11.0%, n = 85,135) STEM students when compared to the present sample.
Instrumentation
Participants completed a demographic questionnaire by indicating their informed consent, then confirming they met the following inclusion criteria for participation: (a) 18 years or older, (b) enrolled in at least one undergraduate STEM course, and (c) currently a STEM major. The demographic questionnaire concluded with questions about respondents’ age, gender identity, ethnoracial identity, help-seeking history, and if they had referred one or more peers to the counseling center.
The Revised FSV Scale
The RFSV Scale is a screening tool that was designed to measure barriers to seeking counseling (Kalkbrenner, Neukrug, & Griffith, 2019). Participants respond to a prompt (“I am less likely to attend counseling because . . . ”) for 14 declarative statements on the following Likert scale: 1 = Strongly Disagree, 2 = Disagree, 3 = Neither Agree nor Disagree, 4 = Agree, or 5 = Strongly Agree. The RFSV Scale is composed of three subscales or latent traits behind one’s reticence to seek counseling, including Fit, Stigma, and Value. Scores on the Fit subscale can range from 5 to 25, with higher scores indicating more restraint from seeking counseling because one believes the process of counseling is not suitable with their personal worldview (e.g., “I couldn’t find a counselor who would understand me”). Scores on the Stigma subscale also range from 5 to 25, and higher scores denote a greater hesitation to seek counseling due to feelings of embarrassment or shame (e.g., “It would damage my reputation”). Scores on the Value subscale range from 4 to 20, with higher scores indicating a greater disinclination to seek counseling because they believe the effort required would not be worth the potential benefits (e.g., “Counseling is unnecessary because my problems will resolve naturally”).
The Global Barriers to Counseling scale is composed of test takers’ average composite score across the three Fit, Stigma, and Value subscales and produces an overall estimation of a test taker’s sensitivity to barriers toward seeking counseling. Scores on the Global Barriers to Counseling scale range from 13 to 65, with higher scores indicating a greater reticence to seek counseling. The collective findings of past investigators demonstrated evidence for the internal structure validity (confirmatory factor analysis) and internal consistency reliability (α = .70 to α = .91) of scores on the RFSV Scale with a number of non-college populations (Kalkbrenner, Goodman-Scott, & Neukrug, 2020; Kalkbrenner & Neukrug, 2018, 2019; Kalkbrenner et al., 2019).
Data Analysis
A confirmatory factor analysis (CFA) based on structural equation modeling was computed in IBM SPSS AMOS version 26 to answer the first RQ about the dimensionality of STEM students’ RFSV scores. We used the joint suggestions from Dimitrov (2012) and Schreiber et al. (2006) for acceptable model fit in CFA: chi-square absolute fit index (CMIN; non-significant p-value or χ2 to df < 3), comparative fit index (CFI; .90 to .95 = acceptable fit and > .95 = close fit), root mean square error of approximation (RMSEA; ≤ .08), and the standardized root mean square residual (SRMR; ≤ .08). Internal consistency reliability evidence of test scores is another important step in testing a scale’s psychometric properties. Cronbach’s coefficient alpha (α) is the most popular internal consistency reliability estimate; however, its proper use is dependent on the data meeting several statistical assumptions (McNeish, 2018). Composite internal consistency reliability estimates, such as McDonald’s coefficient omega (ω), tend to produce more stable reliability estimates of scores. Accordingly, the present investigators computed both α and ω.
College students are more likely to discuss mental health concerns with their peers than with faculty, staff, or other university personnel (Wawrzynski et al., 2011; Woodhead et al., 2021). Accordingly, college counseling researchers and practitioners are devoting more time to peer-to-peer mental health support initiatives with the goal of increasing peer-to-peer referrals to the counseling center (Kalkbrenner, Sink, & Smith, 2020; Olson et al., 2016). Past investigators (e.g., Kalkbrenner, Neukrug, & Esquivel, 2022) found that the RFSV barriers were significant predictors of peer-to-peer referrals to the counseling center with non-STEM students. To test the generalizability of this finding with STEM students, we conducted a logistic regression analysis to answer the second RQ regarding the capacity of STEM students’ RFSV scores to predict at least one peer referral to the counseling center. STEM students’ interval-level composite scores on the Fit, Stigma, and Value subscales were entered into the model as predictor variables. The criterion variable was quantified on a categorical scale. On the demographic questionnaire, students responded to the following question: “Have you ever referred (recommended) another student to counseling services?” and selected either “0 = never referred a peer to the counseling center” or “1 = referred one or more peers to the counseling center.”
A 2(gender) X 3(race/ethnicity) X 2(help-seeking history) multivariate analysis of variance (MANOVA) was computed to investigate the third RQ regarding demographic differences in RFSV barriers among STEM students. The three categorical-level independent variables included gender (male or female), race/ethnicity (Latinx, White, or other ethnicity), and help-seeking history (never attended counseling or attended at least one counseling session). The three interval-level dependent variables included STEM students’ composite scores on the Fit, Stigma, and Value subscales. Discriminant analysis was employed as a post hoc test for MANOVA (Warne, 2014).
Results
The RFSV Scale items were entered into a CFA to test the dimensionality of scores with STEM students (RQ1). Excluding the CMIN (χ2 [74] = 257.55, p < .001, χ2 to df = 3.48), results revealed a satisfactory model fit: CFI = .92; RMSEA = .08, 90% CI [.07, .10]; and SRMR = .08. The CMIN tends to underestimate model fit with samples that are large enough for CFA (Dimitrov, 2012). Thus, adequate internal structure validity evidence of scores was achieved based on the collective CFI, RMSEA, and SRMR results. The standardized factor loadings were all acceptable-to-strong and ranged from .48 to .90 (see Figure 1, Model 1).
Figure 1
Revised FSV Scale Path Models With Standardized Coefficients
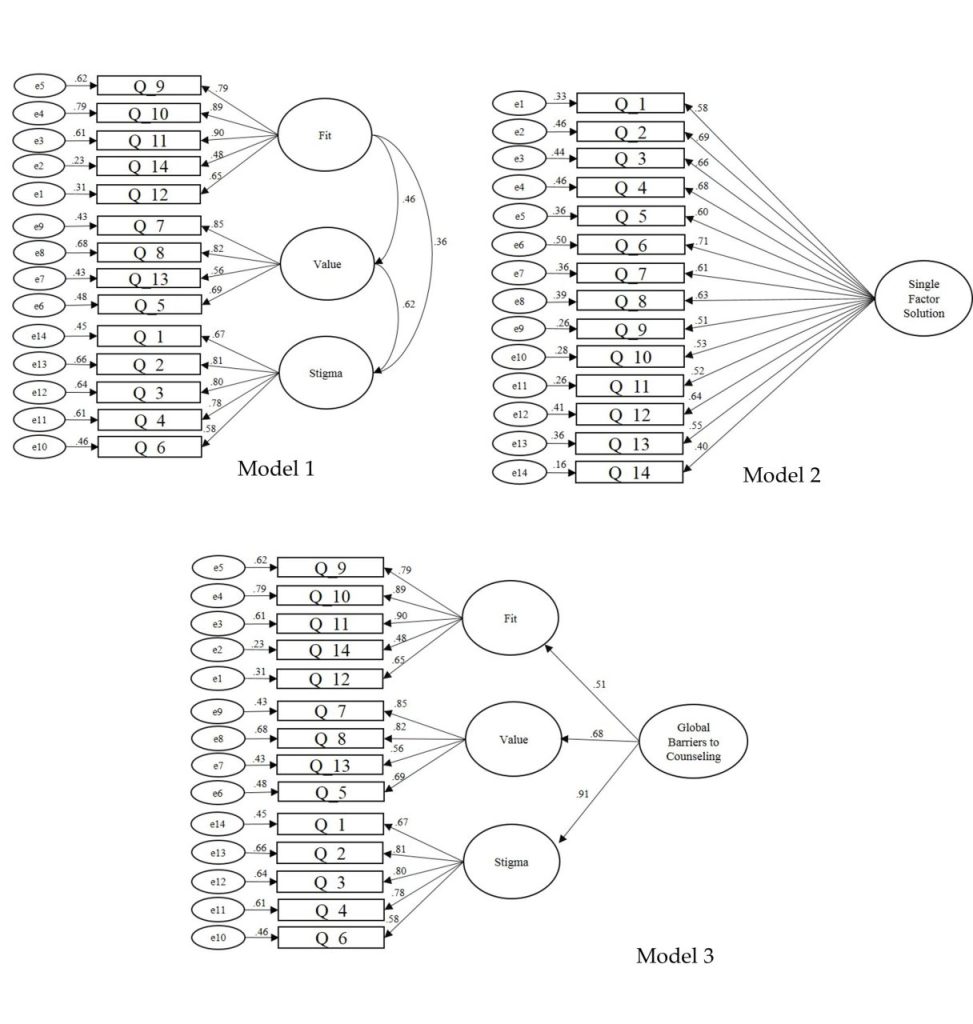
Based on the findings of Kalkbrenner and Neukrug (2019), we computed a higher-order confirmatory factor analysis (HCFA) to test for a Global Barriers to Counseling scale. As expected, the single-factor RFSV model (see Figure 1, Model 2) revealed poor model fit: CMIN (χ2 [77] = 1,013.71, p < .001, χ2 to df = 13.17); CFI = .61; RMSEA = .19, 90% CI [.18, .20]; and SRMR = .13. Accordingly, the theoretical support for a higher-order model (Kalkbrenner & Neukrug, 2019) coupled with the poor fitting single-factor model (see Figure 1, Model 2) indicated that computing an HCFA was appropriate. Except for the CMIN (χ2 [74] = 257.55, p < .001, χ2 to df = 3.48), the higher-order model (see Figure 1, Model 3) displayed a satisfactory model fit: CFI = .92; RMSEA = .08, 90% CI [.07, .10]; and SRMR = .08. Tests of internal consistency reliability revealed satisfactory reliability evidence of scores on the Fit (α = .84, ω = .83), Stigma (α = .86, ω = .87), and Value (α = .79, ω = .79) subscales and the Global Barriers to Counseling scale (α = .88, ω = .88).
STEM students’ RFSV scores were entered into a logistic regression analysis to answer RQ2 regarding the capacity of STEM students’ RFSV scores to predict at least one referral to the counseling center. The logistic regression model was statistically significant, X2(1) = 80.97, p < .001, Nagelkerke R2 = .064. The odds ratios, Exp(B), revealed that a decrease of one unit in STEM students’ scores on the Value subscale (higher scores = less value toward counseling) was associated with a decrease in the odds of having made at least one peer-to-peer referral to the counseling center by a factor of .559.
A factorial MANOVA was computed to answer RQ3 regarding demographic differences in RFSV barriers among STEM students. A significant main effect emerged for gender on the combined dependent variables, F(3, 316) = 5.23, p = .002, Pillai’s Trace = 0.05, η2p = 0.047. The post hoc discriminant analysis (DA) revealed a significant discriminant function, Wilks λ = 0.93, χ2 = 23.60, df = 3, canonical correlation = 0.26, p < .001. The standardized canonical discriminant function coefficients between the latent factors and discriminant functions showed that the Value factor loaded more strongly on the discriminant function (1.10) than the Stigma (0.17) or Fit (−0.62) factors. The mean discriminant score on the function for male participants was 0.40. The mean discriminant score on the function for female participants was −0.19. In other words, the MANOVA and post hoc DA revealed that male STEM students scored significantly higher (higher scores reflect greater reluctance to seek counseling) on the Value barrier when compared to female STEM students.
A significant main effect also emerged for help-seeking history on the combined dependent variables, F(3, 467) = 4.65, p = .003, Pillai’s Trace = 0.04, η2p = 0.042. The post hoc DA displayed a significant discriminant function, Wilks λ = 0.93, χ2 = 24.10, df = 3, canonical correlation = 0.26, p < .001. The standardized canonical discriminant function coefficients between the latent factors and discriminant functions showed that the Value factor loaded more strongly on the discriminant function (1.10) than the Stigma (0.01) or Fit (−0.71) factors. The mean discriminant score on the function for participants without a help-seeking history was 0.25. The mean discriminant score on the function for participants with a help-seeking history was −0.29. In other words, the MANOVA and post hoc DA showed that STEM students without a help-seeking history scored significantly higher on the Value barrier than STEM students with a help-seeking history.
Discussion
The purpose of the present study was to validate STEM students’ scores on the RFSV Scale and investigate demographic correlates with the Fit, Stigma, and Value barriers. The CFA results demonstrated that the RFSV Scale and its dimensions were estimated adequately with a sample of STEM students. This finding is consistent with the existing body of literature on the generalizability of scores on the RFSV Scale with a number of non-college populations (e.g., Kalkbrenner, Goodman-Scott, & Neukrug, 2020; Kalkbrenner & Neukrug, 2018). In addition to a stringent test of internal structure validity, CFA is also a theory-testing procedure (Mvududu & Sink, 2013). Thus, our CFA results indicated that Fit, Stigma, and Value comprise a tri-dimensional theoretical model of barriers to counseling among STEM students. Consistent with the results of Kalkbrenner and Neukrug (2019), we found support for a higher-order Global Barriers to Counseling scale. The presence of a higher-order factor (see Figure 1, Model 3) indicates that the covariation between the first-order Fit, Stigma, and Value subscales comprises a meta-level latent trait. Collectively, the single-order and higher-order CFA results indicate that Fit, Stigma, and Value are discrete dimensions of an interconnected latent trait. Accordingly, CFA results provided support for the dimensionality of both the single-order RFSV model (see Figure 1, Model 1) and the higher-order model (see Figure 1, Model 3) with STEM students.
STEM students face unique risks for mental health issues, including maladaptive perfectionism as well as intense pressure to perform in harsh and competitive academic environments (Rice et al. 2015; Shapiro & Sax, 2011). These unique risk factors coupled with STEM students’ reticence to seek counseling (Kalkbrenner, James, & Pérez-Rojas, 2022) created a need for a screening tool for appraising why STEM students might avoid accessing counseling services. The results of the CFA and HCFA in the present study begin to address the gap in the literature regarding the lack of a screening tool with validated scores for appraising barriers to counseling among STEM students. Our CFA and HCFA results suggest that college counselors can use the RFSV Scale as one way to understand why STEM students on their campus are reluctant to access counseling services.
Consistent with the findings of Kalkbrenner and Neukrug (2019), we found statistically significant differences in peer-to-peer referrals and demographic differences in STEM students’ scores on the Value barrier. Specifically, increases in STEM students’ belief in the value of attending counseling were associated with significant increases in the odds of making one or more peer referrals to the counseling center, as indicated by the moderate effect size of the finding. It appears that STEM students’ attendance in personal counseling increases their propensity for recommending counseling to their peers. Similar to Kalkbrenner and Neukrug (2018), tests of group demographic differences revealed that STEM students in the present study with a help-seeking history were less sensitive to the Value barrier than STEM students without a help-seeking history. These findings indicate that attendance in counseling might enhance STEM students’ belief that the effort required to attend counseling is worth the benefits. Perhaps experiencing counseling firsthand increases STEM students’ belief in the value of counseling as well as their disposition to refer a peer to counseling. This finding has particularly important implications, as STEM students are a distinct college-based population with unique mental health needs who tend to utilize mental health support services at lower rates than non-STEM students (Kalkbrenner, James, & Pérez-Rojas, 2022; Rice et al., 2015; Shapiro & Sax, 2011). In particular, our results suggest that STEM students who access counseling services usually see value in the process. STEM students’ general attitudes about counseling might become more positive if more and more STEM students participate in counseling.
Also, consistent with the findings of Kalkbrenner and Neukrug (2018), we found demographic differences in STEM students’ scores on the Value barrier by gender identity, with males attributing less value to attending counseling than females. Macro- and micro-systemic gender role forces tend to contribute to men’s reticence to seek counseling (Neukrug et al., 2013). These forces might be intensified among male STEM students considering the intersectionality between gender roles and the high-pressure environment in STEM majors to not show vulnerability (Lipson et al., 2016; Neukrug et al., 2013). Specifically, gender-role pressures to avoid showing vulnerability coupled with a high-pressure academic environment might make male STEM students especially reluctant to seek counseling. Men are also less likely than women to recognize and seek treatment for mental health issues (Kalkbrenner & Neukrug 2018; Neukrug et al., 2013). Thus, it is also possible that male STEM students are less likely to recognize mental distress as a potentially serious health issue, which contributes to them placing less value on the benefits of counseling when compared to their female counterparts. Future research is needed to test these possible explanations for this finding.
Implications
The findings of this study have a number of implications for professional counselors who work in college settings. The CFA and HCFA results extend the psychometric properties of the RFSV Scale to STEM students (RQ1), which is an important contribution to the measurement literature, as the scale offers professional counselors a brief screening tool that usually takes 10 minutes or less to complete. The RFSV Scale can be administered at the systemic level (e.g., all STEM students at a university). Tests of internal structure reveal support for a three-dimensional RFSV model (see Figure 1, Model 1) as well as a higher-order model (see Figure 1, Model 3) with STEM students. Accordingly, professional counselors can administer and score one or both RFSV models depending on their mental health screening goals. The Global Barriers to Counseling scale might have utility for college counselors who are aiming to gather baseline information about STEM students’ general reticence to seek counseling. The three-dimensional model can provide more specific information (Fit, Stigma, and/or Value) about the reasons why STEM students on a particular campus are reluctant to seek counseling.
Our results reveal that increases in STEM students’ scores on the Value subscale were associated with a noteworthy increase in the odds of making a peer-to-peer referral to the counseling center. This finding coupled with STEM students’ vulnerability to mental distress (Daker et al., 2021; Kalkbrenner, James, & Pérez-Rojas, 2022; Lipson et al., 2016; Shapiro & Sax, 2011) suggests that peer-to-peer referrals to mental health support services might be more important than ever before in connecting STEM students in mental distress to support services. Professional counselors who work in college settings can administer the RFSV Scale to STEM students and use the results as one method of informing the content of peer-to-peer mental health support initiatives. If, for example, STEM students on a particular campus score higher on the Value subscale (higher scores denote less value toward counseling), there might be utility in including information about the many benefits of counseling in peer-to-peer outreach initiatives for STEM students. Specifically, it might be beneficial to discuss both the academic and personal benefits associated with attending counseling. For groups of STEM students who score higher on the Stigma scale, college counselors might take a strengths-based perspective by discussing how attending counseling takes courage and strength.
College counselors and student affairs officials can reach STEM students by partnering with STEM faculty and administrators to attend STEM orientations and classes that are held in large lecture halls. College counselors may build relationships with department heads and program directors of STEM programs through sharing empirical evidence on STEM students’ unique mental health needs and their reticence to access mental health support services (Kalkbrenner, James, & Pérez-Rojas, 2022; Lipson et al., 2016; Shapiro & Sax, 2011). College counselors might also discuss how increases in STEM students’ mental health is associated with greater retention and academic success, which are key values in STEM programs (Daker et al., 2021; Lockard et al., 2019; Meaders et al., 2020; Muenks et al., 2020). As buy-in from STEM department heads and program directors increases, there might be utility in professional counselors regularly making presentations and facilitating discussions about mental health and the benefits of attending counseling during new STEM student orientations. The content of these presentations can be based on the extant literature regarding the socio-personal factors that can place STEM students at risk for mental distress—for example, maladaptive perfectionism (Rice et al., 2015), high-pressure academic environments (Shapiro & Sax, 2011), and difficulty recognizing warning signs for mental distress (Kalkbrenner, James, & Pérez-Rojas, 2022). Once STEM students learn about these socio-personal factors, the presentation content can shift to psychoeducation about the utility of counseling for improving both personal and academic outcomes (Lockard et al., 2019).
The RFSV Scale can also be administered on more targeted levels, for example, to specific groups of STEM students who might be particularly vulnerable to mental health distress. There might be utility in administering the RFSV Scale to male STEM students considering that we found male STEM students were more sensitive to the Value barrier than female STEM students. College counselors can use the RFSV results to identify specific barriers (e.g., Value) that might be making STEM students on their campus unlikely to access counseling services. Such results can be used to inform thes curriculum of mental health programming (e.g., peer-to-peer support initiatives). When working with male STEM students, college counselors might consider the intersectionality of academic pressure (Lipson et al., 2016) and gender-role–based mental health stressors (Neukrug et al., 2013) they might be facing. In all likelihood, considering the intersectionality between these socio-personal factors will help college counselors address their clients’ presenting concerns holistically.
Limitations and Future Research
The methodological limitations of this research should be reviewed when considering the implications of the results. The preset data were collected from STEM students in three different cities located in the Southwestern United States; however, results might not generalize to STEM students in other geographical locations. Future researchers can validate RFSV scores with national and international samples of STEM students. Moreover, the findings of cross-sectional research designs are correlational, which prevents researchers from drawing conclusions regarding cause-and-effect. Now that STEM students’ scores on the RFSV Scale are validated, future investigators can extend this line of inquiry by conducting outcome research on the effectiveness of interventions geared toward promoting the utilization of mental health support services among STEM students.
Although factor analytic results in the present study were promising, STEM students are not a homogenous group. To this end, future investigators can extend this line of research by conducting factorial invariance testing to examine the psychometric equivalence of RFSV scores across subgroups of STEM students. As just one example, past investigators (e.g., Shapiro & Sax, 2011) found differences in STEM students’ mental health by gender identity. Relatedly, our results did not reveal demographic differences by race/ethnicity in STEM students’ vulnerability to barriers to counseling. However, we used a dummy-coding procedure to create racial/ethnic identity comparison groups (Latinx, White, or other ethnicity) that were large enough for statistical analyses. Clustering participants with racial/ethnic identities other than White or Latinx into one group might have masked significant findings within the other race/ethnicity group. It is also possible that some participants identified as White and Latinx, as White is a racial category and Latinx is an ethnic category. Future researchers should examine potential disparities in barriers to counseling among more racially and ethnically diverse samples of STEM students. In an extension of the extant literature on samples of primarily male STEM students, the present study included notably more (> 50%) female STEM students when compared to a national demographic profile of STEM students (NCES, 2020). However, the findings of the present study might not generalize to STEM students with gender identities that extend beyond only male or female. Accordingly, future researchers can test the invariance of RFSV scores with more gender-diverse samples.
The findings of the CFA and HCFA in the present study supported Fit, Stigma, and Value as barriers to counseling among STEM students. However, the deductive nature of quantitative research does not capture the nuances of participants’ lived experiences. One way that future investigators can extend this line of research is through qualitative investigations of STEM students’ attitudes and values about seeking counseling services. Qualitative results might reveal important nuances and insights into STEM students’ propensity to access mental health support services.
Conclusion
To the best of our knowledge, the present investigation is the first to establish the psychometric properties of a barriers to counseling tool with STEM students. The results represent an important contribution to the measurement literature, as confirming the internal structure of test scores on an existing measure with a previously untested population is a vital step in demonstrating construct validity. We also found that decreases in STEM students’ reticence to seek counseling was predictive of statistically significant increases in the odds of making a peer referral to the counseling center. In addition, results revealed demographic differences in barriers to counseling among STEM students by gender and help-seeking history. Collectively, our findings suggest that professional counselors who work in college settings can use the RFSV Scale as one way to support STEM college student mental health by identifying why STEM students might be reticent to access counseling services. Supporting STEM students’ mental health has implications for increasing their retention rates, completion rates, and overall psychological well-being.
Conflict of Interest and Funding Disclosure
The authors reported no conflict of interest
or funding contributions for the development
of this manuscript.
References
Al-Maraira, O. A., & Shennaq, S. Z. (2021). Investigation of depression, anxiety and stress levels of health-care students during COVID-19 pandemic. Mental Health Review Journal, 26(2), 113–127.
https://doi.org/10.1108/MHRJ-10-2020-0070
Bryan, A. E. B., & Arkowitz, H. (2015). Meta-analysis of the effects of peer-administered psychosocial interventions on symptoms of depression. American Journal of Community Psychology, 55(3–4), 455–471. https://doi.org/10.1007/s10464-015-9718-y
Byrom, N. (2018). An evaluation of a peer support intervention for student mental health. Journal of Mental Health, 27(3), 240–246. https://doi.org/10.1080/09638237.2018.1437605
Caporale-Berkowitz, N. A. (2022). Let’s teach peer support skills to all college students: Here’s how and why. Journal of American College Health, 70(7), 1921–1925. https://doi.org/10.1080/07448481.2020.1841775
Daker, R. J., Gattas, S. U., Sokolowski, H. M., Green, A. E., & Lyons, I. M. (2021). First-year students’ math anxiety predicts STEM avoidance and underperformance throughout university, independently of math ability. NPJ Science of Learning, 6(1), Article 17. https://doi.org/10.1038/s41539-021-00095-7
Dimitrov, D. M. (2012). Statistical methods for validation of assessment scale data in counseling and related fields. American Counseling Association.
Hong, V., Busby, D. R., O’Chel, S., & King, C. A. (2022). University students presenting for psychiatric emergency services: Socio-demographic and clinical factors related to service utilization and suicide risk. Journal of American College Health, 70(3), 773–782. https://doi.org/10.1080/07448481.2020.1764004
Kalkbrenner, M. T., Goodman-Scott, E., & Neukrug, E. S. (2020). Validation of high school students’ scores on the Revised Fit, Stigma, and Value Scale: Implications for school counseling screening. Professional School Counseling, 23(1). https://doi.org/10.1177/2156759X20912750
Kalkbrenner, M. T., James, C., & Pérez-Rojas, A. E. (2022). College students’ awareness of mental disorders and resources: Comparison across academic disciplines. Journal of College Student Psychotherapy, 36(2), 113–134. https://doi.org/10.1080/87568225.2020.1791774
Kalkbrenner, M. T., Lopez, A. L., & Gibbs, J. R. (2020). Establishing the initial validity of the REDFLAGS Model: Implications for college counselors. Journal of College Counseling, 23(2), 98–112. https://doi.org/10.1002/jocc.12152
Kalkbrenner, M. T., & Neukrug, E. S. (2018). Identifying barriers to attendance in counseling among adults in the United States: Confirming the factor structure of the Revised Fit, Stigma, & Value Scale. The Professional Counselor, 8(4), 299–313. https://doi.org/10.15241/mtk.8.4.299
Kalkbrenner, M. T., & Neukrug, E. S. (2019). The utility of the Revised Fit, Stigma, and Value Scale with counselor trainees: Implications for enhancing clinical supervision. The Clinical Supervisor, 38(2), 262–280. https://doi.org/10.1080/07325223.2019.1634665
Kalkbrenner, M. T., Neukrug, E. S., & Esquivel, L. E. (2022). Mental health literacy screening of students in Hispanic Serving Institutions. Journal of Counseling & Development, 100(3), 319–329. https://doi.org/10.1002/jcad.12428
Kalkbrenner, M. T., Neukrug, E. S., & Griffith, S. A. (2019). Appraising counselor attendance in counseling: The validation and application of the Revised Fit, Stigma, and Value Scale. Journal of Mental Health Counseling, 41(1), 21–35. https://doi.org/10.17744/mehc.41.1.03
Kalkbrenner, M. T., Sink, C. A., & Smith, J. L. (2020). Mental health literacy and peer-to-peer counseling referrals among community college students. Journal of Counseling & Development, 98(2), 172–182. https://doi.org/10.1002/jcad.12311
Kivlighan, D. M., III, Schreier, B. A., Gates, C., Hong, J. E., Corkery, J. M., Anderson, C. L., & Keeton, P. M. (2021). The role of mental health counseling in college students’ academic success: An interrupted time series analysis. Journal of Counseling Psychology, 68(5), 562–570. https://doi.org/10.1037/cou0000534
Lipson, S. K., Zhou, S., Wagner, B., Beck, K., & Eisenberg, D. (2016). Major differences: Variations in undergraduate and graduate student mental health and treatment utilization across academic disciplines. Journal of College Student Psychotherapy, 30(1), 23–41. https://doi.org/10.1080/87568225.2016.1105657
Lockard, A. J., Hayes, J. A., Locke, B. D., Bieschke, K. J., & Castonguay, L. G. (2019). Helping those who help themselves: Does counseling enhance retention? Journal of Counseling & Development, 97(2), 128–139. https://doi.org/10.1002/jcad.12244
McNeish, D. (2018). Thanks coefficient alpha, we’ll take it from here. Psychological Methods, 23(3), 412–433. https://doi.org/10.1037/met0000144
Meaders, C. L., Lane, A. K., Morozov, A. I., Shuman, J. K., Toth, E. S., Stains, M., Stetzer, M. R., Vinson, E., Couch, B. A., & Smith, M. K. (2020). Undergraduate student concerns in introductory STEM courses: What they are, how they change, and what influences them. Journal for STEM Education Research, 3(2), 195–216. https://doi.org/10.1007/s41979-020-00031-1
Muenks, K., Canning, E. A., LaCosse, J., Green, D. J., Zirkel, S., Garcia, J. A., & Murphy, M. C. (2020). Does my professor think my ability can change? Students’ perceptions of their STEM professors’ mindset beliefs predict their psychological vulnerability, engagement, and performance in class. Journal of Experimental Psychology, 149(11), 2119–2144. https://doi.org/10.1037/xge0000763
Mvududu, N. H., & Sink, C. A. (2013). Factor analysis in counseling research and practice. Counseling Outcome Research and Evaluation, 4(2), 75–98. https://doi.org/10.1177/2150137813494766
National Center for Educational Statistics. (2020). Science, Technology, Engineering, and Mathematics (STEM) education, by gender. https://nces.ed.gov/fastfacts/display.asp?id=899
Neukrug, E., Britton, B. S., & Crews, R. C. (2013). Common health-related concerns of men: Implications for counselors. Journal of Counseling & Development, 91(4), 390–397. https://doi.org/10.1002/j.1556-6676.2013.00109
Neukrug, E. S., Kalkbrenner, M. T., & Griffith, S.-A. M. (2017). Barriers to counseling among human service professionals: The development and validation of the Fit, Stigma, & Value (FSV) Scale. Journal of Human Services, 37(1), 27–40. https://digitalcommons.odu.edu/cgi/viewcontent.cgi?article=1016&context=chs_pubs
Olson, K., Koscak, G., Foroudi, P., Mitalas, E., & Noble, L. (2016). Recognize and refer: Engaging the Greek community in active bystander training. College Student Affairs Journal, 34(3), 48–61. https://doi.org/10.1353/csj.2016.0018
Rice, K. G., Ray, M. E., Davis, D. E., DeBlaere, C., & Ashby, J. S. (2015). Perfectionism and longitudinal patterns of stress for STEM majors: Implications for academic performance. Journal of Counseling Psychology, 62(4), 718–731. https://doi.org/10.1037/cou0000097
Rincon, B. E., & George-Jackson, C. E. (2016). STEM intervention programs: Funding practices and challenges. Studies in Higher Education, 41(3), 429–444. https://doi.org/10.1080/03075079.2014.927845
Schreiber, J. B., Nora, A., Stage, F. K., Barlow, E. A., & King, J. (2006). Reporting structural equation modeling and confirmatory factor analysis results: A review. The Journal of Educational Research, 99(6), 323–338. https://doi.org/10.3200/JOER.99.6.323-338
Schwitzer, A. M., Moss, C. B., Pribesh, S. L., St. John, D. J., Burnett, D. D., Thompson, L. H., & Foss, J. J. (2018). Students with mental health needs: College counseling experiences and academic success. Journal of College Student Development, 59(1), 3–20. https://doi.org/10.1353/csd.2018.0001
Shapiro, C. A., & Sax, L. J. (2011). Major selection and persistence for women in STEM. New Directions for Institutional Research, 2011(152), 5–18. https://doi.org/10.1002/ir.404
U.S. Department of Education. (2020). Science, technology, engineering, and math, including computer science. https://www.ed.gov/stem
Warne, R. (2014). A primer on multivariate analysis of variance (MANOVA) for behavioral scientists. Practical Assessment, Research, and Evaluation, 19, 1–10. https://doi.org/10.7275/sm63-7h70
Wawrzynski, M. R., LoConte, C. L., & Straker, E. J. (2011). Learning outcomes for peer educators: The national survey on peer education. Emerging Issues and Practices in Peer Education, 2011(133), 17–27.
https://doi.org/10.1002/ss.381
Woodhead, E. L., Chin-Newman, C., Spink, K., Hoang, M., & Smith, S. A. (2021). College students’ disclosure of mental health problems on campus. Journal of American College Health, 69(7), 734–741.
https://doi.org/10.1080/07448481.2019.170653
Michael T. Kalkbrenner, PhD, NCC, is an associate professor at New Mexico State University. Gabriella Miceli, MS, LPC-A, is a doctoral student at New Mexico State University. Correspondence may be addressed to Michael T. Kalkbrenner, 1780 E. University Ave., Las Cruces, NM 88003, mkalk001@nmsu.edu.
Aug 10, 2022 | Volume 12 - Issue 2
Sabina Remmers de Vries, Christine D. Gonzales-Wong
U.S. consumers are spending billions on complementary and alternative medicines, and nearly half of those consumers on psychiatric prescription drugs also use herbal remedies. Clients may take herbaceuticals, over-the-counter drugs, and dietary supplements instead of, or in combination with, prescription drugs. This frequently occurs without the input or knowledge of prescribers, which can create significant problems for clients. There is a growing need for counselors to be familiar with herbal remedies, over-the-counter drugs, and dietary supplements. It is vital that counselors understand the potential interaction of these substances with prescribed medications, as well as their impact on clients’ emotions, thoughts, and behaviors. This article reviews relevant research and professional publications in order to provide an overview of the most commonly used psychoactive non-prescription products, counselor roles, client concerns, associated counseling ethics, diversity and cultural considerations, and counselor supervision concerns.
Keywords: counseling ethics, herbaceuticals, over-the-counter drugs, dietary supplements, diversity
A recent survey by the World Health Organization (WHO) World Mental Health Survey Consortium reported inadequate treatment of mental health conditions, especially in disadvantaged populations (Borges et al., 2020). In 2019, an estimated 20.6% of adults in the United States (51.5 million adults) experienced some type of mental health problem (National Institute of Mental Health, 2019). In an attempt to address mental health concerns, clients may take a variety of drugs, which can range from prescribed psychotropic medications to self-administered herbal remedies, over-the-counter drugs (OTCs), and dietary supplements (Ravven et al., 2011). Researchers have found that older adults, particularly, use prescription drugs, herbal remedies, and dietary supplements concurrently (Agbabiaka et al., 2017; Kaufman et al., 2002). Herbal remedies and dietary supplements are part of complementary and alternative medicines (CAMs), which consist of various products and practices (Nahin et al., 2009).
In terms of mental health diagnoses (e.g., major depressive disorder, bipolar disorder, schizophrenia, anxiety disorder), prescription medication noncompliance can range between 28%–72% (Julius et al., 2009). There are many reasons clients do not adhere to their psychotropic medication regimens, including client-specific factors (psychological factors, habits, and beliefs), drug-specific factors (side effects), social/environmental factors (support system issues), and financial considerations (cost of medications, copays, and deductibles; Freudenberg-Hua et al., 2019; Julius et al., 2009; Phillips et al., 2016). There are clients who want to take their medication as prescribed but may not be able to afford it (Wang et al. 2015). Researchers found that clients might be prone to reduce use of prescription medication or substitute with OTCs and CAMs when experiencing financial pressures (Agbabiaka et al., 2017; Gibson, 2005; Wang et al., 2015). Another concern is lack of client knowledge pertaining to medications and diagnoses. Makaryus and Friedman (2005) found that only 27.9% of surveyed patients knew the names of all of the medications they had been prescribed, only 37.2% knew the purpose of all of their prescribed drugs, and only 14% knew the most frequent side effects.
For a variety of reasons, a substantial number of clients do not readily disclose the use of CAMs and OTCs to physicians or therapists (Agbabiaka et al., 2017; Ravven et al., 2011). This is concerning, as clients may be unaware of the pharmacological properties and side effects of these products. Considering these factors, counselors have a professional and ethical obligation to possess a working knowledge of psychopharmacology (American Counseling Association [ACA], 2014; Council for Accreditation of Counseling and Related Educational Programs [CACREP], 2016; Murray & Murray, 2007). We assert that this knowledge should include herbal remedies, OTCs, and dietary supplements.
Despite the potential impact of psychoactive drugs on mental health, there is a paucity of research in the counseling literature that addresses psychopharmacology (Ingersoll, 2005; Sepulveda et al., 2016). There is even less counseling literature available that references herbal remedies, dietary supplements, and OTCs (Ingersoll, 2005; Kaut & Dickerson, 2007). A recent search of the ACA and ACA division journals returned very limited results on psychopharmacology, herbal remedies, OTCs, and dietary supplements. For example, the greatest number of articles pertaining to psychopharmacology was found in the Journal of Mental Health Counseling. The journal published five articles that ranged in year of publication from 2002 to 2011. The Journal of Counseling & Development published three articles that ranged in year of publication from 1985 to 2004. The only article related to herbaceuticals was published in the Journal of Counseling & Development in 2005. This article by Ingersoll (2005) discussed herbaceuticals in reference to the counseling profession. Although this review provided an overview of herbal remedies, it did not explore OTCs or dietary supplements. The counseling literature is in urgent need of expansion in this area because the scope of the counseling profession and mental health care are steadily evolving (Kaut, 2011; Sepulveda et al., 2016).
Given the lack of literature, counseling professionals providing services to clients may lack practical information pertaining to herbal remedies, OTCs, and dietary supplements. The goal of this primer is to provide counselors with an introduction to CAMs and OTCs that clients may be taking. It provides an overview of the most frequently used non-prescription psychoactive products, and addresses the actions of these products (pharmacodynamics) and how the body responds (pharmacokinetics) to these substances. The most significant effects as well as side effects are also discussed. In addition, effective communication with clients about prescription and non-prescription drugs is examined. It reviews ethical and cultural considerations pertaining to counseling clients who use psychoactive herbal remedies, OTCs, and dietary supplements. The herbal remedies, OTCs, and dietary supplements selected for this article were those that, based on the literature, appeared to be most commonly used.
Definition of Terms
For the purpose of this article, several terms are defined. For example, pharmacodynamics is the study of how the body responds to a drug. As such, it addresses therapeutic effects as well as side effects (Stahl, 2021). Pharmacokinetics describes how the body absorbs, distributes, metabolizes, and excretes drugs and herbal remedies (He et al., 2011). Drugs and herbal remedies may affect organs, enzymes, and receptor sites. There are receptors located on neurons, which offer binding sites for neurotransmitters. These receptors are designed to respond to specific neurotransmitters. For example, dopamine will only bind to dopamine receptors and will not impact receptors designed for other neurotransmitters (Preston et al., 2021).
There are several neurotransmitters that are considered important in terms of mental health. Neurotransmitters can be agonistic, which means they can activate specific receptors. Neurotransmitters can also exert antagonistic effects by blocking receptor sites and preventing the activation of receptors (Preston et al., 2021). The most important neurotransmitters in terms of mental health are serotonin, dopamine, GABA, norepinephrine, glutamate, and acetylcholine (Stahl, 2021). It is important to note that these neurotransmitters are involved in complex brain functions and often act in combination with other substances and neurotransmitters. Serotonin plays a role in anxiety disorders and depression. Dopamine has been implicated in psychotic disorders as well as bipolar disorder. GABA is considered to be inhibitory to the firing of neurons. Norepinephrine is involved in many functions including memory and mood. Glutamate is an excitatory neurotransmitter. Too much glutamate can lead to cell death. It has been implicated in bipolar disorder and Alzheimer’s disease. Acetylcholine is involved in memory and it has also been implicated in Alzheimer’s disease (Ingersoll & Rak, 2016).
The therapeutic index or window describes the parameter between an effective dose and a toxic dose of a drug. Some drugs such as lithium (used for the treatment of bipolar disorder) have a narrow therapeutic window, meaning that the effective dose and the toxic dose are in close proximity to each other and care must be taken when prescribing these drugs (Preston et al., 2021).
Drugs and herbal remedies may be additive (or synergistic). Additive effects are those in which a drug or herbal remedy may increase or improve the action of another drug or herbal remedy. Drugs or herbal remedies may also act antagonistically, which means the drug/herbal remedy renders another drug/herbal remedy less effective (Sharma et al., 2021). Drug interaction refers to how two or more drugs impact each other in terms of changes in absorption, distribution, metabolism, and excretion (Preston et al., 2021). Half-life refers to the time it takes the body to decrease the blood level of a drug by 50%. The half-life of drugs and herbal remedies can vary greatly, ranging from hours to days (Ingersoll & Rak, 2016). Many herbal remedies and drugs are metabolized through the cytochrome P450 enzymatic system located primarily in the liver and the gastrointestinal system (Stahl, 2021).
Finally, serotonin syndrome can be a life-threatening, adverse reaction to the often unintentional overuse of drugs containing serotonin, or drugs that inhibit serotonin reuptake. Scotton et al. (2019) provided an overview of serotonin syndrome, noting that serotonin serves many functions in the brain and body, including regulating cognitive, emotional, and behavioral functions as well as regulating body temperature and digestion. Serotonin syndrome symptoms can range from mild to severe and can even lead to death. There are a host of symptoms caused by serotonin toxicity (too much serotonin) ranging from diarrhea, tachycardia, agitation, and experiencing tremors to life-threatening symptoms such as delirium, neuromuscular rigidity, hyperthermia, seizures, and coma. The main group of drugs implicated in serotonin syndrome are SSRIs in combination with other serotonergic substances, which also include herbal remedies and OTCs (Scotton et al., 2019). The following sections provide counselors with a detailed overview of herbal remedies and OTCs.
Herbal Remedies
It has been estimated that about 25%–35% of Americans use or have used herbal medicines (Rashrash et al., 2017; Wu et al., 2011). A National Institute of Health survey (Nahin et al., 2009) revealed that in the United States, consumers spent $33.9 billion on CAMs, with $14.8 billion going toward non-vitamin, non-mineral, and natural products (e.g., herbal remedies, melatonin, fish oil, glucosamine). This is roughly equivalent to one-third of the out-of-pocket expenditure for prescription drugs (Nahin et al., 2009). Ravven et al. (2011) found that 44.7% of those using psychiatric prescription drugs also used herbal remedies at the same time.
The WHO defines herbal medicines as consisting of “herbs, herbal materials, herbal preparations, and finished herbal products” (Disch et al. 2017, p. 7). The U.S. Food and Drug Administration (FDA) considers herbal products to be botanicals, which include plant parts, fungi, and algae (FDA, 2015). Many herbal remedies contain compounds that are pharmaceutically active. These compounds can exert an effect on the body or the central nervous system (Sarris, 2018). It has been estimated that about 40% of modern pharmaceuticals originated from naturally occurring treatments (Balick & Cox, 2021). However, in accordance with U.S. laws, herbal remedies or herbaceuticals cannot be marketed as drugs. The FDA is only able to regulate herbaceuticals as dietary supplements. In general, oversight seems marginal in comparison to prescription drugs. For example, manufacturers do not have to seek FDA approval before selling herbal remedies as is required for prescription drugs, and claims made by manufacturers pertaining to dietary supplements are not evaluated by the FDA (A. C. Brown, 2017). Herbal remedies and dietary supplements do not undergo rigorous research and development in the same manner as pharmaceuticals. The FDA is currently only able to monitor those herbal remedies and dietary supplements (and their corresponding ingredients) after they are sold and adverse reactions have been reported, making possible adulteration one of the most worrisome safety concerns pertaining to herbal remedies and dietary supplements (A. C. Brown, 2017). Research has shown that many herbaceuticals are contaminated and are augmented with unlabeled fillers (Crighton et al., 2019; Newmaster et al., 2013). Herbaceuticals can be contaminated by dust and pollen; microbes; parasites; fungi; pesticides; and heavy metals such as lead, arsenic, mercury, and cadmium (de Sousa Lima et al., 2020; Posadzki et al., 2013,: P. Singh et al., 2008). Also, product substitution is a common problem; however, the lack of more effective FDA oversight does not limit herbaceutical popularity or use (Newmaster et al., 2013).
Ravven et al. (2011) estimated that one-quarter to one-third of all herbal remedies in the United States are purchased with the intent to treat mental health conditions, especially anxiety and depression. CAMs such as herbal remedies and dietary supplements can create problems when they interact with medication prescribed by a physician. It is also important to note that many herbal remedies are not harmless; some can cause significant toxic side effects. Counselors must be familiar with the benefits and risks of the more widely used remedies, including St. John’s wort, valerian, kava, ginkgo, and cannabidiol.
St. John’s Wort
St. John’s wort has been found to be effective in the treatment of mild to moderate depression (Apaydin et al., 2016). There are some indications that it is comparable in effectiveness to tricyclic antidepressants and selective serotonin reuptake inhibitors (SSRIs) while also offering greater tolerability (Zirak et al., 2019). A meta-analysis including 27 studies and 3,808 participants confirmed that St. John’s wort seems to be as effective as SSRIs and tricyclic antidepressants when used in the treatment of depression (Q. X. Ng et al., 2017). St. John’s wort was found to be associated with significantly lower discontinuation rates when compared to prescribed antidepressants, may cause fewer side effects than prescription antidepressants, and might be beneficial for clients who struggle with tolerating the side effects of commonly prescribed antidepressants (Q. X. Ng et al., 2017; Zirak et al., 2019). St. John’s wort is also considered a low-cost alternative to prescription antidepressants (Zirak et al., 2019). It is most frequently taken orally as either a whole herb formulation or as an extract, and can also be prepared as an herbal tea (Kladar et al., 2020).
Despite all the benefits it offers, taking St. John’s wort is not without risks. It acts as an SSRI and can lead to serotonin syndrome if combined with other SSRIs (Apaydin et al., 2016). In addition to affecting serotonin levels, St. John’s wort also impacts the neurotransmitters dopamine, norepinephrine, GABA, and glutamate (Brahmachari, 2018). A main side effect is photosensitivity. It is also possible for St. John’s wort to negatively interact with MAOIs (LaFrance et al., 2000; Sidhu & Marwaha, 2021). In addition, due to cytochrome P450 induction, it also impacts the effectiveness of commonly used medications such as warfarin (used to treat blood clots), ciclosporin (an immunosuppressant), digoxin (for arrythmias and heart failure), some anticonvulsants, oral contraceptives, and other drugs (Barnes et al., 2001; Chrubasik-Hausmann et al., 2019; Sharma et al., 2021). It has been noted that consumers continue to take St. John’s wort in combination with other drugs despite warnings, and it is important that clients receive further education on this topic (Chrubasik-Hausmann et al., 2019).
Valerian
Valerian root has been used as a sedative and hypnotic since antiquity (Perry et al., 2006). In Europe, valerian is widely used for the treatment of anxiety and sleep disorders (Shinjyo et al., 2020). It is considered to be effective in the treatment of anxiety, certain sleep disorders, some seizure disorders, possibly OCD, cognitive problems, and menstrual and menopausal symptoms (LaFrance et al., 2000; Shinjyo et al., 2020). The medicinal parts of the plant consist of the underground segments and roots and can be ingested as a juice, tea, dried herb, extract, or tincture (Gruenwald et al. 2007). Valerian is thought to enhance GABA transmission and prevent enzymatic breakdown of GABA in the brain (Mulyawan et al., 2020; K. Savage et al., 2018).
No noteworthy adverse side effects seem to occur when it is taken at an appropriate dose (LaFrance et al., 2000; Shinjyo et al., 2020). Effective doses can range from 450mg–1410mg per day for whole herb preparations, and 300mg–600mg per day for valerian extract (Shinjyo et al., 2020). The non–habit-forming properties and limited potential for side effects may be beneficial for some clients (Al-Attraqchi et al., 2020). However, if valerian is combined with hepatoxic drugs, it may increase the risk of hepatoxicity and could lead to liver damage. Also, taking valerian in combination with other sedating drugs or alcohol may result in additive or synergistic effects, resulting in amplification of sedation or intoxication greater than their combined effect; when taken with loperamide (anti-diarrhea drug), it may also cause delirium (Gruenwald et al., 2007).
Kava
Kava is a medicinal plant belonging to the pepper family with origins in the South Pacific. Traditionally, it has been used as a relaxant. Kava ingested in larger quantities can cause intoxication (Sarris, 2018). Kava is considered to be a hypnotic and a sedative, and it also has analgesic properties (Gruenwald et al., 2007). Hypnotics are drugs that tend to be sleep inducing, whereas sedatives tend to have calming, anxiety-reducing effects (Perry et al., 2006). The medicinally active part of the plant are the rhizomes or creeping rootstalks (Gruenwald et al., 2007). Traditionally, kava beverages were made from the rhizomes; however, in the United States it is mainly available as dry-filled capsule preparations and less commonly as a tincture (Liu et al., 2018). It acts on GABA and has been found to be effective in the treatment of anxiety and insomnia (Gruenwald et al., 2007; LaFrance et al., 2000; Perry et al., 2006; Sarris, 2018). It also has muscle-relaxing, anticonvulsive, and antispasmodic effects (Gruenwald et al., 2007). It is comparable to diazepam in its effectiveness when used to treat anxiety, but it can cause elevation of liver enzymes, which may be an indication of inflammation or even damage to liver cells (Gruenwald et al., 2007; Pantano et al., 2016). When combined with benzodiazepines, kava can cause disorientation and lethargy due to an additive effect in which both substances bind to similar neuron receptors (Surana et al., 2021; Tallarida, 2007).
It is important to note that in the 1990s, Germany approved the use of kava to treat anxiety-related disorders. In 2001, it was banned in Germany and across the European Union because of concerns over liver toxicity. The FDA issued a consumer advisory warning pertaining to the use of kava (Liu et al., 2018). Additional findings indicated only limited risk of liver toxicity when kava was used appropriately, and in 2015 the kava ban in Germany was lifted; however, kava products remain strictly regulated and monitored. In the United States, kava remains available over the counter (Liu et al., 2018).
Ginkgo
Ginkgo has been used in Chinese medicine for a millennium. The herbal remedy is derived from an ancient tree native to China, Japan, and Korea (Gruenwald et al., 2007; Ingersoll, 2005). Ginkgo biloba extract is made from the ginkgo tree leaves (S. K. Singh et al., 2019). It can be difficult to obtain a high-quality product because of poor oversight and regulation of herbal remedies (Booker et al., 2016); however, a standardized ginkgo biloba extract (EGb761) is available (Hashiguchi et al., 2015). Ginkgo shows some effectiveness in the treatment of dementia, Alzheimer’s disease, and other neurodegenerative disorders (S. K. Singh et al., 2019). Several meta-analyses have confirmed the effectiveness of ginkgo biloba. For example, a meta-analysis conducted by Liao et al. (2020) that included seven studies and 939 participants found that standardized gingko extract was effective in improving cognitive function in Alzheimer’s patients. It has been shown that ginkgo has anti-inflammatory, vascular, and cognition enhancing effects. Ginkgo is considered a GABA agonist as well as an antioxidant (S. K. Singh et al., 2019). In addition to improving cognitive function, it may also lessen oxidative damage, which has been implicated in the development of Alzheimer’s disease (S. K. Singh et al., 2019; Solas et al., 2015). Ginkgo appears to be effective in the treatment of mild to moderate memory loss in the elderly and it may slow the deterioration rate in severe dementia. In addition to neuroprotective properties, ginkgo also appears to be effective in the treatment of asthma, depression, and vascular deficiencies (S. K. Singh et al., 2019.) In terms of adverse effects, it may cause mild gastrointestinal upset, and it may also lower the seizure threshold in vulnerable individuals (Gruenwald et al., 2007).
Cannabidiol
Cannabidiol (CBD) is an active compound found in the cannabis plant (FDA, 2020a) and is most commonly promoted online as a remedy for anxiety and physical pain (Tran & Kavuluru, 2020). It also has promising potential for anti-inflammatory effects and has shown positive results in treating schizophrenia and social anxiety disorder (Burstein, 2015; Millar et al., 2019). CBD is a cannabinoid system modulator (Darkovska-Serafimovska et al., 2018) and differs from delta-9-tetrahydrocannabinol (THC) in that it does not produce intoxication (Burstein, 2015). The FDA has approved EpidiolexTM, a prescribed CBD-derived oral solution, for use with treating rare forms of epilepsy (FDA, 2020a).
Although under federal law it is currently illegal to add CBD to food or beverages, individual states have differing laws regarding the distribution of CBD, so the dosage of CBD products remains mostly unregulated (FDA, 2020b). Researchers examined 84 CBD products including vaporization liquids, oils, and tinctures and found that 69% of dosage labels were inaccurate (Bonn-Miller et al., 2017). Although unlikely, it is possible for consumers to test positive for THC in some drug screening tests because up to 0.3% THC may be allowed in CBD products in the United States (Gerace et al., 2021; Spindle et al., 2020). CBD taken in combination with other drugs can cause adverse drug reactions and drug–drug interactions (J. D. Brown & Winterstein, 2019). For example, when CBD is taken with a benzodiazepine (e.g., alprazolam for anxiety), it can increase the risk of side effects of alprazolam. It should be noted that researchers mainly examined EpidiolexTM in studies exploring drug–drug interactions and adverse side effects, as the CBD dosage is controlled in this formulation (J. D. Brown & Winterstein, 2019). Because of the wide dosage variance in unregulated CBD products, it is difficult to research and predict the effects. In a review of clinical studies, the therapeutic window appears to be wide, but phase III trials have not been conducted to provide conclusive evidence (Millar et al., 2019).
Over-the-Counter Medications
Globally, in 2017 the OTC market reached $80.2 billion in consumer spending (PR Newswire, n.d.) and research indicates that 81% of American adults reach for OTCs, or medicine that can be purchased without a prescription, as an initial treatment for minor medical conditions. The average American makes 26 trips to OTC outlets compared to three doctor’s visits annually, and there are around 54,000 pharmacies in the United States compared to over 750,000 retailers that sell OTCs (Consumer Healthcare Products Association, n.d.). Despite the popularity of OTCs, many clients lack the required health knowledge to safely self-medicate.
Acetaminophen
Many consumers do not know that an overly high dose of acetaminophen could be lethal, or that varying OTCs contain acetaminophen and taking more than one of these products simultaneously might lead to an unintentional overdose (Boudjemai et al., 2013; Wolf et al., 2012). There are a number of OTCs that have psychotropic properties. For example, Durso et al. (2015) found that acetaminophen blunts more than just pain—it seems that the OTC pain medication also diminishes emotional responses to both negative and positive events. Researchers went so far as to label acetaminophen as an “all-purpose emotional reliever” (Durso et al., 2015, p. 756). In addition, it is of interest to note that acetaminophen decreases a person’s ability to empathize with pain experienced by others (Durso et al., 2015). Roughly one-quarter of American adults are taking this drug on a weekly basis. It begs the question as to the societal implications or social cost of its frequent use (Mischkowski et al., 2016, 2019).
Sleep Aids
It is common for people to experience trouble with falling asleep or staying asleep. The Diagnostic and Statistical Manual of Mental Disorders (5th ed.; DSM-5; American Psychiatric Association, 2013) indicates that one-third of adults in the United States experience insomnia symptoms. This issue is evident in consumer spending: In 2018 Americans spent $410 million on OTC sleep aids (Consumer Healthcare Products Association, n.d.).
Diphenhydramine and doxylamine are OTC antihistamines with considerable sedative properties and are marketed as treatment options for sleep disturbances (Perry et al., 2006). It was found that doxylamine seems to be as effective as the barbiturate secobarbital; also, doxylamine is comparable to zolpidem, a frequently prescribed sleep aid. Diphenhydramine and doxylamine are considered to be non-selective histamine H1 receptor antagonists (antihistamines for the prevention of allergies) and they are also anticholinergic (causing dry mouth, constipation, urinary retention, blurred vision, and sedation; Perry et al., 2006). Abraham et al. (2017) found that 58.6% of the elderly sample surveyed used at least one sleep aid containing diphenhydramine or doxylamine.
Chlorpheniramine is also an OTC antihistamine, and it can be found as the sole active compound in remedies such as Chlor-TrimetonTM and similar generic formulations (Hellbom, 2006), or in combination with other substances to treat cold and allergy symptoms. Popular cold remedy combinations of chlorpheniramine and dextromethorphan (a cough suppressant also available over the counter) can be problematic. Dextromethorphan is a moderate SSRI (Boyer & Shannon, 2005; Foong et al., 2018), which means it acts like an SSRI antidepressant. Furthermore, diphenhydramine and chlorpheniramine have also been found to block serotonin reuptake, making them some of the oldest SSRIs (Foong et al., 2018; Hellbom, 2006; Ravina, 2011). It is not commonly known that fluoxetine (Prozac®) was derived from diphenhydramine as a result of attempts to make this drug less sedating (Ravina, 2011).
Despite the fact that these products are readily available over the counter, drugs like diphenhydramine as well as doxylamine are not designed for the long-term treatment of sleep disorders (Abraham et al., 2017). There is a lack of supporting literature in terms of using these drugs for treatment of mental health concerns (Culpepper & Wingertzahn, 2015). It is important to note that if clients are prescribed an antidepressant, chlorpheniramine as well as diphenhydramine can increase the risk of serotonin syndrome (Abraham et al., 2017). It is also important to keep in mind that diphenhydramine can be found in combination with pain relievers/fever reducers such as acetaminophen. This may add to the risk of developing serotonin syndrome because clients may not be aware of the exact content of these formulations (Abraham et al., 2017). Diphenhydramine may also be a drug of abuse. When taken in high doses, it may create a buzz or high because of possible activation of the dopamine-related reward pathways of the brain, which may lead to drug-seeking behaviors (Saran et al., 2017). Finally, a lethal dose of doxylamine can range from 25mg–250mg per kg in body weight (Müller, 1992, as cited in Bockholdt et al., 2001). Doxylamine overdose symptoms include respiratory depression, sedation, and coma (Bockholdt et al., 2001).
Dietary Supplements
Dietary supplements are defined as dietary ingredients that include vitamins, minerals, amino acids, and herbs or botanicals, as well as other substances that can be used to supplement the diet (FDA, 2015). Much like herbal remedies, the FDA does not sufficiently regulate dietary supplements.
Melatonin
Melatonin is a naturally occurring substance that is synthesized from tryptophan. It is secreted by the pineal gland in order to regulate the circadian rhythm. Melatonin is effective in inducing sleep when taken orally as well. In the United States, synthesized melatonin is marketed as a dietary supplement and can be purchased over the counter in doses ranging from 0.3mg–10mg (Perry et al., 2006).
Because the FDA does not sufficiently regulate melatonin, it is important to note that specific dosing guidelines do not exist (R. A. Savage et al., 2020). However, studies have found that doses over 5mg are no more effective than lower doses. Side effects may include headache, fatigue, dizziness, irritability, abdominal cramps, itchiness, and elevated alkaline phosphatase in long-term use (Perry et al., 2006). Furthermore, it was found that the labeled concentration of melatonin content frequently does not match actual content. Erland and Saxena (2017) found variability of melatonin in various samples ranging between ˗83% (lesser dose) to +478% (higher dose). Erland and Saxena also found that eight of their 30 samples contained undisclosed/unlabeled serotonin in addition to melatonin, which may add to health concerns. The majority of supplements that were found to include serotonin also contained other additives such as passionflower, hops, and valerian root. Interestingly, serotonin is a precursor to melatonin (Erland & Saxena, 2017). Unlabeled serotonin content poses a significant problem because many clients self-prescribe melatonin supplements and, under the right circumstances, a relatively small dose can lead to serotonin syndrome (Erland & Saxena, 2017).
SAMe
SAMe (S-Adenosyl-L-methionine) is required for the brain to synthesize the neurotransmitters norepinephrine, dopamine, and serotonin. In the United States, SAMe has been widely available over the counter since the late 1990s (Mischoulon & Fava, 2002). The general consensus is that it is effective in treating depression (Sakurai et al., 2020). Also, SAMe can be utilized as an adjunct to antidepressant medications (Papakostas, 2009; Sakurai et al., 2020). It can be taken orally or be administered by intravenous infusion (Sakurai et al. 2020). A recommended dose of SAMe can range from 400mg–1600mg per day; however, some individuals may have to take a higher dose to achieve improvement of depressive symptoms (Mischoulon & Fava, 2002; Olsufka & Abraham, 2017; Sakurai et al., 2020). Overall, use of SAMe results in little to no side effects, although at higher doses SAMe may cause gastrointestinal discomfort (Sakurai et al., 2020). In clients diagnosed with bipolar disorder it may cause anxiety and mania (Mischoulon & Fava, 2002; Olsufka & Abraham, 2017).
Tryptophan
Tryptophan is an amino acid that the body requires to synthesize proteins (Modoux et al., 2020). Tryptophan is also needed to synthesize serotonin and melatonin (Modoux et al., 2020). Tryptophan was available in the United States in the 1990s. At that time, there was some evidence that it might be effective in treating depression (Perry et al., 2006). Tryptophan was taken off the market after there were concerns that it caused several deaths because of eosinophilia-myalgia syndrome (EMS), an inflammatory disorder that affects multiple body parts and causes high white blood cell counts. There was some speculation that in these cases the ingested tryptophan may have been contaminated (Perry et al., 2006). Tryptophan can now be purchased over the counter again; however, Perry et al. (2006) suggested that because of EMS risks, clients should be encouraged to consult with their physician before taking this product.
The Role of the Counselor
Concerns regarding psychotropic medication can find their way into counseling settings. Clients may take any number of drugs, ranging from prescribed psychotropic medications to herbal remedies, OTCs, and dietary supplements. In order to be able to provide effective counseling services, counselors must attempt to understand the role these drugs play in clients’ lives. Areas to consider include education, assessment, diagnosis, case conceptualization, treatment planning, and client advocacy, such as referral and consultation with medical and psychiatric treatment providers.
Education
Clinicians should be knowledgeable about the intended use of prescribed psychoactive medications as well as herbal remedies, OTCs, and dietary supplements. It is also important to be familiar with route of administration, pharmacokinetics/pharmacodynamics, therapeutic effects, side effects, and contraindications. CAMs frequently fall in and out of favor because of marketing efforts and fads (Crawford & Leventis, 2005; Smith et al., 2017). Consequently, in order to stay abreast of current trends, it is prudent to pursue continuing education in this area. Counselors should be skilled in nonjudgmentally addressing CAMs and OTCs in a variety of areas, including assessment, education, and referrals.
CACREP’s 2016 standards require that counseling students receive education in the “classifications, indications, and contraindications of commonly prescribed psychopharmacological medications for appropriate medical referrals and consultation” (CACREP, 2015, Section 5.2.h., p. 18). Many states, including Texas (Professional Counselors, 2021), require psychopharmacology training for counselor licensure. It could be argued that this education should also extend to herbal remedies, OTCs, and dietary supplements.
Assessment
Counselors also have the option to be proactive and include questions inquiring about CAMs, OTCs, and prescription medication during the intake process, as well as intermittently throughout the counseling relationship with clients. Assessment may include questions about dosage, frequency, and reason for use. Because clients may not think to share CAM and OTC use with counselors, direct questions during the intake process can initiate conversations about psychoactive drugs. Counselors also have the opportunity to educate clients on the biopsychosocial impact of psychoactive drugs that may play a role in their presenting concerns (Kaut & Dickinson, 2007). Assessment also allows counselors to educate clients on the risks and benefits of CAM and OTC use.
Diagnosis
Knowledge about clients’ use of herbal supplements, OTCs, and dietary supplements is important, as clients may unknowingly experience substance-induced problems. For example, garcinia cambogia, a popular weight-loss herbal supplement, can induce mania (Hendrickson et al., 2016). Clients who have taken garcinia cambogia may present with manic symptoms such as grandiosity, decreased need for sleep, irritability, and hallucinations (Hendrickson et al., 2016). Psychosis has also been induced by L-dopa and dendrobium extract, found in OTC performance-enhancing supplements (Flynn et al., 2016), and by herb–herb interactions when taking multiple supplements simultaneously (Wong et al., 2016). Because of the potential for substance-induced problems, counselors should make differential diagnoses by discussing all potential conditions that may be causing the client’s symptoms, which includes ruling out substance etiology (First, 2013).
Case Conceptualization
To understand the nature, history, and context of clients’ presenting concerns, counselors should engage in a case conceptualization process. Macneil et al. (2012) recommended considering predisposing, precipitating, perpetuating, and protective/positive factors that may contribute to or alleviate the client’s presenting concerns. Counselors should consider how herbal supplements, OTCs, and dietary supplements may be a precipitating, perpetuating, and/or positive factor, as these substances may contribute to or alleviate clients’ symptoms.
Treatment Planning
Counselors consider a client’s diagnosis, presenting concerns, and case conceptualization information to make a personalized treatment plan (Macneil et al., 2012). If CAMs and OTCs are relevant to the client’s treatment, counselors may include the monitoring of such substances as an intervention. This would include assessing the client’s use and compliance with their medication regimen, inquiring about side effects, and evaluating how these factors relate to the client’s mental health. Counselors should only practice within the scope of their license, and clients must be referred to qualified medical providers for any medical or medicinal concerns. Counselor roles may include the referral of a client to a specialist such as a psychiatrist for medication evaluation as a component of the client’s treatment plan. Counselors should ensure that physicians they refer to provide quality care.
Client Advocacy
Counselors may advocate for their clients and consult with prescribers on clients’ behalf (Bentley & Walsh, 2013). Again, a significant concern is that clients frequently do not discuss the use of alternative treatments with their physician (Abraham et al., 2017; Agbabiaka et al., 2017). Direct inquiry into the use of CAMs and OTCs and client education can bring about greater clarity and the opportunity to ask clients to discuss these with their medical providers (Agbabiaka et al., 2017). Counselors can encourage and educate clients on how to discuss CAMs and OTCs with their physician or psychiatrist. When assessing, educating, referring, and advocating, counselors must abide by ethical and legal standards.
Ethical Considerations
It is important to note that counselors should under no circumstances recommend herbal remedies, OTCs, or dietary supplements to clients because doing so would be outside of the scope of their practice (ACA, 2014; Ingersoll & Rak, 2016). The ACA (2014) Code of Ethics specifies that “counselors practice only within the boundaries of their competence, based on their education, training, supervised experience, state and national professional credentials, and appropriate professional experience” (Section C.2.a, p. 8). Despite this, professional role boundaries related to psychopharmacology between prescribing physicians and counselors can be unclear at times (Ingersoll & Rak, 2016). For example, clients may ask counselors for advice on medication. So, in addition to keeping abreast of trends in the use of CAMs and OTCs and attending to this during intake and work with clients, developing consultation and referral resources in this area is an important consideration for counselors (Preston et al., 2021). Resources may vary from state to state given differences in licensing and certification of health professionals and general prescribing privileges for psychotropic medications.
There are wide-ranging opinions among counselors pertaining to prescribing psychotropic medications to clients (Ingersoll & Rak, 2016). These opinions cannot dictate whether a client is referred to the medical community for medication evaluation. Counselors are ethically obligated to refer clients to a medical professional when necessary, including referrals related to pharmacotherapy as well as non-prescription drugs, herbal remedies, or dietary supplements. Withholding such a referral may constitute malpractice. The ACA (2014) Code of Ethics states that “counselors act to avoid harming their clients, trainees, and research participants and to minimize or to remedy unavoidable or unanticipated harm” (ACA, 2014, Section A.4.a., p. 4) and also specifies that “counselors are aware of—and avoid imposing—their own values, attitudes, beliefs, and behaviors” (ACA, 2014, Section A.4.b., p. 8).
Diversity and Cultural Considerations
It is important that counselors are able to discuss racial and cultural considerations with clients to ensure competence and to promote the welfare of clients (ACA, 2014). Our commitment to diversity and inclusion must also be extended to clients who are taking psychoactive substances and herbal remedies. It should be noted that genetic research has found that there are a number of significant differences in terms of drug metabolism, effectiveness, and side effects among ethnic groups (Burroughs et al., 2002). At the same time, race, age, and gender can be crude or flawed yardsticks for predicting responsiveness to drugs; however, counselors do need to be aware that there are significant variations in response to drugs based on multiple factors, and that these variations are more the norm than the exception (Bhugra & Bhui, 2018; Burroughs et al., 2002).
Further, racial and ethnic disparities persist in health care, and this may contribute to clients’ decisions to take CAMs and OTCs (Gureje et al., 2015). Less than 6% of active physicians are Hispanic and less than 5% are Black (American Association of Medical Colleges, 2019), even though 40% of Americans are non-White or Hispanic (U.S. Census Bureau, 2020). This can create barriers to obtaining and providing appropriate care, as it has been found that racial or ethnic minority clients are less likely than their White counterparts to receive prescriptions to treat their mental health conditions (Coleman et al., 2016). This inequality may lead clients to seek CAMs or OTCs to treat mental health issues (Coleman et al., 2016; Gureje et al., 2015).
Counselors should consider cultural factors such as a preference for herbal remedies, immigration status and language use, socioeconomic status, and availability of insurance coverage. Traditional medicine often involves the use of herbal remedies and is closely connected to one’s culture, so counselors should be mindful to discuss CAMs with clients in a nonjudgmental and empathetic manner. Traditional forms of medicine have a long history, having evolved over thousands of years (Gureje et al., 2015). Depending on historical or cultural background, there are numerous ways in which these healing methods are being implemented (Gureje et al., 2015).
It is also important for counselors to recognize that traditional medicine is commonly used in middle- and low-income countries and that transplants from these cultural groups in the United States may use or even prefer these types of healing approaches (Gureje et al., 2015). Poverty also plays a role in the use of traditional medicine versus conventional medicine. For many, traditional medicine may be the only affordable or accessible health care option (Gureje et al., 2015). In Mexican culture, individuals may seek assistance from curandera/os for physical or psychological issues (Hoskins & Padrón, 2018). Traditional medicine may be used to treat nervios, depression, and anxiety (Guzmán Gutierrez et al., 2014). For example, an infusion of the yoloxchitl (magnolia) plant may be used to treat nervios, a culture-specific syndrome that can share symptoms of depression and anxiety (Guzmán Gutierrez et al., 2014). Because curanderismo is also a spiritual practice, counselors should be sensitive to the values that may be tied to the use of herbs for mental health concerns.
In addition, some clients prefer to use traditional medicine as well as conventional medicine (Gureje et al., 2015). Although countries such as China and India are formally supporting the integration of traditional and conventional medicine (Gureje et al., 2015), Western medicine and traditional herbal medicine use are not always compatible (C. H. Ng & Bousman, 2018). Because traditional medicine practices are culture-specific, asking clients if they utilize traditional medicine can be an invitation to share about their practices and allow counselors to approach their clients holistically.
Conclusion
There is a growing need for counselors to possess a working knowledge not only of prescribed psychotropic medications, but also of herbal remedies, OTCs, and dietary supplements. As more training programs and licensure boards require psychopharmacology education, counselors should be invested in learning about other psychoactive products clients may be taking. Counselors have the opportunity to assess clients’ use of CAMs and OTCs and consider how they may be relevant to diagnosis, case conceptualization, and treatment planning. In addition, counselors can educate clients about psychoactive products and their impact on mental health. Counselors can also provide referrals and serve as advocates for their clients when working with prescribing providers. From an ethical perspective, psychopharmacology knowledge is increasingly required in order to provide adequate client care. Although this may appear to move counseling practices more toward the medical model, in reality it means the profession is responding to current trends in counseling and client needs. Understanding the potential impact of herbal remedies, OTCs, and dietary supplements on clients’ mood, thinking, and behavior is imperative to understand the whole person and to maintain a holistic counseling approach.
Conflict of Interest and Funding Disclosure
The authors reported no conflict of interest
or funding contributions for the development
of this manuscript.
References
Abraham, O., Schleiden, L., & Albert, S. M. (2017). Over-the-counter medications containing diphenhydramine and doxylamine used by older adults to improve sleep. International Journal of Clinical Pharmacy, 39(4), 808–817. https://doi.org/10.1007/s11096-017-0467-x
Agbabiaka, T. B., Wider, B., Watson, L. K., & Goodman, C. (2017). Concurrent use of prescription drugs and herbal medicinal products in older adults: A systematic review. Drugs & Aging, 34(12), 891–905.
https://doi.org/10.1007/s40266-017-0501-7
Al-Attraqchi, O. H. A., Deb, P. K., & Al-Attraqchi, N. H. A. (2020). Review of the phytochemistry and pharmacological properties of valeriana officinalis. Current Traditional Medicine, 6(4), 260–277.
https://doi.org/10.2174/2215083805666190314112755
American Association of Medical Colleges. (2019). Figure 18. Percentage of all active physicians by race/ethnicity, 2018 [Figure]. https://www.aamc.org/data-reports/workforce/interactive-data/figure-18-percentage-all-active-physicians-race/ethnicity-2018
American Counseling Association. (2014). ACA code of ethics. https://www.counseling.org/Resources/aca-code-of-ethics.pdf
American Psychiatric Association. (2013). Diagnostic and statistical manual of mental disorders (5th ed.).
https://doi.org/10.1176/appi.books.9780890425596
Apaydin, E. A., Maher, A. R., Shanman, R., Booth, M. S., Miles, J. N. V., Sorbero, M. E., & Hempel, S. (2016). A systematic review of St. John’s wort for major depressive disorder. Systematic Reviews, 5(1), Article 148. https://doi.org/10.1186/s13643-016-0325-2
Balick, M. J., & Cox, P. A. (2021). Plants, people, and culture: The science of ethnobotany (2nd ed.). CRC Press.
Barnes, J., Anderson, L. A., & Phillipson, J. D. (2001). St John’s wort (Hypericum perforatum L.): A review of its chemistry, pharmacology and clinical properties. Journal of Pharmacy and Pharmacology, 53(5), 583–600. https://doi.org/10.1211/0022357011775910
Bentley, K. J., & Walsh, J. (2013). The social worker and psychotropic medication: Toward effective collaboration with mental health clients, families, and providers (4th ed.). Brooks/Cole.
Bhugra, D., & Bhui, K. (Eds.). (2018). Textbook of cultural psychiatry (2nd ed.). Cambridge University Press.
Bockholdt, B., Klug, E., & Schneider, V. (2001). Suicide through doxylamine poisoning. Forensic Science International, 119(1), 138–140. https://doi.org/10.1016/S0379-0738(00)00393-5
Bonn-Miller, M. O., Loflin, M. J. E., Thomas, B. F., Marcu, J. P., Hyke, T., & Vandrey, R. (2017). Labeling accuracy of cannabidiol extracts sold online. JAMA, 318(17), 1708–1709. https://doi.org/10.1001/jama.2017.11909
Booker, A., Frommenwiler, D., Reich, E., Horsfield, S., & Heinrich, M. (2016). Adulteration and poor quality of Ginkgo biloba supplements. Journal of Herbal Medicine, 6(2), 79–87.
https://doi.org/10.1016/j.hermed.2016.04.003
Borges, G., Aguilar-Gaxiola, S., Andrade, L., Benjet, C., Cia, A., Kessler, R. C., Orozco, R., Sampson, N., Stagnaro, J. C., Torres, Y., Viana, M. C., & Medina-Mora, M. E. (2020). Twelve-month mental health service use in six countries of the Americas: A regional report from the World Mental Health Surveys. Epidemiology and Psychiatric Sciences, 29, 1–15. https://doi.org/10.1017/S2045796019000477
Boudjemai, Y., Mbida, P., Potinet-Pagliaroli, V., Géffard, F., Leboucher, G., Brazier, J.-L., Allenet, B., & Charpiat, B. (2013). Patients’ knowledge about paracetamol (acetaminophen): A study in a French hospital emergency department. Annales Pharmaceutiques Françaises, 71(4), 260–267. https://doi.org/10.1016/j.pharma.2013.03.001
Boyer, E. W., & Shannon, M. (2005). The serotonin syndrome. The New England Journal of Medicine, 352(11), 1112–1120. https://doi.org/10.1056/NEJMra041867
Brahmachari, G. (Ed.). (2018). Discovery and development of neuroprotective agents from natural products. Elsevier. https://doi.org/10.1016/B978-0-12-809593-5.12001-4
Brown, A. C. (2017). An overview of herb and dietary supplement efficacy, safety and government regulations in the United States with suggested improvements. Part 1 of 5 series. Food and Chemical Toxicology, 107 (Part A), 449–471. https://doi.org/10.1016/j.fct.2016.11.001
Brown, J. D., & Winterstein, A. G. (2019). Potential adverse drug events and drug–drug interactions with medical and consumer cannabidiol (CBD) use. Journal of Clinical Medicine, 8(7), 989.
https://doi.org/10.3390/jcm8070989
Burroughs, V. J., Maxey, R. W., Crawley, L. M., & Levy, R. A. (2002). Cultural and genetic diversity in America: The need for individualized pharmaceutical treatment. National Medical Association and National Pharmaceutical Council. https://www.nccdp.org/resources/CulturalandGeneticDiversity.pdf
Burstein, S. (2015). Cannabidiol (CBD) and its analogs: A review of their effects on inflammation. Bioorganic and Medicinal Chemistry, 23(7), 1377–1385. https://doi.org/10.1016/j.bmc.2015.01.059
Chrubasik-Hausmann, S., Vlachojannis, J., & McLachlan, A. J. (2019). Understanding drug interactions with St John’s wort (Hypericum perforatum L.): Impact of hyperforin content. Journal of Pharmacy and Pharmacology, 71(1), 129–138. https://doi.org/10.1111/jphp.12858
Coleman, K. J., Stewart, C., Waitzfelder, B. E., Zeber, J. E., Morales, L. S., Ahmed, A. T., Ahmedani, B. K., Beck, A., Copeland, L. A., Cummings, J. R., Hunkeler, E. M., Lindberg, N. M., Lynch, F., Lu, C. Y., Owen-Smith, A. A., Trinacty, C. M., Whitebird, R. R., & Simon, G. E. (2016). Racial-ethnic differences in psychiatric diagnoses and treatment across 11 health care systems in the Mental Health Research Network. Psychiatric Services, 67(7), 749–757. https://doi.org/10.1176/appi.ps.201500217
Consumer Healthcare Products Association. (n.d.). OTC sales statistics. https://chpa.org/about-consumer-healthcare/research-data/otc-use-statistics
Council for Accreditation of Counseling and Related Educational Programs. (2015). 2016 CACREP standards. http://www.cacrep.org/wp-content/uploads/2017/08/2016-Standards-with-citations.pdf
Crawford, S. Y., & Leventis, C. (2005). Herbal product claims: Boundaries of marketing and science. Journal of Consumer Marketing, 22(7), 432–436. https://doi.org/10.1108/07363760510631183
Crighton, E., Coghlan, M. L., Farrington, R., Hoban, C. L., Power, M. W. P., Nash, C., Mullaney, I., Byard, R. W., Trengove, R., Musgrave, I. F., Bunce, M., & Maker, G. (2019). Toxicological screening and DNA sequencing detects contamination and adulteration in regulated herbal medicines and supplements for diet, weight loss and cardiovascular health. Journal of Pharmaceutical and Biomedical Analysis, 176, 1–7. https://doi.org/10.1016/j.jpba.2019.112834
Culpepper, L., & Wingertzahn, M. A. (2015). Over-the-counter agents for the treatment of occasional disturbed sleep or transient insomnia: A systematic review of efficacy and safety. The Primary Care Companion for CNS Disorders, 17(6). https://doi.org/10.4088/PCC.15r01798
Darkovska-Serafimovska, M., Serafimovska, T., Arsova-Sarafinovska, Z., Stefanoski, S., Keskovski, Z., & Balkanov, T. (2018). Pharmacotherapeutic considerations for use of cannabinoids to relieve pain in patients with malignant diseases. Journal of Pain Research, 11, 837–842. https://doi.org/10.2147/JPR.S160556
de Sousa Lima, C. M., Fujishima, M. A. T., de Paula Lima, B., Mastroianni, P. C., de Sousa, F. F. O., & da Silva, J. O. (2020). Microbial contamination in herbal medicines: A serious health hazard to elderly consumers. BMC Complementary Medicine and Therapies, 20(1), 17.
Disch, L., Drewe, J., & Fricker, G. (2017). Dissolution testing of herbal medicines: Challenges and regulatory standards in Europe, the United States, Canada, and Asia. Dissolution Technologies, 24, 6–12.
https://doi.org/10.14227/DT240217P6
Durso, G. R. O., Luttrell, A., & Way, B. M. (2015). Over-the-counter relief from pains and pleasures alike: Acetaminophen blunts evaluation sensitivity to both negative and positive stimuli. Psychological Science, 26(6), 750–758. https://doi.org/10.1177/0956797615570366
Erland, L. A. E., & Saxena, P. K. (2017). Melatonin natural health products and supplements: Presence of serotonin and significant variability of melatonin content. Journal of Clinical Sleep Medicine, 13(2), 275–281. https://doi.org/10.5664/jcsm.6462
First, M. B. (2013). DSM-5® handbook of differential diagnosis. American Psychiatric Association.
Flynn, A., Lincoln, J., & Burke, M. (2016). Homicidality and psychosis caused by an over-the-counter performance-enhancing supplement containing dendrobium extract and L-dopa. Pharmacy & Therapeutics, 41(6), 381–384.
Foong, A.-L., Patel, T., Kellar, J., & Grindrod, K. A. (2018). The scoop on serotonin syndrome. Canadian Pharmacists Journal/Revue des Pharmaciens du Canada, 151(4), 233–239. https://doi.org/10.1177/1715163518779096
Freudenberg-Hua, Y., Kaufman, R., Alafris, A., Mittal, S., Kremen, N., & Jakobson, E. (2019). Medication nonadherence in the geriatric psychiatric population: Do seniors take their pills? In V. Fornari & I. Dancyger (Eds.), Psychiatric nonadherence: A solutions-based approach (pp. 81–99). Springer.
Gerace, E., Bakanova, S. P., Di Corcia, D., Salomone, A., & Vincenti, M. (2021). Determination of cannabinoids in urine, oral fluid and hair samples after repeated intake of CBD-rich cannabis by smoking. Forensic Science International, 318, 1–6. https://doi.org/10.1016/j.forsciint.2020.110561
Gibson, T. B., Ozminkowski, R. J., & Goetzel, R. Z. (2005). The effects of prescription drug cost sharing: A review of the evidence. The American Journal of Managed Care, 11(11), 730–740.
Gruenwald, J., Brendler, T., & Jaenicke, C. (2007). PDR for herbal medicines (4th ed.). Thomson Healthcare.
Gureje, O., Nortje, G., Makanjuola, V., Oladeji, B. D., Seedat, S., & Jenkins, R. (2015). The role of global traditional and complementary systems of medicine in the treatment of mental health disorders. The Lancet Psychiatry, 2(2), 168–177. https://doi.org/10.1016/S2215-0366(15)00013-9
Guzmán Gutierrez, S. L., Reyes Chilpa, R., & Bonilla Jaime, H. (2014). Medicinal plants for the treatment of “nervios”, anxiety, and depression in Mexican traditional medicine. Revista Brasileira de Farmacognosia, 24(5), 591–608. https://doi.org/10.1016/j.bjp.2014.10.007
Hashiguchi, M., Ohta, Y., Shimizu, M., Maruyama, J., & Mochizuki, M. (2015). Meta-analysis of the efficacy and safety of Ginkgo biloba extract for the treatment of dementia. Journal of Pharmaceutical Health Care and Sciences, 1(1), 1–12. https://doi.org/10.1186/s40780-015-0014-7
He, S.-M., Chan, E., & Zhou, S.-F. (2011). ADME properties of herbal medicines in humans: Evidence, challenges and strategies. Current Pharmaceutical Design, 17(4), 357–407. https://doi.org/10.2174/138161211795164194
Hellbom, E. (2006). Chlorpheniramine, selective serotonin-reuptake inhibitors (SSRIs) and over-the-counter (OTC) treatment. Medical Hypotheses, 66(4), 689–690. https://doi.org/10.1016/j.mehy.2005.12.006
Hendrickson, B. P., Shaikh, N., Occhiogrosso, M., & Penzner, J. B. (2016). Mania induced by Garcinia cambogia: A case series. The Primary Care Companion for CNS Disorders, 18(2). https://doi.org/10.4088/PCC.15l01890
Hoskins, D., & Padrón, E. (2018). The practice of Curanderismo: A qualititative study from the perspectives of Curandera/os. Journal of Latina/o Psychology, 6(2), 79–93. https://doi.org/10.1037/lat0000081
Ingersoll, R. E. (2005). Herbaceuticals: An overview for counselors. Journal of Counseling & Development, 83(4), 434–443. https://doi.org/10.1002/j.1556-6678.2005.tb00365.x
Ingersoll, R. E., & Rak, C. F. (2016). Psychopharmacology for mental health professionals: An integrative approach (2nd ed.). Cengage.
Julius, R. J., Novitsky, M. A., Jr., & Dubin, W. R. (2009). Medication adherence: A review of the literature and implications for clinical practice. Journal of Psychiatric Practice, 15(1), 34–44.
https://doi.org/10.1097/01.pra.0000344917.43780.77
Kaufman, D. W., Kelly, J. P., Rosenberg, L., Anderson, T. E., & Mitchell, A. A. (2002). Recent patterns of medication use in the ambulatory adult population of the United States: The Slone survey. JAMA, 287(3), 337–344. https://doi.org/10.1001/jama.287.3.337
Kaut, K. (2011). Psychopharmacology and mental health practice: An important alliance. Journal of Mental Health Counseling, 33(3), 196–222. https://doi.org/10.17744/mehc.33.3.u357803u508r4070
Kaut, K. P., & Dickinson, J. A. (2007). The mental health practitioner and psychopharmacology. Journal of Mental Health Counseling, 29(3), 204–225. https://doi.org/10.17744/mehc.29.3.t670636302771120
Kladar, N., Anačkov, G., Srđenović, B., Gavarić, N., Hitl, M., Salaj, N., Jeremić, K., Babović, S., & Božin, B. (2020). St. John’s wort herbal teas – Biological potential and chemometric approach to quality control. Plant Foods for Human Nutrition, 75, 390–395. https://doi.org/10.1007/s11130-020-00823-1
LaFrance, W. C., Lauterbach, E. C., Coffey, C. E., Salloway, S. P., Kaufer, D. I., Reeve, A., Royall, D. R., Aylward, E., Rummans, T. A., & Lovell, M. R. (2000). The use of herbal alternative medicines in neuropsychiatry: A report of the ANPA Committee on Research. The Journal of Neuropsychiatry and Clinical Neurosciences, 12(2), 177–192. https://doi.org/10.1176/appi.neuropsych.12.2.177
Liao, Z., Cheng, L., Li, X., Zhang, M., Wang, S., & Huo, R. (2020). Meta-analysis of Ginkgo biloba preparation for the treatment of Alzheimer’s disease. Clinical Neuropharmacology, 43(4), 93–99.
https://doi.org/10.1111/j.1468-1331.2006.01605.x
Liu, Y., Lund, J. A., Murch, S. J., & Brown, P. N. (2018). Single-lab validation for determination of kavalactones and flavokavains in Piper methysticum (Kava). Planta Medica, 84(16), 1213–1218.
https://doi.org/10.1055/a-0637-2400
Macneil, C. A., Hasty, M. K., Conus, P., & Berk, M. (2012). Is diagnosis enough to guide interventions in mental health? Using case formulation in clinical practice. BMC Medicine, 10, Article 111.
https://doi.org/10.1186/1741-7015-10-111
Makaryus, A. N., & Friedman, E. A. (2005). Patients’ understanding of their treatment plans and diagnosis at discharge. Mayo Clinic Proceedings, 80(8), 991–994. https://doi.org/10.4065/80.8.991
Millar, S. A., Stone, N. L., Bellman, Z. D., Yates, A. S., England, T. J., & O’Sullivan, S. E. (2019). A systematic review of cannabidiol dosing in clinical populations. British Journal of Clinical Pharmacology, 85(9), 1888–1900. https://doi.org/10.1111/bcp.14038
Mischkowski, D., Crocker, J., & Way, B. M. (2016). From painkiller to empathy killer: Acetaminophen (paracetamol) reduces empathy for pain. Social Cognitive and Affective Neuroscience, 11(9), 1345–1353. https://doi.org/10.1093/scan/nsw057
Mischkowski, D., Crocker, J., & Way, B. M. (2019). A social analgesic? Acetaminophen (paracetamol) reduces positive empathy. Frontiers in Psychology, 10, 538. https://doi.org/10.3389/fpsyg.2019.00538
Mischoulon, D., & Fava, M. (2002). Role of S-adenosyl-L-methionine in the treatment of depression: A review of the evidence. The American Journal of Clinical Nutrition, 76(5), 1158–1161. https://doi.org/10.1093/ajcn/76.5.1158S
Modoux, M., Rolhion, N., Mani, S., & Sokol, H. (2020). Tryptophan metabolism as a pharmacological target. Trends in Pharmacological Sciences, 42(1), 60–73. https://doi.org/10.1016/j.tips.2020.11.006
Mulyawan, E., Ahmad, M. R., Islam, A. A., Massi, M. N., Hatta, M., & Arif, S. K. (2020). Analysis of GABRB3 protein level after administration of valerian extract (Valeriana officinalis) in BALB/c mice. Pharmacognosy Journal, 12(4), 821–827. https://doi.org/10.5530/pj.2020.12.118
Murray, C. E., & Murray, T. L., Jr. (2007). The family pharm: An ethical consideration of psychopharmacology in couple and family counseling. The Family Journal, 15(1), 65–71. https://doi.org/10.1177/1066480706294123
Nahin, R. L., Barnes, P. M., Stussman, B. J., & Bloom, B. (2009). Costs of complementary and alternative medicine (CAM) and frequency of visits to CAM practitioners: United States, 2007. National Health Statistics Reports, 18, 1–14. https://stacks.cdc.gov/view/cdc/11548
National Institute of Mental Health. (2019). Prevalence of any mental illness (AMI). https://www.nimh.nih.gov/health/statistics/mental-illness.shtml
Newmaster, S. G., Grguric, M., Shanmughanandhan, D., Ramalingam, S., & Ragupathy, S. (2013). DNA barcoding detects contamination and substitution in North American herbal products. BMC Medicine, 11(1), 222. https://doi.org/10.1186/1741-7015-11-222
Ng, C. H., & Bousman, C. A. (2018). Cross-cultural psychopharmacotherapy. In D. Bhugra & K. Bhui (Eds.), Textbook of cultural psychiatry (2nd ed., pp. 432–441). Cambridge University Press.
Ng, Q. X., Venkatanarayanan, N., & Ho, C. Y. X. (2017). Clinical use of Hypericum perforatum (St John’s wort) in depression: A meta-analysis. Journal of Affective Disorders, 210, 211–221.
https://doi.org/10.1016/j.jad.2016.12.048
Olsufka, W., & Abraham, M.-A. (2017). Treatment-emergent hypomania possibly associated with over-the-counter supplements. Mental Health Clinician, 7(4), 160–163. https://doi.org/10.9740/mhc.2017.07.160
Pantano, F., Tittarelli, R., Mannocchi, G., Zaami, S., Ricci, S., Giorgetti, R., Terranova, D., Busardò, F. P., & Marinelli, E. (2016). Hepatotoxicity induced by “the 3Ks”: Kava, kratom and khat. International Journal of Molecular Sciences, 17(4), 580. https://doi.org/10.3390/ijms17040580
Papakostas, G. I. (2009). Evidence for S-adenosyl-L-methionine (SAM-e) for the treatment of major depressive disorder. The Journal of Clinical Psychiatry, 70(Suppl. 5), 18–22. https://doi.org/10.4088/JCP.8157su1c.04
Perry, P. J., Alexander, B., Liskow, B. I., & DeVane, C. L. (2006). Psychotropic drug handbook (8th ed.). Lippincott Williams & Wilkins.
Phillips, L. A., Cohen, J., Burns, E., Abrams, J., & Renninger, S. (2016). Self-management of chronic illness: The role of ‘habit’ versus reflective factors in exercise and medication adherence. Journal of Behavioral Medicine, 39(6), 1076–1091. https://doi.org/10.1007/s10865-016-9732-z
Posadzki, P., Watson, L., & Ernst, E. (2013). Contamination and adulteration of herbal medicinal products (HMPs): An overview of systematic reviews. European Journal of Clinical Pharmacology, 69(3), 295–307. https://doi.org/10.1007/s00228-012-1353-z
Preston, J. D., O’Neal, J. H., Talaga, M. C., & Moore, B. A. (2021). Handbook of clinical psychopharmacology for therapists (9th ed.). New Harbinger.
PR Newswire. (n.d.). Global over-the-counter drug markets hit $80.2 billion in 2017: Report. https://www.prnewswire.com/news-releases/global-over-the-counter-drug-markets-hit-802-billion-in-2017-report-300588867.html
Professional Counselors, 22 Texas Administrative Code § 681.83 (2021). https://texreg.sos.state.tx.us/public/readtac$ext.ViewTAC?tac_view=5&ti=22&pt=30&ch=681&sch=C&rl=Y
Rashrash, M., Schommer, J. C., & Brown, L. M. (2017). Prevalence and predictors of herbal medicine use among adults in the United States. Journal of Patient Experience, 4(3), 108–113.
https://doi.org/10.1177/2374373517706612
Ravina, E. (2011). The evolution of drug discovery: From traditional medicines to modern drugs. Wiley.
Ravven, S. E., Zimmerman, M. B., Schultz, S. K., & Wallace, R. B. (2011). 12-month herbal medicine use for mental health from the National Comorbidity Survey Replication (NCS-R). Annals of Clinical Psychiatry, 23(2), 83–94.
Sakurai, H., Carpenter, L. L., Tyrka, A. R., Price, L. H., Papakostas, G. I., Dording, C. M., Yeung, A. S., Cusin, C., Ludington, E., Bernard-Negron, R., Fava, M., & Mischoulon, D. (2020). Dose increase of S-adenosyl-methionine and escitalopram in a randomized clinical trial for major depressive disorder. Journal of Affective Disorders, 262, 118–125. https://doi.org/10.1016/j.jad.2019.10.040
Saran, J. S., Barbano, R. L., Schult, R., Wiegand, T. J., & Selioutski, O. (2017). Chronic diphenhydramine abuse and withdrawal: A diagnostic challenge. Neurology: Clinical Practice, 7(5), 439–441.
https://doi.org/10.1212/CPJ.0000000000000304
Sarris, J. (2007). Herbal medicines in the treatment of psychiatric disorders: A systematic review. Phytotherapy Research, 21(8), 703–716. https://doi.org/10.1002/ptr.2187
Sarris, J. (2018). Herbal medicines in the treatment of psychiatric disorders: 10-year updated review. Phytotherapy Research, 32(7), 1147–1162. https://doi.org/10.1002/ptr.6055
Savage, K., Firth, J., Stough, C., & Sarris, J. (2018). GABA-modulating phytomedicines for anxiety: A systematic review of preclinical and clinical evidence. Phytotherapy Research, 32(1), 3–18.
https://doi.org/10.1002/ptr.5940
Savage, R. A., Basnet, S., & Miller, J. M. (2020). Melatonin. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK534823
Scotton, W. J., Hill, L. J., Williams, A. C., & Barnes, N. M. (2019). Serotonin syndrome: Pathophysiology, clinical features, management, and potential future directions. International Journal of Tryptophan Research, 12, 1–14. https://doi.org/10.1177/1178646919873925
Sepulveda, V. I., Piazza, N. J., Devlin, M., Ritchie, M. H., Salyers, K., & Tucker-Gail, K. (2016). Psychopharmacology in counseling, psychology, and social work education: An interdisciplinary history and implications for professional counselors. Wisconsin Counseling Association Journal, 29, 35–48.
Sharma, V., Madaan, R., Bala, R., Goyal, A., & Sindhu, R. K. (2021). Pharmacodynamic and pharmacokinetic interactions of herbs with prescribed drugs: A review. Plant Archives, 21(1), 185–198.
https://doi.org/10.51470/PLANTARCHIVES.2021.v21.S1.033
Shinjyo, N., Waddell, G., & Green, J. (2020). Valerian root in treating sleep problems and associated disorders—A systematic review and meta-analysis. Journal of Evidence-Based Integrative Medicine, 25, 1–31.
https://doi.org/10.1177/2515690X20967323
Sidhu, G., & Marwaha, R. (2021). Phenelzine. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK554508
Singh, P., Srivastava, B., Kumar, A., & Dubey, N. K. (2008). Fungal contamination of raw materials of some herbal drugs and recommendation of Cinnamomum camphora oil as herbal fungitoxicant. Microbial Ecology, 56(3), 555–560. https://doi.org/10.1007/s00248-008-9375-x
Singh, S. K., Srivastav, S., Castellani, R. J., Plascencia-Villa, G., & Perry, G. (2019). Neuroprotective and antioxidant effect of Ginkgo biloba extract against AD and other neurological disorders. Neurotherapeutics, 16(3), 666–674. https://doi.org/10.1007/s13311-019-00767-8
Smith, T., Kawa, K., Eckl, V., Morton, C., & Stredney, R. (2017). Herbal supplement sales in US increase 7.7% in 2016: Consumer preferences shifting toward ingredients with general wellness benefits, driving growth of adaptogens and digestive health products. HerbalGram, 115, 56–65. https://www.herbalgram.org/media/15603/hg115-mktrpt.pdf
Solas, M., Puerta, E., & Ramirez, M. J. (2015). Treatment options in Alzheimer’s disease: The GABA story. Current Pharmaceutical Design, 21(34), 4960–4971. https://doi.org/10.2174/1381612821666150914121149
Spindle, T. R., Cone, E. J., Kuntz, D., Mitchell, J. M., Bigelow, G. E., Flegel, R., & Vandrey, R. (2020). Urinary pharmacokinetic profile of cannabinoids following administration of vaporized and oral cannabidiol and vaporized CBD-dominant cannabis. Journal of Analytical Toxicology, 44(2), 109–125.
https://doi.org/10.1093/jat/bkz080
Stahl, S. M. (2021). Stahl’s essential psychopharmacology: Neuroscientific basis and practical applications (5th ed.). Cambridge University Press.
Surana, A. R., Agrawal, S. P., Kumbhare, M. R., & Gaikwad, S. B. (2021). Current perspectives in herbal and conventional drug interactions based on clinical manifestations. Future Journal of Pharmaceutical Sciences, 7(1), 1–12. https://doi.org/10.1186/s43094-021-00256-w
Tallarida, R. J. (2007). Interactions between drugs and occupied receptors. Pharmacology & Therapeutics, 113(1), 197–209. https://doi.org/10.1016/j.pharmthera.2006.08.002
Tran, T., & Kavuluru, R. (2020). Social media surveillance for perceived therapeutic effects of cannabidiol (CBD) products. International Journal of Drug Policy, 77, 1–7. https://doi.org/10.1016/j.drugpo.2020.102688
U.S. Census Bureau. (2020). Quick facts [Table]. https://www.census.gov/quickfacts/fact/table/US/PST045219
U.S. Food & Drug Administration. (2015). FDA 101: Dietary supplements. https://www.fda.gov/consumers/consumer-updates/fda-101-dietary-supplements
U.S. Food & Drug Administration. (2020a). FDA approves new indication for drug containing an active ingredient derived from cannabis to treat seizures in rare genetic disease. https://www.fda.gov/news-events/press-announcements/fda-approves-new-indication-drug-containing-active-ingredient-derived-cannabis-treat-seizures-rare
U.S. Food & Drug Administration. (2020b). What you need to know (and what we’re working to find out) about products containing cannabis or cannabis-derived compounds, including CBD. https://www.fda.gov/consumers/consumer-updates/what-you-need-know-and-what-were-working-find-out-about-products-containing-cannabis-or-cannabis
Wang, C.-C., Kennedy, J., & Wu, C.-H. (2015). Alternative therapies as a substitute for costly prescription medications: Results from the 2011 National Health Interview Survey. Clinical Therapeutics, 37(5), 1022–1030. https://doi.org/10.1016/j.clinthera.2015.01.014
Wolf, M. S., King, J., Jacobson, K., Di Francesco, L., Bailey, S. C., Mullen, R., McCarthy, D., Serper, M., Davis, T. C., & Parker, R. M. (2012). Risk of unintentional overdose with non-prescription acetaminophen products. Journal of General Internal Medicine, 27(12), 1587–1593. https://doi.org/10.1007/s11606-012-2096-3
Wong, M. K., Darvishzadeh, A., Maler, N. A., & Bota, R. G. (2016). Five supplements and multiple psychotic symptoms: A case report. The Primary Care Companion for CNS Disorders, 18(1).
https://doi.org/10.4088/PCC.15br01856
Wu, C.-H., Wang, C.-C., & Kennedy, J. (2011). Changes in herb and dietary supplement use in the US adult population: A comparison of the 2002 and 2007 National Health Interview Surveys. Clinical Therapeutics, 33(11), 1749–1758. https://doi.org/10.1016/j.clinthera.2011.09.024
Zirak, N., Shafiee, M., Soltani, G., Mirzaei, M., & Sahebkar, A. (2019). Hypericum perforatum in the treatment of psychiatric and neurodegenerative disorders: Current evidence and potential mechanisms of action. Journal of Cellular Physiology, 234(6), 8496–8508. https://doi.org/10.1002/jcp.27781
Sabina Remmers de Vries, PhD, NCC, LPC-S, is an associate professor at Texas A&M University–San Antonio. Christine D. Gonzales-Wong, PhD, NCC, LPC, is an assistant professor at Texas A&M University–San Antonio. Correspondence may be addressed to Sabina de Vries, One University Way, San Antonio, TX 78224, sabina.devries@tamusa.edu.
Aug 10, 2022 | Volume 12 - Issue 2
Phillip L. Waalkes, Daniel A. DeCino, Maribeth F. Jorgensen, Tiffany Somerville
Supportive relationships with counselor educators as dissertation chairs are valuable to doctoral students overcoming barriers to successful completion of their dissertations. Yet, few have examined the complex and mutually influenced dissertation-chairing relationships from the perspective of dissertation chairs. Using hermeneutic phenomenology, we interviewed counselor educators (N = 15) to identify how they experienced dissertation-chairing relationship dynamics with doctoral students. Counselor educators experienced relationships characterized by expansive connections, growth in student autonomy, authenticity, safety and trust, and adaptation to student needs. They viewed chairing relationships as fluid and non-compartmentalized, which cultivated mutual learning and existential fulfillment. Our findings provide counselor educators with examples of how empathy and encouragement may help doctoral students overcome insecurities and how authentic and honest conversations may help doctoral students overcome roadblocks. Counselor education programs can apply these findings by building structures to help facilitate safe and trusting relationships between doctoral students and counselor educators.
Keywords: dissertation-chairing relationships, hermeneutic phenomenology, counselor education, doctoral students, relationship dynamics
According to the Council for Accreditation of Counseling and Related Educational Programs (CACREP; 2015), doctoral students must develop research skills and complete counseling-focused dissertation research. Research mentorship is often important to counselor education doctoral students’ development as researchers (Flynn et al., 2012; Lamar & Helm, 2017; Neale-McFall & Ward, 2015). One of the central research mentoring relationships in doctoral programs is the dissertation-chairing relationship. Supportive research mentoring relationships in counselor education are invaluable to students (Lamar & Helm, 2017), are necessary to successful dissertation chairing (Ghoston et al., 2020; Jorgensen & Wester, 2020), and are a central factor in high-quality doctoral programs (Preston et al., 2020). In fact, a meaningful connection between students and their dissertation chairperson predicts students’ successful completion of their dissertations (Neale-McFall & Ward, 2015; Rigler et al., 2017) and positive dissertation experiences (Burkard et al., 2014). Therefore, to help promote intentional and supportive dissertation-chairing relationships, we examined counselor educators’ experiences of relationship dynamics with doctoral students.
Challenges in Dissertation Completion
Across disciplines, doctoral students can struggle with isolation, motivation, time management, self-regulation, and self-efficacy (Pyhältö et al., 2012). In their development as researchers, doctoral students in counselor education can experience intense emotions, including excitement, exhaustion, frustration, distrust, confusion, disconnection, and pride (Lamar & Helm, 2017). Negative relationships with dissertation chairs can exacerbate challenges to dissertation completion. In one meta-analysis study examining doctoral student attrition across disciplines, doctoral students identified a problematic relationship with their dissertation chairperson as the most significant barrier to their completion of their degrees (Rigler et al., 2017). Doctoral students in counselor education have reported negative experiences when their dissertation chairs were unenthusiastic, unsupportive, and unavailable, and when their guidance was not concrete (Flynn et al., 2012; Lamar & Helm, 2017). In addition, counselor education doctoral students involved in negative dissertation-chairing relationships can feel like they are on their own in their dissertation journeys (Protivnak & Foss, 2009). This feeling of isolation can intensify existing barriers in completing dissertations, including struggles with motivation, self-regulation, self-criticism, and self-efficacy (Burkard et al., 2014; Pyhältö et al., 2012).
Power differentials between doctoral students and dissertation chairs also can serve as a barrier to supportive dissertation-chairing relationships and dissertation completion (Burkard et al., 2014). For example, doctoral students are likely to remain silent in difficult relationships with dissertation chairs unless students perceive there to be a strong relationship built on respect and open communication (Schlosser et al., 2003). Cultural differences and systemic oppression may also impact dissertation-chairing relationships. According to Brown and Grothaus (2019), Black counselor education students can experience overt racism, tokenism, isolation, and internalized racism, which can foster mistrust in cross-racial mentoring relationships. Numerous researchers in counselor education (Borders et al., 2012; Ghoston et al., 2020; Neale-McFall & Ward, 2015; Purgason et al., 2018) have recommended mentors use transparent and honest dialogue with explicit attention to expectations, power dynamics, cultural differences, and potential conflicts.
Supportive Dissertation-Chairing Relationships
Dissertation-chairing relationships with individualized supports can help students overcome barriers to completing their dissertations (Ghoston et al., 2020; Purgason et al., 2018). According to Flynn and colleagues (2012), increased dissertation chairperson involvement can counteract counselor education students’ isolation, burnout, and perceptions of lacking support. Dissertation chairs can help doctoral students identify their low research self-efficacy and offer support, encouragement, and instruction to help address it (Burkard et al., 2014). According to Ghoston and colleagues (2020), a supportive relationship during the dissertation process can help doctoral students be more honest about when they are stuck, which, in turn, allows chairs to give more targeted direction and feedback.
Beginning counselor educators have reported faculty mentoring, care, and support were the most valuable components of their doctoral training (Perera-Diltz & Sauerheber, 2017). Specifically, doctoral students in counselor education value when faculty take time with them, express genuine caring, offer guidance, validate and believe in them, and celebrate their efforts and achievements (Neale-McFall & Ward, 2015; Protivnak & Foss, 2009; Purgason et al., 2018). Counselor education doctoral students also appreciate dissertation chairs who offer regular contact, timely support, and clear and authentic communication (Borders et al., 2012; Ghoston et al., 2020; Jorgensen & Wester, 2020).
Despite the importance of supportive dissertation-chairing relationships in counselor education (Flynn et al., 2012; Jorgensen & Wester, 2020; Neale-McFall & Ward, 2015), little research exists on how counselor educators experience dissertation-chairing relationships with doctoral students. Although researchers have studied dissertation-chairing relationships from the perspectives of counselor education doctoral students (e.g., Flynn et al., 2012; Lamar & Helm, 2017; Neale-McFall & Ward, 2015) and examined relational strategies counselor educators use (e.g., Ghoston et al., 2020; Jorgensen & Wester, 2020), few have examined counselor educators’ perceptions of the relationship as dynamic and mutually constructed. Given their role as faculty and their experiences in multiple dissertation-chairing relationships, dissertation chairs may have more awareness of and broader perspectives on the mutually influenced dissertation relationship and process. Understanding the complexities and nuances of dynamics in chairing relationships may help counselor educators develop more intentional dissertation-chairing practices, subsequently resulting in more successfully completed dissertations. Therefore, we asked the following research question in this hermeneutic phenomenological investigation: What are counselor educators’ lived experiences of dissertation-chairing relationship dynamics with doctoral students?
Method
We utilized a hermeneutic perspective rooted in an interpretive paradigm to guide this study. This perspective aligns with the focus on relationships in our study and emphasizes how individuals make meaning in interaction with others (Heidegger, 1962). Anchored by the viewpoint that all knowledge is relative and based on cultural context, Heidegger’s (1962) hermeneutic phenomenology helped us to construct an evocative description of the essence of participants’ experiences of chairing dissertations in a multi-dimensional and multi-layered way (van Manen, 1990). Hermeneutic phenomenology focuses on uncovering the participants’ experiences of the lifeworld, or their experience of everyday situations and relations (van Manen, 1990). The concept of lifeworld in hermeneutic phenomenology allowed us to examine participants’ lived experiences of human relation, or how they maintain relationships in shared interpersonal space. Therefore, we utilized hermeneutic phenomenology (van Manen, 1990) to investigate counselor educators’ experiences of dissertation-chairing relationships.
Participants and Sampling Procedure
Of 15 participants in our study, eight self-identified as female and seven self-identified as male. Ten participants self-identified as White. Three self-identified with multiple racial and ethnic groups, and two self-identified as African American or Black. Seven participants worked as an associate professor, seven participants worked as a full professor, and one participant worked as an assistant professor. Participants’ ages ranged from 33 to 68 (M = 47.93, SD = 10.18). Years of experience working as a counselor educator ranged from 4 to 29 (M = 16.40, SD = 7.92). Participants reported a wide range of successful chairing experiences, with one to 40 (M = 10.47, SD = 10.39) of their doctoral student advisees defending their dissertations. Nine participants worked at institutions in the Southern Association for Counselor Education and Supervision (ACES) region, three participants worked at institutions in the Western ACES region, two participants worked at institutions in the North Central ACES region, and one participant worked at an institution in the Northeastern ACES region. Five participants worked at institutions with an R2 Carnegie classification (doctoral universities with high research activity). Five participants worked at institutions with an R1 Carnegie classification (doctoral universities with very high research activity). Three participants worked at institutions with an M1 Carnegie classification (master’s colleges and universities with larger programs). Two participants worked at an institution with a D/PU classification (doctoral/professional universities).
Participants qualified for inclusion in this study if they self-identified as a counselor educator working in a CACREP-accredited program and had chaired at least one counseling doctoral student through a successful dissertation defense. After compiling a list of all CACREP-accredited counselor education doctoral programs (N = 33) from information available through the CACREP website, we created a list of names and email addresses of all counselor education faculty (N = 330) working at each of these institutions based on information available on programs’ websites. After receiving IRB approval, we randomly selected 249 faculty members from this list and sent each person a recruitment email and one follow-up email about a week later. Fifteen counselor educators expressed interest, yielding a response rate of 6.05%.
Data Collection
After counselor educators expressed interest in the study, we emailed them a brief demographic data survey, the informed consent document, and the interview questions. We scheduled a time for a semi-structured interview with them and asked them to return their demographic data survey before their interviews. All interviews were conducted through Zoom and audio recorded. The interview protocol consisted of six main open-ended questions and two to four scripted probes for each main question (Patton, 2014). We developed interview questions based on themes within the literature on dissertations and research mentorship (e.g., Flynn et al., 2012; Jorgensen & Wester, 2020; Neale-McFall & Ward, 2015) as well as our own experiences chairing dissertations. Sample interview questions included “How would you describe the characteristics of relationships you want to foster with students?” and “What relational factors help students successfully complete their dissertations with you as a dissertation chair?” Interviews lasted between 38 and 64 minutes. After transcribing the interviews using Rev.com, we deleted the audio files. We determined that we reached saturation at our sample size of 15 participants as we observed the same themes repeatedly emerging in our coding process (Patton, 2014).
Research Team
Our research team consisted of four members. Phillip Waalkes and Daniel DeCino served as the coding team. They both identify as White cisgender male counselor educators with experience chairing dissertations. Maribeth Jorgensen and Tiffany Somerville served as auditors. Jorgensen identifies as a White cisgender female counselor educator with experience chairing dissertations, while Somerville identifies as a White cisgender female counselor education doctoral student. Waalkes, DeCino, and Jorgensen developed the study after a conversation of their experiences chairing dissertations and conducting research in this topic area. We identified how we grew in our identities as dissertation chairs and how we adapted our mentoring styles to meet the needs of students. Considering our experiences as dissertation chairs and doctoral students, we wanted to know how counselor educators developed supportive dissertation-chairing relationships.
To promote reflexivity, the coding team, Waalkes and DeCino, used bridling throughout the data analysis process, utilizing written statements and discussion. Bridling is a process in which researchers actively wait for the phenomenon and its meaning to show itself while also scrutinizing their own involvement with the phenomenon. Bridling requires researchers to acknowledge their pre-understandings and loosen them to allow space for holistic understanding of the phenomenon without seeking to understand too quickly or too carelessly (Dahlberg, 2006). In his reflexivity statement, Waalkes wrote about the importance of timely and individualized feedback and the challenges of building relationships when taking over as dissertation chairperson in the middle of a student’s dissertation process. DeCino discussed his beliefs about the importance of individualized mentoring relationships and the impact of his dissertation experience as a doctoral student on his current dissertation-chairing identity. These reflexive conversations continued between Waalkes and DeCino throughout the data analysis process.
Data Analysis
Based on van Manen’s (1990) inductive data analysis procedure for hermeneutic phenomenology, we coded our data with hermeneutic awareness, reflecting on the data in multidimensional context as opposed to accepting it at face value. Additionally, we designed our procedure to create a hermeneutic circle by shifting between examining parts of the text and reflecting on the interviews as a whole (van Manen, 1990). The development of a thematic structure and a holistic statement (a one-sentence summary of the essence of each participant’s experience) as products of our data analysis reflect our hermeneutic circle.
Our data analysis process consisted of four stages. First, for each interview, Waalkes and DeCino individually created initial holistic statements for each participant. Holistic statements summarized the central significance or fundamental meaning of the participant’s transcript (i.e., text) as a whole. For example, Participant 6’s holistic statement was “Structure, organization, following rules, empathy, scheduled standing meetings to check in personally and professionally, and constructive feedback tailored to students’ needs with an awareness of cultural differences are essential to their dissertation-chairing relationships.” Then, they met to discuss their individual holistic statements and reach consensus on the content of each holistic statement. Second, they individually reviewed each transcript and highlighted essential passages throughout each transcript. Waalkes and DeCino selected passages that were particularly essential or revealing (van Manen, 1990). After selecting a passage, they rewrote it with attention to the context of what was below or above each highlighted section. After rewriting a passage, they reviewed the participants’ holistic statement to ensure that the rewritten passage reflected the interview as a whole. They combined their summary statements of essential passages into a shared spreadsheet. Third, in a series of meetings, Waalkes and DeCino discussed their summary statements and coded each one with a possible theme name. Afterward, they looked for frequently reoccurring codes and combined similar codes to create an initial theme list. Then, they checked that their themes were essential and not incidental by assessing them against the holistic statements and using imaginative variation by asking: “Is this phenomenon still the same if we imaginatively change or delete this theme from the phenomenon?” (van Manen, 1990, p. 107). In conversation, Waalkes and DeCino revised the theme list and structure throughout the imaginative variation process. Finally, Jorgensen and Somerville reviewed the theme list and the holistic statements and offered suggestions that helped refine them.
Trustworthiness
We established trustworthiness in the present study through an iterative data analysis process with hermeneutic awareness and a hermeneutic circle, triangulation of investigators, and bridling through reflexive journaling (Dahlberg, 2006; Hays & Singh, 2012). First, our iterative data analysis process promoted hermeneutic awareness and helped us achieve a hermeneutic circle in checking our thematic structure and our holistic statements compared to each other (van Manen, 1990). Reflecting on the data in context involved approaching the data with an awareness that meaning is never simple or one-dimensional but rather multidimensional and multilayered (van Manen, 1990). To do this, we used individual and consensus coding, evaluation of the data in holistic context using holistic statements, and imaginative variation to summarize only essential parts of participants’ experiences (van Manen, 1990). Second, to achieve triangulation of investigators, Waalkes and DeCino reached consensus throughout the data analysis process (Hays & Singh, 2012). We also utilized two external auditors who read the interview transcripts and provided feedback on our thematic structure and holistic statements. Third, we engaged in reflexive journaling and bridling as described in the research team section above.
Findings
We arranged our findings into five themes: (a) expansive connections, (b) growth in student autonomy, (c) authenticity, (d) safety and trust, and (e) adaptation to student needs. We arrived at these five themes by using imaginative variation to determine which of our themes were essential to participants’ experiences. Each theme is described in the sections below.
Expansive Connections
In the expansive connections theme, participants (n = 11) described how chairing relationships defy compartmentalized definitions and can have wide-ranging and mutually beneficial impacts that extend beyond the dissertation project. For example, Participant 15 offered herself “as a person” to students:
When you sign on to . . . work with me on a dissertation, you don’t just get my technical expertise, you get me as a person . . . and that’s what you get first, actually. So again, it’s not a relationship that’s contained in a box. Hopefully, this is something that grows and actually is something we both are learning from and continues to sustain.
Similarly, Participant 9’s relationships with students extended beyond discussions of dissertations:
I try to talk to [the students I chair] about personal stuff as well as just the dissertation stuff. Because it’s not little neat cubby holes that they put their lives in. What’s going on in their personal life is what’s impacting their progress towards completion. Sometimes it’s just a sigh [of] relief when I ask them “How’s your wife doing? Is the baby walking?” And it gives them a chance to just decompress for a moment and regroup.
Participant 5 described a mutuality in learning through an intense working relationship:
It’s not really a top-down thing, but it’s about learning a craft, and intensely working together to learn that craft . . . it’s a formative process. We’re learning about ourselves as we’re going through it. And I learn from my students as well, while I’m chairing their projects . . . this is a career-building, life-extending experience.
Growth in Student Autonomy
Participants (n = 8) described the importance of using the dissertation relationship to help students take initiative and learn to conduct research on their own. Often participants set clear expectations and boundaries in their relationships to help students do this. For example, Participant 9 encouraged students to take accountability over maintaining momentum in the working alliance:
The student has to recognize this as a partnership, and I can’t react until the student acts. So to me, if I don’t see any action taking place, it’s much more difficult to give you feedback, to give you some kind of response. So that working alliance, I keep pushing that to a student. “What’s your responsibility. What’s my responsibility?”
Participant 2 talked about how he wanted students to be autonomous in planning their dissertations while offering resources:
I’m not the timekeeper. I’m not the helicopter parent. . . . “This is your dissertation, right? This is . . . your life. I will help get you resources, figure out what you need to do to get it done, you know? Beg, buy, borrow, and steal resources to get it done, but you gotta come to me with that.” I’m not gonna say, “Okay, you’re done with stuff a. Stuff b is this. Here’s what you need to do.”
Participant 8 did not want to micromanage students even if students expected that of her:
I don’t want to be your mother. . . he’s like this helpless person. So, I was a little worried that he was continuing to perpetuate these types of dynamics in his life where he was looking for maybe strong women to just come in and take care of things for him . . . I’ve had to be really, really clear about that.
Authenticity
In the authenticity theme, nearly all participants (n = 13) described valuing genuine conversations with students, in which there was a mutuality in sharing vulnerable parts of themselves. These conversations involved discussing both parties’ roles and responsibilities in the relationship. Participants co-constructed the dissertation process by inviting students into honest discussions of the abilities of both parties. For example, Participant 3 described facilitating authentic conversations:
It’s not a one-size-fits-all model . . . every student is different and . . . the process of having the conversation about what they need is a really good relationship-building conversation. And I’m quick to say, “There may be things you want that I can’t provide,” just because I don’t have this skill set or the capacity or the bandwidth in a given day . . . just having those conversations that start that co-constructed collaborative process and empowering them to do their work.
Additionally, participants transparently revealed vulnerable parts about themselves to help students overcome anxiety or other challenges. For example, Participant 12 described the importance of mutual authenticity to facilitate using immediacy to address issues that were causing students to get stuck:
I really need to be able to call out what I see if [the student] may be stuck . . . there needs to be that mutual authentic exchange too . . . authentic relating is my really being able [to feel] like there’s someone for me to call out when I noticed there might be something obstructing [the student’s] capacity to keep moving forward.
Participant 7 viewed being humble and inviting students to share their knowledge as part of being genuine:
I mentioned having that mutual learning attitude and when you do that, that’s being open and honest and genuine with them. Not acting like you know everything. I may be perceived as an expert in some areas, but I don’t want to come off that way actually sometimes. I’ve done a lot of this stuff, but I’m not an expert on this particular area. Tell me what you know. Tell me what you think you know. Tell me what you don’t know that you want to do and I will help you try to get there.
Safety and Trust
In the safety and trust theme, participants (n = 10) discussed how trust and safety served as the foundation for their chairing relationships. Participants acknowledged how mutual trust deepened their connections and helped students feel like their chairperson would help them grow without leaving them floundering. Participants believed safety and trust helped assure students they were going to complete their dissertation and they were not going to be abandoned. For example, Participant 7 discussed the importance of students’ trusting her to offer consistent support:
[Students should] trust me that we can work collaboratively together to make it a good study, that I have the background or I know where to get [help], if you don’t as a student, to help figure out methodology, how to write that prospectus, how to write period. . . . You have to trust me to know how to do that or at least have the resources to help you figure it out, and to trust me that we’re going to be in this together. I’m not going to leave you hanging.
Numerous participants conceptualized students’ needs for safety in terms of expressing and processing strong and often hidden emotions. For example, Participant 5 discussed how students coped with their vulnerability and shame of not feeling good enough:
They need to feel safe . . . I think there’s a lot of shame that goes into developing as a student and maybe even overt or covert. It’s just really tough. It’s such a vulnerable time in your life. I think that doc students, when you get them into groups, they just are very sure and confident. . . . I think that’s such a defensive mechanism to kind of bolster themselves and to kind of propel themselves forward because they’re really trying to, at times, step into these very big roles.
Similarly, Participant 3 conceptualized safety in terms of helping students of color feel like they could make mistakes with him as they navigate biased academic systems:
I really try to bring my years of experience, but I also try to diminish the hierarchy as much as I can. So we have conversations about why we might go this way or why we might go that way rather than it being an edict from me. And I think students appreciate that. I think they feel respected. I think they feel valued. One of the things that I feel very grateful for is that I’ve had the opportunity to have a lot of students of color select me as their dissertation chair. . . . And I think part of that, as they navigate a system that’s still kind of incredibly White and largely biased . . . they feel safe . . . it’s safe to make mistakes . . . They’re going to hand in some versions of drafts that are just not very good. And that’s part of the learning process.
Adaptation to Student Needs
In the adaptation to student needs theme, participants (n = 12) discussed assessing their students’ personalities and tailoring their approaches to meet unique student needs with a mix of support and challenge. For example, Participant 3 described making adjustments based on students’ levels of self-efficacy:
There are some students that I think have a lot of self-efficacy and don’t want me to sugar-coat anything. I can just be very direct and they want me to be direct. They tell me they want me to be direct, but I also recognize for some students, what they’re going to respond better to is more a carrot, less stick. And so, even how I language a comment or something, I’m paying attention to that based on my sense of the student and what they can navigate. If I have a draft of something that it feels like I’ve kind of bled all over and I’ve done a real hatchet job on . . . I’m going to make sure that in the body of the email . . . I’m encouraging.
Similarly, Participant 4 discussed how she personalized encouragement based on students’ needs:
I think of a student I had who needed a lot of validation in the moment, of, “Hey, you’re doing really well. You have all these strengths. These are all the things you’re doing well and I know you can do this. I believe in you.” And then, for others, I know that they needed to sit in the stress or the disappointment a little bit. So to say like, “I hear you. You are struggling right now and I’m going to give you the space for that. And when you’re ready, I’ve got a lot of positive things to say about you. So you let me know when you’re ready for that feedback. It doesn’t sound like you’re ready for it right now.”
Discussion
Because developing as researchers is important for doctoral students (CACREP, 2015) and research mentorship is critical for this purpose (Flynn et al., 2012; Lamar & Helm, 2017; Neale-McFall & Ward, 2015), we investigated counselor educators’ experiences of relationship dynamics with doctoral students when chairing dissertations. Participants reported the complex and mutually influenced dynamics of expansive connections, growth in student autonomy, authenticity, safety and trust, and adaptation to student needs. Our finding of dissertation-chairing relationship dynamics as wide-reaching broadens the focus of previous researchers who have explored these relationships in terms of a series of strategies used by the chairperson (Ghoston et al., 2020) or a list of components contributing to successful dissertation completion (Jorgensen & Wester, 2020). Participants viewed chairing relationships as fluid, mutually influenced, and non-compartmentalized (Purgason et al., 2016), involving a blending of personal and collegial connection that could offer shared learning and fulfillment. Numerous researchers (e.g., Burkard et al., 2014; Flynn et al., 2012) have found that supportive dissertation-chairing relationships can have positive impacts on doctoral students. Yet, a unique finding of this study is that chairing relationships can also positively affect dissertation chairs. Participants discussed growing and experiencing feelings including pride, frustration, and fulfillment from their chairing relationships.
In the growth in student autonomy theme, numerous participants discussed helping students develop more independence and step into a more collegial role in their dissertation-chairing relationships. To a degree, this theme aligns with how Jorgensen and Wester (2020) and Ghoston and colleagues (2020) highlighted the need for accountability and developing doctoral students’ researcher identities in chairing relationships. However, our participants framed helping students become more autonomous as a mutually influenced working alliance that required doctoral student initiative and effort for their chairs to reciprocate. In other words, it seems that dissertation chairs believed doctoral students’ steady effort played a role in creating positive relational momentum throughout a consistent pattern of feedback and support. Additionally, for some participants, fostering student autonomy involved discussing boundaries and the navigation of transference and countertransference within the relationship dynamic. Completing a dissertation can be a challenging process in which students face numerous emotional roadblocks (Lamar & Helm, 2017; Pyhältö et al., 2012) and, for some participants, promoting student autonomy involved exploring and discussing how dependence may function as a defense mechanism for students to cover up their embarrassment, fear, or low self-efficacy.
Our findings also deepen the previous research on the importance of authenticity in dissertation-chairing relationships (Ghoston et al., 2020; Jorgensen & Wester, 2020; Purgason et al., 2016). Many participants directed the relationship toward mutually vulnerable places relevant to students’ dissertations. For example, some participants initiated authentic conversations when students felt stuck. When conflict in a relationship is unacknowledged, the person with less power in the relationship often responds in inauthentic ways; therefore, chairs should take the lead in venturing into vulnerable areas to help move the dissertation forward (Jordan, 2000). For participants, vulnerability included helping students overcome roadblocks and honest discussions and broaching of relationship dynamics, emotions, life experiences, and culture (Jordan, 2010; Purgason et al., 2016).
Our theme of adaptation to student needs highlights the way feedback plays out in mutually impacted relationship dynamics (Ghoston et al., 2020; Jorgensen & Wester, 2020). For example, numerous participants described how they adjusted their feedback styles to meet students’ sensitivity levels. In these cases, participants seemed to be using anticipatory empathy, or the ability to recognize and respond to covert and contextual life circumstances that influence a person (Jordan, 2010). These individualized and emotionally aware strategies can help students overcome barriers in their dissertation processes (Purgason et al., 2018). Additionally, consistent with relational pedagogy (Noddings, 2003), participants viewed dissertation-chairing relationships characterized by trust and safety as critical for helping reduce students’ feelings of shame or inadequacy and helping them feel safe in making mistakes. For many participants, developing trust seemed intertwined with their consistent availability and responding to students with empathy instead of judgment (Purgason et al., 2016).
Interestingly, no participants discussed specific methods they used to evaluate their dissertation-chairing relationships despite previous researchers’ calls to strengthen evaluation of research mentoring relationships (Protivnak & Foss, 2009; Purgason et al., 2018). Utilizing evaluative instruments or conversations in combination with reflection of prior or current experiences with dissertation chairing may help chairs intentionally adjust their feedback and relational styles (Ghoston et al., 2020). The list of items contributing to dissertation chair success developed by Jorgensen and Wester (2020) in their Delphi study of expert dissertation chairpersons may serve as a starting point to develop of such an instrument or help facilitate authentic conversations of needs and expectations between chairs and students.
Implications
Doctoral Students
Because chairing relationships can have broad impacts and can evolve into other professional relationships after dissertation completion, doctoral students might recognize the importance of choosing a chairperson—if they have that luxury—with whom they see potential for deeper connection. Identifying their needs in a chairing relationship might help them choose a chair. To do this, doctoral students might reflect on questions such as: “Which characteristics of a dissertation chairperson are most important to me?” or “What do I need to feel safety and trust in a dissertation-chairing relationship?” Additionally, doctoral students may want to learn more about their program faculty before selecting a chairperson. Doctoral students might interview potential chairs and ask them questions about their relationship styles. Such questions might include: “What did being authentic look like for you in previous chairing relationships?” and “How do you adapt your dissertation chairing to meet student needs?” Doctoral students might also consider their feelings and intuitions about relationships with faculty by assessing the levels of safety, trust, and authenticity they experience with various faculty members.
Ideally, dissertation chairs should facilitate authentic conversations about roadblocks for doctoral students throughout the dissertation process. However, sometimes chairs might be unaware of these roadblocks and doctoral students might consider taking risks to share their insecurities and relational needs with their chairs. Depending on the relational dynamics and power differential, doctoral students might consider the potential benefits and downsides of sharing such information and gauge the level of trust and safety they feel in the relationship. If a dissertation-chairing relationship does not feel safe, a student may consider broaching the topic with their chairperson or, depending upon the culture and policies of their program, switching to another chairperson who feels safer. Alternatively, doctoral students could work on their insecurities and roadblocks with others in their lives, including possibly in their own personal counseling. Personal counseling may be a more appropriate venue to discuss some issues as opposed to the dissertation-chairing relationship. Finally, given the prevalence of intense feelings doctoral students can experience during the dissertation process (Lamar & Helm, 2017; Pyhältö et al., 2012), they might reflect on their insecurities related to their dissertations and the ways their insecurities might affect their dissertation-chairing relationships. As participants discussed in the growth in student autonomy theme, discussing these thoughts and feelings through open and honest dialogue within trusting and safe relationships with their dissertation chairs might help deepen relationships and allow for opportunities to receive more personalized support.
Counselor Educators
To help doctoral students overcome roadblocks and insecurities, dissertation chairs can help students feel more connected through intentional creation of mutually empathic, safe, trusting, and authentic relationships. As the individuals with more power in the relationship, chairs should be ready to initiate conversations that are authentic and help set expectations, including conversations where they broach culture (Jordan, 2010; Purgason et al., 2016). For example, dissertation chairs may consider sharing vulnerable stories from their dissertation journeys or their lives to validate and normalize students’ experiences. Similarly, they might demonstrate humility by admitting the limits of their knowledge and skills and apologizing to students for relational ruptures when appropriate. For instance, a chairperson might admit their lack of knowledge about the methodology a student is using in their dissertation while helping them develop autonomy to seek out resources (e.g., other faculty, books, videos) to get the support they need. Additionally, consistently responding to students with empathy and encouragement if they make mistakes or do not meet deadlines may help build trust and self-confidence for students, creating an environment where they feel safer taking risks interpersonally and with their research. A safe and supportive relational foundation is essential for the trust-building required for learning to take place (Noddings, 2003).
Finally, authentic conversations might also include using immediacy to talk about relationship and cultural dynamics. Utilizing relational-cultural theory (Jordan, 2010; Purgason et al., 2016) may help chairs develop skills for initiating authentic and culturally infused conversations with their students. These conversations might happen throughout the dissertation-chairing relationship. Toward the beginning of the relationship, chairs might ask: “What do you need to build trust and safety in a relationship?” or “How do our cultural differences impact our work together?” At this phase in the relationship, chairs may also openly share their cultural backgrounds and their dissertation styles, including strengths and areas for growth as a dissertation chairperson. Closer to the completion of the dissertation, counselor educators can facilitate discussions with students on the wide-reaching impact of their relationships given the non-compartmentalized nature of dissertation relationships. Chairs might ask students questions such as “How are you different because of our relationship?” or “In what ways has our relationship helped you overcome barriers in your dissertation process?” and be willing to share how the relationship has affected them as well. Acknowledging and reflecting on that shared growth in conversation together may help both parties learn and feel more connected (Purgason et al., 2016).
Counselor educators can use ongoing reflective practice to develop and hone intentional approaches to building dissertation-chairing relationships. Counselor educators might ask themselves, “What relational qualities do I have to offer that contribute to helpful dissertation-chairing relationships?”, “How do I believe that mentoring relationships impact mentees’ development as researchers?”, or “What theories drive my research mentorship philosophy?” As a tangible output for addressing these questions, counselor educators can write philosophy of research mentorship statements, similar to philosophy of teaching or supervision statements. These statements can help counselor educators comprehensively define their approaches to research mentoring relationships. Counselor educators might revisit these statements throughout their careers as research on mentoring and their beliefs about dissertation chairing evolve. Additionally, counselor educators might create and share advisor disclosure statements with doctoral students to help clarify roles and expectations (Sangganjanavanich & Magnuson, 2009). Advisor statements may help alleviate role confusion and emphasize to students early in the relationship that doctoral students should grow as autonomous researchers and contribute to building a working alliance.
Counseling Programs
Numerous researchers have called for doctoral counseling programs to integrate more purposeful research mentorship in structured and systematic ways that could help offer more supportive relationships for doctoral students (Lamar & Helm, 2017; Perera-Diltz & Sauerheber, 2017). Counseling programs could establish structures that allow counselor educators and doctoral students to build trust early on in students’ programs. Connections developed between dissertation chairs and students in research apprenticeships; research teams; and co-teaching, advising, and informal program gatherings may provide relationships space to grow before students start their dissertations. Counseling programs might also establish methods for helping counselor educators evaluate dissertation-chairing relationships (Protivnak & Foss, 2009). Gaining an understanding of how students internalize feedback may help dissertation chairs better adapt to student needs and intentionally build expansive relationships (Ghoston et al., 2020). In line with CACREP’s requirement that counseling programs comprehensively evaluate their effectiveness, programs could regularly send out surveys to doctoral students who have recently completed their dissertations or withdrew during the dissertation stage to seek feedback on former students’ experiences of dissertation-chairing relationships (CACREP, 2015, Section 4). Such surveys might ask former students about their experiences of receiving feedback, the impact of their dissertation-chairing relationship, time and resources their chairperson dedicated to them, and challenges and successes they faced during the dissertation process. Program faculty could then use this feedback to improve their research mentoring programs by developing strategic plans including both individual and programmatic concrete goals (Purgason et al., 2018). Alternatively, dissertation chairs could conduct exit interviews with students.
Limitations
We identified several limitations in our study. First, all research team members identified as White, which may have limited our data analysis process based on our shared, privileged racial/ethnic identity. A coding team with different races and ethnicities may have arrived at a different thematic structure and may have more heavily emphasized cultural considerations in dissertation-chairing relationship dynamics. Second, in our interview protocol and demographic data survey, we did not ask many questions eliciting depth on the culture of participants’ institutions. Knowing more about the structures of participants’ programmatic and institutional supports and stressors for faculty members (e.g., teaching loads, policies that may contradict supporting student success) may have helped us analyze our data with a richer appreciation of contexts (van Manen, 1990; Hays & Singh, 2012). Third, our worldviews possibly influenced the questions we did not ask participants regarding how they navigated cultural differences with their students. Even though a few participants talked about navigating cultural differences, we do not have a clear sense of how cultural differences influenced participants’ chairing relationships. Cross-cultural mentorship relationships in counselor education are influenced by a myriad of complex relational and contextual factors related to racial/ethnic identity and White racism inherent in the field of counseling (Brown & Grothaus, 2019). These cross-cultural relationships warrant more focused investigation. Fourth, counselor educators who emphasized relationship-building in their dissertation chairing may have been more likely to participate in our study because they believed in the importance of our topic. Therefore, our findings may not reflect the relationships of those who do not emphasize relational approaches to dissertation chairing. Fifth, we did not explore dissertation relationships that took place in virtual programs. Chairs may experience relationship dynamics differently when interactions only occur virtually as opposed to mostly in person.
Directions for Future Research
First, future researchers might explore how counselor educators and doctoral students navigate power dynamics and cultural context in dissertation-chairing relationships (Borders et al., 2012; Jorgensen & Wester, 2020; Neale-McFall & Ward, 2015; Purgason et al., 2018). Fostering mutually fulfilling connections in dissertation-chairing relationships may help counselor educators attend to the unique needs of underrepresented students (Purgason et al., 2016) and help make research more accessible to doctoral students from more collectivist cultural backgrounds. Given the importance of authentic conversations and egalitarian relationships expressed by participants, further exploration of how counselor educators approach cultural, country of origin, worldview, gender, and other differences in dissertation-chairing relationships between themselves and students seems warranted. Second, participants in this study mostly talked about positive outcomes of dissertation-chairing relationships and helpful strategies they used to build relationships. Given the prevalence of negative dissertation relationships reported by doctoral students and their harmful impact on completion rates and mental health (Flynn et al., 2012; Lamar & Helm, 2017; Protivnak & Foss, 2009; Rigler et al., 2017), future researchers might examine ways that dissertation chairs can identify, navigate, and heal relational ruptures. Third, outcome research could illuminate the positive and negative impacts that dissertation-chairing relationships can have on students’ researcher self-efficacy, researcher identity development, and future research productivity. Because participants described tailoring their feedback styles to meet students’ unique needs but did not clearly describe evaluating the impact of their feedback, future researchers might examine the impact that different forms and styles of feedback have on students. Fourth, future researchers should explore institutional and programmatic factors that complicate chairs’ abilities to provide research mentorship to students. Finally, there are numerous theories of counseling supervision and adult learning that may apply to dissertation-chairing relationships but few theories specific to research mentorship or dissertation-chairing relationships in counselor education (Purgason et al., 2016). Future researchers might develop theories in this area by asking counselor educators about values, beliefs, and attitudes that drive their research mentorship philosophy and practice or by writing conceptual articles applying existing counseling theories to dissertation chairing.
Conclusion
Our research offers insights from counselor educators on how to foster supportive dissertation-chairing relationships. Counselor educators may utilize our findings to facilitate reflection regarding their relationship-building skills in dissertation-chairing relationships. Counselor educators intentionally build dissertation-chairing relationships to help their students overcome barriers to completing their dissertations and preparing them as future scholars.
Conflict of Interest and Funding Disclosure
The authors reported no conflict of interest
or funding contributions for the development
of this manuscript.
References
Borders, L. D., Wester, K. L., Granello, D. H., Chang, C. Y., Hays, D. G., Pepperell, J., & Spurgeon, S. L. (2012). Association for Counselor Education and Supervision guidelines for research mentorship: Development and implementation. Counselor Education and Supervision, 51(3), 162–175.
https://doi.org/10.1002/j.1556-6978.2012.00012.x
Brown, E. M., & Grothaus, T. (2019). Experiences of cross-racial trust in mentoring relationships between Black doctoral counseling students and White counselor educators and supervisors. The Professional Counselor, 9(3), 211–225. https://doi.org/10.15241/emb.9.3.211
Burkard, A. W., Knox, S. K., DeWalt, T., Fuller, S., Hill, C., & Schlosser, L. Z. (2014). Dissertation experiences of doctoral graduates from professional psychology programs. Counselling Psychology Quarterly, 27(1), 19–54. https://doi.org/10.1080/09515070.2013.821596
Council for Accreditation of Counseling and Related Educational Programs. (2015). 2016 CACREP standards. https://www.cacrep.org/for-programs/2016-cacrep-standards
Dahlberg, K. (2006). The essence of essences: The search for meaning structures in phenomenological analysis of lifeworld phenomena. International Journal of Qualitative Studies on Health and Well-Being, 1(1), 11–19. https://doi.org/10.1080/17482620500478405
Flynn, S. V., Chasek, C. L., Harper, I. F., Murphy, K. M., & Jorgensen, M. F. (2012). A qualitative inquiry of the counseling dissertation process. Counselor Education and Supervision, 51(4), 242–255.
https://doi.org/10.1002/j.1556-6978.2012.00018.x
Ghoston, M., Grimes, T., Graham, J., Grimes, J., & Field, T. A. (2020). Faculty perspectives on strategies for successful navigation of the dissertation process in counselor education. The Professional Counselor, 10(4), 615–631. https://doi.org/10.15241/mg.10.4.615
Hays, D. G., & Singh, A. A. (2012). Qualitative inquiry in clinical and educational settings. Guilford.
Heidegger, M. (1962). Being and time (J. Macquarrie & E. Robinson, Trans.). Harper and Row.
Jordan, J. V. (2000). The role of mutual empathy in relational/cultural theory. Journal of Clinical Psychology, 56(8), 1005–1016. https://doi.org/cfp6pr
Jordan, J. V. (2010). Relational–cultural therapy. American Psychological Association.
Jorgensen, M. F., & Wester, K. L. (2020). Aspects contributing to dissertation chair success: Consensus among counselor educators. Journal of Counselor Preparation and Supervision, 13(3), 117–144.
http://doi.org/10.7729/42.1404
Lamar, M. R., & Helm, H. M. (2017). Understanding the researcher identity development of counselor education and supervision doctoral students. Counselor Education and Supervision, 56(1), 2–18.
https://doi.org/10.1002/ceas.12056
Neale-McFall, C., & Ward, C. A. (2015). Factors contributing to counselor education doctoral students’ satisfaction with their dissertation chairperson. The Professional Counselor, 5(1), 185–194.
https://doi.org/10.15241/cnm.5.1.185
Noddings, N. (2003). Caring: A feminine approach to ethics and moral education (2nd ed.). University of California Press.
Patton, M. Q. (2014). Qualitative research & evaluation methods: Integrating theory and practice (4th ed.). SAGE.
Perera-Diltz, D., & Sauerheber, J. D. (2017). Mentoring and other valued components of counselor educator doctoral training: A Delphi study. International Journal of Mentoring and Coaching in Education, 6(2), 116–127. https://doi.org/10.1108/IJMCE-09-2016-0064
Preston, J., Trepal, H., Morgan, A., Jacques, J., Smith, J. D., & Field, T. A. (2020). Components of a high-quality doctoral program in counselor education and supervision. The Professional Counselor, 10(4), 453–471. https://doi.org/10.15241/jp.10.4.453
Protivnak, J. J., & Foss, L. L. (2009). An exploration of themes that influence the counselor education doctoral student experience. Counselor Education and Supervision, 48(4), 239–256.
https://doi.org/10.1002/j.1556-6978.2009.tb00078.x
Purgason, L. L., Avent, J. R., Cashwell, C. S., Jordan, M. E., & Reese, R. F. (2016). Culturally relevant advising: Applying relational-cultural theory in counselor education. Journal of Counseling & Development, 94(4), 429–436. https://doi.org/10.1002/jcad.12101
Purgason, L. L., Lloyd-Hazlett, J., & Avent Harris, J. R. (2018). Mentoring counselor education students: A Delphi study with leaders in the field. Journal of Counselor Leadership and Advocacy, 5(2), 122–136.
https://doi.org/10.1080/2326716X.2018.1452080
Pyhältö, K., Toom, A., Stubb, J., & Lonka, K. (2012). Challenges of becoming a scholar: A study of doctoral students’ problems and well-being. International Scholarly Research Notices, 2012.
https://doi.org/10.5402/2012/934941
Rigler, K. L., Bowlin, L. K., Sweat, K., Watts, S., & Thorne, R. (2017). Agency, socialization, and support: A critical review of doctoral student attrition. Paper presented at the 3rd International Conference on Doctoral Education, University of Central Florida.
Sangganjanavanich, V. F., & Magnuson, S. (2009). Averting role confusion between doctoral students and major advisers: Adviser disclosure statements. Counselor Education and Supervision, 48(3), 194–203.
https://doi.org/10.1002/j.1556-6978.2009.tb00074.x
Schlosser, L. Z., Knox, S., Moskovitz, A. R., & Hill, C. E. (2003). A qualitative examination of graduate advising relationships: The advisee perspective. Journal of Counseling Psychology, 50(2), 178–188.
https://doi.org/10.1037/0022-0167.50.2.178
van Manen, M. (1990). Researching lived experience: Human science for an action sensitive pedagogy (1st ed.). Althouse Press.
Phillip L. Waalkes, PhD, NCC, ACS, is an assistant professor at the University of Missouri – St. Louis. Daniel A. DeCino, PhD, NCC, LPC, is an assistant professor at the University of South Dakota. Maribeth F. Jorgensen, PhD, NCC, LPC, LMHC, LIMHP, is an assistant professor at Central Washington University. Tiffany Somerville, MS, is a doctoral student at the University of Missouri – Saint Louis. Correspondence may be addressed to Phillip L. Waalkes, 415 Marillac Hall, 1 University Blvd., St. Louis, MO 63121, waalkesp@umsl.edu.

 I thoroughly enjoyed this book. The authors of this book present the material in an authentic voice that makes the reader feel accepted and understood at whatever stage of the process they are at in the counseling program. The authors readily present their own fears and expectations when they began graduate school. They are humble and honest about things they wish they had done differently, and they embody a calm and considerate approach with a welcome addition of humor.
I thoroughly enjoyed this book. The authors of this book present the material in an authentic voice that makes the reader feel accepted and understood at whatever stage of the process they are at in the counseling program. The authors readily present their own fears and expectations when they began graduate school. They are humble and honest about things they wish they had done differently, and they embody a calm and considerate approach with a welcome addition of humor. Dr. Samuel T. Gladding’s third edition of Becoming a Counselor: The Light, the Bright, and the Serious offers a genuine and insightful reflection of his experiences both as an individual and as a counselor.
Dr. Samuel T. Gladding’s third edition of Becoming a Counselor: The Light, the Bright, and the Serious offers a genuine and insightful reflection of his experiences both as an individual and as a counselor.